4. The Integument
Authors: Corwin, Elizabeth J.
Title: Handbook of Pathophysiology, 3rd Edition
Copyright 2008 Lippincott Williams & Wilkins
> Table of Contents > Unit II - Effective and Ineffective Health Protection > Chapter 4 - The Integument
Chapter 4
The Integument
The integument is the skin, the largest mass of tissue in the body. The skin functions to protect and insulate underlying structures and serves as a calorie reserve. The skin mirrors our emotions and stresses and impacts how others relate to and treat us. In a lifetime, the skin may be cut, bitten, irritated, burned, or infected. The skin has enormous resilience and capacity for recovery.
Physiologic Concepts
Structure and Function of the Skin
The skin is composed of three layers, each consisting of different cell types and serving different functions. The three layers are the epidermis, dermis, and subcutaneous layer. A diagram of the skin is shown in Figure 4-1.
Epidermis
The outermost layer of the skin is the epidermis. The cells of the epidermis continually undergo mitosis and are replaced approximately every 30 days. The epidermis contains sensory receptors for touch, temperature, vibration, and pain.
The main component of the epidermis is the protein keratin, produced by cells called keratinocytes. Keratin is an extremely durable, tough substance that is insoluble in water. Keratin prevents loss of body water and protects the epidermis from irritants and infection-causing
P.88
microorganisms. Keratin is the main component of the skin appendages: the nails and the hair.
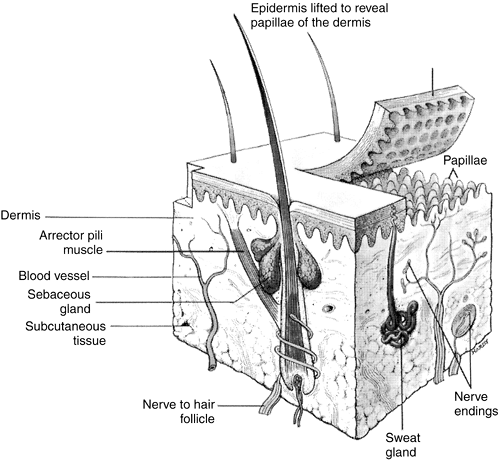 |
Figure 4-1. Three-dimensional view of the skin. (From Porth, C. [2005]. Pathophysiology: Concepts of altered health states [7th ed.]. Philadelphia: Lippincott Williams & Wilkins. ). |
Melanocyte cells are present at the base of the epidermis. Melanocytes synthesize and secrete melanin in response to stimulation by melanocyte-stimulating hormone, which is produced by the anterior pituitary. Melanin is a black pigment that disperses throughout the epidermis to protect cells from ultraviolet radiation.
Immune cells, called Langerhans' cells, are present throughout the epidermis. Langerhans' cells recognize foreign particles or microorganisms that enter the skin and present them to T lymphocytes as the first step in initiating an immune attack. Langerhans' cells may be responsible for recognizing and eliminating dysplastic or neoplastic skin cells. Langerhans' cells are physically associated with sympathetic nerves, suggesting a relation between the nervous system and the ability of the skin to fight off infection or prevent skin cancer. Stress may affect the functioning of Langerhans' cells by increasing sympathetic stimulation. Ultraviolet radiation may damage Langerhans' cells, reducing their ability to prevent cancer.
P.89
Dermis
Lying immediately under the epidermis, the dermis is considered loose connective tissue and is composed of fibroblast cells that secrete the proteins collagen and elastin. The collagen and elastin fibers are arranged haphazardly, giving the dermis distensibility and resilience. A gel-like substance, hyaluronic acid, is secreted by the connective tissue cells. Hyaluronic acid surrounds the proteins and gives the skin elasticity and turgor (tension). Throughout the dermis are blood vessels, sensory and sympathetic nerves, lymphatic vessels, hair follicles, and sweat and sebaceous glands. Mast cells, which release histamine during injury or inflammation, and macrophages, which phagocytize dead cells and microorganisms, are also present.
Blood vessels in the dermis supply the dermis and epidermis with nutrients and oxygen and remove waste products. Dermal blood flow offers a means for the body to control its temperature. With a decrease in body temperature, sympathetic nerves to the blood vessels are activated and increase the release of norepinephrine, causing constriction of the vessels and a conservation of body heat. If body temperature is too high, sympathetic stimulation of the dermal blood vessels is reduced, dilating the vessels and allowing for the transfer of body heat to the environment. Arteriovenous (AV) connections, called anastomoses, are present on some blood vessels. AV anastomoses facilitate skin temperature regulation by allowing blood to bypass the upper layers of the dermis in times of severe cold. Sympathetic nerves to the dermis also innervate sweat glands, sebaceous (oil) glands, and hair follicles.
Subcutaneous Layer
Lying beneath the dermis, the subcutaneous layer of the skin is composed of fat and connective tissue and acts as both a shock absorber and a heat insulator. The subcutaneous layer is a calorie reserve station as well: fat can be stored in this layer and, if needed, broken down to serve as an energy source.
Hair and Nails
The nails are keratinized plates that extend from the fingers and the toes. The nails protect the fingertips and most likely evolved with an original purpose of defense. The hair is hardened keratin that grows at variable rates on different parts of the body. Hair grows as a follicle shaft in a canal, beginning deep in the dermis. In addition to a hair follicle, each canal contains a sebaceous gland and a smooth muscle fiber, called an arrector pili muscle. When this muscle cell is stimulated by the sympathetic nervous system, it causes the hair to stand on end. Hair on the head may protect against sunburn.
Sebaceous Glands
The sebaceous glands accompany the hair follicles. They secrete an oily substance called sebum into the surrounding canal. Sebaceous glands are
P.90
present all over the body, especially on the face, chest, and back. Testosterone increases the size of the sebaceous glands and the production of sebum. Testosterone levels increase in males and females during puberty.
Sweat Glands
There are two types of sweat glands: eccrine and apocrine. Eccrine sweat glands open directly onto the surface of the skin and are distributed over the entire body. Eccrine glands function mainly in cooling the body by means of evaporative heat loss. They are especially concentrated on the hands, feet, and forehead. Apocrine glands are mainly located in the axillae (armpits) and in the pubic and anal areas. Apocrine glands secrete sweat into the canals of the hair follicles. When acted upon by surface bacteria, the secretions of the apocrine glands cause the characteristic odor of perspiration.
![]() eriatric Consideration
eriatric Consideration
As an individual ages, all three layers of the skin change. The epidermis loses its elasticity and turgor and has a reduced capacity to produce and distribute melanin. Age spots (concentrated deposits of melanin) appear. The hair and nails become thin and brittle. The hair grays as melanocytes are lost. The number of Langerhans' cells decreases, increasing the skin's susceptibility to solar damage. Both poor blood flow and decreased Langerhans' cell function increase the risk of infection. Sensory receptors are reduced in number, contributing to an increased risk of injury. Poor blood flow and reduced immune function delay wound healing. Decreased sebaceous and sweat gland functioning cause drying and wrinkling of the skin. The ability of the body to cool itself by sweating and vasodilatation, or to conserve heat by vasoconstriction, is reduced, most likely due to a decreased responsiveness of the vasculature to sympathetic stimulation. A reduced ability to cool or warm the body by changing the skin's blood flow increases the risk of hyperthermia in elderly adults exposed to prolonged heat and the risk of hypothermia in elderly adults exposed to severe cold.
Vitamin D
The skin plays a vital role in the body's use of vitamin D. Vitamin D is a hormone obtained in the diet in an inactive form. It is required both for the absorption of calcium from the gut and in order to reduce the renal excretion of calcium. For vitamin D to function, however, it first must be activated by the body. The initial step in vitamin D activation occurs in the skin as a result of ultraviolet (UV) radiation, after which it is further acted upon by the kidney and the liver. Vitamin D activation is increased in response to a decrease in serum calcium. Because vitamin D acts as a hormone, the skin may be considered an endocrine gland.
P.91
Pathophysiologic Concepts
Many different lesions occur on the skin. They are described on the basis of size, depth, color, and consistency.
Bulla
Measuring more than 1.0 cm and filled with watery fluid, a bulla is a large, raised area on the skin. Bullae are large blisters that can occur after a burn.
Crust
A crust is the accumulation of dried serous (serum-like) or seropurulent (pus) exudate on the skin (e.g., the crust seen on an impetigo or herpes lesion). It is usually golden in color.
Erosion
An erosion is an area on the body characterized by the loss of superficial epidermis. Typically the area is moist, but it does not bleed (e.g., the skin after bursting of a blister or vesicle).
Excoriation
An excoriation is a scratch on the skin (e.g., a skinned knee). There may be slight bleeding.
Fissure
A fissure is a linear crack in the skin, for example, as seen with athlete's foot. The fissure may be pink or red, but there is usually no bleeding.
Keloid
A keloid is a scar formation on the skin, occurring after a trauma, injury, or piercing, that is out of proportion to the injury. Keloids appear raised, red, and firm. There is a genetic tendency to develop keloids, and this type of scarring is especially common in African-Americans. An individual prone to keloid formation should alert a health care provider when a skin injury occurs. Prevention of keloid formation is supported by careful surgical techniques, pressure dressings, good wound care, and adequate nutrition. There is no single best treatment for an existing keloid, although topical dressings, steroid injections, and laser therapy all have been used with some success. Immunotherapy is under investigation. Removal of a keloid may worsen scarring in some cases.
P.92
Lichenification
Thickened, roughened skin that may occur with constant irritation is known as lichenification. This condition is seen, for example, in skin with atopic dermatitis.
Macule
A macule is a flattened area of the skin, characterized by a change in color. A macule (e.g., a freckle or a flat mole, also called a nevus) is typically smaller than 1.0 cm in diameter.
Nodule
A nodule is a solid, elevated mass with a measurement between 1.0 cm and 2.0 cm in diameter. It is firmer in consistency than a papule and occurs deeper in the dermis (e.g., a cyst).
Papule
A papule is a solid, elevated mass, smaller than 1.0 cm in diameter. Examples of papules include elevated moles and warts.
Petechia
A deep red spot of pinpoint hemorrhage under the skin is called petechia. Petechiae may signify a bleeding disorder or fragility of the capillaries and may accompany a serious infection.
Plaque
A plaque is a flat, raised surface with a measurement larger than 1.0 cm. Examples of plaques are several papules grouped together or the lesions seen with psoriasis.
Pruritus
Pruritus refers to itching of the skin. Pruritus may occur as a primary response to a surface irritant or inflammation, for example, after a mosquito bite, or with dry skin. Primary pruritus results from release of histamine during inflammation. Pruritus may occur secondarily to a systemic disease, such as liver or kidney failure. With systemic disease, metabolic toxins may accumulate in the interstitial fluid under the skin.
Purpura
A purpuric lesion is a large patch of purple discoloration under the skin associated with hemorrhage. It may result from a variety of causes,
P.93
including thrombocytopenia (decreased platelets), trauma (a black and blue mark ), or an allergic response. A purpuric lesion occurring without trauma may be a red flag for bleeding elsewhere in the body, including the brain.
Pustule
A pustule is an elevated vesicle filled with pus. Examples of pustules are the lesions of impetigo or acne.
Scale
A scale is a flake of epidermis. Examples of scaling are seen in dandruff or dried skin.
Scar
A scar is an area of the body where the skin has been replaced by fibrous tissue (e.g., a burn scar). A scar may be thin or thick.
Tumor
A tumor is a large, solid mass that is elevated and larger than 1.0 to 2.0 cm. Tumors may be neoplastic or benign, as, for example, a breast cancer versus a lipoma (a benign tumor made up mostly of adipose tissue).
Ulcer
An ulcer is an area with loss of epidermal and deeper layers of the skin that may bleed and scar. An example of an ulcer is a decubitus ulcer (pressure sore).
Urticaria
Urticaria, also known as hives, consists of raised edematous plaques (wheals) associated with intense itching (pruritus). Urticaria results from the release of histamine during an inflammatory response to an allergen to which the individual has become sensitized. Chronic urticaria may accompany systemic disorders such as hepatitis, some cancers, or thyroid abnormality.
Vesicle
A vesicle is a small, raised area on the skin with a measurement of less than 1.0 cm. It is formed by the presence of serous fluid within the skin layers (e.g., a chickenpox blister).
P.94
Wheal
A wheal is a raised area of skin edema that exists only temporarily and itches (e.g., the area surrounding a mosquito bite or an area of the skin during an occurrence of urticaria [hives]). The center of a wheal is pink or red, with a surrounding circle of paler skin.
![]() eriatric Consideration
eriatric Consideration
The elderly frequently present with purpura and petechia, especially on the legs. Petechia and purpura in the elderly usually indicate fragility of the blood vessels or a platelet disorder. However, in some cases, these lesions may be caused by a fall or may result from elder abuse. Idiopathic purpura may occur in young women.
Conditions of Disease or Injury
Contact Dermatitis
Contact dermatitis is an acute or chronic inflammation of the skin caused by exposure to an irritant (irritant dermatitis) or allergen (allergic dermatitis). The location of the dermatitis on the skin corresponds to the site of exposure. Allergic contact dermatitis occurs when Langerhans' cells process and present an allergen to nearby T cells. The T cells respond with a type IV hypersensitivity response against the allergen. The response is delayed in that it takes hours to days to become evident. Irritant dermatitis occurs when the skin is exposed to a substance that dries out or irritates it. Irritant dermatitis does not involve a specific immune response, but instead is only inflammatory.
Common causes of allergic dermatitis include poison ivy or poison oak and chemicals found in jewelry. Common causes of irritant dermatitis include soaps, detergents, household cleaners, insecticides, and dusts. Some foods and spices may also cause contact dermatitis.
Clinical Manifestations
Both types of dermatitis present acutely with localized papules, erythema (redness), and oozing vesicles in an area of contact. The vesicles burst and crust. Pruritus may be intense.
Allergic dermatitis typically presents 1 to 2 days after exposure.
Diagnosis
Dermatitis usually follows the pattern of exposure for example, poison ivy typically travels vertically up the legs or may be present only on areas of the skin that were uncovered when exposed to the plant. A circle of lesions around the wrist may indicate an allergy to a bracelet or watch,
P.95
whereas lesions below the umbilicus may indicate an allergy to the metal of a zipper. Reddened, irritated hands may indicate an inflammatory response to dishwashing. A good history accompanying the physical pattern is the key to diagnosis.Allergy skin testing may be indicated.
Complications
Chronic conditions may cause lichenification, fissures, and scales.
An infection of the skin may result from repeated scratching and skin breakdown.
A severe response to poison ivy or another potent allergen may result in significant reddening and swelling of the face. The eyes may be closed because of edema.
Treatment
Identifying the cause of the dermatitis and avoiding exposure prevents recurrence.
Cool compresses reduce inflammation. Oatmeal soaks or baths in other soothing chemicals may provide relief. Antihistamines may be used to reduce itching.
Short-term, topical, anti-inflammatory, steroidal therapy may be used to interrupt the inflammation. For severe attacks involving the eyes and face, a burst of systemic corticosteroids often is used.
Atopic Dermatitis
Atopic dermatitis is an inflammation of the skin involving overstimulation of T lymphocytes and mast cells. Histamine from the mast cells causes itching and erythema. Scratching can cause skin breakdown. Atopic dermatitis is frequently seen in infants and children, but it may persist into adulthood. There appears to be a genetic tendency toward the disease. In addition, it is frequently seen in families with a high rate of other inflammatory disorders such as asthma or allergy.
Clinical Manifestations
Erythema with crusted or oozing lesions. In infants, lesions often appear on the face and buttocks. In older children and teens, the lesions appear more commonly on the hands and feet, behind the knees, and in the bends of the elbows.
Pruritus is intense and leads to a continual cycle of inflammation and lesion formation.
Diagnosis
Diagnosis is usually accomplished with the help of a good history and physical examination.
P.96
Complications
Infection of the skin with common surface bacteria, especially Staphylococcus aureus, or with viruses such as herpes simplex may develop. Individuals should avoid inoculation with live, attenuated viruses.
Treatment
Avoidance of known irritants or allergens.
Antihistamines to help control itching.
Cool compresses to reduce inflammation.
Topical low-dose steroids to reduce inflammation and allow healing.
Acne
Acne is a common inflammatory disease of a sebaceous gland associated with a hair follicle, called the pilosebaceous unit. There are two types of acne: inflammatory and non-inflammatory. Both types of acne are characterized by excessive sebum production. The excess sebum accumulates in the follicle, causing the follicle to swell.
In inflammatory acne, the follicle becomes blocked by the sebum and a type of acne-specific bacterium, Propionibacterium acnes, proliferates in the canal. Eventually, the follicle ruptures and the sebum and bacteria are released into the dermis, causing inflammation of the dermal tissue. In non-inflammatory acne, the follicle does not burst but remains dilated. The sebum either moves to the skin surface (a blackhead) or the canal remains blocked (a whitehead).
Acne is commonly seen in teenagers and young adults, beginning with the onset of puberty. Although both boys and girls suffer from acne, it is especially severe and common in boys. Adults, especially women, may have a recurrence of acne.
Causes of Acne
Sebum production is stimulated by androgens, especially testosterone. The sharp increase in androgens seen in both girls and boys during puberty is largely responsible for the onset and severity of acne. There is little research support for traditional biases that diet or lack of facial cleansing contributes to acne, although P. acne infection of the obstructed follicle may be worsened by poor nutrition. Instead, there is a strong genetic influence over the development of acne that may be related to oversensitivity of the sebaceous glands to androgen or the presence of an environment favorable to the proliferation of bacteria. Other contributors to acne may be important and vary for any given individual. Protective against acne is estrogen, which opposes the action of androgen on the sebaceous glands and reduces the development of acne. In adult women, the development of acne may be related to other systemic conditions or
P.97
may occur as the level of testosterone relative to estrogen begins to rise in the early perimenopausal years.
Acne rosacea is a condition of the skin that develops in middle-aged adults of both sexes and is characterized by redness (erythema), papules, and pustules, especially on the forehead, nose, cheeks, and chin. Although no specific cause of acne rosacea has been identified, it is associated with heightened sensitivity to the sun. The condition may come and go and is typically exacerbated by hot drinks and alcohol. It may result in hypertrophy of the sebaceous glands, with thickening of the nose (rhinophyma), a permanent development. Eye irritation, including conjunctivitis, may be present. There is also a genetic tendency to develop rosacea, with light-skinned populations especially susceptible.
Clinical Manifestations
Acne may present with a variety of lesions on one individual. Lesions can include blackheads, whiteheads, nodules, pustules, cysts, and scars. Lesions are commonly over the face, back, and shoulders.
In women, acne may increase before or during the menstrual period when estrogen levels are lowest.
With rosacea, the face may turn bright red with even limited sun or alcohol exposure, and papules and pustules may develop.
Complications
Scarring may occur in severe cases of acne.
Self-esteem may be affected even with less severe conditions.
Rhinophyma may occur with rosacea.
Treatment
Topical agents such as benzoyl peroxide and retinoic acid (vitamin A, Retin A) are used to dry and to peel the skin. This effect increases cell turnover and opens the follicles and facilitates the movement of sebum to the skin. Benzoyl peroxide also works to eliminate P. acnes. Retin A may lead to excessive drying and redness of the skin, and individuals using Retin A must avoid unprotected sun exposure. Pregnant women are advised to avoid using Retin A.
Antibacterial soap may reduce bacterial contamination of the skin.
Topically applied antibiotics, often in combination with benzoyl peroxide, may be prescribed for use once or twice a day. Topical antibiotics, usually tetracycline, erythromycin, or clindamycin, work to reduce P. acnes proliferation. Treatment with this regimen typically takes at least 4 weeks to induce notable improvement.
Oral low-dose antibiotic therapy (e.g., tetracycline, doxycycline) may be administered to reduce bacterial proliferation in the follicle. Antibiotic therapy requires several weeks to be effective and may induce photosensitivity. Oral tetracycline damages developing teeth; therefore, it is
P.98
contraindicated in pregnant women or women planning to get pregnant. Tetracycline is also a drug of choice for rosacea.Birth-control pills containing estrogen can reduce sebum production. They may be used to treat acne in girls and women.
Systemic 13-cis-retinoic acid (isotretinoin) may be used for severe nodular cystic acne. This drug can cause severe birth defects and should not be used by young women who are or may get pregnant. Males likewise should avoid impregnating a partner while on isotretinoin.
Psoriasis
Psoriasis is a chronic, inflammatory skin disease first defined as a distinct disease entity in 1841 but described by its appearance centuries before. Psoriasis is characterized by rapid turnover of epidermal cells, leading to abnormal proliferation of the epidermis and the dermis. The skin demonstrates red, raised scaly plaques that can cover any body surface. Psoriasis has a strong genetic component and its prevalence varies by ethnicity, with Caucasians more frequently affected than those of African descent. The quality of life reported by patients with moderate or severe psoriasis can be quite compromised, with studies reporting life quality levels reduced to those reported by patients with severe diseases such as emphysema and heart failure. Psoriasis typically is established by the late 20s but may occur earlier.
Causes of Psoriasis
Although previously described as a disease of benign epithelial proliferation, it has become increasingly clear that psoriasis is in fact an autoimmune disorder. T lymphocytes are activated in response to an unknown stimulus, through an association with the skin's Langerhans' cells. Activation of localized T cells leads to the production of pro-inflammatory cytokines, including tumor necrosis factor alpha, and growth factors that stimulate abnormal cellular proliferation and turnover. Normal epidermal cell turnover is approximately 28 to 30 days; with psoriasis, the epidermis in affected areas may shed every 3 to 4 days. Rapid cell turnover results in increased metabolic rate and increased blood flow to the cells to support the high metabolism. Increased blood flow causes the erythema, and the rapid turnover and proliferation lead to poorly developed and immature cells. Small trauma to the skin results in exaggerated inflammation, causing epidermal thickening and plaque formation.
Risk Factors for Psoriasis
There is a genetic tendency for the development of psoriasis, with an increased incidence among family members. Over a thousand genes, primarily immune response and proliferation genes, have been identified that appear to play a role in the pathogenesis and maintenance of psoriasis. Environmental factors, including trauma to the skin, viral or bacterial infection, cigarette smoking, and stress, may worsen the condition. Certain drugs, including angiotensin-converting enzyme inhibitors and lithium, can precipitate or worsen an outbreak.
P.99
Clinical Manifestations
Well-demarcated (clearly bordered) erythematous plaques covered with silvery white scales develop, especially over knees, elbows, scalp, and in skin folds.
Lesions typically develop insidiously, with just one or two lesions later coalescing into many.
Nail pitting or separation of the nail is common.
Symptoms typically improve in summer and worsen in winter.
Diagnosis
Diagnosis is made based on history and physical examination. A family history of the disease may be recalled.
Complications
Severe infections of the lesions may develop.
A deforming arthritis similar to rheumatoid arthritis, called psoriatic arthritis, occurs in approximately 30 to 40% of individuals. When severe, this can be a disabling disease.
Because of the impact on patients' self-esteem, psychological stress, anxiety, depression, and anger may develop.
Treatment
The severity of disease determines treatment.
Mild disease is usually treated successfully with topical emollients to soften plaques, vitamin D analogues to reduce inflammation, or topical retinoids to peel the skin, the latter often in combination with topical steroids to reduce inflammation. Coal tar is an old and effective treatment that is applied to the skin for several weeks. Its exact mechanism of action is unknown.
Phototherapy with UVB may be used.
For more serious conditions, photochemotherapy is often used. This type of treatment employs a light-activated drug, methoxsalen (Psoralen), given orally to a patient 1 to 2 hours before he or she is exposed to ultraviolet radiation. Activated methoxsalen blocks DNA synthesis and so slows cellular replication and turnover. This treatment is identified by the acronym PUVA, referring to its combination of Psoralen (P) and long-wave ultraviolet radiation (UVA). Some concerns exist regarding its long-term effects, and individuals using PUVA should be screened regularly for skin cancer.
Moderate disease and flare-ups are often treated systemically, using chemotherapeutic drugs to affect cell turnover, antimetabolites to prevent cell cycling, or oral immunosuppressive drugs, such as corticosteroids, to suppress inflammation.
New treatment strategies for moderate or severe disease include immune modulating drugs. These drugs work by decreasing the number or functioning of pathogenic T cells or by blocking the effects
P.100
of the proinflammatory cytokines. Examples of immune modulating drugs approved by the FDA for the treatment of moderate or severe psoriasis include alefacept, efalizumab, and etanercept. Others are under development.Severe disease may require hospitalization and systemic steroids.
![]() eriatric Consideration
eriatric Consideration
The prevalence of psoriasis increases with age, making it a common disorder of the elderly. Because of changes in renal and hepatic clearance rates in the elderly, there is an increased risk of adverse drug side effects and drug interactions with several of the treatment options.
Viral Infections of the Skin
A variety of viral infections may present with a skin rash. Many of these rashes are most common during childhood (Table 4-1) but may occur at any time.
Rubeola
Rubeola, also called 10-day measles or red measles, is an upper respiratory tract infection caused by the paramyxovirus. Rubeola is usually seen in children and is transmitted by way of inspired droplets. It has a 7- to 12-day asymptomatic incubation period before signs of the disease appear and is highly contagious. Active disease is characterized by early (prodromal) symptoms followed by a rash.
Clinical Manifestations
Prodromal symptoms include high fever, barking cough, runny nose, and enlargement of lymph nodes. Active infection is characterized by Koplik's spots over the buccal (cheek) mucosa. A Koplik's spot is a pinpoint white spot surrounded by a red ring.
A maculopapular rash with erythema, beginning on approximately day 3 or 4, is another manifestation. The rash starts on the face, spreads to the trunk, and finally the extremities. The rash lasts approximately 4 days.
Diagnosis
Diagnosis is usually made by history and physical examination.
Complications
Measles encephalitis is a common complication of rubeola. It may be caused by the measles virus, or it may be a secondary bacterial infection. Recovery is usually complete, but lasting brain damage and death might occur.
Pneumonia may occur after measles.
Table 4-1. Common Childhood Rashes | ||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
P.101
P.102
Treatment
Primary treatment is prevention by vaccination with a live attenuated virus at 15 months after birth. A booster is usually administered at 4 to 5 years, and sometimes in the teen years. Treatment of measles infection is supportive and may involve antibiotics if a secondary bacterial infection develops.
Rubella
Rubella, also called German measles or 3-day measles, is a viral infection of the respiratory tract caused by the rubella virus. There is a 14- to 21-day incubation period after infection, followed by prodromal symptoms lasting 1 to 4 days. A rash then develops. Rubella is very contagious during the prodromal stage, but it may not be contagious once a rash develops.
Clinical Manifestations
Prodromal stage is characterized by low-grade fever, malaise, lymph node enlargement (especially post-auricular), sore throat, and headache.
Active infection is characterized by a diffuse maculopapular rash, which begins on the trunk and spreads to the extremities. The rash lasts for approximately 2 to 3 days.
Diagnosis
Diagnosis is made by history and physical examination.
Complications
Infection in a pregnant woman, especially during the first trimester, may cause severe birth defects in her infant.
Treatment
Primary treatment is prevention by vaccination with a live, attenuated virus at 15 months, at 4 to 5 years, and in the teen years. The vaccine, called an MMR vaccine, for measles (rubeola), mumps, and rubella, typically used is a combination vaccine for these three diseases.
All women of childbearing age should be tested for the presence of antibodies against rubella (a rubella titer test). A woman who is antibody negative (has never had rubella or been adequately vaccinated against it) should be immunized against the virus.
Treatment of rubella infection is supportive, and is focused on keeping the individual well-hydrated and rested.
![]() ediatric Consideration
ediatric Consideration
Rubella is a strong teratogenic agent (one that causes birth defects) and is most highly contagious before an individual develops obvious signs of infection. To protect pregnant women from infection and subsequent injury to a developing fetus, it is
P.103
imperative that all children be vaccinated against the virus during early childhood. Vaccinating young children protects any pregnant woman with whom the child may come in contact.
Roseola Infantum
Roseola is a common infection of infants between the ages of 6 months and 2 years, although children as old as 4 years may also develop the infection. Roseola appears to be viral in origin and is characterized by a sudden onset of high fever (38.9 C to 40.5 C; 100 F to 104 F) in an otherwise well child, lasting 3 to 5 days. After this time, a rash develops, especially over the trunk.
Clinical Manifestations
Sudden, high fever in an apparently well child, followed 3 to 5 days later by a red, lacy, macular rash over the trunk and neck.
Diagnosis
Diagnosis is made by history and physical examination. Typically, there is no lymph node enlargement (adenopathy).
Treatment
Reassurance is usually the only treatment required. Fever medication may be used.
Herpes Simplex 1 and 2
The herpesviruses include herpes simplex 1 and 2. Herpesviruses cause characteristic skin and mucous membrane lesions and are passed by viral shedding from the lesions. The incubation period for both viruses is approximately 2 to 24 days after infection. A prodromal period often precedes the appearance of lesions. During the prodromal period and the time of open lesions (a 2- to 6-week period), the virus is contagious. After an initial infection, the virus may lay dormant in the sensory nerve tract innervating the primary lesion. The dormant virus may become active again at any time, causing the reappearance of lesions. Reactivation of a latent herpes infection may occur with illness, stress, excessive sun exposure, or at certain times of the menstrual cycle.
Herpes simplex 2 is typically a genital or anal infection, whereas herpes simplex 1 is usually responsible for cold sores on the face. Either virus, however, is capable of infecting any site on the body. Herpes simplex 2 is considered a sexually transmitted disease.
Clinical Manifestations
Symptoms during the prodromal stage may include low-grade fever, malaise, and a burning or itching on the mouth or genitals.
With active infection, clusters of painful vesicles erupt on the lips, face, skin, nose, oral mucosa, genitalia, or anus. The vesicles may burn and itch. The vesicles rupture within 3 to 4 days and crust over. They usually disappear within the next week.
P.104
Diagnosis
Diagnosis is made by history and physical examination, although cell culture may be used to confirm a suspected outbreak.
Complications
Secondary bacterial infection of the vesicles may develop.
Herpes simplex may infect the eye, causing blindness (keratoconjunctivitis). A primary herpes simplex 2 infection during pregnancy may cause damage to the fetal central nervous system, including blindness and mental retardation. Risk to the fetus is especially high if the pregnant woman is exposed to the virus for the first time late in her pregnancy.
Neonatal infection by the virus may occur with an ascending vaginal or cervical infection during the pregnancy or during passage of the newborn through an infected birth canal.
Treatment
Oral or topical treatment with an antiviral drug (acyclovir, famciclovir), may reduce the frequency, duration, and intensity of the lesions.
Cesarean section is performed if active genital herpes infection is present or if there is suspicion that the pregnant woman is in the prodromal stage.
Chickenpox and Shingles
Chickenpox (varicella) and shingles (zoster) are infections caused by another herpesvirus, the varicella-zoster virus. Infection by the varicella-zoster virus causes the development of pruritic, fluid-filled vesicles on the skin.
Chickenpox is the primary infection by the virus. Chickenpox is highly contagious and is transmitted person to person by way of respiratory droplets. Chickenpox is usually an illness of childhood, but adults exposed to the virus for the first time may develop the disease. The varicella virus has an incubation period of 7 to 21 days and is contagious during a brief prodromal period (approximately 24 hours before lesions appear) and until all lesions are crusted over. The disease is usually self-limiting and resolves within 7 to 14 days.
Shingles typically occurs years after a chickenpox infection. Shingles is caused by varicella virus that has remained latent in a sensory nerve tract after recovery from chickenpox. When the virus is expressed again, it is called zoster. Zoster typically occurs along the dermatome (skin region) innervated by the infected nerve. Zoster often is seen in the elderly or in individuals who have a reduced immune system caused by illness or stress. Zoster appears to spread by direct contact with the lesion.
P.105
Clinical Manifestations
Low-grade fever and malaise may be present 24 hours before vesicles appear.
The rash of chickenpox begins as red macules, usually first appearing on the trunk and spreading to the face and extremities. Within a few hours, the macules become fluid-filled vesicles, with more macules developing in the mouth, axilla, labia, and vagina. These later vesicles progress to become fluid-filled. The vesicles burst after a few days and crust over.
Numerous macules, vesicles, and scabs at different stages may be present at any one time.
The vesicles of shingles typically present on the skin, unilaterally (on one side of the body) along the infected dermatome. Frequent sites of eruptions are the face, neck, and thoracic areas. The lesions may be small or large and few or many in number. Shingles may be very painful.
Diagnosis
Diagnosis is made by history and physical examination.
The key diagnostic tool for shingles is the unilateral location and pain.
Complications
Secondary bacterial infection of the vesicles may develop.
Pneumonia, encephalitis, or joint inflammation and pain may follow chickenpox infection.
Reye's syndrome may develop in children given aspirin during a chickenpox infection.
Adults who acquire chickenpox may have a particularly severe disease course and are at higher risk of developing pneumonia or other complications.
Chickenpox and shingles may spread internally in immunocompromised individuals, leading to increased morbidity and mortality.
Post-herpetic neuralgia (pain) may occur in a large percentage (10% to 70%) of individuals suffering from shingles. Post-herpetic neuralgia refers to pain that persists for longer than 1 month after the acute onset of shingles. It is most common in elderly patients and is difficult to relieve once it becomes established.
Treatment
Prevention of chickenpox is possible with the varicella vaccine. This vaccine can be given to children or adults, and is highly successful in preventing infection. Some individuals (approximately 10%) may develop a few vesicles 10 to 20 days after immunization and may be contagious to others at that time. It is hoped that by preventing varicella, the incidence of shingles will also decline, although this has not as yet been documented.
Treatment of active chickenpox infection is mainly supportive and is geared at preventing the development of secondary skin infections. Oatmeal baths, calamine lotion, and antihistamines may be used to reduce itching. In children, the nails may be cut, or mittens may be worn, to reduce scratching.
Antiviral drugs (acyclovir, vidarabine, sorivudine) may be prescribed after exposure or at the earliest sign of chickenpox infection in adults or in immunocompromised children to limit the degree of infection. The use of antiviral drugs in healthy children who have chickenpox may also be considered to reduce lesion number and length of infection.
Treatment of shingles includes analgesics for pain and antiviral drugs to limit viral replication. Systemic corticosteroids may be provided to reduce the risk of developing post-herpetic neuralgia. Individuals who do develop post-herpetic neuralgia may be treated with topical anesthetic agents, neural stabilizing drugs, or tricyclic antidepressants for pain relief. Better outcomes are achieved when treatment is instituted early.
P.106
Warts
In humans, warts (verrucae) are caused by infection with the human papillomavirus (HPV). Warts are benign papules that can occur anywhere on the skin. There are many different strains of HPV. Some strains preferentially infect the genital or anal region, causing genital warts, whereas others colonize the fingers and hands, causing simple warts. Plantar warts are warts on the bottom of the feet that grow in rather than out from the skin. Warts are passed by skin-to-skin contact. Genital warts are considered a sexually transmitted disease.
Some studies suggest that over 40% of young women using university health care centers for their gynecologic care have genital warts. Certain strains of genital warts have been identified as causing cervical cancer; other strains are unlikely to progress to cancer. The risk of developing cervical cancer is especially high in women with genital warts who smoke. This increased risk most likely occurs because cervical mucus concentrates tobacco toxins, which may then act synergistically with HPV to produce cancer.
Clinical Manifestations
Skin warts may be flat or round, large or small.
Genital warts have a cauliflower-type appearance. They may be seen on the head or shaft of the penis, on the labia, in the vagina, or surrounding the anus.
Diagnosis
Diagnosis is made by history and physical examination.
Occasionally, a biopsy of the lesion may be taken for histologic confirmation of HPV. Typing of the lesion may be performed at that time as well.
P.107
Complications
Cervical cancer in women may be considered a complication of HPV infection in that it most commonly results from infection with certain strains of the virus.
Infrequently, a newborn exposed to genital warts during the birth process may develop esophageal warts.
With genital warts, low self-esteem and feelings of guilt and shame may occur. Individuals who have HPV may be reluctant to establish new relationships.
Treatment
Warts go away on their own when the immune system is stimulated to recognize their presence. Such stimulation typically happens with vascularization or bleeding of the wart.
Irritation of a skin or plantar wart by the application of salicylic acid, formaldehyde, podophyllum, or other skin irritants may stimulate an immune reaction against the wart. All types of warts frequently reappear after treatment.
Liquid nitrogen, cryosurgery, or laser may be used to remove stubborn or unsightly warts, or warts on the genital or esophageal regions.
Bacterial Infections of the Skin
Impetigo
A superficial skin infection, usually caused by Staphylococcus or group A streptococcal infection, is known as impetigo. There are two types of impetigo: vesicular and bullous.
Vesicular impetigo most commonly occurs in children, presenting as pustules on the skin filled with a honey-colored fluid. The pustules burst and crust over. Vesicular impetigo is highly contagious, and easily passes from one area of the body to another and from person to person with contact.
Neonates may develop bullous impetigo from cross-contamination in the nursery. This type of impetigo is caused by Staphylococcus aureus and is highly contagious. Bullous impetigo is characterized by vesicles that burst and crust. Any area of the body may be infected.
Clinical Manifestations
Localized pustules, which burst and crust, anywhere on the body. Crusts and fluid are honey-colored.
Lesions often spread.
Diagnosis
Diagnosis is made by history and physical examination.
Bacterial culture and drug sensitivity testing is recommended.
P.108
Complications
Acute post-streptococcal glomerulonephritis (inflammation of the nephron) may occur from antibody-antigen complexes depositing in the kidney (type III hypersensitivity response). Widespread infection in an infant is possible.
Treatment
Systemic antibiotics may be administered after culture and identification of the organism. Topical antibiotics may be adequate if the lesion is small.
Sterilization of towels and frequent hand washing must be done to prevent spread on the body and to family members.
![]() ediatric Consideration
ediatric Consideration
Impetigo is a common childhood skin infection. It is highly contagious in crowded environments, such as schools and day care centers, especially if sanitary practices are poor.
Cellulitis
Cellulitis is a bacterial infection of the dermis or subcutaneous layer of the skin. Cellulitis typically occurs after a surface wound, bite, or untreated carbuncle or furuncle.
Clinical Manifestations
The skin appears swollen and red and is tender and warm to the touch. An exudate of serous or purulent fluid may be present.
Fever may be present.
Diagnosis
Diagnosis is made by history and physical examination.
Treatment
Warm soaks in an antibacterial medium or Burow's solution may be used.
Systemic antibiotics are necessary.
Folliculitis
Infection of a hair follicle, usually by the bacterium Staphylococcus aureus, is known as folliculitis. Inflammation occurs in the follicle. Risk factors include trauma to the skin and poor hygiene.
P.109
Clinical Manifestations
Surface pustules characterized by redness, pain, and swelling.
Diagnosis
Diagnosis is made by history and physical examination.
Complications
A boil, also called a furuncle, may develop if the inflamed follicle bursts and spreads the bacteria into the dermis. Pain and inflammation worsen. Oozing of pus and cellulitis may develop.
Treatment
Soap and water and topical antibiotics.
Warm compresses and incision of the lesion may be required.
Systemic antibiotics may be required.
Carbuncle
A carbuncle is a collection of hair follicles infected in the subcutaneous and dermal layers. An abscess may develop as immune cells encircle the infection.
Clinical Manifestations
A hard, firm mass under the skin that is painful and may drain purulent material.
Systemic signs of infection, including chills, fever, and malaise.
Diagnosis
Diagnosis is made by history and physical examination.
Treatment
Warm compresses and topical or systemic antibiotics. An abscess may require lancing and drainage.
Scarlet Fever
Although not a bacterial infection, scarlet fever is a skin rash caused by toxins released during infection with group A beta-hemolytic streptococci. Scarlet fever, also called scarletina, is usually associated with a pharyngeal streptococcal infection.
Clinical Manifestations
The rash of scarlet fever is usually pink, mainly over the neck, trunk, and groin, with a feeling similar to fine sandpaper.
The rash is typically accompanied by other signs of a pharyngeal streptococcal infection: sore throat, fever, headache, and nausea.
P.110
Diagnostic Tools
A throat culture is usually positive for group A beta-hemolytic streptococci. This coupled with a good history and physical examination usually confirms scarlet fever.
Complications
Post-streptococcal glomerulonephritis, rheumatic fever, and peritonsillar abscess may all follow a streptococcal infection.
Treatment
Treatment is with penicillin or, if the individual is allergic to penicillin, erythromycin or another macrolide.
Fungal Infections of the Skin
Fungal infections of the skin are considered superficial infections and are typically described based on the site of infection. The infections of the skin are called tinea (mistakenly referring to a worm). Tinea pedis is an infection of the foot (e.g., athlete's foot); tinea corporis (ringworm), an infection of the body; tinea barbae, an infection of the beard; and tinea capitis, an infection of the scalp. Tinea versicolor is a fungal infection of the body that may result in patches of discoloration that are worsened by exposure to sunlight.
Fungal infections of the mouth (thrush), gastrointestinal (GI) tract, and vagina usually are a result of the yeastlike fungus Candida albicans and are called candidiasis. C. albicans is part of the normal human flora that, under some conditions, may multiply excessively and cause symptoms.
Deep fungal infections of the respiratory tract or brain usually occur only in immunocompromised individuals and are considered opportunistic infections. Histoplasmosis is a fungal infection of the respiratory tract that may develop in normal individuals as well.
Causes of Fungal Infections
Fungal infections occur in individuals who are somehow predisposed to their development. Predisposition may exist for no obvious reason, but often individuals are predisposed as a result of their environment or behavior, for example, frequent participation in athletic events associated with perspiration and frequent showering where the fungus may be present (e.g., locker rooms). A predisposition is also present in individuals suffering from decreased immune function (e.g., diabetics, pregnant women, and young infants). Those who have severe immunodeficiency,
P.111
including those suffering from acquired immunodeficiency syndrome (AIDS), are at special risk of chronic, debilitating fungal infections. In fact, vaginal or oral yeast infections are frequently the first opportunistic infections seen in individuals infected with the human immunodeficiency virus (HIV). Persons who have chronic fungal infections should be evaluated for diabetes mellitus and HIV/AIDS.
Treatment with antibiotics for a bacterial infection may kill normal vaginal bacteria that usually exist in balance with vaginal yeast. This decrease in normal vaginal bacteria may predispose women or girls to vaginal yeast infections.
Clinical Manifestations
Skin infections cause inflammation with erythema and itching.
Ringworm may present as a ring of erythema with a pale interior. Scaling of the edges may be present.
Yeast infections may appear as inflamed pustules that itch and are painful. Vaginal infections are associated with a cheese-like white discharge. Oral infections present with multiple white ulcerations surrounded by erythema, which may be extremely painful.
Diagnosis
Fungal infections may be diagnosed by history and physical examination.
Microscopic examination of skin scrapings prepared with potassium hydroxide allows for identification of hyphae (characteristic spores and filaments of fungi) under the microscope.
Viewing the affected area with a special UV light (Wood lamp) may also allow for recognition of fungal infections, as the spores fluoresce blue-green under this lighting condition. If hyphae or spores cannot be seen, scrapings may be sent for culture to confirm or refute diagnosis. Sometimes, cultures are sent even if hyphae or spores are seen.
Complications
Surface infections may become secondarily infected by bacteria.
Deep fungal infections (internal) may cause significant morbidity and mortality.
Scarring of the skin or, with tinea capitis, alopecia (hair loss) may occur.
Painful oral lesions that interfere with eating may contribute to the wasting seen in individuals suffering from AIDS.
Treatment
Skin infections are treated with type-specific antifungal medications applied topically or occasionally given systemically. Scalp and foot infections are often treated with systemic agents.
Candidiasis is treated with antifungal cream or suppositories.
Treatment may be given to partners of women with chronic vaginal yeast infection.
Deep fungal infections may require extensive, specific antifungal therapy and hospitalization.
P.112
![]() ediatric Consideration
ediatric Consideration
Infants who have oral thrush may be asymptomatic or may nurse poorly. If a breast-feeding infant is diagnosed with thrush, both infant and mother should be treated because infection can pass back and forth between the mouth and the nipple.
Scleroderma
Scleroderma is a connective tissue disease. The disease may involve only the skin or may occur systematically and involve the kidneys, lungs, and gut. Scleroderma is autoimmune in nature and affects women more commonly than men.
Scleroderma is characterized by massive deposits of collagen under the skin or in internal organs, resulting in inflammation and fibrosis. Skin deposits are in the dermal and subdermal tissue. Calcium deposits accumulate under the skin as well. The disease may cause Raynaud's phenomenon, characterized by spasms of the arterioles of the fingers.
Clinical Manifestations
The skin appears tight, shiny, and often red from inflammation.
Fingertips and nails may be narrow or missing.
Hard, calcium nodules under the skin may be visible and palpable.
Muscular atrophy, pain, and deformity may develop.
Diagnosis
Often diagnosed by excluding other connective tissue diseases and from the history and physical examination.
Complications
A mortality rate of approximately 50% if the disease progresses to involve internal organs.
Treatment
There is no specific treatment for scleroderma. It is recommended that patients avoid exposure to cold temperature and smoking, both of which cause vasoconstriction and worsen symptoms.
Steroidal anti-inflammatory medication may be used to slow the autoimmune response.
P.113
Burns
Burns may result from exposure of the skin to high temperature, electrical shock, or chemicals. Burns are classified according to tissue depth of the burn and the extent of the body surface area that has been burned.
Depth of a Burn
A burn may be classified as superficial first-degree, superficial partial-thickness second-degree, deep partial-thickness second-degree, or full thickness third-degree.
Superficial first-degree burns are limited to the epidermis. There is erythema and pain but no immediate blistering. Healing is spontaneous and occurs within 3 to 4 days. The burn does not scar. There are usually no complications. Sunburn is an example of a first degree burn.
Superficial partial-thickness second-degree burns extend through the epidermis and into the dermal layer. The burn is extremely painful and blisters within minutes. The burn usually heals without scarring, although certain individuals, especially African-Americans, may scar after this type of burn. Healing usually requires as long as a month. Complications are uncommon, although secondary infection of the wound may occur.
Deep partial-thickness second-degree burns extend through the entire dermis. The hair follicles remain intact and regrow. This type of burn is only partially sensitive to pain because of extensive destruction of the sensory neurons. However, surrounding areas usually have painful superficial second-degree burns. Healing of a deep partial-thickness second-degree burn takes several weeks and includes surgical debridement (cleaning) to remove dead tissue. Grafting is usually required. Scar formation always occurs with this burn.
Full-thickness third-degree burns extend through the epidermis and the dermis and into the subcutaneous tissue layer. Capillaries and veins may be destroyed, and blood flow to the area may be reduced. Nerves are destroyed, so the burn itself is not painful, although surrounding areas typically show extremely painful second-degree burns. A third-degree burn may require months to heal, and surgical debridement and grafting are necessary. A third-degree burn scars, and the tissue appears leathery and hard.
Fourth-degree burns extend through muscle, bone, and internal tissues.
Extent of a Burn
The extent of a burn refers to the total body surface area (TBSA) of an individual's body that has received superficial or deep second-degree burns or full-thickness burns (it does not include first-degree burns). To determine the extent of a burn, the percentage of TBSA affected is estimated. One method for estimating the percentage of a burn is by using the rule of nines. With this method, each arm is considered 9% of the body surface area, each leg 18%,
P.114
the front and back torso each 18%, the head 9%, and the genital area 1%. The percentages of the body burned are added to give the TBSA burned. For children, the rule of nines does not accurately reflect surface area, primarily in that it underestimates the surface area of the head and overestimates the surface area of the limbs. For children, the Lund and Browder chart, which takes into account these differences, may be used instead.
The TBSA burned is especially important during the initial assessment when determining if a patient should be sent to a burn center and when calculating fluid and nutrient requirements. Based on TBSA burned, major burns are defined as those involving between 25% and 40% of the body surface area of an adult and between 15% and 25% of the surface area of a child. Burns of greater than 40% in adults or 25% in children are associated with significant mortality.
Besides considering TBSA burned and depth of burns, the overall health and age of the individual must be taken into consideration when predicting survival from any burn. Children and the elderly have increased mortality compared with middle-aged and young adults. An individual suffering from a severe burn should be transferred to a burn care facility as soon as possible.
Effects of a Major Burn
A major burn affects the metabolism and function of every cell in the body. All systems are compromised, especially the cardiovascular system. Given the dependence of every organ on adequate blood flow, alteration in cardiovascular function has wide-ranging implications for survival and recovery. Cellular changes also occur.
Cardiovascular Response to a Major Burn
Immediately following a severe burn, edema of the burned tissue and directly surrounding areas occurs. Edema of the burned tissue results from a breakdown of the capillaries and from plasma fluid and protein leaking into the interstitial space. The edema leads to increased tissue pressure, exacerbation of tissue hypoxia, and worsening damage. Cytokines, prostaglandins, leukotrienes, and histamine all are released and further increase capillary permeability. White blood cells are attracted to the area, especially neutrophils, which produce free oxygen radicals and contribute to reperfusion injury.
After several more hours, edema spreads beyond the burned tissue, as the ability of distant capillaries to act as barriers to diffusion is lost as well. This later edema of non-burned tissue appears to result from a transient increase in capillary permeability to water and protein. The loss of capillary integrity is described as a loss of capillary seal. The accumulation of fluid in the interstitial space throughout the body results in a significant decrease in circulating blood volume, causing a fall in stroke volume and blood pressure. Pulse rate increases in compensation. Irreversible shock may develop.
P.115
During the period of capillary leakage, blood viscosity increases and blood flow is sluggish. Individuals are at increased risk of clot formation. With a weakly beating heart, blood accumulates in the lungs, causing pulmonary congestion and increasing the risk of embolus formation. Decreased blood flow to the kidneys causes renal hypoxia and a significant decrease in urine output. The renin-angiotensin system is stimulated, resulting in increased salt and water retention. Because the capillaries do not contain the increased volume, additional edema develops, further increasing the risk of pulmonary congestion and pneumonia. Hypoxia of the gut causes injury to the mucus-producing cells, leading to gastric and duodenal ulcers (called Curling's ulcers). Within approximately 24 to 48 hours after a burn, the capillaries reseal and fluid is slowly reabsorbed back into the circulation. However, the effects of the loss of seal remain, and the risk of morbidity and mortality continues to be high.
Cellular Response to a Burn
In response to a major burn, cells outside the burned area may become permeable to electrolytes, causing sodium and calcium to accumulate intracellularly, and magnesium and phosphate to leak out from cells. Water diffuses into the cell and the cell swells. Injured cells burst, releasing potassium into the extracellular fluid. These changes affect the membrane potential of all cells and can lead to cardiac dysrhythmias and alterations in central nervous system function.
Immune function is inhibited by a major burn. Loss of immune function, combined with loss of the barrier function of the skin, puts an individual at high risk for infection. Decreased immune function appears to result from the release of hormones, including but not limited to cortisol. Cortisol is released with stress and is immunosuppressant at high concentrations.
Metabolic rate is significantly increased with a major burn. Hypermetabolism may result from activation of the sympathetic nervous system and the stress response, as well as from attempts to balance the heat loss that occurs when the insulatory function of the skin is lost. Healing of the burn also requires huge amounts of energy. The temperature control center in the hypothalamus is affected by the response to a major burn, leading to an increase in hypothalamic set-point. This increase may result from cytokines and other peptides released during the widespread inflammatory response. The hypermetabolism, as well as the increase in cortisol and epinephrine (hormones of the post-absorptive state) and changes in insulin sensitivity, leads to tissue breakdown and protein and fat wasting. Protein breakdown contributes to severe muscle wasting.
Clinical Manifestations
A superficial first-degree burn is characterized by redness and pain. Blisters may develop after 24 hours, and the skin may later peel.
A superficial partial-thickness second-degree burn is characterized by rapid blister formation (within minutes) and intense pain.
A deep partial-thickness second-degree burn is characterized by blisters or thin dry tissue that covers the wound and peels off. The wound may not be painful.
A full-thickness third-degree burn appears flat, thin, and dry. Coagulated blood vessels may be seen. The skin may be white, red, or black and leathery.
Electrical burns may appear similar to thermal burns, or may appear as silver, raised areas. Electrical burns usually occur at points of electrical contact. The internal damage caused by an electrical burn may be much more severe than is apparent from the external wound.
P.116
Diagnostic Tools
Diagnosis may involve only an inspection of the burn site if the burn is small and uncomplicated. However, for significant burns, the American Burn Association recommends additional evaluation. With a burn of the face or neck, or when a burn covers a large percentage of TBSA, checking the airway is essential since such burns can lead to airway edema requiring intubation. Additionally, determining the mechanism of injury and a comprehensive physical examination to look for other sites of trauma are required.
The rule of nines is used to evaluate the percentage of body surface burned in adults (over age 15). In children, the Lund and Browder chart is used to determine TBSA burned.
Urine output is followed closely during the period of burn shock and after resealing of the capillaries. This is essential for evaluating the success of volume replacement during burn shock. When urine output returns to normal, the capillaries are said to have resealed.
Depth of wound is evaluated to determine the local and surgical treatment of wounds.
Complications
Any burn may become infected, causing further disability or death. Methicillin-resistant Staphylococcus aureus is an especially frequent cause of hospital-acquired (nosocomial) infection in burn patients. Infections are the leading cause of morbidity and mortality in patients who initially survive a major burn.
Sluggish blood flow may lead to the development of a blood clot, causing a cerebral vascular accident, a myocardial infarct, or a pulmonary embolus.
Lung damage may occur from smoke inhalation or embolus formation. Pulmonary congestion may result from left-heart failure or a myocardial infarct. Adult respiratory distress syndrome may develop. The combination of smoke inhalation and a severe body burn increases mortality.
Electrolyte disturbances may lead to a cardiac dysrhythmia and cardiac arrest.
Burn shock may irreversibly damage the kidneys, leading to renal failure within the first week or two after the burn. Renal failure also may develop as a result of renal hypoxia or rhabdomyolysis (myoglobin obstruction of the kidney tubules secondary to widespread muscle necrosis).
Decreased blood flow to the gut may result in hypoxia of the mucus-producing cells, leading to peptic ulcer disease.
Disseminated intravascular coagulation (DIC) may occur with widespread tissue destruction.
With a major or disfiguring burn, psychologic trauma may lead to depression, family breakup, and thoughts of suicide. Psychological symptoms may occur any time after a burn. Symptoms may come and go repeatedly over a lifetime as patients grieve and re-grieve over the losses encountered from the burn injuries.
The financial burden to the family of an individual who has a severe burn is enormous. Not only are wages lost if the individual is an adult, but care is continuing and costly.
P.117
Treatment
Individuals experiencing a burn should immediately be removed from the burning agent, and the burned area of the skin should be immediately immersed under cool water to stop further tissue destruction. The application of ice should be avoided because ice decreases blood flow to the area and may worsen the degree of the burn. Clothes should not be removed from a serious burn, because removing clothes may also remove skin.
Edema associated with superficial or partial-thickness burns may be controlled by cold water immersion. The intravenous administration of large macromolecules, such as albumin, dextran, and starch, may improve non-burn edema, but is unlikely to improve edema of the burned tissue. Heparin may maintain blood flow in burned injuries, but may also contribute to edema.
Individuals who have a severe burn must receive medical treatment. Infants, young children, and the elderly who suffer anything other than a minor burn should be evaluated by a medical provider, as should those who have any chronic illness or condition. Burns to the hands, face, and genitals should be evaluated by medical personnel.
First-degree burns usually require only prolonged exposure to large amounts of cool water or the application of cool compresses and anti-inflammatory medication.
First-degree chemical burns should be flushed with cool water for several minutes.
Burns deeper than first-degree require antimicrobial therapy and should be evaluated by medical personnel. Application of silver-based ointment is especially effective, as silver inhibits bacterial growth. Silver is toxic, however, to keratinocytes and fibroblasts necessary for tissue healing, so risks and benefits should be weighed.
Major burns require quick intravenous fluid replacement to combat the loss of capillary seal. To maintain blood pressure and prevent irreversible shock, infusions in an adult may reach the staggering amount of 30L in 24 hours. The high rate of fluid replacement also flushes the kidney and reduces the risk of renal failure.
Early and continued nutritional support is required for severely burned individuals. Because of the hypermetabolic response to a severe burn, calories and protein must be in adequate supply to prevent muscle catabolism and wasting. Enteral feeding is optimal for those who suffer severe burns, both because of its ability to provide adequate calories for healing and because it appears to protect the gut mucosa, reducing damage to the gut barrier.
In second-degree partial-thickness burns, special dressings that support cell division and growth are applied.
Second-degree, total-thickness, and third-degree burns require near immediate debridement (surgical excision of the wound) and grafting. If possible, grafting should be from non-damaged skin of the burn patient (autograft). Other grafting sources are human donors, alive or dead (allograft), or non-human donors, usually pigs (xenograft). Cultured autografts and artificial skin grafts have been developed as well.
Tissue expansion techniques have been used to improve the chances for successful skin grafting. These techniques stimulate a stretch-induced signal transduction pathway whereby stretch increases the growth of keratinocytes and stimulates protein synthesis in skin to be used for autografts.
Pain relief and pain management are major goals of burn therapy. Burns themselves can be excruciatingly painful, as can the treatments used to help a burn to heal. Alleviating pain as much as possible reduces stress, which may improve immune function and healing. Adequate pain relief also may relieve the psychological trauma associated with burns, some of which continues long after the burn is physically healed.
P.118
![]() ediatric Consideration
ediatric Consideration
Burns are a major cause of morbidity and mortality in children. Most burns to children are preventable. Frequent sources of burns include scalds from kitchen stove spills, or hot water exposure. Because children have skin that is much thinner than that of adults, even brief exposure (less than a second) to hot water can scald a child. Fire injury from being unable to escape a burning home or car and electrical burn injuries from electrical sockets or cords also account for a substantial number of childhood burns. Children may be burned purposefully in situations of abuse. Signs of this type of burn include delays in seeking medical attention, contact burns to parts of the body such as the backs of hands or the genitals, and burns on the buttocks and legs indicative of forced immersion in hot water. Any burn is a frightening, painful experience for a child, and all possible steps should be taken to prevent a burn from occurring.
P.119
Decubitus Ulcer
Decubitus ulcers are of concern worldwide and incur costs in the billions of dollars each year. Decubitus ulcers, also called pressure sores or bed sores, are lesions on the skin that occur after the breakdown of the epidermis, the dermis, and, occasionally, the subcutaneous tissue and underlying bone. Decubitus ulcers are usually seen in individuals who are bedridden or have significantly decreased mobility, especially if these conditions are accompanied by poor nutritional status. Even if mobility is normal, those suffering a reduced sensitivity to pain (e.g., individuals who have diabetes mellitus, spinal cord injuries, or stroke) may develop an ulcer. The severity of an ulcer is based on the depth of erosion into the tissue. Even ulcers that look small on the surface of the skin may be associated with significant injury under the skin. Clinically, the designation decubitus ulcer includes any skin area with blanching erythema, non-blanching erythema, decubitus dermatitis, an ulcer at any stage of healing, or gangrene. See page C2 for illustrations and staging of decubitus ulcers.
There are four forces that together produce a decubitus ulcer: pressure, shearing, friction, and moisture. A decubitus ulcer usually forms on an area of the skin overlying a bony process. It develops when the pressure in that area goes unrelieved for a long period, causing collapse of the supplying blood vessels. This collapse leads to tissue hypoxia and cellular death. Decubitus ulcers are common on skin areas exposed to sliding or shear forces, where there is a high degree of friction between the skin and the surface, and on skin exposed for prolonged periods to the moisture of urine or feces, which further breaks down the skin and makes it susceptible to infection.
Clinical Manifestations
A sign of early injury is an area of redness that does not disappear with fingertip pressure (non-blanching). An ulcer (erosion) on the skin is seen with more severe injury. A visible skin lesion may be partial or full thickness, extending through the dermis or even through the subcutaneous tissue. A full-thickness injury may damage the bone.
Pain and systemic signs of inflammation, including fever and increased white blood cell count, may develop.
Diagnosis
Decubitus ulcers are diagnosed with the help of a good history and physical examination. Individuals at high risk should be checked frequently for an early stage of ulcer development. Early stage is suggested by skin that remains blanched with pressure for more than a brief period.
Complications
Infection leading to prolonged disability and hospitalization may occur with even small ulcers.
P.120
Treatment
Prevention of a decubitus ulcer is essential and involves turning bedridden individuals frequently (at least every 2 hours). Caloric intake should be kept high to assist in immune function and to maintain overall general good health.
If a pressure sore does develop, relief of the pressure on the skin and the placement of a clean, flat, non-bulky dressing are required.
Skin Cancer
Skin cancer is the most common form of cancer in the United States, with over a million cases diagnosed each year. The incidence of skin cancer varies geographically, peaking at high altitude and in sunny regions of the country. Skin cancer is more common in light-skinned individuals than it is in dark-skinned individuals, although individuals from all races are at risk. There are three types of skin cancer: basal cell, squamous cell, and malignant melanoma (Table 4-2). All types of skin cancer are increasing in incidence and developing in individuals at younger ages. These increases
P.121
are most likely because of the increase in recreational sun exposure over the last several decades.
Table 4-2. Skin Cancer | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Basal Cell Carcinoma
Basal cell carcinoma is a superficial cancer of immature epithelial cells. The tumors typically are slow growing and seldom metastasize, although they can cause localized tissue destruction. Basal cell carcinoma is the most common type of skin cancer and is caused by cumulative exposure to ultraviolet (UV) radiation from sunlight. Genetic factors are involved as well.
Squamous Cell Carcinoma
Squamous cell carcinoma is a cancer of the epidermal cells that may spread horizontally over the skin or vertically into the dermis. Spread may be slow or aggressive. Squamous cell carcinoma may metastasize to other sites of the body. Squamous cell cancer is most common in the elderly and develops after prolonged exposure to the sun. It frequently develops on areas of the skin demonstrating precancerous lesions or irregularities, such as keratosis (a horny growth), actinic dermatitis, or areas of previous discoloration. Squamous cell carcinoma may also develop at the site of a previous scar (e.g., a burn scar). The use of immunosuppressive drugs predisposes transplant patients to squamous cell carcinoma due to drug-induced sensitivity to UVA and UVB radiation. The risk for squamous cell carcinoma is highest in sunny climates, with Australia having the highest rates of squamous cell carcinoma in the world.
Malignant Melanoma
Malignant melanoma is an aggressive tumor of the melanin-producing cells at the base of the epidermis. Malignant melanoma may develop at the site of a pre-existing nevus (mole) or may develop spontaneously on the skin. This type of skin cancer often develops during middle age or older, and appears to result from intense burns with blistering at any time in life. Other risk factors include light skin, freckles, and fair-colored hair. Malignant melanoma represents 4% of skin cancers but 79% of cancer deaths.
Research suggests melanoma occurs from a radiation-induced decrease in the functioning of the skin's immune cells, the Langerhans' cells. This makes the cells of the skin less able to identify and repair DNA damage, thus increasing the risk of carcinogenesis. A genetic predisposition for melanoma is likely with gene studies underway. Metastasis is common. The incidence of melanoma is increasing, especially among the young.
Clinical Manifestations
Basal cell carcinoma usually appears on sun-exposed areas of the body, including the face, arms, and chest. Lesions may appear as dome-shaped papules or nodules, well circumscribed, with a pearly white
P.122
color, as in the case of classic nodular basal cell carcinoma, or as scaly reddened patches or plaques (superficial basal cell carcinoma). The lesions are painless.Squamous cell carcinoma usually occurs on sun-exposed areas of the body or on scarred tissue. The lesions appear as scaly red plaques or raised nodules with central necrosis.
Malignant melanoma may appear as a multicolored nodule growing vertically or as a circular spread of pigmentation larger than 1 cm. Borders of either lesion are irregular and often asymmetric, and bleeding may occur. Melanoma may develop on sun-exposed areas, or on the palms of the hands, the soles of the feet, or the oral or vaginal mucosa.
Diagnosis
Skin cancer diagnosis is made as a result of a physical examination followed by the excision and biopsy of a suspicious lesion. Any lesion should be considered suspicious if it demonstrates one of the ABCDs of skin cancer: Asymmetry, irregular Border, a change in Color, or an increasing Diameter such that the lesion is greater than 0.5 cm (approximately the size of a pencil eraser).
Complications
Local invasion and destruction of tissue may occur with any type of skin cancer.
Metastasis to regional lymph nodes and throughout the body may occur, especially with malignant melanoma. Basal cell carcinoma has very low risk for metastasis, while squamous cell carcinoma demonstrates intermediate risk.
Treatment
Prevention of basal and squamous cell carcinoma is possible with rigorous protection from the sun, including avoidance of the sun at peak hours and the use of hats, protective clothing, and broad-spectrum sunscreen.
Individuals can reduce the incidence of malignant melanoma by avoiding sun exposure and by wearing protective clothing. Individuals should avoid or limit the use of indoor tanning beds, as research suggests a strong association between indoor tanning and melanoma. Sunscreen may not protect against the development of malignant melanoma.
Basal cell carcinoma usually is surgically excised. Prognosis is good.
Squamous cell carcinoma is surgically excised and radiation therapy may be required. Prognosis is good, especially if metastasis has not occurred.
Malignant melanoma is surgically excised, along with a margin of surrounding tissue. Lymph node biopsy is performed to determine if metastasis has occurred. Sentinel lymph node biopsy, i.e., biopsy of the
P.123
node closest to the malignancy, has been shown to be an effective predictor of metastasis and a means of directing therapy. Prognosis depends on the size of the lesion and the outcome of the lymph node biopsy. Nodular growth has a worse prognosis.Chemotherapy and immunotherapy both may be required in addition to surgery for malignant melanoma and sometimes squamous cell carcinoma.
Tumor vaccines active against specific antigens in malignant melanoma are being used in selected patients. Gene therapy for malignant melanoma is also being studied.
Selected Bibliography
Abdulla, F.R., Feldman, S.R., Williford, P.M., Krowchuk, D., & Kaur, M. (2005). Tanning and skin cancer. Pediatric Dermatology 22, 501 512.
Atiyeh, B.S., Gunn, S.W., & Hayek, S.N. (2005). State of the art in burn treatment. World Journal of Surgery 29, 131 148.
Bansal, C., Scott, R., Stewart, D., & Cockerell, C.J. (2005). Decubitus ulcers: A review of the literature. International Journal of Dermatology 44, 805 810.
Bates, B. (2002). Visual guide to physical examination. Philadelphia: J. B. Lippincott Company.
Demling, R.H. (2005). The burn edema process: Current concepts. Journal of Burn Care Rehabilitation 26, 207 227.
Gottlieb, A.B. (2005). Psoriasis: Emerging therapeutic strategies. Nature Reviews Drug Discovery 4, 19 34.
Guyton, A.C., & Hall, J. (2006). Textbook of medical physiology (11th ed.). Philadelphia: W.B. Saunders.
Madariaga, M.G., Naldi, L., Chatenoud, L., Khan, S., Schon, M.P., & Boehncke, W.H. (2005). Psoriasis. New England Journal of Medicine 353, 848 850.
Magin, P., Pond, D., Smith, W., & Watson, A. (2005). A systematic review of the evidence for myths and misconceptions in acne management: diet, face washing and sunlight. Family Practice 22, 62 70.
Murase, J.E., Lee, E.E., & Koo, J. (2005). Effect of ethnicity on the risk of developing nonmelanoma skin cancer following long-term PUVA therapy. International Journal of Dermatology 44, 1016 1021.
Parrish, J.A. (2005). Immunosuppression, skin cancer, and ultraviolet A radiation. New England Journal of Medicine 353, 2712 2713.
Porth, C.M. (2005). Pathophysiology: Concepts of altered health states (7th ed.). Philadelphia: Lippincott Williams & Wilkins.
Rigel, D.S., Friedman, R.J., Dzubow, L.M., Reintgen, D.S., Bystryn, J.-C., & Marks, R. (2005). Cancer of the skin. W.B. Saunders: Philadelphia.
Rubin, A.I., Chen, E.H., & Ratner, D. (2005). Basal-cell carcinoma. New England Journal of Medicine 353, 2262 2269.
Schon, M.P., & Boehncke, W.-H. (2005). Psoriasis. New England Journal of Medicine 352, 1899 1912.
Sheridan, R. (2005). Outpatient burn care in the emergency department. Pediatric Emergency Care 21, 449 456.
EAN: 2147483647
Pages: 26