Drugs Used in Psychiatry
Authors: Sadock, Benjamin James; Sadock, Virginia Alcott
Title: Kaplan & Sadock's Synopsis of Psychiatry: Behavioral Sciences/Clinical Psychiatry, 10th Edition
Copyright 2007 Lippincott Williams & Wilkins
> Front of Book > Drugs Used in Psychiatry
Drugs Used in Psychiatry
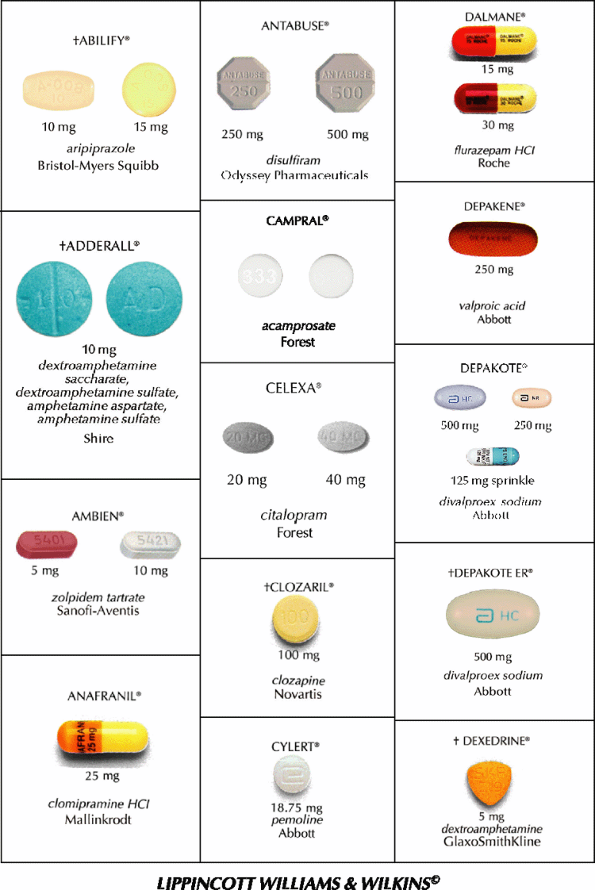
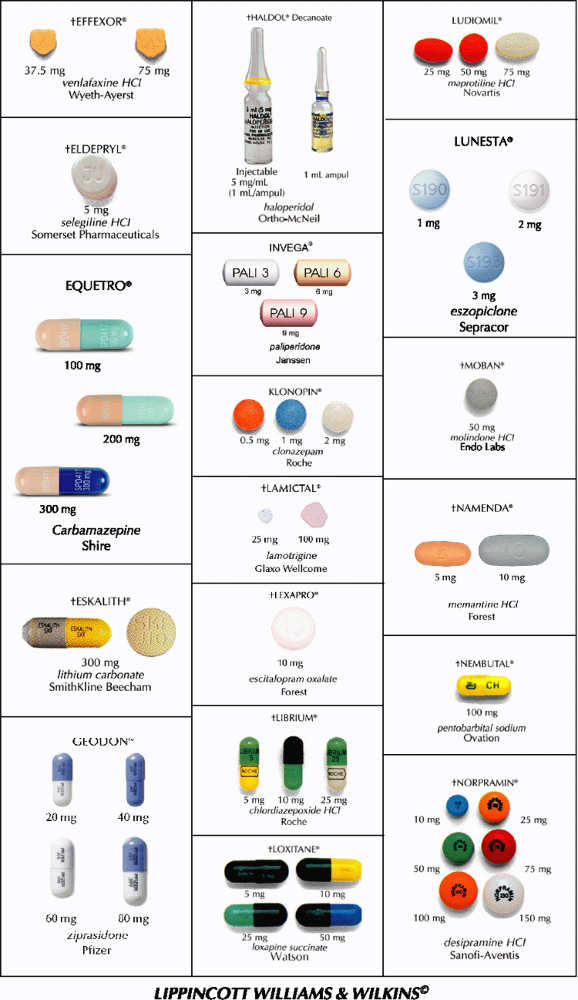
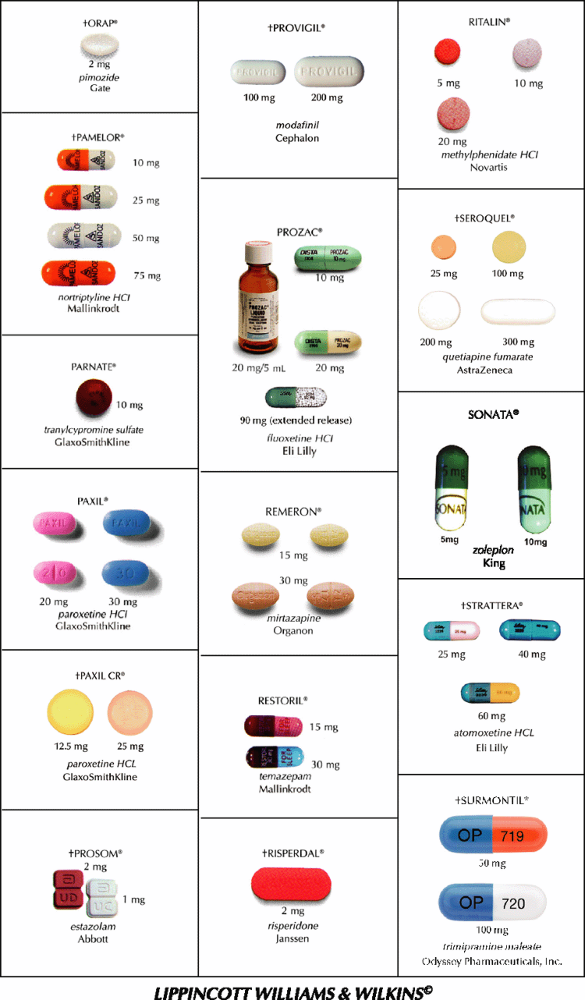
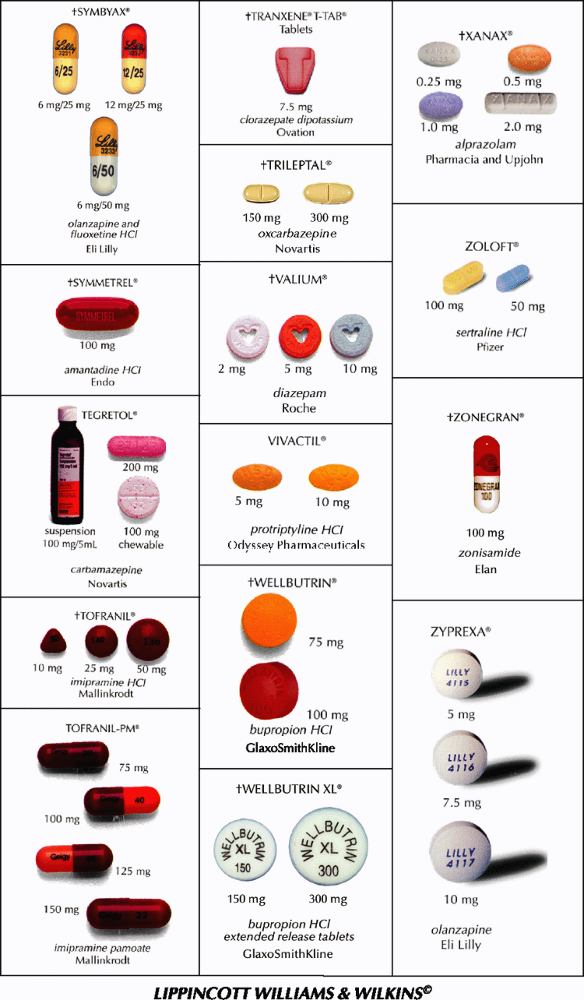
This guide contains color reproductions of some commonly prescribed psychotherapeutic drugs. This guide illustrates proprietary forms of tablets and capsules. A symbol preceding the name of a drug indicates that other doses are available. Check directly with the manufacturer. (Although the photos are intended as accurate reproductions of the drug, this guide should be used only as a quick identification aid.)
 |
 |
 |
 |
Kaplan and Sadocks Synopsis of Psychiatry: Behavioral Sciences/Clinical Psychiatry
ISBN: 078177327X
EAN: 2147483647
EAN: 2147483647
Year: 2007
Pages: 75
Pages: 75
Authors: Benjamin J. Sadock, Virginia A. Sadock