21 - Fluid Electrolyte Disorders
Editors: McPhee, Stephen J.; Papadakis, Maxine A.; Tierney, Lawrence M.
Title: Current Medical Diagnosis & Treatment, 46th Edition
Copyright 2007 McGraw-Hill
> Table of Contents > 24 - Nervous System
function show_scrollbar() {}
24
Nervous System
Michael J. Aminoff MD, DSc, FRCP
Headache
Headache is such a common complaint and can occur for so many different reasons that its proper evaluation may be difficult. Headaches of acute onset are discussed in Chapter 2. Chronic headaches are commonly due to migraine, tension, or depression, but they may be related to intracranial lesions, head injury, cervical spondylosis, dental or ocular disease, temporomandibular joint dysfunction, sinusitis, hypertension, and a wide variety of general medical disorders. Although underlying structural lesions are not present in most patients presenting with headache, it is nevertheless important to bear this possibility in mind. About one-third of patients with brain tumors, for example, present with a primary complaint of headache.
The intensity, quality, and site of pain and especially the duration of the headache and the presence of associated neurologic symptoms may provide clues to the underlying cause. Migraine or tension headaches are often described as pulsating or throbbing; a sense of tightness or pressure is also common with tension headache. Sharp lancinating pain suggests a neuritic cause; ocular or periorbital icepick-like pains occur with migraine or cluster headache; and a dull or steady headache is typical of an intracranial mass lesion. Ocular or periocular pain suggests an ophthalmologic disorder; band-like pain is common with tension headaches; and lateralized headache is common with migraine or cluster headache. In patients with sinusitis, there may be tenderness of overlying skin and bone. With intracranial mass lesions, headache may be focal or generalized; in patients with trigeminal or glossopharyngeal neuralgia, the pain is localized to one of the divisions of the trigeminal nerve or to the pharynx and external auditory meatus, respectively.
Inquiry should be made of precipitating factors. Recent sinusitis or hay fever, dental surgery, head injury, or symptoms suggestive of a systemic viral infection may suggest the underlying cause. Migraine may be exacerbated by emotional stress, fatigue, foods containing nitrite or tyramine, or the menstrual period. Alcohol may precipitate cluster headache. Temporomandibular joint dysfunction causes headache or facial pain that comes on with chewing; trigeminal or glossopharyngeal neuralgia may also be precipitated by chewing, and masticatory claudication sometimes occurs with giant cell arteritis. Cough-induced headache occurs with structural lesions of the posterior fossa, but in many instances no specific cause can be found.
The timing of symptoms is important. Headaches are typically worse on awakening in patients with sinusitis or an intracranial mass. Cluster headaches tend to occur at the same time each day or night. Tension headaches are worse with stress or at the end of the day.
The onset of severe headache in a previously well patient is more likely than chronic headache to relate to an intracranial disorder such as subarachnoid hemorrhage or meningitis. The need for further investigation is determined by the initial clinical impression.
A progressive headache disorder, new onset of headache in middle or later life, headaches that disturb sleep or are related to exertion, and headaches that are associated with neurologic symptoms or a focal neurologic deficit usually require cranial MRI or CT scan to exclude an intracranial mass lesion. Signs of meningeal irritation and impairment of consciousness also indicate the need for further investigation (cranial CT scan or MRI and examination of the cerebrospinal fluid) to exclude subarachnoid hemorrhage or meningeal infection. The diagnosis and treatment of primary neurologic disorders associated with headache are considered separately under these disorders.
1. Tension Headache
Patients frequently complain of poor concentration and other vague nonspecific symptoms, in addition to constant daily headaches that are often vise-like or tight in quality and may be exacerbated by emotional stress, fatigue, noise, or glare. The headaches are usually generalized, may be most intense about the neck or back of the head, and are not associated with focal neurologic symptoms.
When treatment with simple analgesics is not effective, a trial of antimigrainous agents (see Migraine, below) is worthwhile. Techniques to induce relaxation are also useful and include massage, hot baths, and biofeedback. Exploration of underlying causes of chronic anxiety is often rewarding. Local injection of botulinum toxin type A is sometimes helpful, has few systemic adverse effects, and requires only infrequent administration.
2. Depression Headache
Depression headaches are frequently worse on arising in the morning and may be accompanied by other symptoms of depression. Headaches are occasionally the focus
P.999
of a somatic delusional system. Antidepressant drugs are often helpful, as may be psychiatric consultation.
3. Migraine
![]() Essentials of Diagnosis
Essentials of Diagnosis
Headache, usually pulsatile.
Nausea, vomiting, photophobia, and phonophobia are common accompaniments.
May be transient neurologic symptoms (commonly visual) preceding headache of classic migraine.
No preceding aura is common.
General Considerations
The pathophysiology of migraine probably relates to the neurotransmitter serotonin. Headache may result from release of neuropeptides acting as neurotransmitters at trigeminal nerve branches, leading to an inflammatory process; another possible mechanism involves activation of the dorsal raphe nucleus.
Clinical Findings
Classic migrainous headache is a lateralized throbbing headache that occurs episodically following its onset in adolescence or early adult life, although not all headaches that are throbbing in character are of migrainous origin. Moreover, in many cases the headaches do not conform to this pattern, although their associated features and response to antimigrainous preparations nevertheless suggest that they have a similar basis. In this broader sense, migrainous headaches may be lateralized or generalized, may be dull or throbbing, and are sometimes associated with anorexia, nausea, vomiting, photophobia, phonophobia, and blurring of vision. They usually build up gradually and may last for several hours or longer. They have been related to dilation and excessive pulsation of branches of the external carotid artery. Focal disturbances of neurologic function may precede or accompany the headaches and have been attributed to constriction of branches of the internal carotid artery. Visual disturbances occur quite commonly and may consist of field defects; of luminous visual hallucinations such as stars, sparks, unformed light flashes (photopsia), geometric patterns, or zigzags of light; or of some combination of field defects and luminous hallucinations (scintillating scotomas). Other focal disturbances such as aphasia or numbness, tingling, clumsiness, or weakness in a circumscribed distribution may also occur.
Patients often give a family history of migraine. Attacks may be triggered by emotional or physical stress, lack or excess of sleep, missed meals, specific foods (eg, chocolate), alcoholic beverages, menstruation, or use of oral contraceptives.
An uncommon variant is basilar artery migraine, in which blindness or visual disturbances throughout both visual fields are initially accompanied or followed by dysarthria, disequilibrium, tinnitus, and perioral and distal paresthesias and are sometimes followed by transient loss or impairment of consciousness or by a confusional state. This, in turn, is followed by a throbbing (usually occipital) headache, often with nausea and vomiting.
In ophthalmoplegic migraine, lateralized pain often about the eye is accompanied by nausea, vomiting, and diplopia due to transient external ophthalmoplegia. The ophthalmoplegia is due to third nerve palsy, sometimes with accompanying sixth nerve involvement, and may outlast the orbital pain by several days or even weeks. The ophthalmic division of the fifth nerve has also been affected in some patients. Ophthalmoplegic migraine is rare; more common causes of a painful ophthalmoplegia are internal carotid artery aneurysms and diabetes.
In rare instances, the neurologic or somatic disturbance accompanying typical migrainous headaches becomes the sole manifestation of an attack ( migraine equivalent ). Very rarely, the patient may be left with a permanent neurologic deficit following a migrainous attack.
Treatment
Management of migraine consists of avoidance of any precipitating factors, together with prophylactic or symptomatic pharmacologic treatment if necessary.
A. Symptomatic Therapy
During acute attacks, many patients find it helpful to rest in a quiet, darkened room until symptoms subside. A simple analgesic (eg, aspirin, acetaminophen, ibuprofen, or naproxen) taken right away often provides relief, but treatment with extracranial vasoconstrictors or other drugs is sometimes necessary. Cafergot, a combination of ergotamine tartrate (1 mg) and caffeine (100 mg), is often particularly helpful; one or two tablets are taken at the onset of headache or warning symptoms, followed by one tablet every 30 minutes, if necessary, up to six tablets per attack and ten tablets per week. Because of impaired absorption or vomiting during acute attacks, oral medication sometimes fails to help. Cafergot given rectally as suppositories (one-half to one suppository containing 2 mg of ergotamine) or dihydroergotamine mesylate (0.5 1 mg intravenously or 1 2 mg subcutaneously or intramuscularly) may be useful in such cases. Alternatively, prochlorperazine administered rectally (25 mg suppository) or intravenously (10 mg) may be prescribed. Ergotamine-containing preparations may affect the gravid uterus and thus should be avoided during pregnancy. Sumatriptan, which has a high affinity for serotonin1 receptors, is a rapidly effective agent for aborting attacks when given subcutaneously
P.1000
by an autoinjection device. It can also be taken in a nasal form, but absorption is limited, and an oral preparation is available. Zolmitriptan, another selective serotonin1 receptor agonist, has high bioavailability after oral administration and is also effective for the acute treatment of migraine. The optimal initial dose is 5 mg, and relief usually occurs within 1 hour. A newly developed nasal formulation has a rapid onset of action. A number of other triptans are available, including rizatriptan, naratriptan, almotriptan, frovatriptan, and eletriptan. Eletriptan (up to 80 mg over 24 hours) is useful for acute therapy and frovatriptan, which has a longer half-life, may be worthwhile for patients with prolonged attacks (up to 7.5 mg over 24 hours). Triptans should probably be avoided in pregnancy, are contraindicated in patients with coronary or peripheral vascular disease, and may cause nausea or vomiting. The neuroleptic droperidol is also helpful in aborting acute attacks. Metoclopramide given intravenously may be helpful and is being studied. Narcotic analgesics are needed in rare instances, such as meperidine (100 mg intramuscularly) or butorphanol tartrate by nasal spray (1 mg/spray in one nostril, repeated after 3 or 4 hours if necessary). Intravenous propofol in subanesthetic doses may help in intractable cases.
B. Prophylactic Therapy
Prophylactic treatment may be necessary if migrainous headaches occur more frequently than two or three times a month. Some of the more common drugs used for this purpose are listed in Table 24-1. Their mode of action is unclear and may involve both an effect on extracerebral vasculature and a cerebral effect, eg, by stabilizing serotonergic neurotransmission. Several drugs may have to be tried in turn before the headaches are brought under control. Once a drug has been found to help, it should be continued for several months. If the patient remains headache-free, the dose can then be tapered and the drug eventually withdrawn. Botulinum toxin type A is also effective for migraine prevention in some patients; it has few systemic side effects and need only be given at intervals of several months. Although acupuncture has been widely used in the prophylaxis of migraine, a randomized controlled trial failed to show any difference between it and sham acupuncture.
Calcium channel antagonist drugs may decrease the frequency of attacks after an interval of several weeks, but the severity and duration of attacks are not influenced. They should not be used with -blockers. The angiotensin-converting enzyme receptor blocker, candesartan, may also be effective and is undergoing evaluation.
4. Cluster Headache (Migrainous Neuralgia)
Cluster headache affects predominantly middle-aged men. Its cause is unclear but may relate to a vascular headache disorder or a disturbance of serotonergic mechanisms. Activation of cells in the ipsilateral hypothalamus has been shown to occur. There is often no family history of headache or migraine. Episodes of severe unilateral periorbital pain occur daily for several weeks and are often accompanied by one or more of the following: ipsilateral nasal congestion, rhinorrhea, lacrimation, redness of the eye, and Horner's syndrome. Episodes often occur at night, awaken the patient, and last for less than 2 hours. Spontaneous remission then occurs, and the patient remains well for weeks or months before another bout of closely spaced attacks occurs. During a bout, many patients report that alcohol triggers an attack; others report that stress, glare, or ingestion of specific foods occasionally precipitates attacks. In occasional patients, typical attacks of pain and associated symptoms recur at intervals without remission. This variant has been referred to as chronic cluster headache.
Table 24-1. Prophylactic treatment of migraine. | ||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||
P.1001
Examination reveals no abnormality apart from Horner's syndrome that either occurs transiently during an attack or, in longstanding cases, remains as a residual deficit between attacks.
Treatment of an individual attack with oral drugs is generally unsatisfactory, but subcutaneous sumatriptan (6 mg) or dihydroergotamine (1 2 mg) or inhalation of 100% oxygen (7 L/min for 15 minutes) may be effective. Butorphanol tartrate, a synthetic opioid agonist-antagonist, may also be helpful when administered by nasal spray. The dose is 1 mg (one spray in one nostril), repeated after 60 90 minutes if necessary. Ergotamine tartrate is an effective prophylactic and can be given as rectal suppositories (0.5 1 mg at night or twice daily), by mouth (2 mg daily), or by subcutaneous injection (0.25 mg three times daily for 5 days per week). Various prophylactic agents that have been found to be effective in individual patients are valproate, cyproheptadine, lithium carbonate (monitored by plasma lithium determination), prednisone (20 40 mg daily or on alternate days for 2 weeks, followed by gradual withdrawal), and verapamil (240 480 mg daily).
5. Posttraumatic Headache
A variety of nonspecific symptoms may follow closed head injury, regardless of whether consciousness is lost. Headache is often a conspicuous feature. Some authorities believe that psychological factors may be important because there is no correlation of severity of the injury with neurologic signs.
The headache itself usually appears within a day or so following injury, may worsen over the ensuing weeks, and then gradually subsides. It is usually a constant dull ache, with superimposed throbbing that may be localized, lateralized, or generalized. It is sometimes accompanied by nausea, vomiting, or scintillating scotomas.
Disequilibrium, sometimes with a rotatory component, may also occur and is often enhanced by postural change or head movement. Impaired memory, poor concentration, emotional instability, and increased irritability are other common complaints and occasionally are the sole manifestations of the syndrome. The duration of symptoms relates in part to the severity of the original injury, but even trivial injuries are sometimes followed by symptoms that persist for months.
Special investigations are usually not helpful. The electroencephalogram may show minor nonspecific changes, while the electronystagmogram sometimes suggests either peripheral or central vestibulopathy. CT scans or MRI of the head usually show no abnormal findings.
Treatment is difficult, but optimistic encouragement and graduated rehabilitation, depending on the occupational circumstances, are advised. Headaches often respond to simple analgesics, but severe headaches may necessitate treatment with amitriptyline, propranolol, or ergot derivatives.
6. Cough Headache
Severe head pain may be produced by coughing (and by straining, sneezing, and laughing) but, fortunately, usually lasts for only a few minutes or less. The pathophysiologic basis of the complaint is not known, and often there is no underlying structural lesion. However, intracranial lesions, usually in the posterior fossa (eg, Arnold-Chiari malformation), are present in about 10% of cases, and brain tumors or other space-occupying lesions may certainly present in this way. Accordingly, CT scanning or MRI should be undertaken in all patients and repeated annually for several years, since a small structural lesion may not show up initially.
The disorder is usually self-limited, although it may persist for several years. For unknown reasons, symptoms sometimes clear completely after lumbar puncture. Indomethacin (75 150 mg daily) may provide relief.
7. Headache Due to Giant Cell (Temporal or Cranial) Arteritis
The superficial temporal, vertebral, ophthalmic, and posterior ciliary arteries are often the most severely affected pathologically. Most patients are elderly. The major symptom is headache, often associated with or preceded by myalgia, malaise, anorexia, weight loss, and other nonspecific complaints. Loss of vision is the most feared manifestation and occurs quite commonly. Clinical examination often reveals tenderness of the scalp and over the temporal arteries. Further details, including approaches to treatment, are given in Chapter 20.
8. Headache Due to Intracranial Mass Lesions
Intracranial mass lesions of all types may cause headache owing to displacement of vascular structures. Posterior fossa tumors often cause occipital pain, and supratentorial lesions lead to bifrontal headache, but such findings are too inconsistent to be of value in attempts at localizing a pathologic process. The headaches are nonspecific in character and may vary in severity from mild to severe. They may be worsened by exertion or postural change and may be associated with nausea and vomiting, but this is true of migraine also. Headaches are also a feature of pseudotumor cerebri (see below). Signs of focal or diffuse cerebral dysfunction or of increased intracranial pressure will indicate the need for further investigation. Similarly, a progressive headache disorder or the new onset of
P.1002
headaches in middle or later life merits investigation if no cause is apparent.
9. Headache Due to Other Neurologic Causes
Cerebrovascular disease may be associated with headache, but the mechanism is unclear. Headache may occur with internal carotid artery occlusion or carotid dissection and after carotid endarterectomy. Diagnosis is facilitated by the clinical accompaniments and the circumstances in which the headache developed.
Acute severe headache accompanies subarachnoid hemorrhage and meningeal infections; accompanying signs of meningeal irritation and impairment of consciousness indicate the need for further investigations.
Dull or throbbing headache is a frequent sequela of lumbar puncture and may last for several days. It is aggravated by the erect posture and alleviated by recumbency. The exact mechanism is unclear, but it is commonly attributed to leakage of cerebrospinal fluid through the dural puncture site. Its incidence may be reduced if a small-diameter needle is used for the spinal tap, and perhaps also if the patient lies prone or supine after the procedure.
Ashkenazi A et al: The evolving management of migraine. Curr Opin Neurol 2003;16:341.
Friedman BW et al: A trial of metoclopramide vs. sumatriptan for the emergency department treatment of migraines. Neurology 2005;64:463.
Kaniecki R: Headache assessment and management. JAMA 2003; 289:1430.
Linde K et al: Acupuncture for patients with migraine: a randomized controlled trial. JAMA 2005;293:2118.
May A: Cluster headache: pathogenesis, diagnosis, and management. Lancet 2005;366:843.
Parmet S et al: JAMA patient page. Headaches. JAMA 2003;289: 1462.
Schoenen J et al: Headache with focal neurological signs or symptoms: a complicated differential diagnosis. Lancet Neurol 2004;3:237.
Facial Pain
1. Trigeminal Neuralgia
![]() Essentials of Diagnosis
Essentials of Diagnosis
Brief episodes of stabbing facial pain.
Pain is in the territory of the second and third division of the trigeminal nerve.
Pain exacerbated by touch.
General Considerations
Trigeminal neuralgia ( tic douloureux ) is most common in middle and later life. It affects women more frequently than men.
Clinical Findings
Momentary episodes of sudden lancinating facial pain occur and commonly arise near one side of the mouth and shoot toward the ear, eye, or nostril on that side. The pain may be triggered or precipitated by such factors as touch, movement, drafts, and eating. Indeed, in order to lessen the likelihood of triggering further attacks, many patients try to hold the face still while talking. Spontaneous remissions for several months or longer may occur. As the disorder progresses, however, the episodes of pain become more frequent, remissions become shorter and less common, and a dull ache may persist between the episodes of stabbing pain. Symptoms remain confined to the distribution of the trigeminal nerve (usually the second or third division) on one side only.
Differential Diagnosis
The characteristic features of the pain in trigeminal neuralgia usually distinguish it from other causes of facial pain. Neurologic examination shows no abnormality except in a few patients in whom trigeminal neuralgia is symptomatic of some underlying lesion, such as multiple sclerosis or a brainstem neoplasm, in which case the finding will depend on the nature and site of the lesion. Similarly, CT scans and radiologic contrast studies are normal in patients with classic trigeminal neuralgia.
In a young patient presenting with trigeminal neuralgia, multiple sclerosis must be suspected even if there are no other neurologic signs. In such circumstances, findings on evoked potential testing and examination of cerebrospinal fluid may be corroborative. When the facial pain is due to a posterior fossa tumor, CT scanning and MRI generally reveal the lesion.
Treatment
The drugs most helpful for treatment are oxcarbazepine (although not approved by the US Food and Drug Administration [FDA] for this indication) or carbamazepine, with monitoring by serial blood counts and liver function tests. If these medications are ineffective or cannot be tolerated, phenytoin should be tried. (Doses and side effects of these drugs are shown in Table 24-3). Baclofen (10 20 mg three or four times daily) may also be helpful, either alone or in combination with one of these other agents. Gabapentin may also relieve pain, especially in patients who do not respond to conventional medical therapy and those with multiple sclerosis. Depending on response and tolerance, up to 2400 mg/d is given in divided doses.
In the past, alcohol injection of the affected nerve, rhizotomy, or tractotomy was recommended if pharmacologic treatment was unsuccessful. More recently, however, posterior fossa exploration has frequently revealed some structural cause for the neuralgia (despite normal findings on CT scans, MRI, or arteriograms), such as an anomalous artery or vein impinging on the
P.1003
trigeminal nerve root. In such cases, simple decompression and separation of the anomalous vessel from the nerve root produce lasting relief of symptoms. In elderly patients with a limited life expectancy, radiofrequency rhizotomy is sometimes preferred because it is easy to perform, has few complications, and provides symptomatic relief for a period of time. Gamma radiosurgery to the trigeminal root is another noninvasive approach that appears to be successful in 80% of patients, with essentially no side effects other than facial paresthesias in a few instances. Surgical exploration generally reveals no abnormality and is inappropriate in patients with trigeminal neuralgia due to multiple sclerosis.
Liu JK et al: Treatment of trigeminal neuralgia. Neurosurg Clin North Am 2004;15:319.
Rozen TD: Trigeminal neuralgia and glossopharyngeal neuralgia. Neurol Clin 2004;22:185.
2. Atypical Facial Pain
Facial pain without the typical features of trigeminal neuralgia is generally a constant, often burning pain that may have a restricted distribution at its onset but soon spreads to the rest of the face on the affected side and sometimes involves the other side, the neck, or the back of the head as well. The disorder is especially common in middle-aged women, many of them depressed, but it is not clear whether depression is the cause of or a reaction to the pain. Simple analgesics should be given a trial, as should tricyclic antidepressants, carbamazepine, oxcarbazepine, and phenytoin; the response is often disappointing. Opioid analgesics pose a danger of addiction in patients with this disorder. Attempts at surgical treatment are not indicated.
3. Glossopharyngeal Neuralgia
Glossopharyngeal neuralgia is an uncommon disorder in which pain similar in quality to that in trigeminal neuralgia occurs in the throat, about the tonsillar fossa, and sometimes deep in the ear and at the back of the tongue. The pain may be precipitated by swallowing, chewing, talking, or yawning and is sometimes accompanied by syncope. In most instances, no underlying structural abnormality is present; multiple sclerosis is sometimes responsible. Oxcarbazepine and carbamazepine (see Table 24-3) are the treatments of choice and should be tried before any surgical procedures are considered. Microvascular decompression is generally preferred over destructive surgical procedures such as partial rhizotomy in medically refractory cases and is often effective without causing severe complications.
4. Postherpetic Neuralgia
Herpes zoster (shingles) is due to infection of the nervous system by varicella-zoster virus. About 15% of patients who develop shingles suffer from postherpetic neuralgia. This complication seems especially likely to occur in the elderly, when the rash is severe, and when the first division of the trigeminal nerve is affected. A history of shingles and the presence of cutaneous scarring resulting from shingles aid in the diagnosis. Severe pain with shingles correlates with the intensity of postherpetic symptoms.
The incidence of postherpetic neuralgia may be reduced by the treatment of shingles with oral acyclovir or famciclovir, but this is disputed; systemic corticosteroids do not help. Zoster vaccine markedly reduces morbidity from herpes zoster and postherpetic neuralgia among older adults. Management of the established complication is essentially medical. If simple analgesics fail to help, a trial of a tricyclic antidepressant (eg, amitriptyline, up to 100 150 mg/d) in conjunction with a phenothiazine (eg, perphenazine, 2 8 mg/d) is often effective. Other patients respond to carbamazepine (up to 1200 mg/d), phenytoin (300 mg/d), gabapentin (up to 3600 mg/d), or pregabalin (up to 300 mg/d). A combination of gabapentin and morphine taken orally may provide better analgesia at lower doses of each agent than either taken alone. Topical application of capsaicin cream (eg, Zostrix, 0.025%) is sometimes helpful, perhaps because of depletion of pain-mediating peptides from peripheral sensory neurons, and topical lidocaine (5%) is also worthy of trial.
Gilron I et al: Morphine, gabapentin, or their combination for neuropathic pain. N Engl J Med 2005;352:1324.
Johnson RW et al: Treatment of herpes zoster and postherpetic neuralgia. BMJ 2003;326:748.
5. Facial Pain Due to Other Causes
Facial pain may be caused by temporomandibular joint dysfunction in patients with malocclusion, abnormal bite, or faulty dentures. There may be tenderness of the masticatory muscles, and an association between pain onset and jaw movement is sometimes noted. This pattern differs from that of jaw (masticatory) claudication, a symptom of giant cell arteritis, in which pain develops progressively with mastication. Treatment of the underlying joint dysfunction relieves symptoms.
A relationship of facial pain to chewing or temperature changes may suggest a dental disturbance. The cause is sometimes not obvious, and diagnosis requires careful dental examination and x-rays. Sinusitis and ear infections causing facial pain are usually recognized by the history of respiratory tract infection, fever, and, in some instances, aural discharge. There may be localized tenderness. Radiologic evidence of sinus infection or mastoiditis is confirmatory.
Glaucoma is an important ocular cause of facial pain, usually localized to the periorbital region.
On occasion, pain in the jaw may be the principal manifestation of angina pectoris. Precipitation by exertion
P.1004
and radiation to more typical areas establish the cardiac origin.
Epilepsy
![]() Essentials of Diagnosis
Essentials of Diagnosis
Recurrent seizures.
Characteristic electroencephalographic changes accompany seizures.
Mental status abnormalities or focal neurologic symptoms may persist for hours postictally.
General Considerations
The term epilepsy denotes any disorder characterized by recurrent seizures. A seizure is a transient disturbance of cerebral function due to an abnormal paroxysmal neuronal discharge in the brain. Epilepsy is common, affecting approximately 0.5% of the population in the United States.
Etiology
Epilepsy has several causes. Its most likely cause in individual patients relates to the age at onset.
A. Idiopathic or Constitutional Epilepsy
Seizures usually begin between 5 and 20 years of age but may start later in life. No specific cause can be identified, and there is no other neurologic abnormality.
B. Symptomatic Epilepsy
There are many causes for recurrent seizures.
1. Pediatric age groups
Congenital abnormalities and perinatal injuries may result in seizures presenting in infancy or childhood.
2. Metabolic disorders
Withdrawal from alcohol or drugs is a common cause of recurrent seizures, and other metabolic disorders such as uremia and hypoglycemia or hyperglycemia may also be responsible.
3. Trauma
Trauma is an important cause of seizures at any age, but especially in young adults. Posttraumatic epilepsy is more likely to develop if the dura mater was penetrated and generally becomes manifest within 2 years following the injury. However, seizures developing in the first week after head injury do not necessarily imply that future attacks will occur. There is no clear evidence that prophylactic anticonvulsant drug treatment reduces the incidence of posttraumatic epilepsy.
4. Tumors and other space-occupying lesions
Neoplasms may lead to seizures at any age, but they are an especially important cause of seizures in middle and later life, when the incidence of neoplastic disease increases. The seizures are commonly the initial symptoms of the tumor and often are partial (focal) in character. They are most likely to occur with structural lesions involving the frontal, parietal, or temporal regions. Tumors must be excluded by appropriate imaging studies in all patients with onset of seizures after 30 years of age, focal seizures or signs, or a progressive seizure disorder.
5. Vascular diseases
Vascular diseases become increasingly frequent causes of seizures with advancing age and are the most common cause of seizures with onset at age 60 years or older.
6. Degenerative disorders
Alzheimer's disease and other degenerative disorders are a cause of seizures in later life.
7. Infectious diseases
Infectious diseases must be considered in all age groups as potentially reversible causes of seizures. Seizures may occur with an acute infective or inflammatory illness, such as bacterial meningitis or herpes encephalitis, or in patients with more longstanding or chronic disorders such as neurosyphilis or cerebral cysticercosis. In patients with AIDS, they may result from central nervous system toxoplasmosis, cryptococcal meningitis, secondary viral encephalitis, or other infective complications. Seizures are a common sequela of supratentorial brain abscess, developing most frequently in the first year after treatment.
Classification of Seizures
Seizures can be categorized in various ways, but the descriptive classification proposed by the International League Against Epilepsy is clinically the most useful. Seizures are divided into those that are generalized and those affecting only part of the brain (partial seizures) (Table 24-2).
A. Partial Seizures
The initial clinical and electroencephalographic manifestations of partial seizures indicate that only a restricted part of one cerebral hemisphere has been activated. The ictal manifestations depend on the area of the brain involved. Partial seizures are subdivided into simple seizures, in which consciousness is preserved, and complex seizures, in which it is impaired. Partial seizures of either type sometimes become secondarily generalized, leading to a tonic, clonic, or tonic-clonic attack.
Table 24-2. Seizure classification. | ||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
1. Simple partial seizures
Simple seizures may be manifested by focal motor symptoms (convulsive jerking) or somatosensory symptoms (eg, paresthesias or tingling) that spread (or march ) to different parts of the limb or body depending on their cortical representation. In other instances, special sensory symptoms (eg, light flashes or buzzing) indicate involvement of visual, auditory, olfactory, or gustatory regions of the brain, or there may be autonomic symptoms or signs (eg, abnormal epigastric sensations, sweating, flushing,
P.1005
pupillary dilation). The sole manifestations of some seizures are phenomena such as dysphasia, dysmnesic symptoms (eg, d j vu, jamais vu), affective disturbances, illusions, or structured hallucinations, but such symptoms are usually accompanied by impairment of consciousness.
2. Complex partial seizures
Impaired consciousness may be preceded, accompanied, or followed by the psychic symptoms mentioned above, and automatisms may occur. Such seizures may also begin with some of the other simple symptoms mentioned above.
B. Generalized Seizures
There are several different varieties of generalized seizures, as outlined below. In some circumstances, seizures cannot be classified because of incomplete information or because they do not fit into any category.
1. Absence (petit mal) seizures
These are characterized by impairment of consciousness, sometimes with mild clonic, tonic, or atonic components (ie, reduction or loss of postural tone), autonomic components (eg, enuresis), or accompanying automatisms. Onset and termination of attacks are abrupt. If attacks occur during conversation, the patient may miss a few words or may break off in mid sentence for a few seconds. The impairment of external awareness is so brief that the patient is unaware of it. Absence seizures almost always begin in childhood and frequently cease by the age of 20 years, although occasionally they are then replaced by other forms of generalized seizure. Electroencephalographically, such attacks are associated with bursts of bilaterally synchronous and symmetric 3-Hz spike-and-wave activity. A normal background in the electroencephalogram and normal or above-normal intelligence imply a good prognosis for the ultimate cessation of these seizures.
2. Atypical absences
There may be more marked changes in tone, or attacks may have a more gradual onset and termination than in typical absences.
3. Myoclonic seizures
Myoclonic seizures consist of single or multiple myoclonic jerks.
4. Tonic-clonic (grand mal) seizures
In these seizures, which are characterized by sudden loss of consciousness, the patient becomes rigid and falls to the ground, and respiration is arrested. This tonic phase, which usually lasts for less than a minute, is followed by a clonic phase in which there is jerking of the body musculature that may last for 2 or 3 minutes and is then followed by a stage of flaccid coma. During the seizure, the tongue or lips may be bitten, urinary or
P.1006
fecal incontinence may occur, and the patient may be injured. Immediately after the seizure, the patient may either recover consciousness, drift into sleep, have a further convulsion without recovery of consciousness between the attacks (status epilepticus), or after recovering consciousness have a further convulsion (serial seizures). In other cases, patients will behave in an abnormal fashion in the immediate postictal period, without subsequent awareness or memory of events (postepileptic automatism). Headache, disorientation, confusion, drowsiness, nausea, soreness of the muscles, or some combination of these symptoms commonly occurs postictally.
5. Tonic, clonic, or atonic seizures
Loss of consciousness may occur with either the tonic or clonic accompaniments described above, especially in children. Atonic seizures (epileptic drop attacks) have also been described.
Clinical Findings
A. Symptoms and Signs
Nonspecific changes such as headache, mood alterations, lethargy, and myoclonic jerking alert some patients to an impending seizure hours before it occurs. These prodromal symptoms are distinct from the aura which may precede a generalized seizure by a few seconds or minutes and which is itself a part of the attack, arising locally from a restricted region of the brain.
In most patients, seizures occur unpredictably at any time and without any relationship to posture or ongoing activities. Occasionally, however, they occur at a particular time (eg, during sleep) or in relation to external precipitants such as lack of sleep, missed meals, emotional stress, menstruation, alcohol ingestion (or alcohol withdrawal; see below), or use of certain drugs. Fever and nonspecific infections may also precipitate seizures in known epileptics. In a few patients, seizures are provoked by specific stimuli such as flashing lights or a flickering television set (photosensitive epilepsy), music, or reading.
Clinical examination between seizures shows no abnormality in patients with idiopathic epilepsy, but in the immediate postictal period, extensor plantar responses may be seen. The presence of lateralized or focal signs postictally suggests that seizures may have a focal origin. In patients with symptomatic epilepsy, the findings on examination will reflect the underlying cause.
B. Imaging
MRI is indicated for patients with focal neurologic symptoms or signs, focal seizures, or electroencephalographic findings of a focal disturbance; some clinicians routinely order imaging studies for all patients with new-onset seizure disorders. Such studies should certainly be performed in patients with clinical evidence of a progressive disorder and in those presenting with new onset of seizures after the age of 20 years, because of the possibility of an underlying neoplasm. A chest radiograph should also be obtained in such patients, since the lungs are a common site for primary or secondary neoplasms.
C. Laboratory and Other Studies
Initial investigations should always include a full blood count, blood glucose determination, liver and renal function tests, and serologic tests for syphilis. The hematologic and biochemical screening tests are important both in excluding various causes of seizures and in providing a baseline for subsequent monitoring of long-term effects of treatment.
Electroencephalography may support the clinical diagnosis of epilepsy (by demonstrating paroxysmal abnormalities containing spikes or sharp waves), may provide a guide to prognosis, and may help classify the seizure disorder. Classification of the disorder is important for determining the most appropriate anticonvulsant drug with which to start treatment. For example, absence (petit mal) and complex partial seizures may be difficult to distinguish clinically, but the electroencephalographic findings and treatment of choice differ in these two conditions. Finally, by localizing the epileptogenic source, the electroencephalographic findings are important in evaluating candidates for surgical treatment.
Differential Diagnosis
The distinction between the various disorders likely to be confused with generalized seizures is usually made on the basis of the history. The importance of obtaining an eyewitness account of the attacks cannot be overemphasized.
A. Differential Diagnosis of Partial Seizures
1. Transient ischemic attacks
These attacks are distinguished from seizures by their longer duration, lack of spread, and symptoms. Level of consciousness, which is unaltered, does not distinguish them. There is a loss of motor or sensory function (eg, weakness or numbness) with transient ischemic attacks, whereas positive symptoms (eg, convulsive jerking or paresthesias) characterizes seizures.
2. Rage attacks
Rage attacks are usually situational and lead to goal-directed aggressive behavior.
3. Panic attacks
These may be hard to distinguish from simple or complex partial seizures unless there is evidence of psychopathologic disturbances between attacks and the attacks have a clear relationship to external circumstances.
B. Differential Diagnosis of Generalized Seizures
1. Syncope
Syncopal episodes usually occur in relation to postural change, emotional stress, instrumentation, pain, or straining. They are typically preceded by
P.1007
pallor, sweating, nausea, and malaise and lead to loss of consciousness accompanied by flaccidity; recovery occurs rapidly with recumbency, and there is no postictal headache or confusion. In some instances, however, motor accompaniments may simulate a seizure. Serum creatine kinase measured about 3 hours after the event is generally normal after syncopal episodes but markedly elevated after tonic-clonic seizures.
2. Cardiac dysrhythmias
Cerebral hypoperfusion due to a disturbance of cardiac rhythm should be suspected in patients with known cardiac or vascular disease or in elderly patients who present with episodic loss of consciousness. Prodromal symptoms are typically absent. A relationship of attacks to physical activity and the finding of a systolic murmur is suggestive of aortic stenosis. Repeated Holter monitoring may be necessary to establish the diagnosis; monitoring initiated by the patient ( event monitor ) may be valuable if the disturbances of consciousness are rare.
3. Brainstem ischemia
Loss of consciousness is preceded or accompanied by other brainstem signs. Basilar artery migraine and vertebrobasilar vascular disease are discussed elsewhere in this chapter.
4. Pseudoseizures
The term pseudoseizures is used to denote both hysterical conversion reactions and attacks due to malingering when these simulate epileptic seizures. Many patients with pseudoseizures also have true seizures or a family history of epilepsy. Although pseudoseizures tend to occur at times of emotional stress, this may also be the case with true seizures.
Clinically, the attacks superficially resemble tonic-clonic seizures, but there may be obvious preparation before pseudoseizures occur. Moreover, there is usually no tonic phase; instead, there is an asynchronous thrashing of the limbs, which increases if restraints are imposed and which rarely leads to injury. Consciousness may be normal or lost, but in the latter context the occurrence of goal-directed behavior or of shouting, swearing, etc, indicates that it is feigned. Postictally, there are no changes in behavior or neurologic findings.
Laboratory studies may aid in recognition of pseudoseizures. There are no electrocerebral changes, whereas the electroencephalogram changes during organic seizures accompanied by loss of consciousness. The serum level of prolactin has been found to increase dramatically between 15 and 30 minutes after a tonic-clonic convulsion in most patients, whereas it is unchanged after a pseudoseizure. Serum creatine kinase levels also increase after convulsions but not pseudoseizures.
Treatment
A. General Measures
For patients with recurrent seizures, drug treatment is prescribed with the goal of preventing further attacks and is usually continued until there have been no seizures for at least 3 years. Epileptic patients should be advised to avoid situations that could be dangerous or life-threatening if further seizures should occur. State legislation may require clinicians to report to the state department of public health any patients with seizures or other episodic disturbances of consciousness.
1. Choice of medication
The drug with which treatment is best initiated depends on the type of seizures to be treated (Table 24-3). The dose of the selected drug is gradually increased until seizures are controlled or side effects prevent further increases. If seizures continue despite treatment at the maximal tolerated dose, a second drug is added and the dose increased depending on tolerance; the first drug is then gradually withdrawn. In treatment of partial and secondarily generalized tonic-clonic seizures, the success rate is higher with carbamazepine, phenytoin, or valproic acid than with phenobarbital or primidone. Gabapentin, topiramate, lamotrigine, oxcarbazepine, levetiracetam, and zonisamide are newer antiepileptic drugs that are effective for partial or secondarily generalized seizures. Felbamate is also effective for such seizures but, because it may cause aplastic anemia or fulminant hepatic failure, should be used only in selected patients unresponsive to other measures. Tiagabine is another adjunctive agent for partial seizures. In most patients with seizures of a single type, satisfactory control can be achieved with a single anticonvulsant drug. Treatment with two drugs may further reduce seizure frequency or severity, but usually only at the cost of greater toxicity. Treatment with more than two drugs is almost always unhelpful unless the patient is having seizures of different types.
2. Monitoring
Monitoring serum drug levels has led to major advances in the management of seizure disorders. The same daily dose of a particular drug leads to markedly different blood concentrations in different patients, and this will affect the therapeutic response. In general, the dose of an antiepileptic agent is increased depending on the clinical response regardless of the serum drug level. The trough drug level is then measured to provide a reference point for the maximum tolerated dose. Dosing should not be based simply on serum levels because many patients require levels that exceed the therapeutic range ( toxic levels ) but tolerate these without ill effect. Steady-state drug levels in the blood should be measured after treatment is initiated, dosage is changed, or another drug is added to the therapeutic regimen and when seizures are poorly controlled. Dose adjustments are then guided by the laboratory findings. The most common cause of a lower concentration of drug than expected for the prescribed dose is poor patient compliance. Compliance can be improved by limiting to a minimum the number of daily doses. Recurrent seizures or status epilepticus may result if drugs are taken erratically, and in some circumstances noncompliant patients may be better off without any medication.
Table 24-3. Drug treatment for seizures. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
All anticonvulsant drugs have side effects, and some of these are shown in Table 24-3.
P.1008
P.1009
In most patients, a complete blood count should be performed at least annually because of the risk of anemia or blood dyscrasia. Treatment with certain drugs may require more frequent monitoring or use of additional screening tests. For example, periodic tests of hepatic function are necessary if valproic acid, carbamazepine, or felbamate is used, and serial blood counts are important with carbamazepine, ethosuximide, or felbamate.
3. Discontinuance of medication
Only when patients have been seizure-free for several (at least 3) years should withdrawal of medication be considered. Unfortunately, there is no way of predicting which patients can be managed successfully without treatment, although seizure recurrence is more likely in patients who initially failed to respond to therapy, those with seizures having focal features or of multiple types, and those with continuing electroencephalographic abnormalities. Dose reduction should be gradual over a period of weeks or months, and drugs should be withdrawn one at a time. If seizures recur, treatment is reinstituted with the same drugs used previously. Seizures are no more difficult to control after a recurrence than before.
4. Surgical treatment
Patients with surgically remediable epilepsy or seizures refractory to pharmacologic management may be candidates for operative treatment, which is best undertaken in specialized centers.
5. Vagal nerve stimulation
Treatment by chronic vagal nerve stimulation for adults and adolescents with medically refractory partial-onset seizures is approved in the United States and provides an alternative approach for patients who are not optimal candidates for surgical treatment. The mechanism of therapeutic action is unknown. Adverse effects consist mainly of transient hoarseness during stimulus delivery.
B. Special Circumstances
1. Solitary seizures
In patients who have had only one seizure, investigation as outlined above should exclude an underlying cause requiring specific treatment. An EEG should also be performed, preferably within 24 hours after the seizure, because the findings may influence management especially when focal abnormalities are present. Prophylactic anticonvulsant drug treatment is generally not required unless further attacks occur or investigations reveal some underlying pathology that itself is untreatable. The risk of seizure recurrence varies in different series between about 30% and 70%. Epilepsy should not be diagnosed on the basis of a solitary seizure. If seizures occur in the context of transient, nonrecurrent systemic disorders such as acute cerebral anoxia, the diagnosis of epilepsy is inaccurate, and long-term prophylactic anticonvulsant drug treatment is unnecessary.
2. Alcohol withdrawal seizures
One or more generalized tonic-clonic seizures may occur within 48 hours or so of withdrawal from alcohol after a period of high or chronic intake. Patients should be hospitalized for at least 24 hours for observation and to follow
P.1010
the severity of withdrawal symptoms. If the seizures have consistently focal features, the possibility of an associated structural abnormality, often traumatic in origin, must be considered. Head CT scan or MRI should be performed in patients with new onset of generalized seizures and whenever there are focal features associated with any seizures. Treatment with anticonvulsant drugs is generally not required for alcohol withdrawal seizures, since they are self-limited. Benzodiazepines (diazepam or lorazepam) are effective and safe for preventing further seizures. Status epilepticus may rarely follow alcohol withdrawal and is managed along conventional lines (see below). Further attacks will not occur if the patient abstains from alcohol.
3. Tonic-clonic status epilepticus
Poor compliance with the anticonvulsant drug regimen is the most common cause; others include alcohol withdrawal, intracranial infection or neoplasms, metabolic disorders, and drug overdose. The mortality rate may be as high as 20%, and among survivors the incidence of neurologic and mental sequelae may be high. The prognosis relates to the length of time between onset of status epilepticus and the start of effective treatment.
Status epilepticus is a medical emergency. Initial management includes maintenance of the airway and 50% dextrose (25 50 mL) intravenously in case hypoglycemia is responsible. If seizures continue, 10 mg of diazepam is given intravenously over the course of 2 minutes, and the dose is repeated after 10 minutes if necessary. Alternatively, a 4-mg intravenous bolus of lorazepam, repeated once after 10 minutes if necessary, is given in place of diazepam. This is usually effective in halting seizures for a brief period but occasionally causes respiratory depression.
Regardless of the response to diazepam or lorazepam, phenytoin (18 20 mg/kg) is given intravenously at a rate of 50 mg/min; this provides initiation of long-term seizure control. The drug is best injected directly but can also be given in saline; it precipitates, however, if injected into glucose-containing solutions. Because arrhythmias may develop during rapid administration of phenytoin, electrocardiographic monitoring is prudent. Hypotension may complicate phenytoin administration, especially if diazepam has also been given. In the United States, injectable phenytoin has been replaced by fosphenytoin, which is rapidly and completely converted to phenytoin following intravenous administration. No dosing adjustments are necessary because fosphenytoin is expressed in terms of phenytoin equivalents (PE); fosphenytoin is less likely to cause reactions at the infusion site, can be given with all common intravenous solutions, and may be administered at a faster rate (150 mg PE/min). It is also more expensive.
If seizures continue, phenobarbital is then given in a loading dose of 10 20 mg/kg intravenously by slow or intermittent injection (50 mg/min). Respiratory depression and hypotension are common complications and should be anticipated; they may occur also with diazepam alone, although less commonly. If these measures fail, general anesthesia with ventilatory assistance and neuromuscular junction blockade may be required. Alternatively, intravenous midazolam may provide control of refractory status epilepticus; the suggested loading dose is 0.2 mg/kg, followed by 0.05 0.2 mg/kg/h.
After status epilepticus is controlled, an oral drug program for the long-term management of seizures is started, and investigations into the cause of the disorder are pursued.
4. Nonconvulsive status epilepticus
Absence (petit mal) and complex partial status epilepticus are characterized by fluctuating abnormal mental status, confusion, impaired responsiveness, and automatism. Electroencephalography is helpful both in establishing the diagnosis and in distinguishing the two varieties. Initial treatment with intravenous diazepam is usually helpful regardless of the type of status epilepticus, but phenytoin, phenobarbital, carbamazepine, and other drugs may also be needed to obtain and maintain control in complex partial status epilepticus.
Brathen G et al: EFNS guidelines on the diagnosis and management of alcohol-related seizures: report of a EFNS task force. Eur J Neurol 2005;12:816.
Chang BS et al: Epilepsy. N Engl J Med 2003;349:1257.
Kelso AR et al: Advances in epilepsy. Br Med Bull 2005;72:135.
Schachter SC: Epilepsy: major advances in treatment. Lancet Neurol 2004;3:11.
Vazquez B: Monotherapy in epilepsy: role of the newer antiepileptic drugs. Arch Neurol 2004;61:1361.
Dysautonomia
![]() Essentials of Diagnosis
Essentials of Diagnosis
Abnormalities of blood pressure, heart rate, sweating, intestinal motility, sphincter control, sexual function, respiration, or ocular function, occurring in isolation or any combination.
General Considerations
Dysautonomia may occur as a result of central or peripheral pathologic processes. It is manifested by a variety of symptoms that may occur in isolation or in various combinations and relate to abnormalities of blood pressure regulation, thermoregulatory sweating, gastrointestinal function, sphincter control, sexual function, respiration, and ocular function. Syncope, a symptom of dysautonomia, is characterized by a transient loss of consciousness, usually accompanied by hypotension and bradycardia. It may occur in response to emotional stress, postural hypotension, vigorous exercise in a hot environment, obstructed venous return to the heart, acute pain or its anticipation, fluid loss, and a variety of other circumstances.
P.1011
A. Central Neurologic Causes
Disease at certain sites in the central nervous system, regardless of its nature, may lead to dysautonomic symptoms. Postural hypotension, which is usually the most troublesome and disabling symptom, may result from spinal cord transection and other myelopathies (eg, due to tumor or syringomyelia) above the T6 level or from brainstem lesions such as syringobulbia and posterior fossa tumors. Sphincter or sexual disturbances may result from cord lesions below T6. Certain primary degenerative disorders are responsible for dysautonomia occurring in isolation (pure autonomic failure) or in association with more widespread abnormalities (multisystem atrophy or Shy-Drager syndrome) that may include parkinsonian, pyramidal symptoms, and cerebellar deficits.
B. Peripheral Neurologic Causes
A pure autonomic neuropathy may occur acutely or subacutely after a viral infection or as a paraneoplastic disorder related usually to small cell lung cancer, particularly in association with certain antibodies, such as anti-Hu or those directed at neuronal nicotinic acetylcholine receptors. Typically, presenting symptoms include postural hypotension, impaired thermoregulatory sweating, xerostomia or xerophthalmia, abnormal gastrointestinal motility, dilated pupils, or acute urinary retention. Dysautonomia is often conspicuous in patients with Guillain-Barr syndrome, manifesting with marked hypotension or hypertension or cardiac arrhythmias that may have a fatal outcome. It may also occur with diabetic, uremic, amyloidotic, and various other metabolic or toxic neuropathies; in association with leprosy or Chagas' disease; and as a feature of certain hereditary neuropathies with autosomal dominant or recessive inheritance or an X-linked pattern. Autonomic symptoms are prominent in the crises of hepatic porphyria. Patients with botulism or the Lambert-Eaton myasthenic syndrome may have constipation, urinary retention, and a sicca syndrome as a result of impaired cholinergic function.
Clinical Findings
A. Symptoms and Signs
Dysautonomic symptoms include syncope, postural hypotension, paroxysmal hypertension, persistent tachycardia without other cause, facial flushing, hypohidrosis or hyperhidrosis, vomiting, constipation, diarrhea, dysphagia, abdominal distention, disturbances of micturition or defecation, apneic episodes, and declining night vision. In syncope, prodromal malaise, nausea, headache, diaphoresis, pallor, visual disturbance, loss of postural tone, and a sense of weakness and impending loss of consciousness are followed by actual loss of consciousness. Although the patient is usually flaccid, some motor activity is not uncommon, and urinary (and rarely fecal) incontinence may also occur, thereby simulating a seizure. Recovery is rapid once the patient becomes recumbent, but headache, nausea, and fatigue are common postictally.
B. Evaluation of the Patient
Clinical evaluation is important to exclude reversible, nonneurologic causes of symptoms. Postural hypotension and syncope, for example, may relate to a reduced cardiac output (eg, from aortic stenosis or cardiomyopathy), paroxysmal cardiac dysrhythmias, volume depletion, various medications, and endocrine and metabolic disorders such as Addison's disease, hypothyroidism or hyperthyroidism, pheochromocytoma, and carcinoid syndrome. Testing of autonomic function helps establish the diagnosis of dysautonomia, to exclude other causes of symptoms, to assess the severity of involvement, and to guide prognostication. Such testing includes evaluating the cardiovascular response to the Valsalva maneuver, startle, mental stress, postural change, and deep respiration, and the sudomotor (sweating) responses to warming or a deep inspiratory gasp. Tilt-table testing may reproduce syncopal or presyncopal symptoms. Pharmacologic studies to evaluate the pupillary responses, radiologic studies of the bladder or gastrointestinal tract, uroflowmetry and urethral pressure profiles, and recording of nocturnal penile tumescence may also be necessary in selected cases. Further investigation depends on the presence of other associated neurologic abnormalities. In patients with a peripheral cause, work-up for peripheral neuropathy may be required as discussed below. For those with evidence of a central lesion, imaging studies will exclude a treatable structural cause.
Treatment
The most disabling symptom of dysautonomia is usually postural hypotension and syncope. Abrupt postural change, prolonged recumbency, and other precipitants should be avoided. Medications associated with postural hypotension should be discontinued or reduced in dose. Treatment may include wearing waist-high elastic hosiery, salt supplementation, sleeping in a semierect position (which minimizes the natriuresis and diuresis that occur during recumbency), and fludrocortisone (0.1 0.2 mg daily). Vasoconstrictor agents may be helpful and include midodrine (2.5 10 mg three times daily) and ephedrine (15 30 mg three times daily). Other agents that have been used occasionally or experimentally are dihydroergotamine, yohimbine, and clonidine; refractory cases may respond to erythropoietin (epoetin alfa) or desmopressin. Patients must be monitored for recumbent hypertension. Postprandial hypotension is helped by caffeine. There is no satisfactory treatment for disturbances of sweating, but an air-conditioned environment is helpful in avoiding extreme swings in body temperature.
Chen-Scarabelli C et al: Neurocardiogenic syncope. BMJ 2004; 329:336.
P.1012
Freeman R: Autonomic peripheral neuropathy. Lancet 2005;365: 1259.
Sensory Disturbances
Patients may complain of either lost or abnormal sensations. The term numbness is often used by patients to denote loss of feeling, but the word also has other meanings and the patient's intention must be clarified. Abnormal spontaneous sensations are generally called paresthesias, and unpleasant or painful sensations produced by a stimulus that is usually painless are called dysesthesias.
Sensory symptoms may be due to disease located anywhere along the peripheral or central sensory pathways. The character, site, mode of onset, spread, and temporal profile of sensory symptoms must be established and any precipitating or relieving factors identified. These features and the presence of any associated symptoms help identify the origin of sensory disturbances, as do the physical signs as well. Sensory symptoms or signs may conform to the territory of individual peripheral nerves or nerve roots. Involvement of one side of the body or of one limb in its entirety suggests a central lesion. Distal involvement of all four extremities suggests polyneuropathy, a cervical cord or brainstem lesion, or when symptoms are transient a metabolic disturbance such as hyperventilation syndrome. Short-lived sensory complaints may be indicative of sensory seizures or cerebral ischemic phenomena as well as metabolic disturbances. In patients with cord lesions, there may be a transverse sensory level. Dissociated sensory loss is characterized by loss of some sensory modalities with preservation of others. Such findings may be encountered in patients with either peripheral or central disease and must therefore be interpreted in the clinical context in which they are found.
The absence of sensory signs in patients with sensory symptoms does not mean that symptoms have a nonorganic basis. Symptoms are often troublesome before signs of sensory dysfunction have had time to develop.
Weakness & Paralysis
Loss of muscle power may result from central disease involving the upper or lower motor neurons; from peripheral disease involving the roots, plexus, or peripheral nerves; from disorders of neuromuscular transmission; or from primary disorders of muscle. The clinical findings help localize the lesion and thus reduce the number of diagnostic possibilities.
Weakness due to upper motor neuron lesions is characterized by selective involvement of certain muscle groups and is associated with spasticity, increased tendon reflexes, and extensor plantar responses. The site of upper motor neuron (pyramidal) involvement may be indicated by the presence of other clinical signs or by the distribution of the motor deficit. Lower motor neuron lesions lead to muscle wasting as well as weakness, with flaccidity and loss of tendon reflexes, but no change in the plantar responses unless the neurons subserving them are directly involved. Fasciculations may be evident over affected muscles. In distinguishing between a root, plexus, or peripheral nerve lesion, the distribution of the motor deficit and of any sensory changes is of particular importance. In patients with disturbances of neuromuscular transmission, weakness is patchy in distribution, often fluctuates over short periods of time, and is not associated with sensory changes. In myopathic disorders, weakness is usually most marked proximally in the limbs, is not associated with sensory loss or sphincter disturbance, and is not accompanied by muscle wasting or loss of tendon reflexes at least not until an advanced stage.
Transient Ischemic Attacks
![]() Essentials of Diagnosis
Essentials of Diagnosis
Focal neurologic deficit of acute onset.
Clinical deficit resolves completely within 24 hours.
Risk factors for vascular disease often present.
General Considerations
Transient ischemic attacks are characterized by focal ischemic cerebral neurologic deficits that last for less than 24 hours (usually less than 1 2 hours). About 30% of patients with stroke have a history of transient ischemic attacks, and proper treatment of the attacks is an important means of prevention. The incidence of stroke does not relate to either the number or the duration of individual attacks but is increased in patients with hypertension or diabetes. The risk of stroke is highest in the month after a transient ischemic attack (particularly in the first 48 hours) and progressively declines thereafter.
Etiology
An important cause of transient cerebral ischemia is embolization. In many patients with these attacks, a source is readily apparent in the heart or a major extracranial artery to the head, and emboli sometimes are visible in the retinal arteries. Moreover, an embolic phenomenon explains why separate attacks may affect different parts of the territory supplied by the same major vessel. Cardiac causes of embolic ischemic attacks include atrial fibrillation, rheumatic heart disease, mitral valve disease, infective endocarditis, atrial myxoma, and mural thrombi complicating myocardial infarction. Atrial septal defects and patent foramen
P.1013
ovale may permit emboli from the veins to reach the brain ( paradoxical emboli ). An ulcerated plaque on a major artery to the brain may serve as a source of emboli. In the anterior circulation, atherosclerotic changes occur most commonly in the region of the carotid bifurcation extracranially, and these changes may cause a bruit. In some patients with transient ischemic attacks or strokes, an acute or recent hemorrhage is found to have occurred into this atherosclerotic plaque, and this finding may have pathologic significance. Patients with AIDS have an increased risk of developing transient ischemic deficits or strokes.
Less common abnormalities of blood vessels that may cause transient ischemic attacks include fibromuscular dysplasia, which affects particularly the cervical internal carotid artery; atherosclerosis of the aortic arch; inflammatory arterial disorders such as giant cell arteritis, systemic lupus erythematosus, polyarteritis, and granulomatous angiitis; and meningovascular syphilis. Hypotension may cause a reduction of cerebral blood flow if a major extracranial artery to the brain is markedly stenosed, but this is a rare cause of transient ischemic attack.
Hematologic causes of ischemic attacks include polycythemia, sickle cell disease, and hyperviscosity syndromes. Severe anemia may also lead to transient focal neurologic deficits in patients with preexisting cerebral arterial disease.
The subclavian steal syndrome may lead to transient vertebrobasilar ischemia. Symptoms develop when there is localized stenosis or occlusion of one subclavian artery proximal to the source of the vertebral artery, so that blood is stolen from this artery. A bruit in the supraclavicular fossa, unequal radial pulses, and a difference of 20 mm Hg or more between the systolic blood pressures in the arms should suggest the diagnosis in patients with vertebrobasilar transient ischemic attacks.
Clinical Findings
A. Symptoms and Signs
The symptoms of transient ischemic attacks vary markedly among patients; however, the symptoms in a given individual tend to be constant in type. Onset is abrupt and without warning, and recovery usually occurs rapidly, often within a few minutes.
If the ischemia is in the carotid territory, common symptoms are weakness and heaviness of the contralateral arm, leg, or face, singly or in any combination. Numbness or paresthesias may also occur either as the sole manifestation of the attack or in combination with the motor deficit. There may be slowness of movement, dysphasia, or monocular visual loss in the eye contralateral to affected limbs. During an attack, examination may reveal flaccid weakness with pyramidal distribution, sensory changes, hyperreflexia or an extensor plantar response on the affected side, dysphasia, or any combination of these findings. Subsequently, examination reveals no neurologic abnormality, but the presence of a carotid bruit or cardiac abnormality may provide a clue to the cause of symptoms.
Vertebrobasilar ischemic attacks may be characterized by vertigo, ataxia, diplopia, dysarthria, dimness or blurring of vision, perioral numbness and paresthesias, and weakness or sensory complaints on one, both, or alternating sides of the body. These symptoms may occur singly or in any combination. Drop attacks due to bilateral leg weakness, without headache or loss of consciousness, may occur, sometimes in relation to head movements.
The natural history of attacks is variable. Some patients will have a major stroke after only a few attacks, whereas others may have frequent attacks for weeks or months without having a stroke. Attacks may occur intermittently over a long period of time, or they may stop spontaneously. In general, carotid ischemic attacks are more liable than vertebrobasilar ischemic attacks to be followed by stroke. The stroke risk is greater in patients older than 60 years, in diabetics, or after transient ischemic attacks that last longer than 10 minutes and with symptoms or signs of weakness, speech impairment, or gait disturbance.
B. Imaging
CT scan of the head will exclude the possibility of a small cerebral hemorrhage or a cerebral tumor masquerading as a transient ischemic attack. A number of noninvasive techniques, such as ultrasonography, have been developed for studying the cerebral circulation and imaging the major vessels to the head. Carotid duplex ultrasonography is useful for detecting significant stenosis of the internal carotid artery, but arteriography remains important for demonstrating the status of the cerebrovascular system. MR angiography may reveal stenotic lesions of large vessels but is less sensitive than conventional arteriography. Accordingly, if findings on CT scan are normal, if there is no cardiac source of embolization, and if age and general condition indicate that the patient is a good operative risk, bilateral carotid arteriography should be considered in the further evaluation of carotid ischemic attacks, although the ultrasound findings may help in selecting patients for study.
C. Laboratory and Other Studies
Clinical and laboratory evaluation must include assessment for hypertension, heart disease, hematologic disorders, diabetes mellitus, hyperlipidemia, and peripheral vascular disease. It should include complete blood count, fasting blood glucose and serum cholesterol and homocysteine determinations, serologic tests for syphilis, and an ECG and chest x-ray. Echocardiography with bubble contrast is performed if a cardiac source is likely, and blood cultures are obtained if endocarditis is suspected. Holter monitoring is indicated if a transient, paroxysmal disturbance of cardiac rhythm is suspected.
P.1014
Differential Diagnosis
Focal seizures usually cause abnormal motor or sensory phenomena such as clonic limb movements, paresthesias, or tingling, rather than weakness or loss of feeling. Symptoms generally spread ( march ) up the limb and may lead to a generalized tonic-clonic seizure.
Classic migraine is easily recognized by the visual premonitory symptoms, followed by nausea, headache, and photophobia, but less typical cases may be hard to distinguish. The patient's age and medical history (including family history) may be helpful in this regard. Patients with migraine commonly have a history of episodes since adolescence and report that other family members have a similar disorder.
Focal neurologic deficits may occur during periods of hypoglycemia in diabetic patients receiving insulin or oral hypoglycemic agent therapy.
Treatment
When arteriography reveals a surgically accessible high-grade stenosis (70 99% in luminal diameter) on the side appropriate to carotid ischemic attacks and there is relatively little atherosclerosis elsewhere in the cerebrovascular system, operative treatment (carotid thromboendarterectomy) reduces the risk of ipsilateral carotid stroke, especially when transient ischemic attacks are of recent onset (< 1 month). Surgery is not indicated for mild stenosis (< 30%); its benefits are unclear with severe stenosis plus diffuse intracranial atherosclerotic disease. See Chapter 12 for additional discussion.
In patients with carotid ischemic attacks who are poor operative candidates (and thus have not undergone arteriography) or who are found to have extensive vascular disease, medical treatment should be instituted. Similarly, patients with vertebrobasilar ischemic attacks are treated medically and are not subjected to arteriography unless there is clinical evidence of stenosis or occlusion in the carotid or subclavian arteries.
Medical treatment is aimed at preventing further attacks and stroke. Cigarette smoking should be stopped, and cardiac sources of embolization, hypertension, diabetes, hyperlipidemia, arteritis, or hematologic disorders should be treated appropriately.
A. Embolization from the Heart
If anticoagulants are indicated for the treatment of embolism from the heart, they should be started immediately, provided there is no contraindication to their use. There is no advantage in delay, and the common fear of causing hemorrhage into a previously infarcted area is misplaced, since there is a far greater risk of further embolism to the cerebral circulation if treatment is withheld. Treatment is initiated with intravenous heparin (in a loading dose of 5000 10,000 units of standard-molecular-weight heparin, and maintenance infusion of 1000 2000 units per hour depending on the partial thromboplastin time), while warfarin sodium is introduced in a daily dose of 5 15 mg orally, depending on the international normalized ratio (INR). Warfarin is more effective than aspirin in reducing the incidence of cardioembolic events, but when its use is contraindicated, aspirin (325 mg daily) may be used in patients with nonrheumatic atrial fibrillation to reduce the risk of stroke.
B. Embolization from the Cerebrovascular System
In patients with presumed or angiographically verified atherosclerotic changes in the extracranial or intracranial cerebrovascular circulation, antithrombotic medication is prescribed. The evidence supporting a therapeutic role for aspirin to suppress platelet aggregation is convincing. Platelets adhere to and aggregate around an atherosclerotic plaque and release various substances including thromboxane A2. Treatment with aspirin significantly reduces the frequency of transient ischemic attacks and the incidence of stroke or myocardial infarcts in high-risk patients. A daily dose of 325 mg is adequate; higher doses may provide added benefit but are associated with a higher incidence of gastrointestinal side effects. Dipyridamole is not as effective; it is unclear whether it offers any advantage over aspirin alone when added to aspirin for stroke prevention. In patients intolerant of aspirin, clopidogrel (75 mg) can be used instead. Some physicians use anticoagulant drugs (eg, warfarin, with temporary heparinization until the dose of warfarin is adequate) unless they are medically contraindicated, continuing them for 3 6 months before they are tapered and ultimately replaced with aspirin, which is continued for another year. However, a recent study concluded that warfarin was associated with higher rates of adverse effects without providing benefit over aspirin.
Surgical extracranial-intracranial arterial anastomosis is generally not helpful in patients with transient ischemic attacks associated with stenotic lesions of the distal internal carotid or the proximal middle cerebral arteries.
Chimowitz MI et al: Comparison of warfarin and aspirin for symptomatic intracranial arterial stenosis. N Engl J Med 2005;352:1305.
Elkind MS: Secondary stroke prevention: review of clinical trials. Clin Cardiol 2004;27(Suppl 2):II25.
Nguyen-Huynh MN et al: Transient ischemic attack: a neurologic emergency. Curr Neurol Neurosci Rep 2005;5:13.
Stroke
![]() Essentials of Diagnosis
Essentials of Diagnosis
Sudden onset of characteristic neurologic deficit.
Patient often has history of hypertension, diabetes mellitus, valvular heart disease, or atherosclerosis.
Distinctive neurologic signs reflect the region of the brain involved.
P.1015
General Considerations
In the United States, stroke remains the third leading cause of death, despite a general decline in the incidence of stroke in the last 30 years. The precise reasons for this decline are uncertain, but increased awareness of risk factors (hypertension, diabetes, hyperlipidemia, cigarette smoking, cardiac disease, AIDS, recreational drug abuse, heavy alcohol consumption, family history of stroke) and improved prophylactic measures and surveillance of those at increased risk have been contributory. Elevation of the blood homocysteine level is also a risk factor for stroke, but it is unclear whether this risk is reduced by treatment to lower the level. A previous stroke makes individual patients more susceptible to additional strokes.
For years, strokes have been subdivided pathologically into infarcts (thrombotic or embolic) and hemorrhages, and clinical criteria for distinguishing between these possibilities have been emphasized. However, it is often difficult to determine on clinical grounds the pathologic basis for stroke (Table 24-4).
1. Lacunar Infarction
Lacunar infarcts are small lesions (usually < 5 mm in diameter) that occur in the distribution of short penetrating arterioles in the basal ganglia, pons, cerebellum, anterior limb of the internal capsule, and, less commonly, the deep cerebral white matter. Lacunar infarcts are associated with poorly controlled hypertension or diabetes and have been found in several clinical syndromes, including contralateral pure motor or pure sensory deficit, ipsilateral ataxia with crural paresis, and dysarthria with clumsiness of the hand. The neurologic deficit may progress over 24 36 hours before stabilizing.
Lacunar infarcts are sometimes visible on CT scans as small, punched-out, hypodense areas, but in other patients no abnormality is seen. In some instances, patients with a clinical syndrome suggestive of lacunar infarction are found on CT scanning to have a severe hemispheric infarct.
The prognosis for recovery from the deficit produced by a lacunar infarct is usually good, with partial or complete resolution occurring over the following 4 6 weeks in many instances.
Norrving B: Long-term prognosis after lacunar infarction. Lancet Neurology 2003;2:238.
2. Cerebral Infarction
Thrombotic or embolic occlusion of a major vessel leads to cerebral infarction. Causes include the disorders predisposing to transient ischemic attacks (see above) and atherosclerosis of cerebral arteries. The resulting deficit depends on the particular vessel involved and the extent of any collateral circulation. Cerebral ischemia leads to release of excitatory and other neuropeptides that may augment calcium flux into neurons, thereby leading to cell death and increasing the neurologic deficit.
Clinical Findings
A. Symptoms and Signs
Onset is usually abrupt, and there may then be very little progression except that due to brain swelling. Clinical evaluation should always include examination of the heart and auscultation over the subclavian and carotid vessels to determine whether there are any bruits.
1. Obstruction of carotid circulation
Occlusion of the ophthalmic artery is probably symptomless in most cases because of the rich orbital collaterals, but its transient embolic obstruction can lead to amaurosis fugax sudden and brief loss of vision in one eye.
Occlusion of the anterior cerebral artery distal to its junction with the anterior communicating artery causes weakness and cortical sensory loss in the contralateral leg and sometimes mild weakness of the arm, especially proximally. There may be a contralateral grasp reflex, paratonic rigidity, and abulia (lack of initiative) or frank confusion. Urinary incontinence is not uncommon, particularly if behavioral disturbances are conspicuous. Bilateral anterior cerebral infarction is especially likely to cause marked behavioral changes and memory disturbances. Unilateral anterior cerebral artery occlusion proximal to the junction with the anterior communicating artery is generally well tolerated because of the collateral supply from the other side.
Middle cerebral artery occlusion leads to contralateral hemiplegia, hemisensory loss, and homonymous hemianopia (ie, bilaterally symmetric loss of vision in half of the visual fields), with the eyes deviated to the side of the lesion. If the dominant hemisphere is involved, global aphasia is also present. It may be impossible to distinguish this clinically from occlusion of the internal carotid artery. With occlusion of either of these arteries, there may also be considerable swelling of the hemisphere, leading to drowsiness, stupor, and coma in extreme cases. Occlusions of different branches of the middle cerebral artery cause more limited findings. For example, involvement of the anterior main division leads to a predominantly expressive dysphasia and to contralateral paralysis and loss of sensations in the arm, the face, and, to a lesser extent, the leg. Posterior branch occlusion produces a receptive (Wernicke's) aphasia and a homonymous visual field defect. With involvement of the nondominant hemisphere, speech and comprehension are preserved, but there may be a confusional state, dressing apraxia, and constructional and spatial deficits.
Table 24-4. Features of the major stroke subtypes. | ||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||
2. Obstruction of vertebrobasilar circulation
Occlusion of the posterior cerebral artery may lead to a thalamic syndrome in which contralateral hemisensory
P.1016
P.1017
disturbance occurs, followed by the development of spontaneous pain and hyperpathia. There is often a macular-sparing homonymous hemianopia and sometimes a mild, usually temporary, hemiparesis. Depending on the site of the lesion and the collateral circulation, the severity of these deficits varies and other deficits may also occur, including involuntary movements and alexia. Occlusion of the main artery beyond the origin of its penetrating branches may lead solely to a macular-sparing hemianopia.
Vertebral artery occlusion distally, below the origin of the anterior spinal and posterior inferior cerebellar arteries, may be clinically silent because the circulation is maintained by the other vertebral artery. If the remaining vertebral artery is congenitally small or severely atherosclerotic, however, a deficit similar to that of basilar artery occlusion is seen unless there is good collateral circulation from the anterior circulation through the circle of Willis. When the small paramedian arteries arising from the vertebral artery are occluded, contralateral hemiplegia and sensory deficit occur in association with an ipsilateral cranial nerve palsy at the level of the lesion. An obstruction of the posterior inferior cerebellar artery or an obstruction of the vertebral artery just before it branches to this vessel leads ipsilaterally to spinothalamic sensory loss involving the face, ninth and tenth cranial nerve lesions, limb ataxia and numbness, and Horner's syndrome, combined with contralateral spinothalamic sensory loss involving the limbs.
Occlusion of both vertebral arteries or the basilar artery leads to coma with pinpoint pupils, flaccid quadriplegia and sensory loss, and variable cranial nerve abnormalities. With partial basilar artery occlusion, there may be diplopia, visual loss, vertigo, dysarthria, ataxia, weakness or sensory disturbances in some or all of the limbs, and discrete cranial nerve palsies. In patients with hemiplegia of pontine origin, the eyes are often deviated to the paralyzed side, whereas in patients with a hemispheric lesion, the eyes commonly deviate from the hemiplegic side.
Occlusion of any of the major cerebellar arteries produces vertigo, nausea, vomiting, nystagmus, ipsilateral limb ataxia, and contralateral spinothalamic sensory loss in the limbs. If the superior cerebellar artery is involved, the contralateral spinothalamic loss also involves the face; with occlusion of the anterior inferior cerebellar artery, there is ipsilateral spinothalamic sensory loss involving the face, usually in conjunction with ipsilateral facial weakness and deafness. Massive cerebellar infarction may lead to coma, tonsillar herniation, and death.
3. Coma
Infarction in either the carotid or vertebrobasilar territory may lead to loss of consciousness. For example, an infarct involving one cerebral hemisphere may lead to such swelling that the function of the other hemisphere or the rostral brainstem is disturbed and coma results. Similarly, coma occurs with bilateral brainstem infarction when this involves the reticular formation, and it occurs with brainstem compression after cerebellar infarction.
B. Imaging
Radiography of the chest may reveal cardiomegaly or valvular calcification; the presence of a neoplasm would suggest that the neurologic deficit is due to metastasis rather than stroke, or rarely to nonbacterial thrombotic endocarditis. A CT scan of the head (without contrast) is important in excluding cerebral hemorrhage, but it may not permit distinction between a cerebral infarct and tumor. CT scanning is preferable to MRI in the acute stage because it is quicker and because intracranial hemorrhage is not easily detected by MRI within the first 48 hours after a bleeding episode. In selected patients, carotid duplex studies, MRI and MR angiography, and conventional angiography may also be necessary. Diffusion-weighted MRI is more sensitive than standard MRI in detecting cerebral ischemia.
C. Laboratory and Other Studies
Investigations should include a complete blood count, sedimentation rate, blood glucose determination, and serologic tests for syphilis. Antiphospholipid antibodies (lupus anticoagulants and anticardiolipin antibodies) promote thrombosis and are associated with an increased incidence of stroke. Similarly, elevated serum cholesterol and lipids and serum homocysteine may indicate an increased risk of thrombotic stroke. Electrocardiography will help exclude a cardiac arrhythmia or recent myocardial infarction that might be serving as a source of embolization. Blood cultures should be performed if endocarditis is suspected, echocardiography if heart disease is suspected, and Holter monitoring if paroxysmal cardiac arrhythmia requires exclusion. Examination of the cerebrospinal fluid is not always necessary but may be helpful if there is diagnostic uncertainty; it should be delayed until after CT scanning.
Treatment
If the neurologic deficit progresses over the following minutes or hours, administering heparin may limit or arrest further deterioration. Since the signs of progressing stroke may be simulated by an intracerebral hematoma, the latter must be excluded by immediate CT scanning or angiography before the patient is heparinized.
Intravenous thrombolytic therapy with recombinant tissue plasminogen activator (0.9 mg/kg to a maximum of 90 mg, with 10% given as a bolus over 1 minute and the remainder over 1 hour) is effective in reducing the neurologic deficit in selected patients without CT evidence of intracranial hemorrhage when administered within 3 hours after onset of ischemic stroke, but later administration has not been proved effective or safe. Recent hemorrhage, increased risk of hemorrhage (eg, treatment with anticoagulants), arterial puncture at a noncompressible site, and systolic pressure above 185
P.1018
mm Hg or diastolic pressure above 110 mm Hg are among the contraindications to this treatment. Early management of a completed stroke otherwise consists of attention to general supportive measures. During the acute stage, there may be marked brain swelling and edema, with symptoms and signs of increasing intracranial pressure, an increasing neurologic deficit, or herniation syndrome. Prednisone (up to 100 mg/d) or dexamethasone (16 mg/d) has been used in an attempt to reduce vasogenic cerebral edema, but the evidence that corticosteroids are of any benefit is conflicting. Dehydrating hyperosmolar agents have also been prescribed in efforts to reduce brain swelling, but there is little evidence of any lasting benefit. Likewise, clinical benefit from treatment with vasodilators such as papaverine is minimal. Neither hypercapnia nor hypocapnia has been shown to have any benefit. Barbiturates are known to decrease neuronal metabolism and energy requirements and have been reported to improve functional recovery in experimental stroke models; their use in humans, however, is experimental. Attempts to lower the blood pressure of hypertensive patients during the acute phase (ie, within 2 weeks) of a stroke should generally be avoided, as there is loss of cerebral autoregulation and lowering the blood pressure may further compromise ischemic areas. However, if the systolic pressure exceeds 200 mm Hg, it can be lowered with continuous monitoring to 170 200 mm Hg and then, after 2 weeks, it can be reduced further to less than 140/90 mm Hg.
Anticoagulant drugs should be started when there is a cardiac source of embolization. Treatment is with intravenous heparin while warfarin is introduced. The target is an INR of 2.0 3.0 for the prothrombin time. If the CT scan shows no evidence of hemorrhage and the cerebrospinal fluid is clear, anticoagulant treatment may be started without delay. Some physicians prefer to wait for 2 or 3 days before initiating anticoagulant treatment; the CT scan is then repeated and anticoagulant therapy is initiated if it again shows no evidence of hemorrhagic transformation.
Physical therapy has an important role in the management of patients with impaired motor function. Passive movements at an early stage will help prevent contractures. As cooperation increases and some recovery begins, active movements will improve strength and coordination. In all cases, early mobilization and active rehabilitation are important. Occupational therapy may improve morale and motor skills, while speech therapy may be beneficial in patients with expressive dysphasia or dysarthria. When there is a severe and persisting motor deficit, a device such as a leg brace, toe spring, frame, or cane may help the patient move about, and the provision of other aids to daily living may improve the quality of life.
Prognosis
The prognosis for survival after cerebral infarction is better than after cerebral or subarachnoid hemorrhage. The only proved effective therapy for acute stroke requires initiation within 3 hours after stroke onset, and the prognosis therefore depends on the time that elapses before arrival at the hospital. Patients receiving such treatment with tissue plasminogen activator are at least 30% more likely to have minimal or no disability at 3 months than those not treated by this means. Loss of consciousness after a cerebral infarct implies a poorer prognosis than otherwise. The extent of the infarct governs the potential for rehabilitation. Patients who have had a cerebral infarct are at risk for additional strokes and for myocardial infarcts. Statin therapy to lower serum lipid levels may reduce this risk. Antiplatelet therapy reduces the recurrence rate by 30% among patients without a cardiac cause for the stroke who are not candidates for carotid endarterectomy. Nevertheless, the cumulative risk of recurrence of noncardioembolic stroke is still 3 7% annually. A 2-year comparison did not show benefit of warfarin (INR 1.4 2.8) over aspirin (325 mg daily), and higher doses of warfarin should be avoided as they lead to an increased incidence of major bleeding. Patients with massive strokes from which meaningful recovery is unlikely should receive palliative care (see Chapter 5).
Anticoagulants and antiplatelet agents in acute ischemic stroke: report of the Joint Stroke Guideline Development Committee of the American Academy of Neurology and the American Stroke Association (a division of the American Heart Association). Stroke 2002;33:1934.
Bath P: Anticoagulants and antiplatelet agents in acute ischaemic stroke. Lancet Neurol 2002;1:405.
Caplan LR: Treatment of patients with stroke. Arch Neurol 2002; 59:703.
Hart RG et al: Lessons from the Stroke Prevention in Atrial Fibrillation trials. Ann Intern Med 2003;138:831.
Straus SE et al: New evidence for stroke prevention: scientific review. JAMA 2002;288:1388.
Subramaniam S et al: Massive cerebral infarction. Neurologist 2005;11:150.
3. Intracerebral Hemorrhage
Spontaneous intracerebral hemorrhage in patients with no angiographic evidence of an associated vascular anomaly (eg, aneurysm or angioma) is usually due to hypertension. The pathologic basis for hemorrhage is probably the presence of microaneurysms that develop on perforating vessels of 100 300 mcm in diameter in hypertensive patients. Hypertensive intracerebral hemorrhage occurs most frequently in the basal ganglia and less commonly in the pons, thalamus, cerebellum, and cerebral white matter. Hemorrhage may extend into the ventricular system or subarachnoid space, and signs of meningeal irritation are then found. Hemorrhages usually occur suddenly and without warning, often during activity.
In addition to its association with hypertension, nontraumatic intracerebral hemorrhage may occur with hematologic and bleeding disorders (eg, leukemia,
P.1019
thrombocytopenia, hemophilia, or disseminated intravascular coagulation), anticoagulant therapy, liver disease, cerebral amyloid angiopathy, high alcohol intake, and primary or secondary brain tumors. There is also an association with advancing age and male sex. Bleeding is primarily into the subarachnoid space when it occurs from an intracranial aneurysm or arteriovenous malformation (see below), but it may be partly intraparenchymal as well. In some cases, no specific cause for cerebral hemorrhage can be identified.
Clinical Findings
A. Symptoms and Signs
With hemorrhage into the cerebral hemisphere, consciousness is initially lost or impaired in about one-half of patients. Vomiting occurs very frequently at the onset of bleeding, and headache is sometimes present. Focal symptoms and signs then develop, depending on the site of the hemorrhage. With hypertensive hemorrhage, there is generally a rapidly evolving neurologic deficit with hemiplegia or hemiparesis. A hemisensory disturbance is also present with more deeply placed lesions. With lesions of the putamen, loss of conjugate lateral gaze may be conspicuous. With thalamic hemorrhage, there may be a loss of upward gaze, downward or skew deviation of the eyes, lateral gaze palsies, and pupillary inequalities.
Cerebellar hemorrhage may present with sudden onset of nausea and vomiting, disequilibrium, headache, and loss of consciousness that may terminate fatally within 48 hours. Less commonly, the onset is gradual and the course episodic or slowly progressive clinical features suggesting an expanding cerebellar lesion. In yet other cases, however, the onset and course are intermediate, and examination shows lateral conjugate gaze palsies to the side of the lesion; small reactive pupils; contralateral hemiplegia; peripheral facial weakness; ataxia of gait, limbs, or trunk; periodic respiration; or some combination of these findings.
B. Imaging
CT scanning (without contrast) is important not only in confirming that hemorrhage has occurred but also in determining the size and site of the hematoma. It is superior to MRI for detecting intracranial hemorrhage of less than 48 hours duration. If the patient's condition permits further intervention, cerebral angiography may be undertaken thereafter to determine whether an aneurysm or arteriovenous malformation is present (see below).
C. Laboratory and Other Studies
A complete blood count, platelet count, bleeding time, prothrombin and partial thromboplastin times, and liver and renal function tests may reveal a predisposing cause for the hemorrhage. Lumbar puncture is contraindicated because it may precipitate a herniation syndrome in patients with a large hematoma, and CT scanning is superior in detecting intracerebral hemorrhage.
Treatment
Neurologic management is generally conservative and supportive, regardless of whether the patient has a profound deficit with associated brainstem compression, in which case the prognosis is grim, or a more localized deficit not causing increased intracranial pressure or brainstem involvement. Such therapy may include ventilatory support, blood pressure regulation, seizure prophylaxis, control of fever, osmotherapy, and nutritional supplementation. Intracranial pressure may require monitoring. Ventricular drainage may be required in patients with intraventricular hemorrhage and acute hydrocephalus. Decompression may be helpful when a superficial hematoma in cerebral white matter is exerting a mass effect and causing incipient herniation. In patients with cerebellar hemorrhage, prompt surgical evacuation of the hematoma is appropriate, because spontaneous unpredictable deterioration may otherwise lead to a fatal outcome and because operative treatment may lead to complete resolution of the clinical deficit. The treatment of underlying structural lesions or bleeding disorders depends on their nature. Randomized trials of recombinant activated factor VII given within a few hours of onset are in progress, and preliminary reports are encouraging.
Mayer SA et al: Treatment of intracerebral haemorrhage. Lancet Neurol 2005;4:662.
4. Subarachnoid Hemorrhage
![]() Essentials of Diagnosis
Essentials of Diagnosis
Sudden severe headache.
Signs of meningeal irritation usually present.
Obtundation is common.
Focal deficits frequently absent.
General Considerations
Between 5% and 10% of strokes are due to subarachnoid hemorrhage. Although hemorrhage is usually from rupture of an aneurysm or arteriovenous malformation, no specific cause can be found in 20% of cases.
Clinical Findings
A. Symptoms and Signs
Subarachnoid hemorrhage has a characteristic clinical picture. Its onset is with sudden headache of a severity never experienced previously by the patient. This may be followed by nausea and vomiting and by a loss or impairment of consciousness that can either be transient
P.1020
or progress inexorably to deepening coma and death. If consciousness is regained, the patient is often confused and irritable and may show other symptoms of an altered mental status. Neurologic examination generally reveals nuchal rigidity and other signs of meningeal irritation, except in deeply comatose patients. A focal neurologic deficit is occasionally present and may suggest the site of the underlying lesion.
B. Imaging
A CT scan should be performed immediately to confirm that hemorrhage has occurred and to search for clues regarding its source. It is preferable to MRI because it is faster and more sensitive in detecting hemorrhage in the first 24 hours. CT findings sometimes are normal in patients with suspected hemorrhage, and the cerebrospinal fluid must then be examined for the presence of blood or xanthochromia before the possibility of subarachnoid hemorrhage is discounted.
Cerebral arteriography may be undertaken to determine the source of bleeding; it is not performed unless or until the patient's condition has stabilized and is good enough so that operative treatment is feasible. In general, bilateral carotid and vertebral arteriography are necessary because aneurysms are often multiple, while arteriovenous malformations may be supplied from several sources. MR angiography may also permit these vascular anomalies to be visualized but is less sensitive than conventional arteriography.
Treatment
The measures outlined below in the section on stupor and coma are applied to comatose patients. Conscious patients are confined to bed, advised against any exertion or straining, treated symptomatically for headache and anxiety, and given laxatives or stool softeners. If there is severe hypertension, the blood pressure can be lowered gradually, but not below a diastolic level of 100 mm Hg. Phenytoin is generally prescribed routinely to prevent seizures. Further comment concerning the specific operative management of arteriovenous malformations and aneurysms follows.
5. Intracranial Aneurysm
![]() Essentials of Diagnosis
Essentials of Diagnosis
Subarachnoid hemorrhage or focal deficit.
Abnormal imaging studies.
General Considerations
Saccular aneurysms ( berry aneurysms) tend to occur at arterial bifurcations, are frequently multiple (20% of cases), and are usually asymptomatic. They may be associated with polycystic kidney disease and coarctation of the aorta. Risk factors for aneurysm formation include smoking, hypertension, and hypercholesterolemia. Most aneurysms are located on the anterior part of the circle of Willis particularly on the anterior or posterior communicating arteries, at the bifurcation of the middle cerebral artery, and at the bifurcation of the internal carotid artery.
Clinical Findings
A. Symptoms and Signs
Aneurysms may cause a focal neurologic deficit by compressing adjacent structures. However, most are asymptomatic or produce only nonspecific symptoms until they rupture, at which time subarachnoid hemorrhage results. There is often a paucity of focal neurologic signs in patients with subarachnoid hemorrhage, but when present, such signs may relate either to a focal hematoma or to ischemia in the territory of the vessel with the ruptured aneurysm. Hemiplegia or other focal deficit sometimes occurs after a delay of 4 14 days and is due to focal arterial spasm in the vicinity of the ruptured aneurysm. This spasm is of uncertain, probably multifactorial, cause, but it sometimes leads to significant cerebral ischemia or infarction, and it may further aggravate any existing increase in intracranial pressure. Subacute hydrocephalus due to interference with the flow of cerebrospinal fluid may occur after 2 or more weeks, and this leads to a delayed clinical deterioration that is relieved by shunting.
In some patients, warning leaks of a small amount of blood from the aneurysm precede the major hemorrhage by a few hours or days. They lead to headaches, sometimes accompanied by nausea and neck stiffness, but the true cause of these symptoms is often not appreciated until massive hemorrhage occurs.
B. Imaging
The CT scan generally confirms that subarachnoid hemorrhage has occurred, but occasionally it is normal. Angiography (bilateral carotid and vertebral studies) generally indicates the size and site of the lesion, sometimes reveals multiple aneurysms, and may show arterial spasm. If subarachnoid hemorrhage is confirmed by lumbar puncture or CT scanning but arteriograms show no abnormality, the examination should be repeated after 2 weeks, because vasospasm may have prevented detection of an aneurysm during the initial study.
C. Laboratory and Other Studies
The cerebrospinal fluid is bloodstained. The electroencephalogram sometimes indicates the side or site of hemorrhage but frequently shows only a diffuse abnormality. Electrocardiographic evidence of arrhythmias or myocardial ischemia has been well described and probably relates to excessive sympathetic activity. Peripheral leukocytosis and transient glycosuria are also common findings.
P.1021
Treatment
The major aim of treatment is to prevent further hemorrhages. Definitive treatment requires surgical clipping of the aneurysm base or endovascular treatment (coil embolization) by interventional radiologists; the latter is sometimes feasible even for inoperable aneurysms. Otherwise, medical management as outlined above for subarachnoid hemorrhage is continued for about 6 weeks and is followed by gradual mobilization.
The risk of further hemorrhage is greatest within a few days of the first hemorrhage; approximately 20% of patients will have further bleeding within 2 weeks and 40% within 6 months. Attempts have been made to reduce this risk pharmacologically. Treatment with an antifibrinolytic agent such as aminocaproic acid during the first 14 days reduces the risk of recurrent hemorrhage but is associated with such an increase in cerebral ischemic complications that the mortality rate and the degree of disability among survivors are unchanged. Thus, early operation (ie, within about 2 days of hemorrhage) is preferred for good operative candidates.
Calcium channel-blocking agents have helped reduce or reverse experimental vasospasm, and nimodipine has been shown to reduce, in neurologically normal patients, the incidence of ischemic deficits from arterial spasm without producing any side effects. The dose of nimodipine is 60 mg every 4 hours orally for 21 days. After surgical obliteration of any aneurysms, symptomatic vasospasm may also be treated by intravascular volume expansion, induced hypertension, or transluminal balloon angioplasty of involved intracranial vessels.
With regard to unruptured aneurysms, those that are symptomatic merit prompt treatment, either surgically or by endovascular coil embolization, whereas small asymptomatic ones discovered incidentally are often monitored arteriographically and corrected surgically only if they increase in size to over 10 mm.
Doerfler A et al: Endovascular treatment of cerebrovascular disease. Curr Opin Neurol 2004;17:481.
Molyneux AJ et al: International Subarachnoid Aneurysm Trial (ISAT) of neurosurgical clipping versus endovascular coiling in 2143 patients with ruptured intracranial aneurysms: a randomised comparison of effects on survival, dependency, seizures, rebleeding, subgroups, and aneurysm occlusion. Lancet 2005;366:809.
Roos Y et al: Antifibrinolytic therapy for aneurysmal subarachnoid hemorrhage: a major update of a Cochrane review. Stroke 2003;34:2308.
Wiebers DO et al: Unruptured intracranial aneurysms: natural history, clinical outcome, and risks of surgical and endovascular treatment. Lancet 2003;362:103.
6. Arteriovenous Malformations
![]() Essentials of Diagnosis
Essentials of Diagnosis
Sudden onset of subarachnoid and intracerebral hemorrhage.
Distinctive neurologic signs reflect the region of the brain involved.
Signs of meningeal irritation in patients presenting with subarachnoid hemorrhage.
Seizures or focal deficits may occur.
General Considerations
Arteriovenous malformations are congenital vascular malformations that result from a localized maldevelopment of part of the primitive vascular plexus and consist of abnormal arteriovenous communications without intervening capillaries. They vary in size, ranging from massive lesions that are fed by multiple vessels and involve a large part of the brain to lesions so small that they are hard to identify at arteriography, surgery, or autopsy. In approximately 10% of cases, there is an associated arterial aneurysm, while 1 2% of patients presenting with aneurysms have associated arteriovenous malformations. Clinical presentation may relate to hemorrhage from the malformation or an associated aneurysm or may relate to cerebral ischemia due to diversion of blood by the anomalous arteriovenous shunt or due to venous stagnation. Regional maldevelopment of the brain, compression or distortion of adjacent cerebral tissue by enlarged anomalous vessels, and progressive gliosis due to mechanical and ischemic factors may also be contributory. In addition, communicating or obstructive hydrocephalus may occur and lead to symptoms.
Clinical Findings
A. Symptoms and Signs
1. Supratentorial lesions
Most cerebral arteriovenous malformations are supratentorial, usually lying in the territory of the middle cerebral artery. Initial symptoms consist of hemorrhage in 30 60% of cases, recurrent seizures in 20 40%, headache in 5 25%, and miscellaneous complaints (including focal deficits) in 10 15%. Up to 70% of arteriovenous malformations bleed at some point in their natural history, most commonly before the patient reaches the age of 40 years. This tendency to bleed is unrelated to the lesion site or to the patient's sex, but small arteriovenous malformations are more likely to bleed than large ones. Arteriovenous malformations that have bled once are more likely to bleed again. Hemorrhage is commonly intracerebral as well as into the subarachnoid space, and it has a fatal outcome in about 10% of cases. Focal or generalized seizures may accompany or follow hemorrhage, or they may be the initial presentation, especially with frontal or parietal arteriovenous malformations. Headaches are especially likely when the external carotid arteries are involved in the malformation. These sometimes simulate migraine but more commonly are nonspecific in character, with nothing about them to suggest an underlying structural lesion.
P.1022
In patients presenting with subarachnoid hemorrhage, examination may reveal an abnormal mental status and signs of meningeal irritation. Additional findings may help localize the lesion and sometimes indicate that intracranial pressure is increased. A cranial bruit always suggests the possibility of a cerebral arteriovenous malformation, but bruits may also be found with aneurysms, meningiomas, acquired arteriovenous fistulas, and arteriovenous malformations involving the scalp, calvarium, or orbit. Bruits are best heard over the ipsilateral eye or mastoid region and are of some help in lateralization but of no help in localization. Absence of a bruit in no way excludes the possibility of arteriovenous malformation.
2. Infratentorial lesions
Brainstem arteriovenous malformations are often clinically silent, but they may hemorrhage, cause obstructive hydrocephalus, or lead to progressive or relapsing brainstem deficits. Cerebellar arteriovenous malformations may also be clinically inconspicuous but sometimes lead to cerebellar hemorrhage.
B. Imaging
In patients presenting with suspected hemorrhage, CT scanning indicates whether subarachnoid or intracerebral bleeding has recently occurred, helps localize its source, and may reveal the arteriovenous malformation. If the CT scan shows no evidence of bleeding but subarachnoid hemorrhage is diagnosed clinically, the cerebrospinal fluid should be examined.
When intracranial hemorrhage is confirmed but the source of hemorrhage is not evident on the CT scan, arteriography is necessary to exclude aneurysm or arteriovenous malformation. MR angiography is not sensitive enough for this purpose. Even if the findings on CT scan suggest arteriovenous malformation, arteriography is required to establish the nature of the lesion with certainty and to determine its anatomic features so that treatment can be planned. The examination must generally include bilateral opacification of the internal and external carotid arteries and the vertebral arteries. Arteriovenous malformations typically appear as a tangled vascular mass with distended tortuous afferent and efferent vessels, a rapid circulation time, and arteriovenous shunting. Findings on plain radiographs of the skull are often normal unless an intracerebral hematoma is present, in which case there may be changes suggestive of raised intracranial pressure and displacement of a calcified pineal gland.
In patients presenting without hemorrhage, CT scan or MRI usually reveals the underlying abnormality, and MRI frequently also shows evidence of old or recent hemorrhage that may have been asymptomatic. The nature and detailed anatomy of any focal lesion identified by these means are delineated by angiography, especially if operative treatment is under consideration.
C. Laboratory and Other Studies
Electroencephalography is usually indicated in patients presenting with seizures and may show consistently focal or lateralized abnormalities resulting from the underlying cerebral arteriovenous malformation. This should be followed by CT scanning.
Treatment
Surgical treatment to prevent further hemorrhage is justified in patients with arteriovenous malformations that have bled, provided that the lesion is accessible and the patient has a reasonable life expectancy. Surgical treatment is also appropriate if intracranial pressure is increased and to prevent further progression of a focal neurologic deficit. In patients presenting solely with seizures, anticonvulsant drug treatment is usually sufficient, and operative treatment is unnecessary unless there are further developments.
Definitive operative treatment consists of excision of the arteriovenous malformation if it is surgically accessible. Arteriovenous malformations that are inoperable because of their location are sometimes treated solely by embolization; although the risk of hemorrhage is not reduced, neurologic deficits may be stabilized or even reversed by this procedure. Two other techniques for the treatment of intracerebral arteriovenous malformations are injection of a vascular occlusive polymer through a flow-guided microcatheter and permanent occlusion of feeding vessels by positioning detachable balloon catheters in the desired sites and then inflating them with quickly solidifying contrast material. Stereotactic radiosurgery with the gamma knife is also useful in the management of inoperable cerebral arteriovenous malformations.
Choi JH et al: Brain arteriovenous malformations in adults. Lancet Neurol 2005;4:299.
Fleetwood IG et al: Arteriovenous malformations. Lancet 2002; 359:863.
7. Intracranial Venous Thrombosis
Intracranial venous thrombosis may occur in association with intracranial or maxillofacial infections, hypercoagulable states, polycythemia, sickle cell disease, and cyanotic congenital heart disease and in pregnancy or during the puerperium. It is characterized by headache, focal or generalized convulsions, drowsiness, confusion, increased intracranial pressure, and focal neurologic deficits and sometimes by evidence of meningeal irritation. The diagnosis is confirmed by CT scanning, MRI, MR venography, or angiography.
Treatment includes anticonvulsant drugs if seizures have occurred and antiedema agents (eg, dexamethasone, 4 mg four times daily and continued as necessary) or other measures to reduce intracranial pressure. Anticoagulation with dose-adjusted intravenous heparin followed by oral anticoagulation for 6 months reduces morbidity and mortality of venous sinus thrombosis. In cases refractory to heparin, endovascular techniques including catheter-directed thrombolytic therapy (urokinase) and thrombectomy, are sometimes helpful.
P.1023
Biousse V et al: Cerebral venous thrombosis. Curr Treat Options Neurol 2003;5:409.
Cakmak S et al: Cerebral venous thrombosis: clinical outcome and systematic screening of prothrombotic factors. Neurology 2003;60:1175.
8. Spinal Cord Vascular Diseases
![]() Essentials of Diagnosis
Essentials of Diagnosis
Sudden onset of back or limb pain and neurologic deficit in limbs.
Motor, sensory, or reflex changes in limbs depending on level of lesion.
Imaging studies distinguish between infarct and hematoma.
Infarction of the Spinal Cord
Infarction of the spinal cord is rare. It occurs only in the territory of the anterior spinal artery because this vessel, which supplies the anterior two-thirds of the cord, is itself supplied by only a limited number of feeders. Infarction usually results from interrupted flow in one or more of these feeders, eg, with aortic dissection, aortography, polyarteritis, or severe hypotension, or after surgical resection of the thoracic aorta. The paired posterior spinal arteries, by contrast, are supplied by numerous arteries at different levels of the cord.
Since the anterior spinal artery receives numerous feeders in the cervical region, infarcts almost always occur caudally. Clinical presentation is characterized by acute onset of flaccid, areflexive paraplegia that evolves after a few days or weeks into a spastic paraplegia with extensor plantar responses. There is an accompanying dissociated sensory loss, with impairment of appreciation of pain and temperature but preservation of sensations of vibration and position. Treatment is symptomatic.
Goodin DS: Neurological complications of aortic disease and surgery. In: Neurology and General Medicine, 3rd ed. Aminoff MJ (editor). Churchill Livingstone, 2001.
Epidural or Subdural Hemorrhage
Epidural or subdural hemorrhage may lead to sudden severe back pain followed by an acute compressive myelopathy necessitating urgent spinal MRI or myelography and surgical evacuation. It may occur in patients with bleeding disorders or those who are taking anticoagulant drugs, sometimes following trauma or lumbar puncture. Epidural hemorrhage may also be related to a vascular malformation or tumor deposit.
Arteriovenous Malformation of the Spinal Cord
Arteriovenous malformations of the cord are congenital lesions that present with spinal subarachnoid hemorrhage or myeloradiculopathy. Since most of these malformations are located in the thoracolumbar region, they lead to motor and sensory disturbances in the legs and to sphincter disorders. Pain in the legs or back is often severe. Examination reveals an upper, lower, or mixed motor deficit in the legs; sensory deficits are also present and are usually extensive, although occasionally they are confined to radicular distribution. Cervical arteriovenous malformations lead also to symptoms and signs in the arms. Spinal MRI may not detect the arteriovenous malformation, and negative findings do not exclude the diagnosis. In general, the diagnosis is suggested at myelography (performed with the patient prone and supine) when serpiginous filling defects due to enlarged vessels are found. Selective spinal arteriography confirms the diagnosis. Most lesions are extramedullary, are posterior to the cord (lying either intra- or extradurally), and can easily be treated by ligation of feeding vessels and excision of the fistulous anomaly or by embolization procedures. Delay in treatment may lead to increased and irreversible disability or to death from recurrent subarachnoid hemorrhage.
Intracranial & Spinal Space-Occupying Lesions
1. Primary Intracranial Tumors
![]() Essentials of Diagnosis
Essentials of Diagnosis
Generalized or focal disturbance of cerebral function, or both.
Increased intracranial pressure in some patients.
Neuroradiologic evidence of space-occupying lesion.
General Considerations
Half of all primary intracranial neoplasms (Table 24-5) are gliomas and the remainder meningiomas, pituitary adenomas, neurofibromas, and other tumors. Certain tumors, especially neurofibromas, hemangioblastomas, and retinoblastomas, may have a familial basis, and congenital factors bear on the development of craniopharyngiomas. Tumors may occur at any age, but certain gliomas show particular age predilections (Table 24-5).
Table 24-5. Primary intracranial tumors. | |||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Clinical Findings
A. Symptoms and Signs
Intracranial tumors may lead to a generalized disturbance of cerebral function and to symptoms and signs of increased intracranial pressure. In consequence, there may be personality changes, intellectual decline, emotional lability, seizures, headaches, nausea, and malaise.
P.1024
P.1025
If the pressure is increased in a particular cranial compartment, brain tissue may herniate into a compartment with lower pressure. The most familiar syndrome is herniation of the temporal lobe uncus through the tentorial hiatus, which causes compression of the third cranial nerve, midbrain, and posterior cerebral artery. The earliest sign of this is ipsilateral pupillary dilation, followed by stupor, coma, decerebrate posturing, and respiratory arrest. Another important herniation syndrome consists of displacement of the cerebellar tonsils through the foramen magnum, which causes medullary compression leading to apnea, circulatory collapse, and death. Other herniation syndromes are less common and of less clear clinical importance.
Intracranial tumors also lead to focal deficits depending on their location.
1. Frontal lobe lesions
Tumors of the frontal lobe often lead to progressive intellectual decline, slowing of mental activity, personality changes, and contralateral grasp reflexes. They may lead to expressive aphasia if the posterior part of the left inferior frontal gyrus is involved. Anosmia may also occur as a consequence of pressure on the olfactory nerve. Precentral lesions may cause focal motor seizures or contralateral pyramidal deficits.
2. Temporal lobe lesions
Tumors of the uncinate region may be manifested by seizures with olfactory or gustatory hallucinations, motor phenomena such as licking or smacking of the lips, and some impairment of external awareness without actual loss of consciousness. Temporal lobe lesions also lead to depersonalization, emotional changes, behavioral disturbances, sensations of d j vu or jamais vu, micropsia or macropsia (objects appear smaller or larger than they are), visual field defects (crossed upper quadrantanopia), and auditory illusions or hallucinations. Left-sided lesions may lead to dysnomia and receptive aphasia, while right-sided involvement sometimes disturbs the perception of musical notes and melodies.
3. Parietal lobe lesions
Tumors in this location characteristically cause contralateral disturbances of sensation and may cause sensory seizures, sensory loss or inattention, or some combination of these symptoms. The sensory loss is cortical in type and involves postural sensibility and tactile discrimination, so that the appreciation of shape, size, weight, and texture is impaired. Objects placed in the hand may not be recognized (astereognosis). Extensive parietal lobe lesions may produce contralateral hyperpathia and spontaneous pain (thalamic syndrome). Involvement of the optic radiation leads to a contralateral homonymous field defect that sometimes consists solely of lower quadrantanopia. Lesions of the left angular gyrus cause Gerstmann's syndrome (a combination of alexia, agraphia, acalculia, right-left confusion, and finger agnosia), whereas involvement of the left submarginal gyrus causes ideational apraxia. Anosognosia (the denial, neglect, or rejection of a paralyzed limb) is seen in patients with lesions of the nondominant (right) hemisphere. Constructional apraxia and dressing apraxia may also occur with right-sided lesions.
4. Occipital lobe lesions
Tumors of the occipital lobe characteristically produce crossed homonymous hemianopia or a partial field defect. With left-sided or bilateral lesions, there may be visual agnosia both for objects and for colors, while irritative lesions on either side can cause unformed visual hallucinations. Bilateral occipital lobe involvement causes cortical blindness in which there is preservation of pupillary responses to light and lack of awareness of the defect by the patient. There may also be loss of color perception, prosopagnosia (inability to identify a familiar face), simultagnosia (inability to integrate and interpret a composite scene as opposed to its individual elements), and Balint's syndrome (failure to turn the eyes to a particular point in space, despite preservation of spontaneous and reflex eye movements). The denial of blindness or a field defect constitutes Anton's syndrome.
5. Brainstem and cerebellar lesions
Brainstem lesions lead to cranial nerve palsies, ataxia, incoordination, nystagmus, and pyramidal and sensory deficits in the limbs on one or both sides. Intrinsic brainstem tumors, such as gliomas, tend to produce an increase in intracranial pressure only late in their course. Cerebellar tumors produce marked ataxia of the trunk if the vermis cerebelli is involved and ipsilateral appendicular deficits (ataxia, incoordination and hypotonia of the limbs) if the cerebellar hemispheres are affected.
6. False localizing signs
Tumors may lead to neurologic signs other than by direct compression or infiltration, thereby leading to errors of clinical localization. These false localizing signs include third or sixth nerve palsy and bilateral extensor plantar responses produced by herniation syndromes, and an extensor plantar response occurring ipsilateral to a hemispheric tumor as a result of compression of the opposite cerebral peduncle against the tentorium.
B. Imaging
CT scanning or MRI with gadolinium enhancement may detect the lesion and may also define its location, shape, and size; the extent to which normal anatomy is distorted; and the degree of any associated cerebral edema or mass effect. CT scanning is less helpful with tumors in the posterior fossa, but MRI is of particular value there. The characteristic appearance of meningiomas on CT scanning is virtually diagnostic, ie, a lesion in a typical site (parasagittal and sylvian regions, olfactory groove, sphenoidal ridge, tuberculum sellae) that appears as a homogeneous area of increased density in noncontrast CT scans and enhances uniformly with contrast.
Arteriography may show stretching or displacement of normal cerebral vessels by the tumor and the presence of tumor vascularity. The presence of an avascular mass is a nonspecific finding that could be due to tumor, hematoma, abscess, or any space-occupying lesion. In patients with normal hormone levels
P.1026
and an intrasellar mass, angiography is necessary to distinguish with confidence between a pituitary adenoma and an arterial aneurysm.
C. Laboratory and Other Studies
The electroencephalogram provides supporting information concerning cerebral function and may show either a focal disturbance due to the neoplasm or a more diffuse change reflecting altered mental status. Lumbar puncture is rarely necessary; the findings are seldom diagnostic, and the procedure carries the risk of causing a herniation syndrome.
Treatment
Treatment depends on the type and site of the tumor (Table 24-5) and the condition of the patient. Complete surgical removal may be possible if the tumor is extra-axial (eg, meningioma, acoustic neuroma) or is not in a critical or inaccessible region of the brain (eg, cerebellar hemangioblastoma). Surgery also permits the diagnosis to be verified and may be beneficial in reducing intracranial pressure and relieving symptoms even if the neoplasm cannot be completely removed. Clinical deficits are sometimes due in part to obstructive hydrocephalus, in which case simple surgical shunting procedures often produce dramatic benefit. In patients with malignant gliomas, radiation therapy increases median survival rates regardless of any preceding surgery, and its combination with chemotherapy provides additional benefit. Indications for irradiation in the treatment of patients with other primary intracranial neoplasms depend on tumor type and accessibility and the feasibility of complete surgical removal. Corticosteroids help reduce cerebral edema and are usually started before surgery. Herniation is treated with intravenous dexamethasone (10 20 mg as a bolus, followed by 4 mg every 6 hours) and intravenous mannitol (20% solution given in a dose of 1.5 g/kg over about 30 minutes). Anticonvulsants are also commonly administered in standard doses (see Table 24-3) but are not indicated for prophylaxis in patients who have no history of seizures. For those patients whose disease deteriorates despite treatment, palliative care is important (see Chapter 5).
Behin A et al: Primary brain tumours in adults. Lancet 2003; 361:323.
Sarin R et al: Medical decompressive therapy for primary and metastatic intracranial tumours. Lancet Neurol 2003;2: 357.
Sirven JI et al: Seizure prophylaxis in patients with brain tumors: a meta-analysis. Mayo Clin Proc 2004;79:1489.
Taillibert S et al: Palliative care in patients with primary brain tumors. Curr Opin Oncol 2004;16:587.
Wen PY et al: Malignant gliomas. Curr Neurol Neurosci Rep 2004;4:218.
Whittle IR: Surgery for gliomas. Curr Opin Neurol 2002;15:663.
Wrensch M et al: Epidemiology of primary brain tumors: current concepts and review of the literature. Neuro-oncol 2002;4:278.
2. Metastatic Intracranial Tumors
Cerebral Metastases
Metastatic brain tumors present in the same way as other cerebral neoplasms, ie, with increased intracranial pressure, with focal or diffuse disturbance of cerebral function, or with both of these manifestations. Indeed, in patients with a single cerebral lesion, the metastatic nature of the lesion may only become evident on histopathologic examination. In other patients, there is evidence of widespread metastatic disease, or an isolated cerebral metastasis develops during treatment of the primary neoplasm.
The most common source of intracranial metastasis is carcinoma of the lung; other primary sites are the breast, kidney, and gastrointestinal tract. Most cerebral metastases are located supratentorially. Laboratory and radiologic studies used to evaluate patients with metastases are those described for primary neoplasms. They include MRI and CT scanning performed both with and without contrast material. Lumbar puncture is necessary only in patients with suspected carcinomatous meningitis (see below). In patients with verified cerebral metastasis from an unknown primary, investigation is guided by symptoms and signs. In women, mammography is indicated; in men under 50, germ cell origin is sought since both have therapeutic implications.
In patients with only a single cerebral metastasis who are otherwise well, it may be possible to remove the lesion and then treat with irradiation; the latter may also be selected as the sole treatment. In patients with multiple metastases or widespread systemic disease, the prognosis is poor; stereotactic radiotherapy may help in some instances, but in others treatment is palliative only.
Kaal EC et al: Therapeutic management of brain metastases. Lancet Neurol 2005;4:289.
Leptomeningeal Metastases (Carcinomatous Meningitis)
The neoplasms metastasizing most commonly to the leptomeninges are carcinoma of the breast, lymphomas, and leukemia. Leptomeningeal metastases lead to multifocal neurologic deficits, which may be associated with infiltration of cranial and spinal nerve roots, direct invasion of the brain or spinal cord, obstructive hydrocephalus, or some combination of these factors.
The diagnosis is confirmed by examination of the cerebrospinal fluid. Findings may include elevated cerebrospinal fluid pressure, pleocytosis, increased protein concentration, and decreased glucose concentration. Cytologic studies may indicate that malignant cells are present; if not, spinal tap should be repeated at least twice to obtain further samples for analysis.
CT scans showing contrast enhancement in the basal cisterns or showing hydrocephalus without any evidence of a mass lesion support the diagnosis. Gadolinium-enhanced MRI frequently shows enhancing
P.1027
foci in the leptomeninges. Myelography may show deposits on multiple nerve roots.
Treatment is by irradiation to symptomatic areas, combined with intrathecal methotrexate. The long-term prognosis is poor only about 10% of patients survive for 1 year and palliative care is therefore important (see Chapter 5).
3. Intracranial Mass Lesions in AIDS Patients
Primary cerebral lymphoma is a common complication in patients with AIDS. This leads to disturbances in cognition or consciousness, focal motor or sensory deficits, aphasia, seizures, and cranial neuropathies. Similar clinical disturbances may result from cerebral toxoplasmosis, which is also a common complication in patients with AIDS (see Chapters 31 and 35). Neither CT nor MRI findings distinguish these two disorders, and serologic tests for toxoplasmosis are unreliable in AIDS patients. Accordingly, for neurologically stable patients, a trial of treatment for toxoplasmosis with sulfadiazine (100 mg/kg/d up to 8 g/d in four divided doses) and pyrimethamine (75 mg/d for 3 days, then 25 mg/d) is recommended for 3 weeks; the imaging studies are then repeated, and if any lesion has improved, the regimen is continued indefinitely. If any lesion does not improve, cerebral biopsy is necessary. Primary cerebral lymphoma is treated with whole-brain irradiation.
Cryptococcal meningitis is a common opportunistic infection in AIDS patients. Clinically, it may resemble cerebral toxoplasmosis or lymphoma, but cranial CT scans are usually normal. The diagnosis is made on the basis of cerebrospinal fluid studies, with positive India ink staining in 75 80% and cryptococcal antigen tests in 95% of cases. Treatment is with amphotericin B plus flucytosine, as set forth in Table 36-1, followed by fluconazole.
Bicanic T et al: Cryptococcal meningitis. Br Med Bull 2005; 72:99.
4. Primary & Metastatic Spinal Tumors
Approximately 10% of spinal tumors are intramedullary. Ependymoma is the most common type of intramedullary tumor; the remainder are other types of glioma. Extramedullary tumors may be extradural or intradural in location. Among the primary extramedullary tumors, neurofibromas and meningiomas are relatively common, are benign, and may be intradural or extradural. Carcinomatous metastases, lymphomatous or leukemic deposits, and myeloma are usually extradural; in the case of metastases, the prostate, breast, lung, and kidney are common primary sites.
Tumors may lead to spinal cord dysfunction by direct compression, by ischemia secondary to arterial or venous obstruction, and, in the case of intramedullary lesions, by invasive infiltration.
Clinical Findings
A. Symptoms and Signs
Symptoms usually develop insidiously. Pain is often conspicuous with extradural lesions; is characteristically aggravated by coughing or straining; may be radicular, localized to the back, or felt diffusely in an extremity; and may be accompanied by motor deficits, paresthesias, or numbness, especially in the legs. When sphincter disturbances occur, they are usually particularly disabling. Pain, however, often precedes specific neurologic symptoms from epidural metastases.
Examination may reveal localized spinal tenderness. A segmental lower motor neuron deficit or dermatomal sensory changes (or both) are sometimes found at the level of the lesion, while an upper motor neuron deficit and sensory disturbance are found below it.
B. Imaging
Findings on plain radiography of the spine may be normal but are commonly abnormal when there are metastatic deposits. CT myelography or MRI may be necessary to identify and localize the site of cord compression. The combination of known tumor elsewhere in the body, back pain, and either abnormal plain films of the spine or neurologic signs of cord compression is an indication to perform these studies on an urgent basis. Some clinicians proceed to myelography based solely on new back pain in a cancer patient. If a complete block is present at lumbar myelography, a cisternal myelogram is performed to determine the upper level of the block and to investigate the possibility of block higher in the cord.
C. Laboratory Findings
The cerebrospinal fluid removed at myelography is often xanthochromic and contains a greatly increased protein concentration with normal cell content and glucose concentration.
Treatment
Intramedullary tumors are treated by decompression and surgical excision (when feasible) and by irradiation. The prognosis depends on the cause and severity of cord compression before it is relieved.
Treatment of epidural spinal metastases consists of irradiation, irrespective of cell type. Dexamethasone is also given in a high dosage (eg, 25 mg four times daily for 3 days, followed by rapid tapering of the dosage, depending on response) to reduce cord swelling and relieve pain. Surgical decompression is reserved for patients with tumors that are unresponsive to irradiation or have previously been irradiated and for cases in which there is some uncertainty about the diagnosis. The long-term outlook is poor, but radiation treatment may at least delay the onset of major disability.
P.1028
5. Brain Abscess
![]() Essentials of Diagnosis
Essentials of Diagnosis
Symptoms and signs of expanding intracranial mass.
May be signs of primary infection or congenital heart disease.
Fever may be absent.
General Considerations
Brain abscess presents as an intracranial space-occupying lesion and arises as a sequela of disease of the ear or nose, may be a complication of infection elsewhere in the body, or may result from infection introduced intracranially by trauma or surgical procedures. The most common infective organisms are streptococci, staphylococci, and anaerobes; mixed infections are not uncommon.
Clinical Findings
A. Symptoms and Signs
Headache, drowsiness, inattention, confusion, and seizures are early symptoms, followed by signs of increasing intracranial pressure and then a focal neurologic deficit. There may be little or no systemic evidence of infection.
B. Imaging
A CT scan of the head characteristically shows an area of contrast enhancement surrounding a low-density core. Similar abnormalities may be found in patients with metastatic neoplasms. MRI findings often permit earlier recognition of focal cerebritis or an abscess. Arteriography indicates the presence of a space-occupying lesion, which appears as an avascular mass with displacement of normal cerebral vessels, but this procedure provides no clue to the nature of the lesion. Examination of the cerebrospinal fluid does not help in diagnosis and may precipitate a herniation syndrome.
C. Treatment
Treatment consists of intravenous antibiotics, combined with surgical drainage (aspiration or excision) if necessary to reduce the mass effect, or sometimes to establish the diagnosis. Abscesses smaller than 2 cm can often be cured medically. Broad-spectrum antibiotics are used if the infecting organism is unknown. A common regimen is penicillin G (2 million units every 2 hours intravenously) plus either chloramphenicol (1 2 g intravenously every 6 hours), metronidazole (750 mg intravenously every 6 hours), or both. Nafcillin is added if Staphylococcus aureus infection is suspected. Antimicrobial treatment is usually continued parenterally for 6 8 weeks, followed by orally for a further 2 3 weeks. The patient should be monitored by serial CT scans or MRI every 2 weeks and at deterioration. Dexamethasone (4 25 mg four times daily, depending on severity, followed by tapering of dose, depending on response) may reduce any associated edema, but intravenous mannitol is sometimes required.
Kastrup O et al: Neuroimaging of infections. NeuroRx 2005;2: 324.
Nonmetastatic Neurologic Complications of Malignant Disease
A variety of nonmetastatic neurologic complications of malignant disease (see Table 40-6) can be recognized. Metabolic encephalopathy due to electrolyte abnormalities, infections, drug overdose, or the failure of some vital organ may be reflected by drowsiness, lethargy, restlessness, insomnia, agitation, confusion, stupor, or coma. The mental changes are usually associated with tremor, asterixis, and multifocal myoclonus. The electroencephalogram is generally diffusely slowed. Laboratory studies are necessary to detect the cause of the encephalopathy, which must then be treated appropriately.
Immune suppression resulting from either the malignant disease or its treatment (eg, by chemotherapy) predisposes patients to brain abscess, progressive multifocal leukoencephalopathy, meningitis, herpes zoster infection, and other opportunistic infectious diseases. Moreover, an overt or occult cerebrospinal fluid fistula, as occurs with some tumors, may also increase the risk of infection. CT scanning aids in the early recognition of a brain abscess, but metastatic brain tumors may have a similar appearance. Examination of the cerebrospinal fluid is essential in the evaluation of patients with meningitis but is of no help in the diagnosis of brain abscess.
Table 24-6. Some anticholinergic antiparkinsonian drugs. | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||
P.1029
Cerebrovascular disorders that cause neurologic complications in patients with systemic cancer include nonbacterial thrombotic endocarditis and septic embolization. Cerebral, subarachnoid, or subdural hemorrhages may occur in patients with myelogenous leukemia and may be found in association with metastatic tumors, especially malignant melanoma. Spinal subdural hemorrhage sometimes occurs after lumbar puncture in patients with marked thrombocytopenia.
Disseminated intravascular coagulation occurs most commonly in patients with acute promyelocytic leukemia or with some adenocarcinomas and is characterized by a fluctuating encephalopathy, often with associated seizures, that frequently progresses to coma or death. There may be few accompanying neurologic signs. Venous sinus thrombosis, which usually presents with convulsions and headaches, may also occur in patients with leukemia or lymphoma. Examination commonly reveals papilledema and focal or diffuse neurologic signs. Anticonvulsants, anticoagulants, and drugs to lower the intracranial pressure may be of value.
Paraneoplastic cerebellar degeneration occurs most commonly in association with carcinoma of the lung. Symptoms may precede those due to the neoplasm itself, which may be undetected for several months or even longer. Typically, there is a pancerebellar syndrome causing dysarthria, nystagmus, and ataxia of the trunk and limbs. The disorder probably has an autoimmune basis. Treatment is of the underlying malignant disease.
Encephalopathy, characterized by impaired recent memory, disturbed affect, hallucinations, and seizures, occurs in some patients with carcinomas. The cerebrospinal fluid is often abnormal. EEGs may show diffuse slow-wave activity, especially over the temporal regions. Pathologic changes are most marked in the inferomedian portions of the temporal lobes. There is no specific treatment.
Malignant disease may be associated with sensorimotor polyneuropathy and less commonly with pure sensory neuropathy (ie, dorsal root ganglionitis) or autonomic neuropathy. A subacute motor neuronopathy may be associated with lymphomas.
Dermatomyositis or a myasthenic syndrome may be seen in patients with underlying carcinoma (see Chapter 20). The myasthenic syndrome may have an autoimmune basis and differs clinically from myasthenia gravis.
Bataller L et al: Paraneoplastic neurologic syndromes. Neurol Clin 2003;21:221.
Pseudotumor Cerebri (Benign Intracranial Hypertension)
![]() Essentials of Diagnosis
Essentials of Diagnosis
Headache, worse on straining.
Visual obscurations or diplopia may occur.
Level of consciousness may be impaired.
Other deficits depend on cause of intracranial hypertension or on herniation syndrome.
Examination reveals papilledema.
General Considerations
There are many causes of pseudotumor cerebri. Thrombosis of the transverse venous sinus as a noninfectious complication of otitis media or chronic mastoiditis is one cause, and sagittal sinus thrombosis may lead to a clinically similar picture. Other causes include chronic pulmonary disease, endocrine disturbances such as hypoparathyroidism or Addison's disease, vitamin A toxicity, and the use of tetracycline or oral contraceptives. Cases have also followed withdrawal of corticosteroids after long-term use. In many instances, however, no specific cause can be found, and the disorder remits spontaneously after several months.
Clinical Findings
A. Symptoms and Signs
Symptoms of pseudotumor cerebri consist of headache, diplopia, and other visual disturbances due to papilledema and abducens nerve dysfunction. Examination reveals the papilledema and some enlargement of the blind spots, but patients otherwise look well.
B. Imaging
Investigations reveal no evidence of a space-occupying lesion, and the CT scan shows small or normal ventricles. MR venography is helpful in screening for thrombosis of the intracranial venous sinuses.
C. Laboratory Findings
Lumbar puncture confirms the presence of intracranial hypertension, but the cerebrospinal fluid is normal. Laboratory studies help exclude some of the other causes mentioned earlier.
Treatment
Untreated pseudotumor cerebri leads to secondary optic atrophy and permanent visual loss. Acetazolamide (250 mg orally three times daily) reduces formation of cerebrospinal fluid and can be used to start treatment. Oral corticosteroids (eg, prednisone, 60 80 mg daily) may also be necessary. Obese patients should be advised to lose weight. Repeated lumbar puncture to lower the intracranial pressure by removal of cerebrospinal fluid is effective, but pharmacologic approaches to treatment are now more satisfactory. Treatment is monitored by checking visual acuity and visual fields, funduscopic appearance, and pressure of the cerebrospinal fluid.
P.1030
If medical treatment fails to control the intracranial pressure, surgical placement of a lumboperitoneal or other shunt or subtemporal decompression or optic nerve sheath fenestration should be undertaken to preserve vision.
In addition to the above measures, any specific cause of pseudotumor cerebri requires appropriate treatment. Thus, hormone therapy should be initiated if there is an underlying endocrine disturbance. Discontinuing the use of tetracycline, oral contraceptives, or vitamin A will allow for resolution of pseudotumor cerebri due to these agents. If corticosteroid withdrawal is responsible, the medication should be reintroduced and then tapered more gradually.
Friedman DI: Pseudotumor cerebri. Neurol Clin 2004;22:99.
Selected Neurocutaneous Diseases
Tuberous Sclerosis
Tuberous sclerosis may occur sporadically or on a familial basis with autosomal dominant inheritance. The responsible gene is located on the long arm of chromosome 9 in at least some cases. Its pathogenesis is unknown. Neurologic presentation is with seizures and progressive psychomotor retardation beginning in early childhood. The cutaneous abnormality, adenoma sebaceum, becomes manifest usually between 5 and 10 years of age and typically consists of reddened nodules on the face (cheeks, nasolabial folds, sides of the nose, and chin) and sometimes on the forehead and neck. Other typical cutaneous lesions include subungual fibromas, shagreen patches (leathery plaques of subepidermal fibrosis, situated usually on the trunk), and leaf-shaped hypopigmented spots. Associated abnormalities include retinal lesions and tumors, benign rhabdomyomas of the heart, lung cysts, benign tumors in the viscera, and bone cysts.
The disease is slowly progressive and leads to increasing mental deterioration. There is no specific treatment, but anticonvulsant drugs may help in controlling seizures.
Neurofibromatosis
Neurofibromatosis may occur either sporadically or on a familial basis with autosomal dominant inheritance. Two distinct forms are recognized: Type 1 (Recklinghausen's disease) is characterized by multiple hyperpigmented macules and neurofibromas and type 2 by eighth nerve tumors, often accompanied by other intracranial or intraspinal tumors. Among familial cases, the gene for type 1 is located on chromosome 17 and that for type 2 on chromosome 22.
Neurologic presentation is usually with symptoms and signs of tumor. Multiple neurofibromas characteristically are present and may involve spinal or cranial nerves, especially the eighth nerve. Examination of the superficial cutaneous nerves usually reveals palpable mobile nodules. In some cases, there is an associated marked overgrowth of subcutaneous tissues (plexiform neuromas), sometimes with an underlying bony abnormality. Associated cutaneous lesions include axillary freckling and patches of cutaneous pigmentation (caf au lait spots). Malignant degeneration of neurofibromas occasionally occurs and may lead to peripheral sarcomas. Meningiomas, gliomas (especially optic nerve gliomas), bone cysts, pheochromocytomas, scoliosis, and obstructive hydrocephalus may also occur.
It may be possible to correct disfigurement by plastic surgery. Intraspinal or intracranial tumors and tumors of peripheral nerves should be treated surgically if they are producing symptoms.
Neff BA et al: Current concepts in the evaluation and treatment of neurofibromatosis type ll. Otolaryngol Clin North Am 2005;38:671.
Reynolds RM et al: Von Recklinghausen's neurofibromatosis: neurofibromatosis type 1. Lancet 2003;361:1552.
Sturge-Weber Syndrome
Sturge-Weber syndrome consists of a congenital, usually unilateral, cutaneous capillary angioma involving the upper face, leptomeningeal angiomatosis, and, in many patients, choroidal angioma. It has no sex predilection and usually occurs sporadically. The cutaneous angioma sometimes has a more extensive distribution over the head and neck and is often quite disfiguring, especially if there is associated overgrowth of connective tissue. Focal or generalized seizures are the usual neurologic presentation and may commence at any age. There may be contralateral homonymous hemianopia, hemiparesis and hemisensory disturbance, ipsilateral glaucoma, and mental subnormality. Skull x-rays taken after the first 2 years of life usually reveal gyriform ( tramline ) intracranial calcification, especially in the parieto-occipital region, due to mineral deposition in the cortex beneath the intracranial angioma.
Treatment is aimed at controlling seizures pharmacologically. Ophthalmologic advice should be sought concerning the management of choroidal angioma and of increased intraocular pressure.
Movement Disorders
1. Benign Essential (Familial) Tremor
![]() Essentials of Diagnosis
Essentials of Diagnosis
Postural tremor of hands, head, or voice.
Family history common.
May improve temporarily with alcohol.
No abnormal findings other than tremor.
P.1031
General Considerations
The cause of benign essential tremor is uncertain, but it is sometimes inherited in an autosomal dominant manner. Responsible genes have been identified at 3q13 and 2p22-p25.
Clinical Findings
A. Symptoms and Signs
Tremor may begin at any age and is enhanced by emotional stress. The tremor usually involves one or both hands, the head, or the hands and head, while the legs tend to be spared. Examination reveals no other abnormalities. Ingestion of a small quantity of alcohol commonly provides remarkable but short-lived relief by an unknown mechanism.
Although the tremor may become more conspicuous with time, it generally leads to little disability. Occasionally, it interferes with manual skills and leads to impairment of handwriting. Speech may also be affected if the laryngeal muscles are involved.
B. Treatment
Treatment is often unnecessary. When it is required because of disability, propranolol may be helpful but will need to be continued indefinitely in daily doses of 60 240 mg. However, intermittent therapy is sometimes useful in patients whose tremor becomes exacerbated in specific predictable situations. Primidone may be helpful when propranolol is ineffective, but patients with essential tremor are often very sensitive to it. Therefore, the starting dose is 50 mg daily, and the daily dose is increased by 50 mg every 2 weeks depending on the patient's response; a maintenance dose of 125 mg three times daily is commonly effective. Occasional patients do not respond to these measures but are helped by alprazolam (up to 3 mg daily in divided doses), clozapine (30 50 mg twice daily), or mirtazapine (15 or 30 mg at night). Benefit has been reported with topiramate titrated up to a dose of 400 mg daily over about 8 weeks.
Disabling tremor unresponsive to medical treatment may be helped by contralateral thalamotomy. Unilateral high-frequency thalamic stimulation is an alternative approach that is equally effective, is associated with only mild and transient side effects, and is therefore preferred. Bilateral thalamotomy has significant morbidity, whereas the risks of bilateral stimulation are appreciably lower.
Louis ED: Essential tremor. Lancet Neurol 2005;4:100.
Pathwa R et al: Essential tremor: differential diagnosis and current therapy. Am J Med 2003;115:134.
Sydow O et al: Multicentre European study of thalamic stimulation in essential tremor: a six year follow up. J Neurol Neurosurg Psychiatry 2003;74:1387.
2. Parkinsonism
![]() Essentials of Diagnosis
Essentials of Diagnosis
Any combination of tremor, rigidity, bradykinesia, progressive postural instability.
Seborrhea of skin quite common.
Mild intellectual deterioration may occur.
General Considerations
Parkinsonism is a relatively common disorder that occurs in all ethnic groups, with an approximately equal sex distribution. The most common variety, idiopathic Parkinson's disease (paralysis agitans), begins most often between 45 and 65 years of age.
Etiology
Parkinsonism may rarely occur on a familial basis, and the parkinsonian phenotype may result from mutations of several different genes. Postencephalitic parkinsonism is becoming increasingly rare. Exposure to certain toxins (eg, manganese dust, carbon disulfide) and severe carbon monoxide poisoning may lead to parkinsonism. Typical parkinsonism has occurred in individuals who have taken 1-methyl-4-phenyl-1,2,5,6-tetrahydropyridine (MPTP) for recreational purposes. This compound is converted in the body to a neurotoxin that selectively destroys dopaminergic neurons in the substantia nigra. Reversible parkinsonism may develop in patients receiving neuroleptic drugs (see Chapter 25), reserpine, or metoclopramide. Only rarely is hemiparkinsonism the presenting feature of a progressive space-occupying lesion.
In idiopathic parkinsonism, dopamine depletion due to degeneration of the dopaminergic nigrostriatal system leads to an imbalance of dopamine and acetylcholine, which are neurotransmitters normally present in the corpus striatum. Treatment is directed at redressing this imbalance by blocking the effect of acetylcholine with anticholinergic drugs or by the administration of levodopa, the precursor of dopamine.
Clinical Findings
Tremor, rigidity, bradykinesia, and postural instability are the cardinal features of parkinsonism and may be present in any combination. There may also be a mild decline in intellectual function. The tremor of about four to six cycles per second is most conspicuous at rest, is enhanced by emotional stress, and is often less severe during voluntary activity. Although it may ultimately be present in all limbs, the tremor is commonly confined to one limb or to the limbs on one side for months or years before it becomes more generalized. In some patients, tremor is absent.
P.1032
Rigidity (an increase in resistance to passive movement) is responsible for the characteristically flexed posture seen in many patients, but the most disabling symptoms of parkinsonism are due to bradykinesia, manifested as a slowness of voluntary movement and a reduction in automatic movements such as swinging of the arms while walking. Curiously, however, effective voluntary activity may briefly be regained during an emergency (eg, the patient is able to leap aside to avoid an oncoming motor vehicle).
Clinical diagnosis of the well-developed syndrome is usually simple. The patient has a relatively immobile face with widened palpebral fissures, infrequent blinking, and a certain fixity of facial expression. Seborrhea of the scalp and face is common. There is often mild blepharoclonus, and a tremor may be present about the mouth and lips. Repetitive tapping (about twice per second) over the bridge of the nose produces a sustained blink response (Myerson's sign). Other findings may include saliva drooling from the mouth, perhaps due to impairment of swallowing; soft and poorly modulated voice; a variable rest tremor and rigidity in some or all of the limbs; slowness of voluntary movements; impairment of fine or rapidly alternating movements; and micrographia. There is typically no muscle weakness (provided that sufficient time is allowed for power to be developed) and no alteration in the tendon reflexes or plantar responses. It is difficult for the patient to arise from a sitting position and begin walking. The gait itself is characterized by small shuffling steps and a loss of the normal automatic arm swing; there may be unsteadiness on turning, difficulty in stopping, and a tendency to fall.
Differential Diagnosis
Diagnostic problems may occur in mild cases, especially if tremor is minimal or absent. For example, mild hypokinesia or slight tremor is commonly attributed to old age. Depression, with its associated expressionless face, poorly modulated voice, and reduction in voluntary activity, can be difficult to distinguish from mild parkinsonism, especially since the two disorders may coexist; in some cases, a trial of antidepressant drug therapy is necessary. The family history, the character of the tremor, and lack of other neurologic signs should distinguish essential tremor from parkinsonism. Wilson's disease can be distinguished by its early age at onset, the presence of other abnormal movements, Kayser-Fleischer rings, and chronic hepatitis, and by increased concentrations of copper in the tissues. Huntington's disease presenting with rigidity and bradykinesia may be mistaken for parkinsonism unless the family history and accompanying dementia are recognized. In Shy-Drager syndrome (also called multisystem atrophy), the clinical features of parkinsonism are accompanied by autonomic insufficiency (leading to postural hypotension, anhidrosis, disturbances of sphincter control, impotence, etc) and more widespread neurologic deficits (pyramidal, lower motor neuron, or cerebellar signs). In progressive supranuclear palsy, bradykinesia and rigidity are accompanied by a supranuclear disorder of eye movements, pseudobulbar palsy, and axial dystonia. Creutzfeldt-Jakob disease may be accompanied by features of parkinsonism, but dementia is usual, myoclonic jerking is common, ataxia and pyramidal signs may be conspicuous, and the electroencephalographic findings are usually characteristic. In cortical-basal ganglionic degeneration, parkinsonism is accompanied by conspicuous signs of cortical dysfunction (eg, apraxia, sensory inattention, dementia, aphasia).
Treatment
Treatment is symptomatic. No therapy has been shown to slow disease progression, but trials of several putative neuroprotective agents are in progress, as are various trials of gene therapy.
A. Medical Measures
Drug treatment is not required early in the course of parkinsonism, but the nature of the disorder and the availability of medical treatment for use when necessary should be discussed with the patient.
1. Amantadine
Patients with mild symptoms but no disability may be helped by amantadine. This drug improves all of the clinical features of parkinsonism, but its mode of action is unclear. Side effects include restlessness, confusion, depression, skin rashes, edema, nausea, constipation, anorexia, postural hypotension, and disturbances of cardiac rhythm. However, these are relatively uncommon with the usual dose (100 mg twice daily).
2. Anticholinergic drugs
Anticholinergics are more helpful in alleviating tremor and rigidity than bradykinesia. Treatment is started with a small dose (Table 24-6) and gradually increased until benefit occurs or side effects limit further increments. If treatment is ineffective, the drug is gradually withdrawn and another preparation then tried.
Common side effects include dryness of the mouth, nausea, constipation, palpitations, cardiac arrhythmias, urinary retention, confusion, agitation, restlessness, drowsiness, mydriasis, increased intraocular pressure, and defective accommodation.
Anticholinergic drugs are contraindicated in patients with prostatic hyperplasia, narrow-angle glaucoma, or obstructive gastrointestinal disease and are often tolerated poorly by the elderly.
3. Levodopa
Levodopa, which is converted in the body to dopamine, improves all of the major features of parkinsonism, including bradykinesia, but does not stop progression of the disorder. The most common early side effects of levodopa are nausea, vomiting, and hypotension, but cardiac arrhythmias may also occur. Dyskinesias, restlessness, confusion, and other behavioral changes tend to occur somewhat later and become more common with time. Levodopa-induced
P.1033
dyskinesias may take any conceivable form, including chorea, athetosis, dystonia, tremor, tics, and myoclonus. An even later complication is the on-off phenomenon, in which abrupt but transient fluctuations in the severity of parkinsonism occur unpredictably but frequently during the day. The off period of marked bradykinesia has been shown to relate in some instances to falling plasma levels of levodopa. During the on phase, dyskinesias are often conspicuous but mobility is increased.
Carbidopa, which inhibits the enzyme responsible for the breakdown of levodopa to dopamine, does not cross the blood-brain barrier. When levodopa is given in combination with carbidopa, the extracerebral breakdown of levodopa is diminished. This reduces the amount of levodopa required daily for beneficial effects, and it lowers the incidence of nausea, vomiting, hypotension, and cardiac irregularities. Such a combination does not prevent the development of the on-off phenomenon, and the incidence of other side effects (dyskinesias or psychiatric complications) may actually be increased.
Sinemet, a commercially available preparation that contains carbidopa and levodopa in a fixed ratio (1:10 or 1:4), is generally used. Treatment is started with a small dose eg, one tablet of Sinemet 25/100 (containing 25 mg of carbidopa and 100 mg of levodopa) three times daily and gradually increased depending on the response. Sinemet CR is a controlled-release formulation (containing 25 or 50 mg of carbidopa and 100 or 200 mg of levodopa). It is sometimes helpful in reducing fluctuations in clinical response to treatment and in reducing the frequency with which medication must be taken. The commercially available combination of levodopa with both carbidopa and entacapone (Stalevo) may also be helpful in this context and is discussed in the following section on COMT inhibitors. Response fluctuations are also reduced by keeping the daily intake of protein at the recommended minimum and taking the main protein meal as the last meal of the day.
The dyskinesias and behavioral side effects of levodopa are dose-related, but reduction in dose may eliminate any therapeutic benefit.
Levodopa therapy is contraindicated in patients with psychotic illness or narrow-angle glaucoma. It should not be given to patients taking monoamine oxidase A inhibitors or within 2 weeks of their withdrawal, because hypertensive crises may result. Levodopa should be used with care in patients with suspected malignant melanomas or with active peptic ulcers because of concerns that it may exacerbate these disorders.
4. Dopamine agonists
Dopamine agonists act directly on dopamine receptors, and their use in parkinsonism is associated with a lower incidence of the response fluctuations and dyskinesias that occur with long-term levodopa therapy. They were previously reserved for patients who had either become refractory to levodopa or developed the on-off phenomenon. However, they are now best given either before the introduction of levodopa or with a low dose of Sinemet 25/100 (carbidopa 25 mg and levodopa 100 mg), one tablet three times daily when dopaminergic therapy is first introduced; the dose of Sinemet is kept constant, while the dose of the agonist is gradually increased. Two agonists, bromocriptine and pergolide, are ergot derivatives. The initial dosage of bromocriptine is 1.25 mg twice daily; this is increased by 2.5 mg at 2-week intervals until benefit occurs or side effects limit further increments. The usual daily maintenance dose in patients with parkinsonism is between 10 and 30 mg. Pergolide is similarly started in a low dose (eg, 0.05 mg daily) and built up gradually depending on the response and tolerance.
Side effects include anorexia, nausea, vomiting, constipation, postural hypotension, digital vasospasm, cardiac arrhythmias, various dyskinesias and mental disturbances, headache, nasal congestion, erythromelalgia, and pulmonary infiltrates. There are rare reports of pericardial, pleural, or pulmonary fibrosis; cardiac valvopathy has also been associated with pergolide therapy (in as many as 30% of patients). Bromocriptine and pergolide have largely been replaced with other agents because of these side effects.
Pramipexole and ropinirole are two newer dopamine agonists that are not ergot derivatives. They are effective in early Parkinson's disease as well as in advanced stages of the disease. In each case, the daily dose is built up gradually. Pramipexole is started at a dosage of 0.125 mg three times daily, and the dose is doubled after 1 week and again after another week; the daily dose is then increased by 0.75 mg at weekly intervals depending on response and tolerance. Most patients require between 0.5 and 1.5 mg three times daily. Ropinirole is begun in a dosage of 0.25 mg three times daily, and the total daily dose is increased at weekly intervals by 0.75 mg until the fourth week and by 1.5 mg thereafter. Most patients require between 2 and 8 mg three times daily for benefit. Adverse effects include fatigue, somnolence, nausea, peripheral edema, dyskinesias, confusion, and postural hypotension. Less commonly, an irresistible urge to sleep may occur, sometimes in inappropriate and hazardous circumstances.
5. Selegiline
Selegiline is a monoamine oxidase B inhibitor that is sometimes used as adjunctive treatment for parkinsonism in patients receiving levodopa. By inhibiting the metabolic breakdown of dopamine, selegiline has been used to improve fluctuations or declining response to levodopa. In general, however, the response to treatment with it has been disappointing. The drug is taken in a standard dose of 5 mg with breakfast and 5 mg with lunch. It may increase any adverse effects of levodopa.
There are reasons to believe that selegiline may arrest the progression of Parkinson's disease. Studies have failed to establish this conclusively, but this remains an important consideration for patients who are young or have mild disease.
P.1034
6. COMT inhibitors
Catecholamine-O-methyltransferase inhibitors reduce the metabolism of levodopa to 3-O-methyldopa and thereby alter the plasma pharmacokinetics of levodopa, leading to more sustained plasma levels and more constant dopaminergic stimulation of the brain. Two such agents, tolcapone and entacapone, are currently available and may be used as an adjunct to levodopa-carbidopa in patients with response fluctuations or an otherwise inadequate response and who either have failed with other adjunctive therapies or are not candidates for such therapies. Treatment results in reduced response fluctuations, with a greater period of responsiveness to administered levodopa. Tolcapone is given in a dosage of 100 mg or 200 mg three times daily, and entacapone is given as 200 mg with each dose of Sinemet (levodopa-carbidopa). With either preparation, the dose of Sinemet taken concurrently may have to be reduced by up to one-third to avoid side effects such as dyskinesias, confusion, hypotension, and syncope. Diarrhea is sometimes troublesome. Because rare cases of fulminant hepatic failure have followed its use, tolcapone should be avoided in patients with preexisting liver disease. Serial liver function tests should be performed at 2-week intervals for the first year and at longer intervals thereafter in patients receiving the drug as recommended by the manufacturer. Hepatotoxicity has not been reported with entacapone, which is therefore the preferred agent, and serial liver function tests are not required.
Stalevo is the commercial preparation of levodopa combined with both carbidopa and entacapone. It is best used in patients already stabilized on equivalent doses of carbidopa/levodopa and entacapone. It is priced at or below the price of the individual ingredients (ie, carbidopa/levodopa and entacapone) and has the added convenience of requiring fewer tablets to be taken daily. It is available in three strengths: Stalevo 50 (12.5 mg of carbidopa, 50 mg of levodopa, and 200 mg of entacapone), Stalevo 100 (25 mg of carbidopa, 100 mg of levodopa, and 200 mg of entacapone), and Stalevo 150 (37.5 mg of carbidopa, 150 mg of levodopa, and 200 mg of entacapone).
7. Atypical antipsychotics
Confusion and psychotic symptoms, which may be iatrogenic, often respond to atypical antipsychotic agents, which have few extrapyramidal side effects and do not block the effects of dopaminergic medication. Olanzapine, quetiapine, and risperidone may be tried, but the most effective of these agents is clozapine, a dibenzodiazepine derivative. Clozapine may rarely cause marrow suppression, and weekly blood counts are therefore necessary for patients taking it. The patient is started on 6.25 mg at bedtime and the dosage increased to 25 100 mg/d as needed. In low doses, it may also improve iatrogenic dyskinesias.
B. General Measures
Physical therapy or speech therapy helps many patients. The quality of life can often be improved by the provision of simple aids to daily living, eg, rails or banisters placed strategically about the home, special table cutlery with large handles, nonslip rubber table mats, and devices to amplify the voice.
C. Surgical Measures
Thalamotomy or pallidotomy may be helpful for patients who become unresponsive to medical treatment or have intolerable side effects from antiparkinsonian agents, especially if they have no evidence of diffuse vascular disease or significant cognitive decline. Surgery should generally be confined to one side because the morbidity is considerably greater after bilateral procedures. Because of their morbidity, ablative procedures have generally been supplanted by deep brain stimulation, discussed in the following section. Surgical implantation of adrenal medullary or fetal substantia nigra tissue into the caudate nucleus has been reported to benefit some patients, but other investigators have failed to substantiate such claims or have found only modest benefits or major adverse effects. Such procedures are therefore best regarded as experimental, and further studies are required to define the role of cellular therapies.
D. Brain Stimulation
High-frequency thalamic stimulation is effective in suppressing the rest tremor of Parkinson's disease, and chronic bilateral stimulation of the subthalamic nuclei or globus pallidus internus may benefit all the major features of the disease. Electrical stimulation of the brain has the advantage over ablative procedures of being reversible and of causing minimal or no damage to the brain, and is therefore the preferred surgical approach to treatment. There is no evidence that the natural history of Parkinson's disease is affected.
Bjorklund A et al: Neural transplantation for the treatment of Parkinson's disease. Lancet Neurology 2003;2:437.
Christine CW et al: Clinical differentiation of parkinsonian syndromes: prognostic and therapeutic relevance. Am J Med 2004;117:412.
Krack P et al: Five-year follow-up of bilateral stimulation of the subthalamic nucleus in advanced Parkinson's disease. N Engl J Med 2003;349:1925.
Samii A et al: Parkinson's disease. Lancet 2004;363:1783.
Wu SS et al: Treatment of Parkinson's disease: what's on the horizon? CNS Drugs 2005;19:723.
3. Huntington's Disease
![]() Essentials of Diagnosis
Essentials of Diagnosis
Gradual onset and progression of chorea and dementia or behavioral change.
Family history of the disorder.
Responsible gene identified on chromosome 4.
P.1035
General Considerations
Huntington's disease is characterized by chorea and dementia. It is inherited in an autosomal dominant manner and occurs throughout the world, in all ethnic groups, with a prevalence rate of about 5 per 100,000. The gene responsible for the disease is on the short arm of chromosome No. 4. At 4p16.3 there is an expanded and unstable CAG trinucleotide repeat.
Clinical Findings
A. Symptoms and Signs
Clinical onset is usually between 30 and 50 years of age. The disease is progressive and usually leads to a fatal outcome within 15 20 years. The initial symptoms may consist of either abnormal movements or intellectual changes, but ultimately both occur. The earliest mental changes are often behavioral, with irritability, moodiness, antisocial behavior, or a psychiatric disturbance, but a more obvious dementia subsequently develops. The dyskinesia may initially be no more than an apparent fidgetiness or restlessness, but eventually choreiform movements and some dystonic posturing occur. Progressive rigidity and akinesia (rather than chorea) sometimes occur in association with dementia, especially in cases with childhood onset.
B. Imaging
CT scanning usually demonstrates cerebral atrophy and atrophy of the caudate nucleus in established cases. MRI and positron emission tomography (PET) have shown reduced glucose utilization in an anatomically normal caudate nucleus.
Differential Diagnosis
Chorea developing with no family history of choreoathetosis should not be attributed to Huntington's disease, at least not until other causes of chorea have been excluded clinically and by appropriate laboratory studies. Nongenetic causes of chorea include stroke, systemic lupus erythematosus and related disorders, paraneoplastic syndromes, infection with HIV, and various medications. In younger patients, self-limiting Sydenham's chorea develops after group A streptococcal infections on rare occasions. If a patient presents solely with progressive intellectual failure, it may not be possible to distinguish Huntington's disease from other causes of dementia unless there is a characteristic family history or a dyskinesia develops.
A clinically similar autosomal dominant disorder (dentatorubral-pallidoluysian atrophy), manifested by chorea, dementia, ataxia, and myoclonic epilepsy, is uncommon except in persons of Japanese ancestry. It is due to a mutant gene mapping to 12p13.31. Treatment is as for Huntington's disease.
Treatment
There is no cure for Huntington's disease; progression cannot be halted; and treatment is purely symptomatic. The reported biochemical changes suggest a relative underactivity of neurons containing gamma-aminobutyric acid (GABA) and acetylcholine or a relative overactivity of dopaminergic neurons. Treatment with drugs blocking dopamine receptors, such as phenothiazines or haloperidol, may control the dyskinesia and any behavioral disturbances. Haloperidol treatment is usually begun with a dose of 1 mg once or twice daily, which is then increased every 3 or 4 days depending on the response. Tetrabenazine, a drug that depletes central monoamines, is widely used in Europe to treat dyskinesia but is not available in the United States. Reserpine is similar in its actions to tetrabenazine and may be helpful; the daily dose is built up gradually to between 2 and 5 mg, depending on the response. Behavioral disturbances may respond to clozapine. Attempts to compensate for the relative GABA deficiency by enhancing central GABA activity or to compensate for the relative cholinergic underactivity by giving choline chloride have not been therapeutically helpful. High levels of somatostatin (a neuropeptide) have recently been reported in certain areas of the brain in patients with Huntington's disease, and the therapeutic response to cysteamine (a selective depleter of somatostatin in the brain) is currently under study. Neuroprotective strategies are also being explored.
Offspring should be offered genetic counseling. Genetic testing permits presymptomatic detection and definitive diagnosis of the disease.
Cardosi F: Chorea: non-genetic causes. Curr Opin Neurol 2004;17:433.
MacDonald ME et al: Huntington's disease. Neuromolecular Med 2003;4:7.
Rosenblatt A et al: Predictors of neuropathological severity in 100 patients with Huntington's disease. Ann Neurol 2003;54: 488.
4. Idiopathic Torsion Dystonia
![]() Essentials of Diagnosis
Essentials of Diagnosis
Dystonic movements and postures.
Normal birth and developmental history. No other neurologic signs.
Investigations (including CT scan or MRI) reveal no cause of dystonia.
General Considerations
Idiopathic torsion dystonia may occur sporadically or on a hereditary basis, with autosomal dominant, autosomal recessive, and X-linked recessive modes of transmission. One responsible gene is located at 9q34 (and
P.1036
has been named DYT1) and involves a unique mutation consisting of a GAG deletion in the dominantly inherited disorder, and maps to the long arm of the X chromosome in the X-linked recessive form; the responsible gene in the autosomal recessive disorder is unknown. Other autosomal dominant forms have also been recognized, with different or unidentified genetic loci. Symptoms may begin in childhood or later and persist throughout life.
Clinical Findings
The disorder is characterized by the onset of abnormal movements and postures in a patient with a normal birth and developmental history, no relevant past medical illness, and no other neurologic signs. Investigations (including CT scan) reveal no cause for the abnormal movements. Dystonic movements of the head and neck may take the form of torticollis, blepharospasm, facial grimacing, or forced opening or closing of the mouth. The limbs may also adopt abnormal but characteristic postures. The age at onset influences both the clinical findings and the prognosis. With onset in childhood, there is usually a family history of the disorder, symptoms commonly commence in the legs, and progression is likely until there is severe disability from generalized dystonia. In contrast, when onset is later, a positive family history is unlikely, initial symptoms are often in the arms or axial structures, and severe disability does not usually occur, although generalized dystonia may ultimately develop in some patients. If all cases are considered together, about one-third of patients eventually become so severely disabled that they are confined to chair or bed, while another one-third are affected only mildly.
Differential Diagnosis
Before a diagnosis of idiopathic torsion dystonia is made, it is imperative to exclude other causes of dystonia. Perinatal anoxia, birth trauma, and kernicterus are common causes of dystonia, but abnormal movements usually then develop before the age of 5, the early development of the patient is usually abnormal, and a history of seizures is not unusual. Moreover, examination may reveal signs of mental retardation or pyramidal deficit in addition to the movement disorder. Dystonic posturing may also occur in Wilson's disease, Huntington's disease, or parkinsonism; as a sequela of encephalitis lethargica or previous neuroleptic drug therapy; and in certain other disorders. In these cases, diagnosis is based on the history and accompanying clinical manifestations.
Treatment
Idiopathic torsion dystonia usually responds poorly to drugs. Levodopa, diazepam, baclofen, carbamazepine, amantadine, or anticholinergic medication (in high dosage) is occasionally helpful; if not, a trial of treatment with phenothiazines or haloperidol may be worthwhile. In each case, the dose has to be individualized, depending on response and tolerance. However, the doses of these latter drugs that are required for benefit lead usually to mild parkinsonism. Stereotactic thalamotomy is sometimes helpful in patients with predominantly unilateral dystonia, especially when this involves the limbs. The usefulness of deep brain stimulation is under study.
A distinct variety of dominantly inherited dystonia, mapping to a genetic locus on chromosome 14q, is remarkably responsive to levodopa.
Bressman SB et al: Dystonia: phenotypes and genotypes. Rev Neurol (Paris) 2003;159:849.
Defazio G et al: Epidemiology of primary dystonia. Lancet Neurol 2004;3:673.
Kanovsky P: Dystonia: a disorder of motor programming or motor execution? Mov Disord 2002;17:1143.
Nemeth AH: The genetics of primary dystonias and related disorders. Brain 2002;125:695.
5. Focal Torsion Dystonia
A number of the dystonic manifestations that occur in idiopathic torsion dystonia may also occur as isolated phenomena. They are best regarded as focal dystonias that either occur as formes frustes of idiopathic torsion dystonia in patients with a positive family history or represent a focal manifestation of the adult-onset form of that disorder when there is no family history. Mapping of responsible genes to chromosome 8 (DYT6) and chromosome 18 (DYT7) has been reported in some instances of cervical or cranial dystonia. Medical treatment is generally unsatisfactory. A trial of the drugs used in idiopathic torsion dystonia is worthwhile, however, since a few patients do show some response. In addition, with restricted dystonias such as blepharospasm or torticollis, local injection of botulinum A toxin into the overactive muscles may produce worthwhile benefit for several weeks or months and can be repeated as needed.
Both blepharospasm and oromandibular dystonia may occur as an isolated focal dystonia. The former is characterized by spontaneous involuntary forced closure of the eyelids for a variable interval. Oromandibular dystonia is manifested by involuntary contraction of the muscles about the mouth causing, for example, involuntary opening or closing of the mouth, roving or protruding tongue movements, and retraction of the platysma.
Spasmodic torticollis, usually with onset between 25 and 50 years of age, is characterized by a tendency for the neck to twist to one side. This initially occurs episodically, but eventually the neck is held to the side. Spontaneous resolution may occur in the first year or so. The disorder is otherwise usually lifelong. Selective section of the spinal accessory nerve and the upper cervical nerve roots is sometimes helpful if medical treatment is unsuccessful. Local injection of botulinum A toxin provides benefit in most cases.
Writer's cramp is characterized by dystonic posturing of the hand and forearm when the hand is used for writing
P.1037
and sometimes when it is used for other tasks, eg, playing the piano or using a screwdriver or eating utensils. Drug treatment is usually unrewarding, and patients are often best advised to learn to use the other hand for activities requiring manual dexterity. Injections of botulinum A toxin are helpful in some instances.
6. Myoclonus
Occasional myoclonic jerks may occur in anyone, especially when drifting into sleep. General or multifocal myoclonus is common in patients with idiopathic epilepsy and is especially prominent in certain hereditary disorders characterized by seizures and progressive intellectual decline, such as the lipid storage diseases. It is also a feature of various rare degenerative disorders, notably Ramsay Hunt syndrome, and is common in subacute sclerosing panencephalitis and Creutzfeldt-Jakob disease. Generalized myoclonic jerking may accompany uremic and other metabolic encephalopathies, result from therapy with levodopa or cyclic antidepressants, occur in alcohol or drug withdrawal states, or follow anoxic brain damage. It also occurs on a hereditary or sporadic basis as an isolated phenomenon in otherwise healthy subjects.
Segmental myoclonus is a rare manifestation of a focal spinal cord lesion. It may also be the clinical expression of epilepsia partialis continua, a disorder in which a repetitive focal epileptic discharge arises in the contralateral sensorimotor cortex, sometimes from an underlying structural lesion. An electroencephalogram is often helpful in clarifying the epileptic nature of the disorder, and CT or MRI scan may reveal the causal lesion.
Myoclonus may respond to certain anticonvulsant drugs, especially valproic acid, or to one of the benzodiazepines, particularly clonazepam (see Table 24-3). It may also respond to piracetam (up to 16.8 g daily). Myoclonus following anoxic brain damage is often responsive to oxitriptan (5-hydroxytryptophan), an investigational agent that is the precursor of serotonin, and sometimes to clonazepam. Oxitriptan is given in gradually increasing doses up to 1 1.5 mg daily. In patients with segmental myoclonus, a localized lesion should be searched for and treated appropriately.
Caviness JN et al: Myoclonus: current concepts and recent advances. Lancet Neurol 2004;3:598.
Jimenez-Jimenez FJ et al: Drug-induced myoclonus: frequency, mechanisms and management. CNS Drugs 2004;18:93.
7. Wilson's Disease
In this metabolic disorder, abnormal movement and posture may occur with or without coexisting signs of liver involvement. It is discussed in Chapter 15.
8. Drug-Induced Abnormal Movements
Phenothiazines and butyrophenones may produce a wide variety of abnormal movements, including parkinsonism, akathisia (ie, motor restlessness), acute dystonia, chorea, and tardive dyskinesia. These complications are discussed in Chapter 25. Chorea may also develop in patients receiving levodopa, bromocriptine, anticholinergic drugs, phenytoin, carbamazepine, lithium, amphetamines, or oral contraceptives, and it resolves with withdrawal of the offending substance. Similarly, dystonia may be produced by levodopa, bromocriptine, lithium, metoclopramide, or carbamazepine; and parkinsonism by reserpine, tetrabenazine, and metoclopramide. Postural tremor may occur with a variety of drugs, including epinephrine, isoproterenol, theophylline, caffeine, lithium, thyroid hormone, tricyclic antidepressants, and valproic acid.
9. Restless Legs Syndrome
This disorder may occur as a primary (idiopathic) disorder or in relation to pregnancy, iron-deficiency anemia, peripheral neuropathy, or periodic leg movements of sleep. It may have a hereditary basis. Restlessness and curious sensory disturbances lead to an irresistible urge to move the limbs, especially during periods of relaxation. Disturbed nocturnal sleep and excessive daytime somnolences may result. Therapy is with long-acting dopamine agonists or with benzodiazepines such as clonazepam. Levodopa is also helpful but may lead to an augmentation of symptoms, so that its use is generally reserved for those who fail other measures. In some instances, opiates are required to control symptoms.
Schapira AH: Restless legs syndrome: an update on treatment options. Drugs 2004;64:149.
10. Gilles de la Tourette's Syndrome
![]() Essentials of Diagnosis
Essentials of Diagnosis
Multiple motor and phonic tics.
Symptoms begin before age 21 years.
Tics occur frequently for at least 1 year.
Tics vary in number, frequency, and nature over time.
Clinical Findings
Motor tics are the initial manifestation in 80% of cases and most commonly involve the face, whereas in the remaining 20%, the initial symptoms are phonic tics; ultimately a combination of different motor and phonic tics develop in all patients. These are noted first in childhood, generally between the ages of 2 and 15. Motor tics occur especially about the face, head, and shoulders (eg, sniffing, blinking, frowning, shoulder shrugging, head thrusting, etc). Phonic tics commonly
P.1038
consist of grunts, barks, hisses, throat-clearing, coughs, etc, but sometimes also of verbal utterances including coprolalia (obscene speech). There may also be echolalia (repetition of the speech of others), echopraxia (imitation of others' movements), and palilalia (repetition of words or phrases). Some tics may be self-mutilating in nature, such as nail-biting, hair-pulling, or biting of the lips or tongue. The disorder is chronic, but the course may be punctuated by relapses and remissions. Obsessive-compulsive behaviors are commonly associated and may be more disabling than the tics themselves. A family history is sometimes obtained and inheritance has been attributed to an autosomal dominant gene with variable penetrance; linkage to 18q22.1 has been noted in some instances.
Examination usually reveals no abnormalities other than the tics. In addition to obsessive-compulsive behavior disorders, psychiatric disturbances may occur because of the associated cosmetic and social embarrassment. Electroencephalography may show minor nonspecific abnormalities of no diagnostic relevance.
The diagnosis of the disorder is often delayed for years, the tics being interpreted as psychiatric illness or some other form of abnormal movement. Patients are thus often subjected to unnecessary treatment before the disorder is recognized. The tic-like character of the abnormal movements and the absence of other neurologic signs should differentiate this disorder from other movement disorders presenting in childhood. Wilson's disease, however, can simulate the condition and should be excluded.
Treatment
Treatment is symptomatic and may need to be continued indefinitely. Haloperidol is generally regarded as the drug of choice. It is started in a low daily dose (0.25 mg) that is gradually increased (by 0.25 mg every 4 or 5 days) until there is maximum benefit with a minimum of side effects or until side effects limit further increments. A total daily dose of between 2 and 8 mg is usually optimal, but higher doses are sometimes necessary. Treatment with clonazepam (in a dose that depends on response and tolerance) or clonidine (2 5 mcg/kg/d) may also be helpful, and it seems sensible to begin with one of these drugs in order to avoid some of the long-term extrapyramidal side effects of haloperidol. Phenothiazines, such as fluphenazine (2 15 mg daily), have been used, but patients unresponsive to haloperidol are usually unresponsive to these as well.
Pimozide, an oral dopamine-blocking drug related to haloperidol, may be helpful in patients who cannot tolerate or have not responded to haloperidol. Treatment is started with 1 mg daily and the daily dose increased by 1 2 mg every 10 days; the average dose is between 7 and 16 mg daily. Injection of botulinum toxin type A at the site of the most distressing tics is sometimes worthwhile.
Treatment with risperidone, calcium channel blockers, tetrabenazine, clomipramine, metoclopramide, or pergolide has yielded mixed results or encouraging findings in preliminary studies that require confirmation. Bilateral high-frequency thalamic stimulation has been helpful in some, otherwise intractable, cases and is currently under study.
Singer HS: Tourette's syndrome: from behaviour to biology. Lancet Neurol 2005;4:149.
Dementia
Dementia, the symptom complex of progressive global impairment of intellectual function, is a major medical, social, and economic problem that is worsening as the number of elderly people in the general population increases. It is discussed in Chapter 4, and the only point to be reiterated here is the importance of recognizing early any treatable or reversible causes of dementia, such as normal-pressure hydrocephalus, intracranial mass lesions, vascular disease, hypothyroidism, thiamine or vitamin B12 deficiency, Wilson's disease, hepatic or renal failure, neurosyphilis, and the chronic meningitides.
Multiple Sclerosis
![]() Essentials of Diagnosis
Essentials of Diagnosis
Episodic neurologic symptoms.
Patient usually under 55 years of age at onset.
Single pathologic lesion cannot explain clinical findings.
Multiple foci best visualized by MRI.
General Considerations
This common neurologic disorder, which probably has an autoimmune basis, has its greatest incidence in young adults. Epidemiologic studies indicate that multiple sclerosis is much more common in persons of western European lineage who live in temperate zones. No population with a high risk for multiple sclerosis exists between latitudes 40 N and 40 S. Genetic, dietary, and climatic factors cannot account for these differences. Nevertheless, a genetic susceptibility to the disease is likely, based on twin studies, familial cases, and an association with specific HLA antigens (HLA-DR2). Pathologically, focal often perivenular areas of demyelination with reactive gliosis are found scattered in the white matter of brain and spinal cord and in the optic nerves.
Clinical Findings
A. Symptoms and Signs
The common initial presentation is weakness, numbness, tingling, or unsteadiness in a limb; spastic paraparesis; retrobulbar
P.1039
neuritis; diplopia; disequilibrium; or a sphincter disturbance such as urinary urgency or hesitancy. Symptoms may disappear after a few days or weeks, although examination often reveals a residual deficit.
Several forms of the disease are recognized. In most patients, there is an interval of months or years after the initial episode before new symptoms develop or the original ones recur (relapsing-remitting disease). Eventually, however, relapses and usually incomplete remissions lead to increasing disability, with weakness, spasticity, and ataxia of the limbs, impaired vision, and urinary incontinence. The findings on examination at this stage commonly include optic atrophy, nystagmus, dysarthria, and pyramidal, sensory, or cerebellar deficits in some or all of the limbs. In some of these patients, the clinical course changes so that a steady deterioration occurs, unrelated to acute relapses (secondary progressive disease).
Less commonly, symptoms are steadily progressive from their onset, and disability develops at a relatively early stage (primary progressive disease). The diagnosis cannot be made with confidence unless the total clinical picture indicates involvement of different parts of the central nervous system at different times.
A number of factors (eg, infection, trauma) may precipitate or trigger exacerbations. Relapses are also more likely during the 2 or 3 months following pregnancy, possibly because of the increased demands and stresses that occur in the postpartum period.
B. Imaging
MRI of the brain or cervical cord is often helpful in demonstrating the presence of a multiplicity of lesions. CT scans are less helpful.
In patients presenting with myelopathy alone and in whom there is no clinical or laboratory evidence of more widespread disease, myelography or MRI may be necessary to exclude a congenital or acquired surgically treatable lesion. The foramen magnum region must be visualized to exclude the possibility of Arnold-Chiari malformation, in which parts of the cerebellum and the lower brainstem are displaced into the cervical canal and produce mixed pyramidal and cerebellar deficits in the limbs.
C. Laboratory and Other Studies
A definitive diagnosis can never be based solely on the laboratory findings. If there is clinical evidence of only a single lesion in the central nervous system, multiple sclerosis cannot properly be diagnosed unless it can be shown that other regions are affected subclinically. The electrocerebral responses evoked by monocular visual stimulation with a checkerboard pattern stimulus, by monaural click stimulation, and by electrical stimulation of a sensory or mixed peripheral nerve have been used to detect subclinical involvement of the visual, brainstem auditory, and somatosensory pathways, respectively. Other disorders may also be characterized by multifocal electrophysiologic abnormalities.
There may be mild lymphocytosis or a slightly increased protein concentration in the cerebrospinal fluid, especially soon after an acute relapse. Elevated IgG in cerebrospinal fluid and discrete bands of IgG (oligoclonal bands) are present in many patients. The presence of such bands is not specific, however, since they have been found in a variety of inflammatory neurologic disorders and occasionally in patients with vascular or neoplastic disorders of the nervous system.
D. Diagnosis
Multiple sclerosis should not be diagnosed unless there is evidence that two or more different regions of the central white matter have been affected at different times. A diagnosis of clinically definite disease can be made in patients with a relapsing-remitting course and evidence on examination of at least two lesions involving different regions of the central white matter. The diagnosis is probable in patients with multifocal white matter disease but only one clinical attack, or with a history of at least two clinical attacks but signs of only a single lesion.
Treatment
At least partial recovery from acute exacerbations can reasonably be expected, but further relapses may occur without warning, and there is no means of preventing progression of the disorder. Some disability is likely to result eventually, but about half of all patients are without significant disability even 10 years after onset of symptoms.
Recovery from acute relapses may be hastened by treatment with corticosteroids, but the extent of recovery is unchanged. A high dose (eg, prednisone, 60 or 80 mg) is given daily for 1 week, after which medication is tapered over the following 2 or 3 weeks. Such a regimen is often preceded by methylprednisolone, 1 g intravenously for 3 days. Long-term treatment with corticosteroids provides no benefit and does not prevent further relapses. In patients with relapsing-remitting or secondary progressive disease, treatment with -interferon or with daily subcutaneous administration of glatiramer acetate reduces the frequency of exacerbations. Natalizumab, an alpha4 integrin antagonist that reduces the development of brain lesions in experimental models, reduces the relapse rate; however, its use in multiple sclerosis has been suspended after progressive multifocal leukoencephalopathy developed in two patients. Several studies have suggested that immunosuppressive therapy with cyclophosphamide, azathioprine, methotrexate, cladribine, or mitoxantrone may help arrest the course of secondary progressive multiple sclerosis. The evidence of benefit is incomplete, however. There is little evidence that plasmapheresis is helpful in multiple sclerosis. Intravenous immunoglobulins may reduce the clinical attack rate in relapsing-remitting disease, but the available studies are inadequate to permit treatment recommendations. Statins may have immunomodulatory effects, and their possible role in the treatment of multiple sclerosis is being studied.
P.1040
Treatment for spasticity (see below) and for neurogenic bladder may be needed in advanced cases. Excessive fatigue must be avoided, and patients should rest during periods of acute relapse.
Compston A et al: Multiple sclerosis. Lancet 2002;359:1221.
Filippini G et al: Interferons in relapsing remitting multiple sclerosis: a systematic review. Lancet 2003;361:545.
Goodin DS et al: Disease modifying therapies in multiple sclerosis: subcommittee of the American Academy of Neurology and the MS Council for Clinical Practice Guidelines. Neurology 2002;58;169.
Neuhaus O et al: Are statins a treatment option for multiple sclerosis? Lancet Neurol 2004;3:369.
Vitamin E Deficiency
Vitamin E deficiency may produce a disorder somewhat similar to Friedreich's ataxia (see below). There is spinocerebellar degeneration involving particularly the posterior columns of the spinal cord and leading to limb ataxia, sensory loss, absent tendon reflexes, slurring of speech, and, in some cases, pigmentary retinal degeneration. The disorder may occur as a consequence of malabsorption or on a hereditary basis. Treatment is with -tocopheryl acetate (eg, Aquasol E capsules or drops) as discussed in Chapter 29.
Spasticity
The term spasticity is commonly used for an upper motor neuron deficit, but it properly refers to a velocity-dependent increase in resistance to passive movement that affects different muscles to a different extent, is not uniform in degree throughout the range of a particular movement, and is commonly associated with other features of pyramidal deficit. It is often a major complication of stroke, cerebral or spinal injury, static perinatal encephalopathy, and multiple sclerosis.
Physical therapy with appropriate stretching programs is important during rehabilitation after the development of an upper motor neuron lesion and in subsequent management of the patient. The aim is to prevent joint and muscle contractures and perhaps to modulate spasticity.
Drug management is important also, but treatment may increase functional disability when increased extensor tone is providing additional support for patients with weak legs. Dantrolene weakens muscle contraction by interfering with the role of calcium. It is best avoided in patients with poor respiratory function or severe myocardial disease. Treatment is begun with 25 mg once daily, and the daily dose is built up by 25 mg increments every 3 days, depending on tolerance, to a maximum of 100 mg four times daily. Side effects include diarrhea, nausea, weakness, hepatic dysfunction (that may rarely be fatal, especially in women older than 35), drowsiness, light-headedness, and hallucinations.
Lioresal is an effective drug for treating spasticity of spinal origin and painful flexor (or extensor) spasms. The maximum recommended daily dose is 80 mg; treatment is started with a dose of 5 or 10 mg twice daily and then built up gradually. Side effects include gastrointestinal disturbances, lassitude, fatigue, sedation, unsteadiness, confusion, and hallucinations. Diazepam may modify spasticity by its action on spinal interneurons and perhaps also by influencing supraspinal centers, but effective doses often cause intolerable drowsiness and vary with different patients. Tizanidine, a centrally acting 2-adrenergic agonist, is as effective as these other agents but is probably better tolerated. The daily dose is built up gradually, usually to 8 mg taken three times daily. Side effects include sedation, lassitude, hypotension, and dryness of the mouth.
Motor-point blocks by intramuscular phenol have been used to reduce spasticity selectively in one or a few important muscles and may permit return of function in patients with incomplete myelopathies. Intramuscular administration of botulinum toxin may also be helpful. Intrathecal injection of phenol or absolute alcohol may be helpful in more severe cases, but greater selectivity can be achieved by nerve root or peripheral nerve neurolysis. These procedures should not be undertaken until the spasticity syndrome is fully evolved, ie, only after about 1 year or so, and only if long-term drug treatment either has been unhelpful or carries a significant risk to the patient.
In patients with severe spasticity and limited use of the legs, a surgically implanted lioresal pump may provide significant relief and improve hygiene. Repeated transcutaneous electrical nerve stimulation may supplement medical treatment. A number of surgical procedures, eg, adductor or heel cord tenotomy, may also help in the management of spasticity and facilitate patient management. For example, obturator neurectomy is helpful in patients with marked adductor spasms that interfere with personal hygiene or cause gait disturbances. Posterior rhizotomy reduces spasticity, but its effect may be short-lived, whereas anterior rhizotomy produces permanent wasting and weakness in the muscles that are denervated.
Spasticity may be exacerbated by decubitus ulcers, urinary or other infections, and nociceptive stimuli.
Gordon MF et al: Repeated dosing of botulinum toxin type A for upper limb spasticity following stroke. Neurology 2004;63: 1971.
Gracies JM: Pathophysiology of spastic paresis. I: Paresis and soft tissue changes. Muscle Nerve 2005;31:535.
Gracies JM: Pathophysiology of spastic paresis. II: Emergence of muscle overactivity. Muscle Nerve 2005;31:552.
Myelopathies in Aids
A variety of myelopathies may occur in patients with AIDS. These are discussed in Chapter 31.
P.1041
Myelopathy of Human T Cell Leukemia Virus Infection
Human T cell leukemia virus (HTLV-1), a human retrovirus, is transmitted by breast-feeding, sexual contact, blood transfusion, and contaminated needles. Most patients are asymptomatic, but after a variable latent period (which may be as long as several years) a myelopathy develops in some instances. The MRI, electrophysiologic, and cerebrospinal fluid findings are similar to those of multiple sclerosis, but HTLV-1 antibodies are present in serum and spinal fluid. There is no specific treatment.
Nagai M et al: Human T-cell lymphotropic virus type I and neurological diseases. J Neurovirol 2003;9:228.
Subacute Combined Degeneration of the Spinal Cord
Subacute combined degeneration of the spinal cord is due to vitamin B12 deficiency, such as occurs in pernicious anemia. It is characterized by myelopathy with predominant pyramidal and posterior column deficits, sometimes in association with polyneuropathy, mental changes, or optic neuropathy. Megaloblastic anemia may also occur, but this does not parallel the neurologic disorder, and the former may be obscured if folic acid supplements have been taken. Treatment is with vitamin B12. For pernicious anemia, a convenient therapeutic regimen is 100 mg cyanocobalamin intramuscularly daily for 1 week, then weekly for 1 month, and then monthly for the remainder of the patient's life.
Wernicke's Encephalopathy
Wernicke's encephalopathy is characterized by confusion, ataxia, and nystagmus leading to ophthalmoplegia (lateral rectus muscle weakness, conjugate gaze palsies); peripheral neuropathy may also be present. It is due to thiamine deficiency and in the United States occurs most commonly in alcoholics. It may also occur in patients with AIDS. In suspected cases, thiamine (50 mg) is given intravenously immediately and then intramuscularly on a daily basis until a satisfactory diet can be ensured. Intravenous glucose given before thiamine may precipitate the syndrome or worsen the symptoms. The diagnosis is confirmed by the response in 1 or 2 days to treatment, which must not be delayed while laboratory confirmation is obtained.
McIntosh C et al: Alcohol and the nervous system. J Neurol Neurosurg Psychiatry 2004;75 (Suppl 3):iii16.
Stupor & Coma
![]() Essentials of Diagnosis
Essentials of Diagnosis
Level of consciousness is depressed.
Stuporous patients respond only to repeated vigorous stimuli.
Comatose patients are unarousable and unresponsive.
General Considerations
The patient who is stuporous is unresponsive except when subjected to repeated vigorous stimuli, while the comatose patient is unarousable and unable to respond to external events or inner needs, although reflex movements and posturing may be present.
Coma is a major complication of serious central nervous system disorders. It can result from seizures, hypothermia, metabolic disturbances, or structural lesions causing bilateral cerebral hemispheric dysfunction or a disturbance of the brainstem reticular activating system. A mass lesion involving one cerebral hemisphere may cause coma by compression of the brainstem.
Assessment & Emergency Measures
The diagnostic workup of the comatose patient must proceed concomitantly with management. Supportive therapy for respiration or blood pressure is initiated; in hypothermia, all vital signs may be absent and all such patients should be rewarmed before the prognosis is assessed.
The patient can be positioned on one side with the neck partly extended, dentures removed, and secretions cleared by suction; if necessary, the patency of the airways is maintained with an oropharyngeal airway. Blood is drawn for serum glucose, electrolyte, and calcium levels; arterial blood gases; liver and renal function tests; and toxicologic studies as indicated. Dextrose 50% (25 g), naloxone (0.4 1.2 mg), and thiamine (50 mg) are given intravenously.
Further details are then obtained from attendants of the patient's medical history, the circumstances surrounding the onset of coma, and the time course of subsequent events. Abrupt onset of coma suggests subarachnoid hemorrhage, brainstem stroke, or intracerebral hemorrhage, whereas a slower onset and progression occur with other structural or mass lesions. A metabolic cause is likely with a preceding intoxicated state or agitated delirium. On examination, attention is paid to the behavioral response to painful stimuli, the pupils and their response to light, the position of the eyes and their movement in response to passive movement of the head and ice-water caloric stimulation, and the respiratory pattern.
A. Response to Painful Stimuli
Purposive limb withdrawal from painful stimuli implies that sensory pathways from and motor pathways to the stimulated limb are functionally intact. Unilateral absence of responses despite application of stimuli
P.1042
to both sides of the body in turn implies a corticospinal lesion; bilateral absence of responsiveness suggests brainstem involvement, bilateral pyramidal tract lesions, or psychogenic unresponsiveness. Inappropriate responses may also occur. Decorticate posturing may occur with lesions of the internal capsule and rostral cerebral peduncle, decerebrate posturing with dysfunction or destruction of the midbrain and rostral pons, and decerebrate posturing in the arms accompanied by flaccidity or slight flexor responses in the legs in patients with extensive brainstem damage extending down to the pons at the trigeminal level.
B. Ocular Findings
1. Pupils
Hypothalamic disease processes may lead to unilateral Horner's syndrome, while bilateral diencephalic involvement or destructive pontine lesions may lead to small but reactive pupils. Ipsilateral pupillary dilation with no direct or consensual response to light occurs with compression of the third cranial nerve, eg, with uncal herniation. The pupils are slightly smaller than normal but responsive to light in many metabolic encephalopathies; however, they may be fixed and dilated following overdosage with atropine, scopolamine, or glutethimide, and pinpoint (but responsive) with opiates. Pupillary dilation for several hours following cardiopulmonary arrest implies a poor prognosis.
2. Eye movements
Conjugate deviation of the eyes to the side suggests the presence of an ipsilateral hemispheric lesion or a contralateral pontine lesion. A mesencephalic lesion leads to downward conjugate deviation. Dysconjugate ocular deviation in coma implies a structural brainstem lesion unless there was preexisting strabismus.
The oculomotor responses to passive head turning and to caloric stimulation relate to each other and provide complementary information. In response to brisk rotation of the head from side to side and to flexion and extension of the head, normally conscious patients with open eyes do not exhibit contraversive conjugate eye deviation (doll's-head eye response) unless there is voluntary visual fixation or bilateral frontal pathology. With cortical depression in lightly comatose patients, a brisk doll's-head eye response is seen. With brainstem lesions, this oculocephalic reflex becomes impaired or lost, depending on the site of the lesion.
The oculovestibular reflex is tested by caloric stimulation using irrigation with ice water. In normal subjects, jerk nystagmus is elicited for about 2 or 3 minutes, with the slow component toward the irrigated ear. In unconscious patients with an intact brainstem, the fast component of the nystagmus disappears, so that the eyes tonically deviate toward the irrigated side for 2 3 minutes before returning to their original position. With impairment of brainstem function, the response becomes perverted and finally disappears. In metabolic coma, oculocephalic and oculovestibular reflex responses are preserved, at least initially.
C. Respiratory Patterns
Diseases causing coma may lead to respiratory abnormalities. Cheyne-Stokes respiration may occur with bihemispheric or diencephalic disease or in metabolic disorders. Central neurogenic hyperventilation occurs with lesions of the brainstem tegmentum; apneustic breathing (in which there are prominent end-inspiratory pauses) suggests damage at the pontine level (eg, due to basilar artery occlusion); and atactic breathing (a completely irregular pattern of breathing with deep and shallow breaths occurring randomly) is associated with lesions of the lower pontine tegmentum and medulla.
1. Stupor & Coma Due to Structural Lesions
Supratentorial mass lesions tend to affect brain function in an orderly way. There may initially be signs of hemispheric dysfunction, such as hemiparesis. As coma develops and deepens, cerebral function becomes progressively disturbed, producing a predictable progression of neurologic signs that suggest rostrocaudal deterioration.
Thus, as a supratentorial mass lesion begins to impair the diencephalon, the patient becomes drowsy, then stuporous, and finally comatose. There may be Cheyne-Stokes respiration; small but reactive pupils; doll's-head eye responses with side-to-side head movements but sometimes an impairment of reflex upward gaze with brisk flexion of the head; tonic ipsilateral deviation of the eyes in response to vestibular stimulation with cold water; and initially a positive response to pain but subsequently only decorticate posturing. With further progression, midbrain failure occurs. Motor dysfunction progresses from decorticate to bilateral decerebrate posturing in response to painful stimuli; Cheyne-Stokes respiration is gradually replaced by sustained central hyperventilation; the pupils become middle-sized and fixed; and the oculocephalic and oculovestibular reflex responses become impaired, perverted, or lost. As the pons and then the medulla fail, the pupils remain unresponsive; oculovestibular responses are unobtainable; respiration is rapid and shallow; and painful stimuli may lead only to flexor responses in the legs. Finally, respiration becomes irregular and stops, the pupils often then dilating widely.
In contrast, a subtentorial (ie, brainstem) lesion may lead to an early, sometimes abrupt disturbance of consciousness without any orderly rostrocaudal progression of neurologic signs. Compressive lesions of the brainstem, especially cerebellar hemorrhage, may be clinically indistinguishable from intraparenchymal processes.
A structural lesion is suspected if the findings suggest focality. In such circumstances, a CT scan should be performed before, or instead of, a lumbar puncture in order to avoid any risk of cerebral herniation. Further management is of the causal lesion and is considered separately under the individual disorders.
P.1043
2. Stupor & Coma Due to Metabolic Disturbances
Patients with a metabolic cause of coma generally have signs of patchy, diffuse, and symmetric neurologic involvement that cannot be explained by loss of function at any single level or in a sequential manner, although focal or lateralized deficits may occur in hypoglycemia. Moreover, pupillary reactivity is usually preserved, while other brainstem functions are often grossly impaired. Comatose patients with meningitis, encephalitis, or subarachnoid hemorrhage may also exhibit little in the way of focal neurologic signs, however, and clinical evidence of meningeal irritation is sometimes very subtle in comatose patients. Examination of the cerebrospinal fluid in such patients is essential to establish the correct diagnosis.
In patients with coma due to cerebral ischemia and hypoxia, the absence of pupillary light reflexes at the time of initial examination indicates that there is little chance of regaining independence; by contrast, preserved pupillary light responses, the development of spontaneous eye movements (roving, conjugate, or better), and extensor, flexor, or withdrawal responses to pain at this early stage imply a relatively good prognosis.
Treatment of metabolic encephalopathy is of the underlying disturbance and is considered in other chapters. If the cause of the encephalopathy is obscure, all drugs except essential ones may have to be withdrawn in case they are responsible for the altered mental status.
Laureys S et al: Brain function in coma, vegetative state, and related disorders. Lancet Neurol 2004;3:537.
Malik K et al: Evaluating the comatose patient. Rapid neurologic assessment is key to appropriate management. Postgrad Med 2002;111:38.
3. Brain Death
The definition of brain death is controversial, and diagnostic criteria have been published by many different professional organizations. In order to establish brain death, the irreversibly comatose patient must be shown to have lost all brainstem reflex responses, including the pupillary, corneal, oculovestibular, oculocephalic, oropharyngeal, and respiratory reflexes, and should have been in this condition for at least 6 hours. Spinal reflex movements do not exclude the diagnosis, but ongoing seizure activity or decerebrate or decorticate posturing is not consistent with brain death. The apnea test (presence or absence of spontaneous respiratory activity at a PaCO2 of at least 60 mm Hg) serves to determine whether the patient is capable of respiratory activity.
Reversible coma simulating brain death may be seen with hypothermia (temperature < 32 C) and overdosage with central nervous system depressant drugs, and these conditions must be excluded. Certain ancillary tests may assist the determination of brain death but are not essential. An isoelectric electroencephalogram, when the recording is made according to the recommendations of the American Electroencephalographic Society, may help in confirming the diagnosis. Alternatively, the demonstration of an absent cerebral circulation by intravenous radioisotope cerebral angiography or by four-vessel contrast cerebral angiography is confirmatory.
Booth CM et al: Is this patient dead, vegetative, or severely neurologically impaired? Assessing outcome for comatose survivors of cardiac arrest. JAMA 2004;291:870.
Young GB et al: A critique of ancillary tests for brain death. Neurocrit Care 2004;1:499.
4. Persistent Vegetative State
Patients with severe bilateral hemispheric disease may show some improvement from an initially comatose state, so that, after a variable interval, they appear to be awake but lie motionless and without evidence of awareness or higher mental activity. This persistent vegetative state has been variously referred to as akinetic mutism, apallic state, or coma vigil. Most patients in this persistent vegetative state will die in months or years, but partial recovery has occasionally occurred and in rare instances has been sufficient to permit communication or even independent living.
5. Locked-In Syndrome (De-efferented State)
Acute destructive lesions (eg, infarction, hemorrhage, demyelination, encephalitis) involving the ventral pons and sparing the tegmentum may lead to a mute, quadriparetic but conscious state in which the patient is capable of blinking and of voluntary eye movement in the vertical plane, with preserved pupillary responses to light. Such a patient can mistakenly be regarded as comatose. Physicians should recognize that locked-in individuals are fully aware of their surroundings. The prognosis is variable, but recovery has occasionally been reported in some cases including resumption of independent daily life, though this may take up to 2 or 3 years.
Head Injury
Trauma is the most common cause of death in young people, and head injury accounts for almost half of these trauma-related deaths. The prognosis following head injury depends on the site and severity of brain damage. Some guide to prognosis is provided by the mental status, since loss of consciousness for more than 1 or 2 minutes implies a worse prognosis than otherwise. Similarly, the degree of retrograde and posttraumatic amnesia provides an indication of the severity of injury and thus of the prognosis. Absence of skull fracture does not exclude the possibility of severe head injury. During the physical examination, special attention should be given to the level of consciousness and extent of any brainstem dysfunction.
P.1044
Table 24-7. Acute cerebral sequelae of head injury. | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Note: Patients who have lost consciousness for 2 minutes or more following head injury should be admitted to the hospital for observation, as should patients with focal neurologic deficits, lethargy, or skull fractures. If admission is declined, responsible family members should be given clear instructions about the need for, and manner of, checking on them at regular (hourly) intervals and for obtaining additional medical help if necessary.
Skull radiographs or CT scans may provide evidence of fractures. Because injury to the spine may have accompanied head trauma, cervical spine radiographs (especially in the lateral projection) should always be obtained in comatose patients and in patients with severe neck pain or a deficit possibly related to cord compression.
CT scanning has an important role in demonstrating intracranial hemorrhage and may also provide evidence of cerebral edema and displacement of midline structures.
Cerebral Injuries
These are summarized in Table 24-7 along with comments about treatment. Increased intracranial pressure may result from ventilatory obstruction, abnormal neck position, seizures, dilutional hyponatremia, or cerebral edema; an intracranial hematoma requiring surgical evacuation may also be responsible. Other measures that may be necessary to reduce intracranial pressure include induced hyperventilation, intravenous mannitol infusion, and intravenous furosemide; corticosteroids provide no benefit in this context.
Scalp Injuries & Skull Fractures
Scalp lacerations and depressed or compound depressed skull fractures should be treated surgically as appropriate. Simple skull fractures require no specific treatment.
The clinical signs of basilar skull fracture include bruising about the orbit (raccoon sign), blood in the external auditory meatus (Battle's sign), and leakage of cerebrospinal fluid (which can be identified by its glucose content) from the ear or nose. Cranial nerve palsies (involving especially the first, second, third, fourth, fifth, seventh, and eighth nerves in any combination) may also occur. If there is any leakage of cerebrospinal fluid, conservative treatment, with elevation of the head, restriction of fluids, and administration of acetazolamide (250 mg four times daily), is often helpful; but if the leak continues for more than a few days, lumbar subarachnoid drainage may be necessary. Antibiotics are given if infection occurs, based on culture and sensitivity studies. Only very occasional patients require intracranial repair of the dural defect because of persistence of the leak or recurrent meningitis.
Late Complications of Head Injury
The relationship of chronic subdural hemorrhage to head injury is not always clear. In many elderly persons there is no history of trauma, but in other cases a head injury, often trivial, precedes the onset of symptoms by several weeks. The clinical presentation is usually with mental changes such as slowness, drowsiness, headache, confusion, memory disturbances, personality change, or even dementia. Focal neurologic deficits such as hemiparesis or hemisensory disturbance may also occur but are less common. CT scan is an important means of detecting the hematoma, which is sometimes bilateral. Treatment is by surgical evacuation to prevent cerebral compression and tentorial
P.1045
herniation. There is no clear evidence that prophylactic anticonvulsant therapy reduces the incidence of posttraumatic seizures.
Normal-pressure hydrocephalus may follow head injury, subarachnoid hemorrhage, or meningoencephalitis.
Other late complications of head injury include posttraumatic seizure disorder and posttraumatic headache.
Dutton RP et al: Traumatic brain injury. Curr Opin Crit Care 2003;9:503.
Vincent JL et al: Primer on medical management of severe brain injury. Crit Care Med 2005;33:1392.
Winter CD et al: A review of the current management of severe traumatic brain injury. Surgeon 2005;3:329.
Spinal Trauma
![]() Essentials of Diagnosis
Essentials of Diagnosis
History of preceding trauma.
Development of acute neurologic deficit.
Signs of myelopathy on examination.
General Considerations
While spinal cord damage may result from whiplash injury, severe injury usually relates to fracture-dislocation causing compression or angular deformity of the cord either cervically or in the lower thoracic and upper lumbar regions. Extreme hypotension following injury may also lead to cord infarction.
Clinical Findings
Total cord transection results in immediate flaccid paralysis and loss of sensation below the level of the lesion. Reflex activity is lost for a variable period, and there is urinary and fecal retention. As reflex function returns over the following days and weeks, spastic paraplegia or quadriplegia develops, with hyperreflexia and extensor plantar responses, but a flaccid atrophic (lower motor neuron) paralysis may be found depending on the segments of the cord that are affected. The bladder and bowels also regain some reflex function, permitting urine and feces to be expelled at intervals. As spasticity increases, flexor or extensor spasms (or both) of the legs become troublesome, especially if the patient develops bed sores or a urinary tract infection. Paraplegia with the legs in flexion or extension may eventually result.
With lesser degrees of injury, patients may be left with mild limb weakness, distal sensory disturbance, or both. Sphincter function may also be impaired, urinary urgency and urgency incontinence being especially common. More particularly, a unilateral cord lesion leads to an ipsilateral motor disturbance with accompanying impairment of proprioception and contralateral loss of pain and temperature appreciation below the lesion (Brown-S quard syndrome). A central cord syndrome may lead to a lower motor neuron deficit and loss of pain and temperature appreciation, with sparing of posterior column functions. A radicular deficit may occur at the level of the injury or, if the cauda equina is involved, there may be evidence of disturbed function in several lumbosacral roots.
Treatment
Treatment of the injury consists of immobilization and if there is cord compression decompressive laminectomy and fusion. Early treatment with high doses of corticosteroids (eg, methylprednisolone, 30 mg/kg by intravenous bolus, followed by 5.4 mg/kg/h for 23 hours) has been shown to improve neurologic recovery if commenced within 8 hours after injury. Treatment with GM1 ganglioside for 3 or 4 weeks is an experimental approach that has also been helpful. Anatomic realignment of the spinal cord by traction and other orthopedic procedures is also important. Subsequent care of the residual neurologic deficit paraplegia or quadriplegia requires treatment of spasticity and care of the skin, bladder, and bowels.
McDonald JW et al: Spinal-cord injury. Lancet 2002;359:417.
Syringomyelia
Destruction or degeneration of gray and white matter adjacent to the central canal of the cervical spinal cord leads to cavitation and accumulation of fluid within the spinal cord. The precise pathogenesis is unclear, but many cases are associated with Arnold-Chiari malformation, in which there is displacement of the cerebellar tonsils, medulla, and fourth ventricle into the spinal canal, sometimes with accompanying meningomyelocele. In such circumstances, the cord cavity connects with and may merely represent a dilated central canal. In other cases, the cause of cavitation is less clear. There is a characteristic clinical picture, with segmental atrophy and areflexia and loss of pain and temperature appreciation in a cape distribution owing to the destruction of fibers crossing in front of the central canal. Thoracic kyphoscoliosis is usually present. With progression, involvement of the long motor and sensory tracts occurs as well, so that a pyramidal and sensory deficit develops in the legs. Upward extension of the cavitation (syringobulbia) leads to dysfunction of the lower brainstem and thus to bulbar palsy, nystagmus, and sensory impairment over one or both sides of the face.
Syringomyelia, ie, cord cavitation, may also occur in association with an intramedullary tumor or following severe cord injury, and the cavity then does not communicate with the central canal.
In patients with Arnold-Chiari malformation, there are commonly skeletal abnormalities on plain x-rays of the skull and cervical spine. CT scans show
P.1046
caudal displacement of the fourth ventricle. MRI or positive contrast myelography may demonstrate the malformation itself. Focal cord enlargement is found at myelography or by MRI in patients with cavitation related to past injury or intramedullary neoplasms.
Treatment of Arnold-Chiari malformation with associated syringomyelia is by suboccipital craniectomy and upper cervical laminectomy, with the aim of decompressing the malformation at the foramen magnum. The cord cavity should be drained, and if necessary an outlet for the fourth ventricle can be made. In cavitation associated with intramedullary tumor, treatment is surgical, but radiation therapy may be necessary if complete removal is not possible. Posttraumatic syringomyelia is also treated surgically if it leads to increasing neurologic deficits or to intolerable pain.
Arnett B: Arnold-Chiari malformation. Arch Neurol 2003;60: 898.
Levine DN: The pathogenesis of syringomyelia associated with lesions at the foramen magnum: a critical review of existing theories and proposal of a new hypothesis. J Neurol Sci 2004;220:3.
Degenerative Motor Neuron Diseases
![]() Essentials of Diagnosis
Essentials of Diagnosis
Weakness.
No sensory loss or sphincter disturbance.
Progressive course.
No identifiable underlying cause other than genetic basis in familial cases.
General Considerations
This group of degenerative disorders is characterized clinically by weakness and variable wasting of affected muscles, without accompanying sensory changes.
Motor neuron disease in adults generally commences between 30 and 60 years of age. There is degeneration of the anterior horn cells in the spinal cord, the motor nuclei of the lower cranial nerves, and the corticospinal and corticobulbar pathways. The disorder is usually sporadic, but familial cases may occur and several genetic mutations or loci have been identified.
Classification
Five varieties have been distinguished on clinical grounds.
A. Progressive Bulbar Palsy
Bulbar involvement predominates owing to disease processes affecting primarily the motor nuclei of the cranial nerves.
B. Pseudobulbar Palsy
Bulbar involvement predominates in this variety also, but it is due to bilateral corticobulbar disease and thus reflects upper motor neuron dysfunction.
C. Progressive Spinal Muscular Atrophy
This is characterized primarily by a lower motor neuron deficit in the limbs due to degeneration of the anterior horn cells in the spinal cord.
D. Primary Lateral Sclerosis
There is a purely upper motor neuron deficit in the limbs.
E. Amyotrophic Lateral Sclerosis
A mixed upper and lower motor neuron deficit is found in the limbs. This disorder is sometimes associated with dementia or parkinsonism.
Clinical Findings
A. Symptoms and Signs
Difficulty in swallowing, chewing, coughing, breathing, and talking (dysarthria) occur with bulbar involvement. In progressive bulbar palsy, there is drooping of the palate; a depressed gag reflex; pooling of saliva in the pharynx; a weak cough; and a wasted, fasciculating tongue. In pseudobulbar palsy, the tongue is contracted and spastic and cannot be moved rapidly from side to side. Limb involvement is characterized by motor disturbances (weakness, stiffness, wasting, fasciculations) reflecting lower or upper motor neuron dysfunction; there are no objective changes on sensory examination, although there may be vague sensory complaints. The sphincters are generally spared.
The disorder is progressive, and amyotrophic lateral sclerosis is usually fatal within 3 5 years; death usually results from pulmonary infections. Patients with bulbar involvement generally have the poorest prognosis.
B. Laboratory and Other Studies
Electromyography may show changes of chronic partial denervation, with abnormal spontaneous activity in the resting muscle and a reduction in the number of motor units under voluntary control. In patients with suspected spinal muscular atrophy or amyotrophic lateral sclerosis, the diagnosis should not be made with confidence unless such changes are found in at least three spinal regions (cervical, thoracic, lumbosacral) or two spinal regions and the bulbar musculature. Motor conduction velocity is usually normal but may be slightly reduced, and sensory conduction studies are also normal. Biopsy of a wasted muscle shows the histologic changes of denervation. The serum creatine kinase may be slightly elevated but never reaches the extremely high values seen in some of the muscular dystrophies. The cerebrospinal fluid is normal.
P.1047
A familial form of amyotrophic lateral sclerosis has been described with autosomal dominant inheritance, related to mutations in the copper-zinc superoxide dismutase gene on the long arm of chromosome 21. Other familial forms with dominant or recessive inheritance have also been identified and mapped to other genetic loci. X-linked bulbospinal neuronopathy is associated with an expanded trinucleotide repeat sequence on the androgen receptor gene and carries a more benign prognosis than other forms of motor neuron disease. There have been recent reports of juvenile spinal muscular atrophy due to hexosaminidase deficiency, with abnormal findings on rectal biopsy and reduced hexosaminidase A in serum and leukocytes. Pure motor syndromes resembling motor neuron disease may also occur in association with monoclonal gammopathy or multifocal motor neuropathies with conduction block. A motor neuronopathy may also develop in Hodgkin's disease and has a relatively benign prognosis. Infective anterior horn cell diseases (polio virus or West Nile virus infection) can generally be distinguished by the acute onset and monophasic course of the illness, as discussed elsewhere in this book.
Treatment
Riluzole, 50 mg orally twice daily, which reduces the presynaptic release of glutamate, may slow progression of amyotrophic lateral sclerosis. There is otherwise no specific treatment except in patients with gammopathy, in whom plasmapheresis and immunosuppression may lead to improvement. Therapeutic trials of various neurotrophic factors to slow disease progression have yielded generally disappointing results. Symptomatic and supportive measures may include prescription of anticholinergic drugs (such as trihexyphenidyl, amitriptyline, or atropine) or use of a portable suction machine if drooling is troublesome, braces or a walker to improve mobility, and physical therapy to prevent contractures. Behavioral modification (eg, exercising facial muscles and encouraging frequent swallowing) or over-the-counter decongestants may also help mild drooling. Spasticity may be helped by baclofen or diazepam. A semiliquid diet or nasogastric tube feeding may be needed if dysphagia is severe. Gastrostomy or cricopharyngomyotomy is sometimes resorted to in extreme cases of predominant bulbar involvement, and tracheostomy may be necessary if respiratory muscles are severely affected; however, in the terminal stages of these disorders, the aim of treatment should be to keep patients as comfortable as possible. Information on palliative care is provided in Chapter 5.
McGeer EG et al: Pharmacologic approaches to the treatment of amyotrophic lateral sclerosis. BioDrugs 2005;19:31.
Winhammar JM et al: Assessment of disease progression in motor neuron disease. Lancet Neurol 2005;4:229.
Peripheral Neuropathies
Peripheral neuropathies can be categorized on the basis of the structure primarily affected. The predominant pathologic feature may be axonal degeneration (axonal or neuronal neuropathies) or paranodal or segmental demyelination. The distinction may be possible on the basis of neurophysiologic findings. Motor and sensory conduction velocity can be measured in accessible segments of peripheral nerves. In axonal neuropathies, conduction velocity is normal or reduced only mildly and needle electromyography provides evidence of denervation in affected muscles. In demyelinating neuropathies, conduction may be slowed considerably in affected fibers, and in more severe cases, conduction is blocked completely, without accompanying electromyographic signs of denervation.
Nerves may be injured or compressed by neighboring anatomic structures at any point along their course. Common mononeuropathies of this sort are considered below. They lead to a sensory, motor, or mixed deficit that is restricted to the territory of the affected nerve. A similar clinical disturbance is produced by peripheral nerve tumors, but these are rare except in patients with Recklinghausen's disease. Multiple mononeuropathies suggest a patchy multifocal disease process such as vasculopathy (eg, diabetes, arteritis), an infiltrative process (eg, leprosy, sarcoidosis), radiation damage, or an immunologic disorder (eg, brachial plexopathy). Diffuse polyneuropathies lead to a symmetric sensory, motor, or mixed deficit, often most marked distally. They include the hereditary, metabolic, and toxic disorders; idiopathic inflammatory polyneuropathy (Guillain-Barr syndrome); and the peripheral neuropathies that may occur as a nonmetastatic complication of malignant diseases. Involvement of motor fibers leads to flaccid weakness that is most marked distally; dysfunction of sensory fibers causes impaired sensory perception. Tendon reflexes are depressed or absent. Paresthesias, pain, and muscle tenderness may also occur.
1. Polyneuropathies & Mononeuritis Multiplex
![]() Essentials of Diagnosis
Essentials of Diagnosis
Weakness, sensory disturbances, or both in the extremities.
Pain sometimes common.
Depressed or absent tendon reflexes.
May be family history of neuropathy.
May be history of systemic illness or toxic exposure.
The cause of polyneuropathy or mononeuritis multiplex is suggested by the history, mode of onset, and
P.1048
predominant clinical manifestations. Laboratory workup includes a complete blood count and sedimentation rate, serum protein electrophoresis, and immunophoresis, determination of plasma urea and electrolytes, liver and thyroid function tests, tests for rheumatoid factor and antinuclear antibody, HBsAg determination, a serologic test for syphilis, fasting blood glucose level, urinary heavy metal levels, cerebrospinal fluid examination, and chest radiography. These tests should be ordered selectively, as guided by symptoms and signs. Measurement of nerve conduction velocity is important in confirming the peripheral nerve origin of symptoms and providing a means of following clinical changes, as well as indicating the likely disease process (ie, axonal or demyelinating neuropathy). Cutaneous nerve biopsy may help establish a precise diagnosis (eg, polyarteritis, amyloidosis). In about half of cases, no specific cause can be established; of these, slightly less than half are subsequently found to be heredofamilial.
Treatment is of the underlying cause, when feasible, and is discussed below under the individual disorders. Physical therapy helps prevent contractures, and splints can maintain a weak extremity in a position of useful function. Anesthetic extremities must be protected from injury. To guard against burns, patients should check the temperature of water and hot surfaces with a portion of skin having normal sensation, measure water temperature with a thermometer, and use cold water for washing or lower the temperature setting of their hot-water heaters. Shoes should be examined frequently during the day for grit or foreign objects in order to prevent pressure lesions.
Patients with polyneuropathies or mononeuritis multiplex are subject to additional nerve injury at pressure points and should therefore avoid such behavior as leaning on elbows or sitting with crossed legs for lengthy periods.
Neuropathic pain is sometimes troublesome and may respond to simple analgesics such as aspirin. Narcotics or narcotic substitutes may be necessary for severe hyperpathia or pain induced by minimal stimuli, but their use should be avoided as much as possible. The use of a frame or cradle to reduce contact with bedclothes may be helpful. Many patients experience episodic stabbing pains, which may respond to phenytoin, carbamazepine, gabapentin, pregabalin, or tricyclic antidepressants.
Symptoms of autonomic dysfunction are occasionally troublesome. Postural hypotension is often helped by wearing waist-high elastic stockings and sleeping in a semierect position at night. Fludrocortisone reduces postural hypotension, but doses as high as 1 mg/d are sometimes necessary in diabetics and may lead to recumbent hypertension. Midodrine, an -agonist, is sometimes helpful in a dose of 2.5 10 mg three times daily. Impotence and diarrhea are difficult to treat; a flaccid neuropathic bladder may respond to parasympathomimetic drugs such as bethanechol chloride, 10 50 mg three or four times daily.
Inherited Neuropathies
A. Charcot-Marie-Tooth Disease (HMSN Type I, II)
Several distinct varieties of Charcot-Marie-Tooth disease can be recognized. There is usually an autosomal dominant mode of inheritance, but occasional cases occur on a sporadic, recessive, or X-linked basis. The responsible gene is commonly located on the short arm of chromosome 17 and less often shows linkage to chromosome 1 or the X chromosome. It has also been linked to several other chromosomes, emphasizing the genetic heterogeneity of the disorder. Clinical presentation may be with foot deformities or gait disturbances in childhood or early adult life. Slow progression leads to the typical features of polyneuropathy, with distal weakness and wasting that begin in the legs, a variable amount of distal sensory loss, and depressed or absent tendon reflexes. Tremor is a conspicuous feature in some instances. Electrodiagnostic studies show a marked reduction in motor and sensory conduction velocity (hereditary motor and sensory neuropathy [HMSN] type I).
In other instances (HMSN type II), motor conduction velocity is normal or only slightly reduced, sensory nerve action potentials may be absent, and signs of chronic partial denervation are found in affected muscles electromyographically. The predominant pathologic change is axonal loss rather than segmental demyelination.
A similar disorder may occur in patients with progressive distal spinal muscular atrophy, but there is no sensory loss; electrophysiologic investigation reveals that motor conduction velocity is normal or only slightly reduced, and nerve action potentials are normal.
B. Dejerine-Sottas Disease (HMSN Type III)
The disorder may occur on a sporadic, autosomal dominant or, less commonly, autosomal recessive basis. Onset in infancy or childhood leads to a progressive motor and sensory polyneuropathy with weakness, ataxia, sensory loss, and depressed or absent tendon reflexes. The peripheral nerves may be palpably enlarged and are characterized pathologically by segmental demyelination, Schwann cell hyperplasia, and thin myelin sheaths. Electrophysiologically, there is slowing of conduction, and sensory action potentials may be unrecordable.
C. Friedreich's Ataxia
Patients generally present in childhood or early adult life with this autosomal recessive disorder, which has been related to an unstable mutation of the X25 gene on chromosome 9q13-q21.1. The gait becomes atactic, the hands become clumsy, and other signs of cerebellar dysfunction develop accompanied by weakness of the legs and extensor plantar responses. Involvement of peripheral sensory fibers leads to sensory disturbances in the limbs and depressed tendon reflexes.
P.1049
There is bilateral pes cavus. Pathologically, there is a marked loss of cells in the posterior root ganglia and degeneration of peripheral sensory fibers. In the central nervous system, changes are conspicuous in the posterior and lateral columns of the cord. Electrophysiologically, conduction velocity in motor fibers is normal or only mildly reduced, but sensory action potentials are small or absent.
D. Refsum's Disease (HMSN Type IV)
This autosomal recessive disorder is due to a disturbance in phytanic acid metabolism. Clinically, pigmentary retinal degeneration is accompanied by progressive sensorimotor polyneuropathy and cerebellar signs. Auditory dysfunction, cardiomyopathy, and cutaneous manifestations may also occur. Motor and sensory conduction velocity are reduced, often markedly, and there may be electromyographic evidence of denervation in affected muscles. Dietary restriction of phytanic acid and its precursors may be helpful therapeutically. Plasmapheresis to reduce stored phytanic acid may help at the initiation of treatment.
E. Porphyria
Peripheral nerve involvement may occur during acute attacks in both variegate porphyria and acute intermittent porphyria. Motor symptoms usually occur first, and weakness is often most marked proximally and in the upper limbs rather than the lower. Sensory symptoms and signs may be proximal or distal in distribution. Autonomic involvement is sometimes pronounced. The electrophysiologic findings are in keeping with the results of neuropathologic studies suggesting that the neuropathy is axonal in type. Hematin (4 mg/kg intravenously over 15 minutes once or twice daily) may lead to rapid improvement. A high-carbohydrate diet and, in severe cases, intravenous glucose or levulose may also be helpful. Propranolol (up to 100 mg every 4 hours) may control tachycardia and hypertension in acute attacks. Porphyria is discussed further in Chapter 40.
Neuropathies Associated with Systemic & Metabolic Disorders
A. Diabetes Mellitus
In this disorder, involvement of the peripheral nervous system may lead to symmetric sensory or mixed polyneuropathy, asymmetric motor radiculoneuropathy or plexopathy (diabetic amyotrophy), thoracoabdominal radiculopathy, autonomic neuropathy, or isolated lesions of individual nerves. These may occur singly or in any combination and are discussed in Chapter 27.
B. Uremia
Uremia may lead to a symmetric sensorimotor polyneuropathy that tends to affect the lower limbs more than the upper limbs and is more marked distally than proximally (see Chapter 22). The diagnosis can be confirmed electrophysiologically, for motor and sensory conduction velocity is moderately reduced. The neuropathy improves both clinically and electrophysiologically with renal transplantation and to a lesser extent with chronic dialysis.
C. Alcoholism and Nutritional Deficiency
Many alcoholics have an axonal distal sensorimotor polyneuropathy that is frequently accompanied by painful cramps, muscle tenderness, and painful paresthesias and is often more marked in the legs than in the arms. Symptoms of autonomic dysfunction may also be conspicuous. Motor and sensory conduction velocity may be slightly reduced, even in subclinical cases, but gross slowing of conduction is uncommon. A similar distal sensorimotor polyneuropathy is a well-recognized feature of beriberi (thiamine deficiency). In vitamin B12 deficiency, distal sensory polyneuropathy may develop but is usually overshadowed by central nervous system manifestations (eg, myelopathy, optic neuropathy, or intellectual changes).
D. Paraproteinemias
A symmetric sensorimotor polyneuropathy that is gradual in onset, progressive in course, and often accompanied by pain and dysesthesias in the limbs may occur in patients (especially men) with multiple myeloma. The neuropathy is of the axonal type in classic lytic myeloma, but segmental demyelination (primary or secondary) and axonal loss may occur in sclerotic myeloma and lead to predominantly motor clinical manifestations. Both demyelinating and axonal neuropathies are also observed in patients with paraproteinemias without myeloma. A small fraction will develop myeloma if serially followed. The demyelinating neuropathy in these patients may be due to the monoclonal protein's reacting to a component of the nerve myelin. The neuropathy of classic multiple myeloma is poorly responsive to therapy. The polyneuropathy of benign monoclonal gammopathy may respond to immunosuppressant drugs and plasmapheresis.
Polyneuropathy may also occur in association with macroglobulinemia and cryoglobulinemia and sometimes responds to plasmapheresis. Entrapment neuropathy, such as carpal tunnel syndrome, is more common than polyneuropathy in patients with (nonhereditary) generalized amyloidosis. With polyneuropathy due to amyloidosis, sensory and autonomic symptoms are especially conspicuous, whereas distal wasting and weakness occur later; there is no specific treatment.
Neuropathies Associated with Infectious & Inflammatory Diseases
A. Leprosy
Leprosy is an important cause of peripheral neuropathy in certain parts of the world. Sensory disturbances are mainly due to involvement of intracutaneous nerves. In
P.1050
tuberculoid leprosy, they develop at the same time and in the same distribution as the skin lesion but may be more extensive if nerve trunks lying beneath the lesion are also involved. In lepromatous leprosy, there is more extensive sensory loss, and this develops earlier and to a greater extent in the coolest regions of the body, such as the dorsal surfaces of the hands and feet, where the bacilli proliferate most actively. Motor deficits result from involvement of superficial nerves where their temperature is lowest, eg, the ulnar nerve in the region proximal to the olecranon groove, the median nerve as it emerges from beneath the forearm flexor muscle to run toward the carpal tunnel, the peroneal nerve at the head of the fibula, and the posterior tibial nerve in the lower part of the leg; patchy facial muscular weakness may also occur owing to involvement of the superficial branches of the seventh cranial nerve.
Motor disturbances in leprosy are suggestive of multiple mononeuropathy, whereas sensory changes resemble those of distal polyneuropathy. Examination, however, relates the distribution of sensory deficits to the temperature of the tissues; in the legs, for example, sparing frequently occurs between the toes and in the popliteal fossae, where the temperature is higher. Treatment is with antileprotic agents (see Chapter 33).
B. AIDS
A variety of neuropathies occur in HIV-infected patients (see Chapter 31). Patients with AIDS may develop a chronic symmetric sensorimotor axonal polyneuropathy associated usually with no abnormal cerebrospinal fluid findings. Treatment is symptomatic. AIDS patients may also develop progressive polyradiculopathy or radiculomyelopathy that leads to leg weakness and urinary retention; sensory loss is less conspicuous than in polyneuropathy. The cerebrospinal fluid may show mononuclear pleocytosis and increased protein and low glucose concentrations. Cytomegalovirus is responsible in at least some cases. The prognosis is generally poor, but some patients respond to intravenous ganciclovir (2.5 mg/kg every 8 hours for 10 days, then 7.5 mg/kg daily 5 days per week).
An inflammatory demyelinating polyradiculoneuropathy sometimes occurs in HIV-seropositive patients without AIDS and may follow an acute, subacute, or chronic course. Weakness is usually more conspicuous distally than proximally and tends to overshadow sensory symptoms. Tendon reflexes are depressed or absent. The cerebrospinal fluid shows an increased cell count and protein concentration. Treatment with plasmapheresis has helped some patients. Spontaneous improvement may also occur. Seropositive patients without AIDS may also develop a mononeuropathy multiplex that sometimes responds to treatment with plasmapheresis.
C. Lyme Borreliosis
The neurologic manifestations of Lyme disease include meningitis, meningoencephalitis, polyradiculoneuropathy, mononeuropathy multiplex, and cranial neuropathy. Serologic tests establish the underlying disorder. Treatment is described in Chapter 34.
D. Sarcoidosis
Cranial nerve palsies (especially facial palsy), multiple mononeuropathy and, less commonly, symmetric polyneuropathy may all occur, the latter sometimes preferentially affecting either motor or sensory fibers. Improvement may occur with use of corticosteroids.
E. Polyarteritis
Involvement of the vasa nervorum by the vasculitic process may result in infarction of the nerve. Clinically, one encounters an asymmetric sensorimotor polyneuropathy (mononeuritis multiplex) that pursues a waxing and waning course. Corticosteroids and cytotoxic agents especially cyclophosphamide may be of benefit in severe cases.
F. Rheumatoid Arthritis
Compressive or entrapment neuropathies, ischemic neuropathies, mild distal sensory polyneuropathy, and severe progressive sensorimotor polyneuropathy can occur in rheumatoid arthritis.
Neuropathy Associated with Critical Illness
Patients in intensive care units with sepsis and multiorgan failure sometimes develop polyneuropathies. This may be manifested initially by unexpected difficulty in weaning patients from a mechanical ventilator and in more advanced cases by wasting and weakness of the extremities and loss of tendon reflexes. Sensory abnormalities are relatively inconspicuous. The neuropathy is axonal in type. Its pathogenesis is obscure, and treatment is supportive. The prognosis is good provided patients recover from the underlying critical illness.
Toxic Neuropathies
Axonal polyneuropathy may follow exposure to industrial agents or pesticides such as acrylamide, organophosphorus compounds, hexacarbon solvents, methyl bromide, and carbon disulfide; metals such as arsenic, thallium, mercury, and lead; and drugs such as phenytoin, perhexiline, isoniazid, nitrofurantoin, vincristine, and pyridoxine in high doses. Detailed occupational, environmental, and medical histories and recognition of clusters of cases are important in suggesting the diagnosis. Treatment is by preventing further exposure to the causal agent. Isoniazid neuropathy is prevented by pyridoxine supplementation.
Diphtheritic neuropathy results from a neurotoxin released by the causative organism and is common in many areas. Palatal weakness may develop 2 4 weeks after infection of the throat, and infection of the skin may similarly be followed by focal weakness of neighboring
P.1051
muscles. Disturbances of accommodation may occur about 4 5 weeks after infection and distal sensorimotor demyelinating polyneuropathy after 1 3 months.
Neuropathies Associated with Malignant Diseases
Both a sensorimotor and a purely sensory polyneuropathy may occur as a nonmetastatic complication of malignant diseases (see Table 40-6). The sensorimotor polyneuropathy may be mild and occur in the course of known malignant disease, or it may have an acute or subacute onset, lead to severe disability, and occur before there is any clinical evidence of the cancer, occasionally following a remitting course.
Acute Idiopathic Polyneuropathy (Guillain-Barr Syndrome)
![]() Essentials of Diagnosis
Essentials of Diagnosis
Acute or subacute progressive polyradiculoneuropathy.
Usually ascending, symmetric weakness.
Paresthesias are more variable.
Acute dysautonomia may be life-threatening.
A. General Considerations
This acute or subacute polyradiculoneuropathy sometimes follows infective illness, inoculations, or surgical procedures. There is an association with preceding Campylobacter jejuni enteritis. The disorder probably has an immunologic basis, but the precise mechanism is unclear.
B. Clinical Findings
1. Symptoms and signs
The main complaint is of weakness that varies widely in severity in different patients and often has a proximal emphasis and symmetric distribution. It usually begins in the legs, spreading to a variable extent but frequently involving the arms and often one or both sides of the face. The muscles of respiration or deglutition may also be affected. Sensory symptoms are usually less conspicuous than motor ones, but distal paresthesias and dysesthesias are common, and neuropathic or radicular pain is present in many patients. Autonomic disturbances are also common, may be severe, and are sometimes life-threatening; they include tachycardia, cardiac irregularities, hypotension or hypertension, facial flushing, abnormalities of sweating, pulmonary dysfunction, and impaired sphincter control.
2. Laboratory findings
The cerebrospinal fluid characteristically contains a high protein concentration with a normal cell content, but these changes may take 2 or 3 weeks to develop. Electrophysiologic studies may reveal marked abnormalities, which do not necessarily parallel the clinical disorder in their temporal course. Pathologic examination has shown primary demyelination or, less commonly, axonal degeneration.
C. Differential Diagnosis
When the diagnosis is made, the history and appropriate laboratory studies should exclude the possibility of porphyric, diphtheritic, or toxic (heavy metal, hexacarbon, organophosphate) neuropathies. The temporal course excludes other peripheral neuropathies. Poliomyelitis, botulism, and tick paralysis must also be considered as they cause weakness of acute onset. The presence of pyramidal signs, a markedly asymmetric motor deficit, a sharp sensory level, or early sphincter involvement should suggest a focal cord lesion.
D. Prognosis
Most patients eventually make a good recovery, but this may take many months, and 10 20% patients of are left with persisting disability.
E. Treatment
Treatment with prednisone is ineffective and may prolong recovery time. Plasmapheresis is of value; it is best performed within the first few days of illness and is best reserved for clinically severe or rapidly progressive cases or those with ventilatory impairment. Intravenous immunoglobulin (400 mg/kg/d for 5 days) is also helpful and imposes less stress on the cardiovascular system than plasmapheresis. Patients should be admitted to intensive care units if their forced vital capacity is declining, and intubation is considered if the forced vital capacity reaches 15 mL/kg, dyspnea becomes evident, or the oxygen saturation declines. Respiratory toilet and chest physical therapy help prevent atelectasis. Marked hypotension may respond to volume replacement or pressor agents. Low-dose heparin to prevent pulmonary embolism should be considered.
Approximately 3% of patients with acute idiopathic polyneuropathy have one or more clinically similar relapses, sometimes several years after the initial illness. Plasma exchange therapy may produce improvement in chronic and relapsing inflammatory polyneuropathy.
Chronic Inflammatory Polyneuropathy
Chronic inflammatory demyelinating polyneuropathy, an acquired immunologically mediated disorder, is clinically similar to Guillain-Barr syndrome except that it has a relapsing or steadily progressive course over months or years. In the relapsing form, partial recovery may occur after some relapses, but in other instances there is no recovery between exacerbations. Although remission may occur spontaneously with time,
P.1052
the disorder frequently follows a progressive downhill course leading to severe functional disability.
Electrodiagnostic studies show marked slowing of motor and sensory conduction, and focal conduction block. Signs of partial denervation may also be present owing to secondary axonal degeneration. Nerve biopsy may show chronic perivascular inflammatory infiltrates in the endoneurium and epineurium, without accompanying evidence of vasculitis. However, a normal nerve biopsy result or the presence of nonspecific abnormalities does not exclude the diagnosis.
Corticosteroids may be effective in arresting or reversing the downhill course. Treatment is usually begun with prednisone, 60 mg daily, continued for 2 3 months or until a definite response has occurred. If no response has occurred despite 3 months of treatment, a higher dose may be tried. In responsive cases, the dose is gradually tapered, but most patients become corticosteroid-dependent, often requiring prednisone, 20 mg daily on alternate days, on a long-term basis. Patients unresponsive to corticosteroids may benefit instead from treatment with a cytotoxic drug such as azathioprine. There are increasing anecdotal reports of short-term benefit with plasmapheresis; high-dose intravenous immunoglobulin treatment (eg, 400 mg/kg/d) may produce clinical improvement lasting for weeks to months.
Briemberg HR et al: Inflammatory neuropathies. Curr Neurol Neurosci Rep 2005;5:66.
Donofrio PD: Immunotherapy of idiopathic inflammatory neuropathies. Muscle Nerve 2003;28:273.
Kieseier BC et al: Advances in understanding and treatment of immune-mediated disorders of the peripheral nervous system. Muscle Nerve 2004;30:131.
Mendell JR et al: Clinical practice. Painful sensory neuropathy. N Engl J Med 2003;348:1243.
Polydefkis M et al: New insights into diabetic polyneuropathy. JAMA 2003;290:1371.
Wolfe GI et al: Painful peripheral neuropathy and its nonsurgical treatment. Muscle Nerve 2004;30:3.
2. Mononeuropathies
![]() Essentials of Diagnosis
Essentials of Diagnosis
Focal motor or sensory deficit.
Deficit is in territory of an individual peripheral nerve.
An individual nerve may be injured along its course or may be compressed, angulated, or stretched by neighboring anatomic structures, especially at a point where it passes through a narrow space (entrapment neuropathy). The relative contributions of mechanical factors and ischemia to the local damage are not clear. With involvement of a sensory or mixed nerve, pain is commonly felt distal to the lesion. Symptoms never develop with some entrapment neuropathies, resolve rapidly and spontaneously in others, and become progressively more disabling and distressing in yet other cases. The precise neurologic deficit depends on the nerve involved. Percussion of the nerve at the site of the lesion may lead to paresthesias in its distal distribution.
Entrapment neuropathy may be the sole manifestation of subclinical polyneuropathy, and this must be borne in mind and excluded by nerve conduction studies. Such studies are also indispensable for the accurate localization of the focal lesion.
In patients with acute compression neuropathy such as may occur in intoxicated individuals ( Saturday night palsy ), no treatment is necessary. Complete recovery generally occurs, usually within 2 months, presumably because the underlying pathology is demyelination. However, axonal degeneration can occur in severe cases, and recovery then takes longer and may never be complete.
In chronic compressive or entrapment neuropathies, avoidance of aggravating factors and correction of any underlying systemic conditions are important. Local infiltration of the region about the nerve with corticosteroids may be of value; in addition, surgical decompression may help if there is a progressively increasing neurologic deficit or if electrodiagnostic studies show evidence of partial denervation in weak muscles.
Peripheral nerve tumors are uncommon, except in Recklinghausen's disease, but also give rise to mononeuropathy. This may be distinguishable from entrapment neuropathy only by noting the presence of a mass along the course of the nerve and by demonstrating the precise site of the lesion with appropriate electrophysiologic studies. Treatment of symptomatic lesions is by surgical removal if possible.
Carpal Tunnel Syndrome
See Chapter 20.
Pronator Teres or Anterior Interosseous Syndrome
The median nerve gives off its motor branch, the anterior interosseous nerve, below the elbow as it descends between the two heads of the pronator teres muscle. A lesion of either nerve may occur in this region, sometimes after trauma or owing to compression from, for example, a fibrous band. With anterior interosseous nerve involvement, there is no sensory loss, and weakness is confined to the pronator quadratus, flexor pollicis longus, and the flexor digitorum profundus to the second and third digits. Weakness is more widespread and sensory changes occur in an appropriate distribution when the median nerve itself is affected. The prognosis is variable. If improvement does not occur spontaneously, decompressive surgery may be helpful.
Ulnar Nerve Lesions
Ulnar nerve lesions are likely to occur in the elbow region as the nerve runs behind the medial epicondyle
P.1053
and descends into the cubital tunnel. In the condylar groove, the ulnar nerve is exposed to pressure or trauma. Moreover, any increase in the carrying angle of the elbow, whether congenital, degenerative, or traumatic, may cause excessive stretching of the nerve when the elbow is flexed. Ulnar nerve lesions may also result from thickening or distortion of the anatomic structures forming the cubital tunnel, and the resulting symptoms may also be aggravated by flexion of the elbow, because the tunnel is then narrowed by tightening of its roof or inward bulging of its floor. A severe lesion at either site causes sensory changes in the medial 11/2 digits and along the medial border of the hand. There is weakness of the ulnar-innervated muscles in the forearm and hand. With a cubital tunnel lesion, however, there may be relative sparing of the flexor carpi ulnaris muscle. Electrophysiologic evaluation using nerve stimulation techniques allows more precise localization of the lesion.
If conservative measures are unsuccessful in relieving symptoms and preventing further progression, surgical treatment may be necessary. This consists of nerve transposition if the lesion is in the condylar groove, or a release procedure if it is in the cubital tunnel.
Ulnar nerve lesions may also develop at the wrist or in the palm of the hand, usually owing to repetitive trauma or to compression from ganglia or benign tumors. They can be subdivided depending on their presumed site. Compressive lesions are treated surgically. If repetitive mechanical trauma is responsible, this is avoided by occupational adjustment or job retraining.
Radial Nerve Lesions
The radial nerve is particularly liable to compression or injury in the axilla (eg, by crutches or by pressure when the arm hangs over the back of a chair). This leads to weakness or paralysis of all the muscles supplied by the nerve, including the triceps. Sensory changes may also occur but are often surprisingly inconspicuous, being marked only in a small area on the back of the hand between the thumb and index finger. Injuries to the radial nerve in the spiral groove occur characteristically during deep sleep, as in intoxicated individuals (Saturday night palsy), and there is then sparing of the triceps muscle, which is supplied more proximally. The nerve may also be injured at or above the elbow; its purely motor posterior interosseous branch, supplying the extensors of the wrist and fingers, may be involved immediately below the elbow, but then there is sparing of the extensor carpi radialis longus, so that the wrist can still be extended. The superficial radial nerve may be compressed by handcuffs or a tight watch strap.
Femoral Neuropathy
The clinical features of femoral nerve palsy consist of weakness and wasting of the quadriceps muscle, with sensory impairment over the anteromedian aspect of the thigh and sometimes also of the leg to the medial malleolus, and a depressed or absent knee jerk. Isolated femoral neuropathy may occur in diabetics or from compression by retroperitoneal neoplasms or hematomas (eg, expanding aortic aneurysm). Femoral neuropathy may also result from pressure from the inguinal ligament when the thighs are markedly flexed and abducted, as in the lithotomy position.
Meralgia Paresthetica
The lateral femoral cutaneous nerve, a sensory nerve arising from the L2 and L3 roots, may be compressed or stretched in obese or diabetic patients and during pregnancy. The nerve usually runs under the outer portion of the inguinal ligament to reach the thigh, but the ligament sometimes splits to enclose it. Hyperextension of the hip or increased lumbar lordosis such as occurs during pregnancy leads to nerve compression by the posterior fascicle of the ligament. However, entrapment of the nerve at any point along its course may cause similar symptoms, and several other anatomic variations predispose the nerve to damage when it is stretched. Pain, paresthesia, or numbness occurs about the outer aspect of the thigh, usually unilaterally, and is sometimes relieved by sitting. Examination shows no abnormalities except in severe cases when cutaneous sensation is impaired in the affected area. Symptoms are usually mild and commonly settle spontaneously. Hydrocortisone injections medial to the anterosuperior iliac spine often relieve symptoms temporarily, while nerve decompression by transposition may provide more lasting relief.
Sciatic & Common Peroneal Nerve Palsies
Misplaced deep intramuscular injections are probably still the most common cause of sciatic nerve palsy. Trauma to the buttock, hip, or thigh may also be responsible. The resulting clinical deficit depends on whether the whole nerve has been affected or only certain fibers. In general, the peroneal fibers of the sciatic nerve are more susceptible to damage than those destined for the tibial nerve. A sciatic nerve lesion may therefore be difficult to distinguish from peroneal neuropathy unless there is electromyographic evidence of involvement of the short head of the biceps femoris muscle. The common peroneal nerve itself may be compressed or injured in the region of the head and neck of the fibula, eg, by sitting with crossed legs or wearing high boots. There is weakness of dorsiflexion and eversion of the foot, accompanied by numbness or blunted sensation of the anterolateral aspect of the calf and dorsum of the foot.
Tarsal Tunnel Syndrome
The tibial nerve, the other branch of the sciatic, supplies several muscles in the lower extremity, gives origin to the sural nerve, and then continues as the posterior
P.1054
tibial nerve to supply the plantar flexors of the foot and toes. It passes through the tarsal tunnel behind and below the medial malleolus, giving off calcaneal branches and the medial and lateral plantar nerves that supply small muscles of the foot and the skin on the plantar aspect of the foot and toes. Compression of the posterior tibial nerve or its branches between the bony floor and ligamentous roof of the tarsal tunnel leads to pain, paresthesias, and numbness over the bottom of the foot, especially at night, with sparing of the heel. Muscle weakness may be hard to recognize clinically. Compressive lesions of the individual plantar nerves may also occur more distally, with clinical features similar to those of the tarsal tunnel syndrome. Treatment is surgical decompression.
Brown WF, Bolton CF, Aminoff MJ (eds): Neuromuscular Function and Disease, 2 vols. Saunders, 2002.
Katz JN et al: Clinical practice. Carpal tunnel syndrome. N Engl J Med 2002; 346:1807.
Facial Neuropathy
An isolated facial palsy may occur in patients with HIV seropositivity, sarcoidosis, or Lyme disease (see Chapter 34), but most often it is idiopathic (Bell's palsy).
3. Bell's Palsy
![]() Essentials of Diagnosis
Essentials of Diagnosis
Sudden onset of lower motor neuron facial palsy.
Hyperacusis or impaired taste may occur.
No other neurologic abnormalities.
General Considerations
Bell's palsy is an idiopathic facial paresis of lower motor neuron type that has been attributed to an inflammatory reaction involving the facial nerve near the stylomastoid foramen or in the bony facial canal. Increasing evidence incriminates reactivation of herpes simplex virus infection in the geniculate ganglion at least in some instances. The disorder is more common in pregnant women or in persons with diabetes.
Clinical Findings
The facial paresis generally comes on abruptly, but it may worsen over the following day or so. Pain about the ear precedes or accompanies the weakness in many cases but usually lasts for only a few days. The face itself feels stiff and pulled to one side. There may be ipsilateral restriction of eye closure and difficulty with eating and fine facial movements. A disturbance of taste is common, owing to involvement of chorda tympani fibers, and hyperacusis due to involvement of fibers to the stapedius occurs occasionally.
Treatment
Other disorders that can produce a facial palsy and require specific treatment, such as tumors, Lyme disease, AIDS, sarcoidosis, and herpes zoster infection of the geniculate ganglion, must be excluded. The management of Bell's palsy is controversial. Approximately 60% of cases recover completely without treatment, presumably because the lesion is so mild that it leads merely to conduction block. Considerable improvement occurs in most other cases, and only about 10% of all patients have permanent disfigurement or other long-term sequelae. Treatment is unnecessary in most cases but is indicated for patients in whom an unsatisfactory outcome can be predicted. The best clinical guide to progress is the severity of the palsy during the first few days after presentation. Patients with clinically complete palsy when first seen are less likely to make a full recovery than those with an incomplete one. A poor prognosis for recovery is also associated with advanced age, hyperacusis, and severe initial pain. Electromyography and nerve excitability or conduction studies provide a guide to prognosis but not early enough to aid in the selection of patients for treatment.
The only medical treatment that may influence the outcome is administration of corticosteroids, but this is unclear. Many clinicians nevertheless routinely prescribe corticosteroids for patients with Bell's palsy seen within 5 days of onset. The author prescribes them only when the palsy is clinically complete or there is severe pain. Treatment with prednisone, 60 or 80 mg daily in divided doses for 4 or 5 days, followed by tapering of the dose over the next 7 10 days, is a satisfactory regimen. It is helpful to protect the eye with lubricating drops (or lubricating ointment at night) and a patch if eye closure is not possible. It is unclear whether acyclovir or other antiviral agents confer any benefit. There is no evidence that surgical procedures to decompress the facial nerve are of benefit.
Gilden DH: Clinical practice. Bell's palsy. N Engl J Med 2004; 351:1323.
Holland NJ et al: Recent developments in Bell's palsy. BMJ 2004; 329:553.
Discogenic Neck Pain
![]() Essentials of Diagnosis
Essentials of Diagnosis
Neck pain, sometimes radiating to arms.
Restricted neck movements.
Motor, sensory, or reflex changes in arms with root involvement.
Neurologic deficit in legs, gait disorder, or sphincter disturbance with cord involvement.
P.1055
General Considerations
A variety of congenital abnormalities may involve the cervical spine and lead to neck pain; these include hemivertebrae, fused vertebrae, basilar impression, and instability of the atlantoaxial joint. Traumatic, degenerative, infective, and neoplastic disorders may also lead to pain in the neck. When rheumatoid arthritis involves the spine, it tends to affect especially the cervical region, leading to pain, stiffness, and reduced mobility; displacement of vertebrae or atlantoaxial subluxation may lead to cord compression that can be life-threatening if not treated by fixation. Further details are given in Chapter 20 (including a discussion on low back pain), and discussion here is restricted to disk disease.
Acute Cervical Disk Protrusion
Acute cervical disk protrusion leads to pain in the neck and radicular pain in the arm, exacerbated by head movement. With lateral herniation of the disk, motor, sensory, or reflex changes may be found in a radicular (usually C6 or C7) distribution on the affected side (Figure 24-1); with more centrally directed herniations, the spinal cord may also be involved, leading to spastic paraparesis and sensory disturbances in the legs, sometimes accompanied by impaired sphincter function. The diagnosis is confirmed by MRI or CT myelography. In mild cases, bed rest or intermittent neck traction may help, followed by immobilization of the neck in a collar for several weeks. If these measures are unsuccessful or the patient has a significant neurologic deficit, surgical removal of the protruding disk may be necessary.
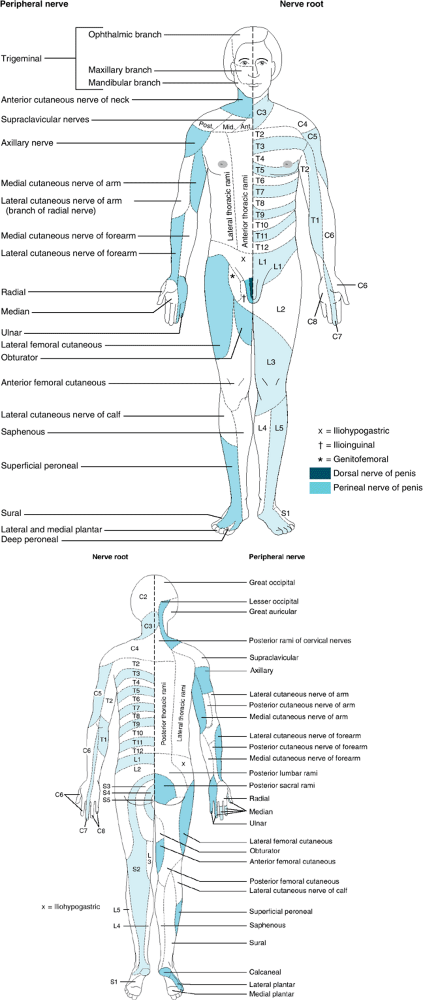 |
Figure 24-1. Cutaneous innervation. The segmental or radicular (root) distribution is shown on the left side of the body and the peripheral nerve distribution on the right side. Above: anterior view; facing page: posterior view. (Reproduced, with permission, from Simon RP et al: Clinical Neurology, 4th ed. McGraw-Hill, 1999. ) |
Cervical Spondylosis
Cervical spondylosis results from chronic cervical disk degeneration, with herniation of disk material, secondary calcification, and associated osteophytic outgrowths. One or more of the cervical nerve roots may be compressed, stretched, or angulated; and myelopathy may also develop as a result of compression, vascular insufficiency, or recurrent minor trauma to the cord. Patients present with neck pain and restricted head movement, occipital headaches, radicular pain and other sensory disturbances in the arms, weakness of the arms or legs, or some combination of these symptoms. Examination generally reveals that lateral flexion and rotation of the neck are limited. A segmental pattern of weakness or dermatomal sensory loss (or both) may be found unilaterally or bilaterally in the upper limbs, and tendon reflexes mediated by the affected root or roots are depressed. The C5 and C6 nerve roots are most commonly involved, and examination frequently then reveals weakness of muscles supplied by these roots (eg, deltoids, supraspinatus and infraspinatus, biceps, brachioradialis), pain or sensory loss about the shoulder and outer border of the arm and forearm, and depressed biceps and brachioradialis reflexes. Spastic paraparesis may also be present if there is an associated myelopathy, sometimes accompanied by posterior column or spinothalamic sensory deficits in the legs.
Plain radiographs of the cervical spine show osteophyte formation, narrowing of disk spaces, and encroachment on the intervertebral foramina, but such changes are common in middle-aged persons and may be unrelated to the presenting complaint. CT or MRI helps confirm the diagnosis and exclude other structural causes of the myelopathy.
Restriction of neck movements by a cervical collar may relieve pain. Operative treatment may be necessary to prevent further progression if there is a significant neurologic deficit or if root pain is severe, persistent, and unresponsive to conservative measures.
Brachial & Lumbar Plexus Lesions
Brachial Plexus Neuropathy
Brachial plexus neuropathy may be idiopathic, sometimes occurring in relationship to a number of different nonspecific illnesses or factors. In other instances, brachial plexus lesions follow trauma or result from congenital anomalies, neoplastic involvement, or injury by various physical agents. In rare instances, the disorder occurs on a familial basis.
Idiopathic brachial plexus neuropathy (neuralgic amyotrophy) characteristically begins with severe pain about the shoulder, followed within a few days by weakness, reflex changes, and sensory disturbances involving especially the C5 and C6 segments. Symptoms and signs are usually unilateral but may be bilateral. Wasting of affected muscles is sometimes profound. The disorder relates to disturbed function of cervical roots or part of the brachial plexus, but its precise cause is unknown. Recovery occurs over the ensuing months but may be incomplete. Treatment is purely symptomatic.
Cervical Rib Syndrome
Compression of the C8 and T1 roots or the lower trunk of the brachial plexus by a cervical rib or band arising from the seventh cervical vertebra leads to weakness and wasting of intrinsic hand muscles, especially those in the thenar eminence, accompanied by pain and numbness in the medial two fingers and the ulnar border of the hand and forearm. The subclavian artery may also be compressed, and this forms the basis of Adson's test for diagnosing the disorder; the radial pulse is diminished or obliterated on the affected side when the seated patient inhales deeply and turns the head to one side or the other. Electromyography, nerve conduction studies, and somatosensory evoked potential studies may help confirm the diagnosis. X-rays sometimes show the cervical rib or a large transverse process of the seventh cervical vertebra, but normal findings do not exclude the possibility of a cervical band. Treatment of the disorder is by surgical excision of the rib or band.
P.1056
Lumbosacral Plexus Lesions
A lumbosacral plexus lesion may develop in association with diseases such as diabetes, cancer, or bleeding disorders or in relation to injury. It occasionally occurs as an isolated phenomenon similar to idiopathic brachial plexopathy, and pain and weakness then tend to be more conspicuous than sensory symptoms. The distribution of symptoms and signs depends on the level and pattern of neurologic involvement.
P.1057
P.1058
Disorders of Neuromuscular Transmission
1. Myasthenia Gravis
![]() Essentials of Diagnosis
Essentials of Diagnosis
Fluctuating weakness of commonly used voluntary muscles, producing symptoms such as diplopia, ptosis, and difficulty in swallowing.
Activity increases weakness of affected muscles.
Short-acting anticholinesterases transiently improve the weakness.
General Considerations
Myasthenia gravis occurs at all ages, sometimes in association with a thymic tumor or thyrotoxicosis, as well as in rheumatoid arthritis and lupus erythematosus. It is most common in young women with HLA-DR3; if thymoma is associated, older men are more commonly affected. Onset is usually insidious, but the disorder is sometimes unmasked by a coincidental infection that leads to exacerbation of symptoms. Exacerbations may also occur before the menstrual period and during or shortly after pregnancy. Symptoms are due to a variable degree of block of neuromuscular transmission caused by autoantibodies binding to acetylcholine receptors; these are found in most patients with the disease and have a primary role in reducing the number of functioning acetylcholine receptors. Additionally, cellular immune activity against the receptor is found. Clinically, this leads to weakness; initially powerful movements fatigue readily. The external ocular muscles and certain other cranial muscles, including the masticatory, facial, and pharyngeal muscles, are especially likely to be affected, and the respiratory and limb muscles may also be involved.
Clinical Findings
A. Symptoms and Signs
Patients present with ptosis, diplopia, difficulty in chewing or swallowing, respiratory difficulties, limb weakness, or some combination of these problems. Weakness may remain localized to a few muscle groups, especially the ocular muscles, or may become generalized. Symptoms often fluctuate in intensity during the day, and this diurnal variation is superimposed on a tendency to longer-term spontaneous relapses and remissions that may last for weeks. Nevertheless, the disorder follows a slowly progressive course and may have a fatal outcome owing to respiratory complications such as aspiration pneumonia.
Clinical examination confirms the weakness and fatigability of affected muscles. In most cases, the extraocular muscles are involved, and this leads to ocular palsies and ptosis, which are commonly asymmetric. Pupillary responses are normal. The bulbar and limb muscles are often weak, but the pattern of involvement is variable. Sustained activity of affected muscles increases the weakness, which improves after a brief rest. Sensation is normal, and there are usually no reflex changes.
The diagnosis can generally be confirmed by the response to a short-acting anticholinesterase. Edrophonium can be given intravenously in a dose of 10 mg (1 mL), 2 mg being given initially and the remaining 8 mg about 30 seconds later if the test dose is well tolerated; in myasthenic patients, there is an obvious improvement in strength of weak muscles lasting for about 5 minutes. Alternatively, 1.5 mg of neostigmine can be given intramuscularly, and the response then lasts for about 2 hours; atropine sulfate (0.6 mg) should be available to reverse muscarinic side effects.
B. Imaging
Lateral and anteroposterior x-rays of the chest and CT scans should be obtained to demonstrate a coexisting thymoma, but normal studies do not exclude this possibility.
C. Laboratory and Other Studies
Electrophysiologic demonstration of a decrementing muscle response to repetitive 2- or 3-Hz stimulation of motor nerves indicates a disturbance of neuromuscular transmission. Such an abnormality may even be detected in clinically strong muscles with certain provocative procedures. Needle electromyography of affected muscles shows a marked variation in configuration and size of individual motor unit potentials, and single-fiber electromyography reveals an increased jitter, or variability, in the time interval between two muscle fiber action potentials from the same motor unit.
Assay of serum for elevated levels of circulating acetylcholine receptor antibodies is useful because it has a sensitivity of 80 90% for the diagnosis of myasthenia gravis. Certain patients without antibodies to acetylcholine receptors have serum antibodies to muscle-specific tyrosine kinase (MuSK), which should therefore be determined; the response to anticholinesterase and immunosuppressive treatment is similar regardless of which of these two antibodies is present.
Treatment
Medication such as aminoglycosides that may exacerbate myasthenia gravis should be avoided. Anticholinesterase drugs provide symptomatic benefit without influencing the course of the disease. Neostigmine, pyridostigmine, or both can be used, the dose being determined on an individual basis. The usual dose of neostigmine is 7.5 30 mg (average, 15 mg) taken four times daily; of pyridostigmine, 30 180 mg (average, 60 mg) four times daily. Overmedication may temporarily increase weakness, which is then unaffected or enhanced by intravenous edrophonium.
Thymectomy usually leads to symptomatic benefit or remission and should be considered in all patients
P.1059
younger than age 60, unless weakness is restricted to the extraocular muscles. If the disease is of recent onset and only slowly progressive, operation is sometimes delayed for a year or so, in the hope that spontaneous remission will occur.
Treatment with corticosteroids is indicated for patients who have responded poorly to anticholinesterase drugs and have already undergone thymectomy. It is often introduced with the patient in the hospital, since weakness may initially be aggravated. Once weakness has stabilized after 2 3 weeks or any improvement is sustained, further management can be on an outpatient basis. Alternate-day treatment is usually well tolerated, but if weakness is enhanced on the nontreatment day it may be necessary for medication to be taken daily. The dose of corticosteroids is determined on an individual basis, but an initial high daily dose (eg, prednisone, 60 100 mg) can gradually be tapered to a relatively low maintenance level as improvement occurs; total withdrawal is difficult, however. Treatment with azathioprine may also be effective. The usual dose is 2 3 mg/kg orally daily after a lower initial dose.
In patients with major disability in whom conventional treatment is either unhelpful or contraindicated, plasmapheresis or intravenous immunoglobulin therapy may be beneficial. It may also be useful for stabilizing patients before thymectomy and for managing acute crisis. Mycophenolate mofetil, an immunosuppressant, has also been used, and preliminary studies indicate that it may provide symptomatic benefit and allow the corticosteroid dose to be reduced.
Keesey JC: Clinical evaluation and management of myasthenia gravis. Muscle Nerve 2004;29:484.
Zhou L et al: Clinical comparison of muscle-specific tyrosine kinase (MuSK) antibody-positive and -negative myasthenic patients. Muscle Nerve 2004;30:55.
2. Myasthenic Syndrome (Lambert-Eaton Syndrome)
![]() Essentials of Diagnosis
Essentials of Diagnosis
Variable weakness, typically improving with activity.
Dysautonomic symptoms may also be present.
A history of malignant disease may be obtained.
General Considerations
Myasthenic syndrome (see Table 40-6) may be associated with small-cell carcinoma, sometimes developing before the tumor is diagnosed, and occasionally occurs with certain autoimmune diseases. There is defective release of acetylcholine in response to a nerve impulse, and this leads to weakness, especially of the proximal muscles of the limbs. As is not the case in myasthenia gravis, however, power steadily increases with sustained contraction. The diagnosis can be confirmed electrophysiologically, because the muscle response to stimulation of its motor nerve increases remarkably if the nerve is stimulated repetitively at high rates, even in muscles that are not clinically weak.
Treatment with plasmapheresis and immunosuppressive drug therapy (prednisone and azathioprine) may lead to clinical and electrophysiologic improvement, in addition to therapy aimed at tumor when present. Prednisone is usually initiated in a daily dose of 60 80 mg and azathioprine in a daily dose of 2 mg/kg. Guanidine hydrochloride (25 50 mg/kg/d in divided doses) is occasionally helpful in seriously disabled patients, but adverse effects of the drug include marrow suppression. The response to treatment with anticholinesterase drugs such as pyridostigmine or neostigmine, either alone or in combination with guanidine, is variable.
3. Botulism
The toxin of Clostridium botulinum prevents the release of acetylcholine at neuromuscular junctions and autonomic synapses. Botulism occurs most commonly following the ingestion of contaminated home-canned food and should be suggested by the development of sudden, fluctuating, severe weakness in a previously healthy person. Symptoms begin within 72 hours following ingestion of the toxin and may progress for several days. Typically, there is diplopia, ptosis, facial weakness, dysphagia, and nasal speech, followed by respiratory difficulty and finally by weakness that appears last in the limbs. Blurring of vision (with unreactive dilated pupils) is characteristic, and there may be dryness of the mouth, constipation (paralytic ileus), and postural hypotension. Sensation is preserved, and the tendon reflexes are not affected unless the involved muscles are very weak. If the diagnosis is suspected, the local health authority should be notified and a sample of serum and contaminated food (if available) sent to be assayed for toxin. Support for the diagnosis may be obtained by electrophysiologic studies; with repetitive stimulation of motor nerves at fast rates, the muscle response increases in size progressively.
Patients should be hospitalized in case respiratory assistance becomes necessary. Treatment is with trivalent antitoxin, once it is established that the patient is not allergic to horse serum. Guanidine hydrochloride (25 50 mg/kg/d in divided doses) to facilitate release of acetylcholine from nerve endings sometimes helps to increase muscle strength. Anticholinesterase drugs are of no value. Respiratory assistance and other supportive measures should be provided as necessary. Further details are provided in Chapter 33.
4. Disorders Associated with Use of Aminoglycosides
Aminoglycoside antibiotics, eg, gentamicin, may produce a clinical disturbance similar to botulism by preventing the release of acetylcholine from nerve endings,
P.1060
but symptoms subside rapidly as the responsible drug is eliminated from the body. These antibiotics are particularly dangerous in patients with preexisting disturbances of neuromuscular transmission and are therefore best avoided in patients with myasthenia gravis.
Myopathic Disorders
1. Muscular Dystrophies
![]() Essentials of Diagnosis
Essentials of Diagnosis
Muscle weakness, often in a characteristic distribution.
Age at onset and inheritance pattern depend on the specific dystrophy.
General Considerations
These inherited myopathic disorders are characterized by progressive muscle weakness and wasting. They are subdivided by mode of inheritance, age at onset, and clinical features, as shown in Table 24-8. In the Duchenne type, pseudohypertrophy of muscles frequently occurs at some stage; intellectual retardation is common; and there may be skeletal deformities, muscle contractures, and cardiac involvement. The serum creatine kinase level is increased, especially in the Duchenne and Becker varieties, and mildly increased also in limb-girdle dystrophy. Electromyography may help confirm that weakness is myopathic rather than neurogenic. Similarly, histopathologic examination of a muscle biopsy specimen may help confirm that weakness is due to a primary disorder of muscle and to distinguish between various muscle diseases.
A genetic defect on the short arm of the X chromosome has been identified in Duchenne dystrophy. The affected gene codes for the protein dystrophin, which is markedly reduced or absent from the muscle of patients with the disease. Dystrophin levels are generally normal in the Becker variety, but the protein is qualitatively altered.
Duchenne muscular dystrophy can now be recognized early in pregnancy in about 95% of women by genetic studies; in late pregnancy, DNA probes can be used on fetal tissue obtained for this purpose by amniocentesis.
P.1061
The genes causing some of the other muscular dystrophies are listed in Table 24-8.
Table 24-8. The muscular dystrophies. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
There is no specific treatment for the muscular dystrophies, but it is important to encourage patients to lead as normal lives as possible. Prednisone (0.75 mg/kg daily) improves muscle strength and function in boys with Duchenne dystrophy, but side effects need to be monitored. Prolonged bed rest must be avoided, as inactivity often leads to worsening of the underlying muscle disease. Physical therapy and orthopedic procedures may help counteract deformities or contractures.
Kirschner J et al: The congenital and limb-girdle muscular dystrophies. Arch Neurol 2004;61:189.
Moxley RT 3rd et al: Practice parameter: corticosteroid treatment of Duchenne dystrophy: report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology 2005;64:13.
2. Myotonic Dystrophy
Myotonic dystrophy, a slowly progressive, dominantly inherited disorder, usually manifests itself in the third or fourth decade but occasionally appears early in childhood. The genetic defect has been localized to the long arm of chromosome 19 in the type 1 disorder. Myotonia leads to complaints of muscle stiffness and is evidenced by the marked delay that occurs before affected muscles can relax after a contraction. This can often be demonstrated clinically by delayed relaxation of the hand after sustained grip or by percussion of the belly of a muscle. In addition, there is weakness and wasting of the facial, sternocleidomastoid, and distal limb muscles. Associated clinical features include cataracts, frontal baldness, testicular atrophy, diabetes mellitus, cardiac abnormalities, and intellectual changes. In myotonic dystrophy type 2, the clinical features are similar but a different gene is involved (3q21.3). Electromyographic sampling of affected muscles reveals myotonic discharges in addition to changes suggestive of myopathy.
Myotonia can be treated with phenytoin (100 mg three times daily), quinine sulfate (300 400 mg three times daily), or procainamide (0.5 1 g four times daily). More recently, tocainide and mexiletine have been used. Phenytoin is preferred, since the other drugs may have undesirable effects on cardiac conduction. Neither the weakness nor the course of the disorder is influenced by treatment.
Machuca-Tzili L et al: Clinical and molecular aspects of the myotonic dystrophies: a review. Muscle Nerve 2005;32:1.
3. Myotonia Congenita
Myotonia congenita is commonly inherited as a dominant trait. The responsible gene may be on the long arm of chromosome 7. Generalized myotonia without weakness is usually present from birth, but symptoms may not appear until early childhood. Patients complain of muscle stiffness that is enhanced by cold and inactivity and relieved by exercise. Muscle hypertrophy, at times pronounced, is also a feature. A recessive form with later onset is associated with slight weakness and atrophy of distal muscles. Treatment with quinine sulfate, procainamide, tocainide, mexiletine, or phenytoin may help the myotonia, as in myotonic dystrophy.
4. Polymyositis & Dermatomyositis
See Chapter 20.
5. Inclusion Body Myositis
This disorder, of unknown cause, begins insidiously, usually after middle age, with progressive proximal weakness of first the lower and then the upper extremities. Distal weakness is usually mild. Serum creatine kinase levels may be normal or increased. The diagnosis is confirmed by muscle biopsy. In contrast to polymyositis, corticosteroid therapy is usually ineffective. The role of intravenous immunoglobulin therapy is unclear.
Mastaglia FL et al: Inflammatory myopathies: clinical, diagnostic and therapeutic aspects. Muscle Nerve 2003;27:407.
6. Mitochondrial Myopathies
The mitochondrial myopathies are a clinically diverse group of disorders that on pathologic examination of skeletal muscle with the modified Gomori stain show characteristic ragged red fibers containing accumulations of abnormal mitochondria. Patients may present with progressive external ophthalmoplegia or with limb weakness that is exacerbated or induced by activity. Other patients present with central neurologic dysfunction, eg, myoclonic epilepsy (myoclonic epilepsy, ragged red fiber syndrome, or MERRF), or the combination of myopathy, encephalopathy, lactic acidosis, and stroke-like episodes (MELAS). These disorders result from separate abnormalities of mitochondrial DNA. (See also Chapter 20.)
7. Myopathies Associated with Other Disorders
Myopathy may occur in association with chronic hypokalemia, any endocrinopathy, and in patients taking corticosteroids, chloroquine, colchicine, clofibrate, emetine, aminocaproic acid, lovastatin, bretylium tosylate, or drugs causing potassium depletion. Weakness is mainly proximal, and serum creatine kinase is typically normal, except in hypothyroidism and some of the toxic myopathies. Treatment is of the underlying cause. Myopathy also occurs with chronic alcoholism, whereas acute reversible muscle necrosis may occur shortly after acute alcohol intoxication. Inflammatory
P.1062
myopathy may occur in patients taking penicillamine; myotonia may be induced by clofibrate, and preexisting myotonia may be exacerbated or unmasked by depolarizing muscle relaxants (eg, suxamethonium), -blockers (eg, propranolol), fenoterol, ritodrine and, possibly, certain diuretics.
Periodic Paralysis Syndrome
Periodic paralysis may have a familial (dominant inheritance) basis. Episodes of flaccid weakness or paralysis occur, sometimes in association with abnormalities of the plasma potassium level. Strength is normal between attacks. Hypokalemic periodic paralysis is characterized by attacks that tend to occur on awakening, after exercise, or after a heavy meal and may last for several days. Patients should avoid excessive exertion. A low-carbohydrate and low-salt diet may help prevent attacks, as may acetazolamide, 250 750 mg/d. An ongoing attack may be aborted by potassium chloride given orally or by intravenous drip, provided the ECG can be monitored and renal function is satisfactory. In young Asian men, it is commonly associated with hyperthyroidism; treatment of the endocrine disorder then prevents recurrences. In hyperkalemic periodic paralysis, attacks also tend to occur after exercise but usually last for less than an hour. They may be terminated by intravenous calcium gluconate (1 2 g) or by intravenous diuretics (furosemide, 20 40 mg), glucose, or glucose and insulin; daily acetazolamide or chlorothiazide may prevent recurrences. Genetic linkage studies suggest that many families with this disorder have a defect in the sodium channel gene on the long arm of chromosome 17. %Normokalemic periodic paralysis is similar clinically to the hyperkalemic variety, but the plasma potassium level remains normal during attacks; treatment is with acetazolamide.
Renner DR et al: Periodic paralyses and nondystrophic myotonias. Adv Neurol 2002;88:235.
EAN: 2147483647
Pages: 49