8 - Ear, Nose, Throat
Editors: McPhee, Stephen J.; Papadakis, Maxine A.; Tierney, Lawrence M.
Title: Current Medical Diagnosis & Treatment, 46th Edition
Copyright 2007 McGraw-Hill
> Table of Contents > 11 - Systemic Hypertension
function show_scrollbar() {}
11
Systemic Hypertension
Michael Sutters MD
Fifty million Americans have elevated blood pressure (systolic blood pressure 140 mm Hg or diastolic blood pressure 90 mm Hg); of these, 70% are aware of their diagnosis, but only 50% are receiving treatment and only 25% are under control using a threshold criterion of 140/90 mm Hg. The prevalence of hypertension increases with age and is more common in blacks than in whites. The mortality rates for stroke and coronary heart disease, two of the major complications of hypertension, have declined by up to 60% over the past three decades but have recently leveled off. The numbers of patients with end-stage renal disease and heart failure two other conditions in which hypertension plays a major causative role continue to rise.
Cardiovascular morbidity and mortality increase as both systolic and diastolic blood pressures rise, but in individuals over age 50 years, the systolic pressure and pulse pressure are better predictors of complications than diastolic pressure. Table 11-1 provides a summary of the classification and management of blood pressure in adults from the 7th Report of the U.S. Joint National Commission on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7).
How Is Blood Pressure Measured and Hypertension Diagnosed?
Blood pressure should be measured with a well-calibrated sphygmomanometer. The bladder width within the cuff should encircle at least 80% of the arm circumference. Readings should be taken after the patient has been resting comfortably, back supported in the sitting or supine position, for at least 5 minutes and at least 30 minutes after smoking or coffee ingestion. Hypertension is diagnosed when blood pressure is consistently elevated above 140/90 mm Hg; a single elevated blood pressure reading is not sufficient to establish the diagnosis of hypertension. The major exceptions to this rule are hypertensive presentations with unequivocal evidence of life-threatening end-organ damage, as seen in hypertensive emergency, or in hypertensive urgency where blood pressure is > 220/125 mm Hg but life-threatening end-organ damage is absent. In less severe cases, the diagnosis of hypertension depends on a series of measurements of blood pressure, since readings can vary and tend to regress toward the mean with time. Patients whose blood pressure is in a hypertensive range initially typically exhibit the greatest fall toward the normal range between the first and second encounters. Although blood pressure readings may still show variability after the third visit, these later changes are mostly random. However, the concern for diagnostic precision needs to be balanced by an appreciation of the importance of establishing the diagnosis of hypertension as quickly as possible, since a 3-month delay in treatment of hypertension in high-risk patients is associated with a twofold increase in cardiovascular morbidity and mortality. The guidelines of the 2005 Canadian Hypertension Education Program provide an algorithm designed to expedite the diagnosis of hypertension (Figure 11-1). To this end, they recommend short intervals between the initial office visits and the early identification of target organ damage which, if present, obviates the need for protracted confirmation of blood pressure elevation prior to pharmacologic intervention. In addition, the Canadian guidelines exploit the less volatile ambulatory and home blood pressure measurements as complements to office-based evaluations; hypertension is diagnosed at lower levels when based on measurements taken outside the office environment.
Prehypertension
Data from the Framingham cohort indicate that blood pressure bears a linear relationship with cardiovascular risk down to a systolic blood pressure of 115 mm Hg; based on these data, it is recommended that individuals with blood pressures in the gray area of 120 139/80 89 mm Hg be categorized as having prehypertension (Table 11-1). This demonstrates a trend away from defining hypertension as a simple numerical threshold and toward a more subtle appreciation of blood pressure as a component of overall cardiovascular risk. Although data concerning the treatment of prehypertension are lacking, the JNC guidelines suggest that antihypertensive medications be offered to persons with prehypertension with compelling indications (Table 11-1).
Table 11-1. Classification and management of blood pressure for adults aged 18 years or older. | |||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||||||||||
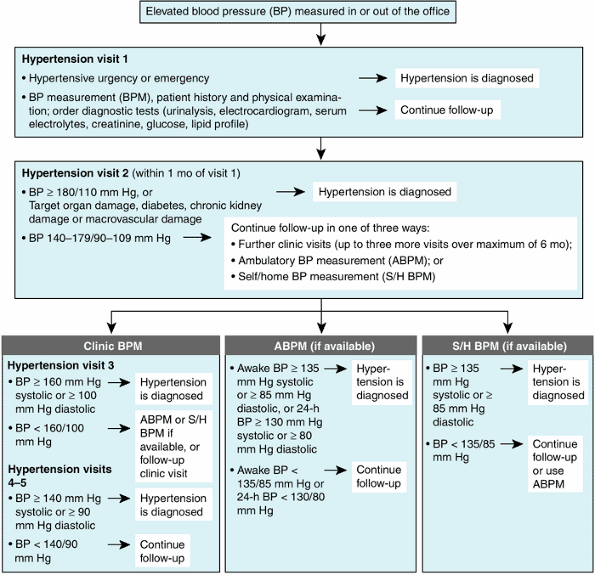 |
Figure 11-1. The 2005 Canadian Hypertension Education Program recommendations for the assessment and diagnosis of hypertension. Patients with an elevated blood pressure measured during visits 4 5 may still have white-coat (office-induced) hypertension. (Applying the 2005 Canadian Hypertension Education Program recommendations: 1. Diagnosis of hypertension Reprinted from, CMAJ 30-Aug-05; 173(5), Page(s) 480 483 by permission of the publisher. 2005 CMA Media Inc. ) |
The British Hypertension Society (BHS) guidelines make similar recommendations but go further by suggesting that antihypertensive medication also be offered to patients with prehypertension who have an elevated projected cardiovascular risk based on Framingham criteria (discussed below). Consequently, a low-risk patient with blood pressure between 120 139/80 89 mm Hg may be advised to make lifestyle modifications (Table 11-2)
P.430
and be monitored without receiving an absolute diagnosis of prehypertension. Circumspection about labeling patients is warranted since there is evidence that simply telling someone that he or she is hypertensive has unintended consequences, transforming a perception of general health into one of general ill-health. Nonetheless, because prehypertension often develops into hypertension (50% of people within 4 years), even low-risk prehypertensive patients should be monitored annually. To summarize, the diagnosis of hypertension is less important than deciding which patients will benefit from blood pressure reduction as part of a comprehensive risk reduction strategy.
Bolli P et al; Canadian Hypertension Education Program: Applying the 2005 Canadian Hypertension Education Program recommendations: 1. Diagnosis of hypertension. CMAJ 2005;173: 480.
Chaudhry SI et al: Systolic hypertension in older persons. JAMA 2004;292:1074.
Chobanian AV et al: The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 Report. JAMA 2003;289: 2560.
European Society of Hypertension-European Society of Cardiology Guidelines Committee: 2003 European Society of Hypertension-European Society of Cardiology guidelines for the management of arterial hypertension J Hypertens 2003; 21:1011.
Hart PD et al: Hypertension control rates: time for translation of guidelines into clinical practice. Am J Med 2004;117: 62.
Kaplan NM et al: Clinical Hypertension, 8th ed. Lippincott Williams & Wilkins, 2002.
Pepine C: What is the optimal blood pressure and drug therapy for patients with coronary artery disease? JAMA 2004;292:2271.
Pickering TG: Now we are sick: labeling and hypertension. J Clin Hypertens (Greenwich) 2006;8:57.
Sheridan S et al: Screening for high blood pressure: a review of the evidence for the U.S. Preventive Services Task Force. Am J Prev Med 2003;25:151.
Williams B et al; British Hypertension Society: Guidelines for management of hypertension: report of the fourth working party of the British Hypertension Society, 2004-BHS IV. J Hum Hypertens 2004;18:139.
Approach To Hypertension
Etiology & Classification
A. Primary (Essential) Hypertension
Primary (essential) hypertension is the term applied to the 95% of cases in which no cause for hypertension can be identified. This occurs in 10 15% of white
P.431
adults and 20 30% of black adults in the United States. The onset is usually between ages 25 and 55 years; it is uncommon before age 20 years. Much less commonly, hypertension arises from an identifiable cause, in which case it is called secondary hypertension (see below). The secondary form should be suspected in children or young adults and in older persons in whom onset of hypertension is new or in whom hypertension suddenly worsens.
The pathogenesis of primary (essential) hypertension is multifactorial. Genetic factors play an important role. Children have higher blood pressure when one parent is hypertensive (and more so when both parents are hypertensive). Environmental factors also are significant. Increased salt intake and obesity have long been incriminated. These factors alone are probably not sufficient to raise blood pressure to abnormal levels but are synergistic with a genetic predisposition. Other factors that may be involved in the pathogenesis of primary (essential) hypertension are sympathetic nervous system hyperactivity, abnormal cardiovascular development, renin-angiotensin system activity, defect in natriuresis, intracellular sodium and calcium, as well as exacerbating factors (including obesity, alcohol, cigarette smoking, and polycythemia).
Table 11-2. Lifestyle modifications to manage hypertension.1 | |||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||
P.432
1. Sympathetic nervous system hyperactivity
This is most apparent in younger persons with hypertension, who may exhibit tachycardia and an elevated cardiac output. However, correlations between plasma catecholamines and blood pressure are poor. Insensitivity of the baroreflexes may play a role in the genesis of adrenergic hyperactivity.
2. Abnormal cardiovascular development
The normal cardiovascular system develops so that elasticity of the great arteries is matched to the resistance in the periphery to optimize large vessel pressure waves. In this way, myocardial oxygen consumption is minimized and coronary flow maximized. Elevated blood pressure later in life could arise from abnormal development of aortic elasticity or reduced development of the microvascular network. This has been postulated as the sequence of events in low birth weight infants who have an increased risk of hypertension developing in adulthood.
3. Renin-angiotensin system activity
Renin, a proteolytic enzyme, is secreted by the juxtaglomerular cells surrounding afferent arterioles in response to a number of stimuli, including reduced renal perfusion pressure, diminished intravascular volume, circulating catecholamines, increased sympathetic nervous system activity, increased arteriolar stretch, and hypokalemia. Plasma renin levels are classified in relation to dietary sodium intake or urinary sodium excretion. Renin acts on angiotensinogen to cleave off the ten-amino-acid peptide angiotensin I. This peptide is then acted upon by angiotensin-converting enzyme (ACE) to create the eight-amino-acid peptide angiotensin II, a potent vasoconstrictor and a major stimulant of aldosterone release from the adrenal glands. The incidence of hypertension and its complications may be increased in individuals with the DD genotype of the allele coding for ACE. Despite the role of this system in the regulation of blood pressure, it probably does not play a central role in the pathogenesis of most primary (essential) hypertension; although approximately 10% of patients have high levels, 60% have normal levels, and 30% have low levels. Black persons with hypertension and older patients tend to have lower plasma renin activity, which may be associated with expanded intravascular volume.
4. Defect in natriuresis
Normal individuals increase their renal sodium excretion in response to elevations in arterial pressure and to a sodium or volume load. Hypertensive patients, particularly when their blood pressure is controlled, exhibit a diminished ability to excrete a sodium load. This defect may result in increased plasma volume and hypertension. During chronic hypertension, a sodium load is usually handled normally.
5. Intracellular sodium and calcium
Intracellular Na+ is elevated in blood cells and other tissues in primary (essential) hypertension. This may result from abnormalities in Na+-K+ exchange and other Na+ transport mechanisms. An increase in intracellular Na+ may lead to increased intracellular Ca2+ concentrations as a result of facilitated exchange and might explain the increase in vascular smooth muscle tone that is characteristic of established hypertension.
6. Exacerbating factors
A number of conditions elevate blood pressure, especially in predisposed individuals. Obesity is associated with an increase in intravascular volume and an elevated cardiac output. Weight reduction lowers blood pressure modestly. The relationship
P.433
between sodium intake and hypertension remains controversial, and some not all persons with hypertension respond to high salt intake with substantial increases in blood pressure. Patients with high normal or elevated blood pressures should consume no more than 100 mmol/d of salt (2.4 g of sodium, 6 g of sodium chloride daily).
Excessive use of alcohol also raises blood pressure, perhaps by increasing plasma catecholamines. Hypertension can be difficult to control in patients who consume more than 40 g of ethanol (two drinks) daily or drink in binges. Cigarette smoking raises blood pressure, again by increasing plasma norepinephrine. Although the long-term effect of smoking on blood pressure is less clear, the synergistic effects of smoking and high blood pressure on cardiovascular risk are well documented. The relationship of exercise to hypertension is variable. Aerobic exercise lowers blood pressure in previously sedentary individuals, but increasingly strenuous exercise in already active subjects has less effect. The relationship between stress and hypertension is not established. Polycythemia, whether primary or due to diminished plasma volume, increases blood viscosity and may raise blood pressure. %Nonsteroidal anti-inflammatory drugs (NSAIDs) produce increases in blood pressure averaging 5 mm Hg and are best avoided in patients with borderline or elevated blood pressures. Low potassium intake is associated with higher blood pressure in some patients; an intake of 90 mmol/d is recommended.
There is a growing recognition that the complex of abnormalities termed the metabolic syndrome is associated with both the development of hypertension and an increased risk of adverse cardiovascular outcomes. The metabolic syndrome (sometimes also called syndrome X or the deadly quartet ) consists of upper body obesity, hyperinsulinemia and insulin resistance, hypertriglyceridemia, and hypertension. Affected patients usually also have low high-density lipoprotein (HDL) cholesterol levels and have been found to have elevated catecholamines and inflammatory markers such as C-reactive protein. Patients with hypertension should be encouraged to follow the lifestyle changes listed in Table 11-2.
B. Secondary Hypertension
Approximately 5% of patients with hypertension have specific causes (Table 11-3). The history, examination, and routine laboratory tests may identify such patients. In particular, patients in whom hypertension develops at an early age, those who first exhibit hypertension when over age 50 years, or those previously well controlled who become refractory to treatment are more likely to have secondary hypertension. Causes include renal disease, genetic causes, renal vascular hypertension, primary hyperaldosteronism, Cushing's syndrome, pheochromocytoma, coarctation of the aorta (uncommon), hypertension associated with pregnancy, estrogen use, as well as other causes (eg, hypercalcemia and medications).
Table 11-3. Identifiable causes of hypertension. | ||
|---|---|---|
|
1. Renal disease
Renal parenchymal disease is the most common cause of secondary hypertension. Hypertension may result from diabetic and inflammatory glomerular diseases, tubular interstitial disease, and polycystic kidneys. Most cases are related to increased intravascular volume or increased activity of the renin-angiotensin-aldosterone system.
2. Genetic causes
Hypertension can be caused by mutations in single genes, inherited on a mendelian basis. Although rare, these conditions provide important insight into blood pressure regulation and possibly, the genetic basis of essential hypertension. Glucocorticoid remediable aldosteronism is an autosomal dominant cause of early-onset hypertension with normal or high aldosterone and low renin levels. It is caused by the formation of a chimeric gene encoding both the enzyme responsible for the synthesis of aldosterone (transcriptionally regulated by AII) and an enzyme responsible for synthesis of cortisol (transcriptionally regulated by ACTH). As a consequence, aldosterone synthesis becomes driven by ACTH, which can be suppressed by exogenous cortisol. In the syndrome of apparent mineralocorticoid excess, early-onset hypertension with hypokalemic metabolic alkalosis is inherited on an autosomal recessive basis. Although plasma renin is low and plasma aldosterone level is very low in these patients, aldosterone antagonists are effective in controlling hypertension. This disease is caused by loss of the enzyme 11 -hydroxysteroid dehydrogenase, which normally protects the otherwise promiscuous mineralocorticoid receptor in the distal nephron from inappropriate glucocorticoid activation, by metabolism of cortisol. Similarly, glycyrrhetinic acid, found in licorice, causes increased blood pressure through inhibition of 11 -hydroxysteroid dehydrogenase. The syndrome of hypertension exacerbated in pregnancy is inherited as an autosomal dominant trait. In these patients, a mutation in the mineralocorticoid receptor makes it abnormally responsive to progesterone and, paradoxically, to spironolactone. Liddle's syndrome is an autosomal dominant condition characterized by early-onset hypertension, hypokalemic alkalosis, low renin and low aldosterone levels. This is caused by a mutation that results in constitutive activation of the epithelial sodium channel of the distal nephron, with resultant unregulated sodium reabsorption and volume expansion.
P.434
3. Renal vascular hypertension
Renal artery stenosis is present in 1 2% of hypertensive patients. Its cause in most younger individuals is fibromuscular hyperplasia, particularly in women under 50 years of age. The remainder of renal vascular disease is due to atherosclerotic stenoses of the proximal renal arteries. The mechanism of hypertension is excessive renin release due to reduction in renal blood flow and perfusion pressure. Renal vascular hypertension may occur when a single branch of the renal artery is stenotic, but in as many as 25% of patients both arteries are obstructed.
Renal vascular hypertension should be suspected in the following circumstances: (1) if the documented onset is before age 20 or after age 50 years, (2) hypertension is resistant to three or more drugs, (3) if there are epigastric or renal artery bruits, (4) if there is atherosclerotic disease of the aorta or peripheral arteries (15 25% of patients with symptomatic lower limb atherosclerotic vascular disease have renal artery stenosis), (5) if there is abrupt deterioration in renal function after administration of ACE inhibitors, or (6) if episodes of pulmonary edema are associated with abrupt surges in blood pressure. There is no ideal screening test for renal vascular hypertension. If suspicion is sufficiently high, renal arteriography, the definitive diagnostic test, is the best approach. Renal arteriography is not recommended as a routine adjunct to coronary studies. Where suspicion is moderate to low, radioisotope renography, duplex ultrasound, magnetic resonance angiography (MRA) or CT angiography have all been used successfully, but the results vary greatly among institutions. The extent of preexisting parenchymal damage to the affected and contralateral kidney has the greatest influence on blood pressure and renal function outcomes following revascularization. Correction of the lesion should be considered in young individuals and in low-risk patients of any age with blood pressure that is resistant to medical therapy. Percutaneous intervention with stent placement is the preferred approach for fibromuscular hyperplasia and for discrete stenotic arteriosclerotic lesions that do not involve the renal artery ostium. In older individuals with arteriosclerosis, only a minority experience complete normalization without continued drug therapy. Thus, it is reasonable to manage these patients medically if renal function does not deteriorate. Although ACE inhibitors have improved the success rate of medical therapy of hypertension due to renal artery stenosis, they have been associated with marked hypotension and (usually reversible) renal dysfunction in individuals with bilateral renal artery stenosis. Thus, renal function and blood pressure should be closely monitored during the first weeks of therapy in patients in whom this is a consideration.
4. Primary hyperaldosteronism
Primary hyperaldosteronism occurs because of excessive secretion of aldosterone by the adrenal cortex. It may, in fact, be the most common potentially curable and specifically treatable cause of hypertension. In the past, the diagnosis was often suspected when hypokalemia prior to diuretic therapy associated with excessive urinary potassium excretion (usually > 40 mEq/L on a spot specimen) and suppressed levels of plasma renin activity presented in hypertensive patients. However, the development and application of new screening tests to the population of hypertensive persons have resulted in a marked increase in the detection rate for primary hyperaldosteronism. It now appears that up to 5 15% of patients in whom primary (essential) hypertension is diagnosed actually have primary hyperaldosteronism, with most having normal serum potassium levels. Currently, the best screening test for primary hyperaldosteronism involves determinations of plasma aldosterone concentration (normal: 1 16 ng/dL) and plasma renin activity (normal: 1 2.5 ng/mL/h) and calculation of the plasma aldosterone/renin ratio (normal: < 25). Medications that alter renin and aldosterone levels, including ACE inhibitors, angiotensin receptor blockers (ARBs), and diuretics (especially spironolactone), should be discontinued at least a week before sampling. Patients with aldosterone/renin ratios of 25 require further evaluation for primary hyperaldosteronism. The lesion responsible is an adrenal adenoma, though some patients have bilateral adrenal hyperplasia. The lesion can be demonstrated by CT or MRI scanning.
5. Cushing's syndrome
Less commonly, hypertension presents in patients with Cushing's syndrome (glucocorticoid excess). However, among those with spontaneous Cushing's syndrome, hypertension occurs in about 75 85% of patients. The exact pathogenesis of the hypertension is unclear. It may be related to salt and water retention from the mineralocorticoid effects of the excess glucocorticoid. Alternatively, it may be due to increased secretion of angiotensinogen. While plasma renin activity and concentrations are generally normal or suppressed in Cushing's syndrome, angiotensinogen levels are elevated to approximately twice normal because of a direct effect of glucocorticoids on its hepatic synthesis, and angiotensin II levels are increased by about 40%. Administration of the angiotensin II antagonist saralasin to patients with Cushing's syndrome causes a prompt 8- to 10-mm Hg drop in systolic and diastolic blood pressure. In addition, glucocorticoids exert permissive effects on vascular tone by a variety of mechanisms.
Diagnosis and treatment of Cushing's syndrome are discussed in Chapter 26.
6. Pheochromocytoma
Pheochromocytomas are uncommon; they are probably found in less than 0.1% of all patients with hypertension and in approximately two individuals per million population. In about 50% of patients with pheochromocytoma, hypertension is sustained but the blood pressure shows marked fluctuations, with peak pressures during symptomatic paroxysms. During a hypertensive episode, the systolic blood pressure can rise to as high as 300 mm Hg. In about one-third of cases, hypertension is truly intermittent. In some cases, hypertension is absent. The blood pressure elevation caused by the catecholamine excess results from two mechanisms: -receptor-mediated vasoconstriction of arterioles, leading to an increase in peripheral
P.435
resistance, and 1-receptor-mediated increases in cardiac output and in renin release, leading to increased circulating levels of angiotensin II. The increased total peripheral vascular resistance is probably primarily responsible for the maintenance of high arterial pressures. Chronic vasoconstriction of the arterial and venous beds leads to a reduction in plasma volume and predisposes to postural hypotension.
Indeed, the majority of patients have orthostatic decreases in blood pressure, the converse of primary (essential) hypertension. Glucose intolerance develops in some patients. Hypertensive crisis in pheochromocytoma may be precipitated by a variety of drugs, including tricyclic antidepressants, antidopaminergic agents, metoclopramide, and naloxone. The diagnosis and treatment of pheochromocytoma are discussed in Chapter 26.
7. Coarctation of the aorta
This uncommon cause of hypertension is discussed in Chapter 10.
8. Hypertension associated with pregnancy
Hypertension occurring de novo or worsening during pregnancy, including preeclampsia and eclampsia, is one of the most common causes of maternal and fetal morbidity and mortality (see Chapter 18).
9. Estrogen use
A small increase in blood pressure occurs in most women taking oral contraceptives, but considerable increases are noted occasionally. This is caused by volume expansion due to increased activity of the renin-angiotensin-aldosterone system. The primary abnormality is an increase in the hepatic synthesis of renin substrate. Five percent of women taking oral contraceptives chronically exhibit a rise in blood pressure above 140/90 mm Hg, twice the expected prevalence. Contraceptive-related hypertension is more common in women over 35 years of age, in those who have taken contraceptives for more than 5 years, and in obese individuals. It is less common in those taking low-dose estrogen tablets. In most, hypertension is reversible by discontinuing the contraceptive, but it may take several weeks. Postmenopausal estrogen does not generally cause hypertension, but rather maintains endothelium-mediated vasodilation.
10. Other causes of secondary hypertension
Hypertension has also been associated with hypercalcemia due to any cause: acromegaly, hyperthyroidism, hypothyroidism, and a variety of neurologic disorders causing increased intracranial pressure. A number of other medications may cause or exacerbate hypertension most importantly cyclosporine and NSAIDs.
August P: Overview: mechanisms of hypertension: cells, hormones, and the kidney. J Am Soc Nephrol 2004;15:1971.
Bravo EL: Pheochromocytoma. Cardiol Rev 2002;10:44.
Failor RA et al: Hyperaldosteronism and pheochromocytoma: new tricks and tests. Prim Care 2003;30:801.
Freel EM et al: Mechanisms of hypertension: the expanding role of aldosterone. J Am Soc Nephrol 2004;15:1993.
Hartman RP et al: Evaluation of renal causes of hypertension. Radiol Clin North Am 2003;41:909.
Lifton RP et al: Molecular mechanisms of human hypertension. Cell 2001;104:545.
Loney EL et al: Renovascular hypertension. Q J Nucl Med 2002; 46:283.
Nordmann AJ et al: Balloon angioplasty versus medical therapy for hypertensive patients with renal artery obstruction. Cochrane Database Syst Rev 2003;(3):CD002944.
Nussberger J: Investigating mineralocorticoid hypertension. J Hypertens Suppl 2003;21(Suppl 2):S25.
Onusko E: Diagnosing secondary hypertension. Am Fam Physician 2003;67:67.
Oparil S et al: Pathogenesis of hypertension. Ann Intern Med 2003;139:761.
Radermacher J et al: Techniques for predicting a favourable response to renal angioplasty in patients with renovascular disease. Curr Opin Nephrol Hypertens 2001;10:799.
Reaven G: Insulin resistance, hypertension, and coronary heart disease. J Clin Hypertens 2003;5:269.
Safar ME et al: Vascular development, pulse pressure, and the mechanisms of hypertension. Hypertension 2005;46:205.
Stas SN et al: Pathogenesis of hypertension in diabetes. Rev Endocr Metab Disord 2004;5:221.
Strazzullo P et al: Altered renal handling of sodium in human hypertension: short review of the evidence. Hypertension 2003;41:1000.
Textor SC: Managing renal arterial disease and hypertension. Curr Opin Cardiol 2003;18:260.
Young WF Jr: Minireview: primary aldosteronism changing concepts in diagnosis and treatment. Endocrinology 2003;144: 2208.
Complications of Untreated Hypertension
Complications of hypertension are related either to sustained elevations of blood pressure, with consequent changes in the vasculature and heart, or to atherosclerosis that accompanies and is accelerated by long-standing hypertension. Most of the adverse outcomes in hypertension are associated with thrombosis rather than bleeding, and there is evidence that increased vascular shear stress converts the normally anticoagulant endothelium to a prothrombotic state. The excess morbidity and mortality related to hypertension are progressive over the whole range of systolic and diastolic blood pressures; the risk approximately doubles for each 6 mm Hg increase in diastolic blood pressure. However, target-organ damage varies markedly between individuals with similar levels of office hypertension. Ambulatory pressures are superior to office readings in the prediction of end-organ damage.
A. Hypertensive Cardiovascular Disease
Cardiac complications are the major causes of morbidity and mortality in primary (essential) hypertension, and preventing them is a major goal of therapy. Electrocardiographic evidence of left ventricular hypertrophy is found in up to 15% of persons with chronic hypertension.
P.436
For any level of blood pressure, its presence is associated with incremental cardiovascular risk. Echocardiographic left ventricular hypertrophy is a powerful predictor of prognosis. Left ventricular hypertrophy may cause or facilitate many cardiac complications of hypertension, including congestive heart failure, ventricular arrhythmias, myocardial ischemia, and sudden death.
Left ventricular diastolic dysfunction, which may present with all of the symptoms and signs of congestive heart failure, is common in patients with long-standing hypertension. The occurrence of heart failure is reduced by 50% with antihypertensive therapy. Hypertensive left ventricular hypertrophy regresses with therapy and is most closely related to the degree of systolic blood pressure reduction. Diuretics have produced equal or greater reductions of left ventricular mass when compared with other drug classes. -Blockers are less effective in reducing left ventricular hypertrophy but play a specific role in patients with established coronary artery disease or impaired left ventricular function.
B. Hypertensive Cerebrovascular Disease and Dementia
Hypertension is the major predisposing cause of hemorrhagic and ischemic stroke. Cerebrovascular complications are more closely correlated with systolic than diastolic blood pressure. The incidence of these complications is markedly reduced by antihypertensive therapy. Preceding hypertension is associated with a higher incidence of subsequent dementia of both vascular and Alzheimer types. Effective blood pressure control may modify the risk or rate of progression of cognitive dysfunction.
C. Hypertensive Renal Disease
Chronic hypertension leads to nephrosclerosis, a common cause of renal insufficiency; aggressive blood pressure control attenuates the process. In patients with hypertensive nephropathy, the blood pressure should be 130/80 mm Hg or lower, especially when proteinuria is present. Secondary renal disease is more common in blacks, particularly when accompanied by diabetes mellitus. Hypertension also plays an important role in accelerating the progression of other forms of renal disease, most commonly diabetic nephropathy. ACE inhibitors are particularly effective in preventing the latter complication, but these agents also appear to prevent the progression of other forms of nephropathy.
D. Aortic Dissection
Hypertension is a contributing factor in many patients with dissection of the aorta. Its diagnosis and treatment are discussed in Chapter 12.
E. Atherosclerotic Complications
Most Americans with hypertension die of complications of atherosclerosis, but the linkage between hypertension and atherosclerotic cardiovascular disease is not as clear as that with the previously discussed complications. Effective antihypertensive therapy is thus less successful in preventing complications of coronary heart disease.
Dielis AW et al: The prothrombotic paradox of hypertension: role of the renin-angiotensin and kallikrein-kinin systems. Hypertension 2005;46:1236.
Forette F et al: The prevention of dementia with antihypertensive treatment. Arch Intern Med 2002;162:2046.
Izzo JL et al: Mechanisms and management of hypertensive heart disease: from left ventricular hypertrophy to heart failure. Med Clin North Am 2004;88:1257.
Lapu-Bula R et al: Diastolic heart failure: the forgotten manifestation of hypertensive heart disease. Curr Hypertens Rep 2004; 6:164.
Luft FC: Hypertensive nephrosclerosis: update. Curr Opin Nephrol Hypertens 2004;13:147.
Manolio TA et al: Hypertension and cognitive function: pathophysiologic effects of hypertension on the brain. Curr Hypertens Rep 2003;5:255.
Persu A et al: Recent insights in the development of organ damage caused by hypertension. Acta Cardiol 2004;59:369.
Clinical Findings
The clinical and laboratory findings are mainly referable to involvement of the target organs: heart, brain, kidneys, eyes, and peripheral arteries.
A. Symptoms
Mild to moderate primary (essential) hypertension is largely asymptomatic for many years. The most frequent symptom, headache, is also very nonspecific. Suboccipital pulsating headaches, occurring early in the morning and subsiding during the day, are said to be characteristic, but any type of headache may occur. Accelerated hypertension is associated with somnolence, confusion, visual disturbances, and nausea and vomiting (hypertensive encephalopathy).
Hypertension in patients with pheochromocytomas that secrete predominantly norepinephrine is usually sustained but may be episodic. The typical attack lasts from minutes to hours and is associated with headache, anxiety, palpitation, profuse perspiration, pallor, tremor, and nausea and vomiting. Blood pressure is markedly elevated, and angina or acute pulmonary edema may occur. In primary aldosteronism, patients may have muscular weakness, polyuria, and nocturia due to hypokalemia; malignant hypertension is rare. Chronic hypertension often leads to left ventricular hypertrophy, which may be associated with diastolic or, in late stages, systolic dysfunction. Exertional and paroxysmal nocturnal dyspnea may result, and ischemic heart disease is more common (especially when concomitant coronary artery disease is present).
Cerebral involvement causes (1) stroke due to thrombosis or (2) small or large hemorrhage from microaneurysms of small penetrating intracranial arteries. Hypertensive encephalopathy is probably caused by acute capillary congestion and exudation with cerebral edema. The findings
P.437
are usually reversible if adequate treatment is given promptly. There is no strict correlation of diastolic blood pressure with hypertensive encephalopathy; but it usually exceeds 130 mm Hg.
B. Signs
Like symptoms, physical findings depend on the cause of hypertension, its duration and severity, and the degree of effect on target organs.
1. Blood pressure
On initial examination, pressure is taken in both arms and, if lower extremity pulses are diminished or delayed, in the legs to exclude coarctation of the aorta. An orthostatic drop is present in pheochromocytoma. Older patients may have falsely elevated readings by sphygmomanometry because of noncompressible vessels. This may be suspected in the presence of Osler's sign a palpable brachial or radial artery when the cuff is inflated above systolic pressure. Occasionally, it may be necessary to make direct measurements of intra-arterial pressure, especially in patients with apparent severe hypertension who do not tolerate therapy.
2. Retinas
Narrowing of arterial diameter to less than 50% of venous diameter, copper or silver wire appearance, exudates, hemorrhages, or papilledema are associated with a worse prognosis.
3. Heart and arteries
Left ventricular enlargement with a left ventricular heave indicates severe or long-standing hypertrophy. Older patients frequently have systolic ejection murmurs resulting from calcific aortic sclerosis, and these may evolve to significant aortic stenosis in some individuals. Aortic insufficiency may be auscultated in up to 5% of patients, and hemodynamically insignificant aortic insufficiency can be detected by Doppler echocardiography in 10 20%. A presystolic (S4) gallop due to decreased compliance of the left ventricle is quite common in patients with sinus rhythm.
4. Pulses
The timing of upper and lower extremity pulses should be compared to exclude coarctation of the aorta. All major peripheral pulses should be evaluated to exclude aortic dissection and peripheral atherosclerosis, which may be associated with renal artery involvement.
C. Laboratory Findings
Recommended testing includes the following: hemoglobin; urinalysis and renal function studies, to detect hematuria, proteinuria, and casts, signifying primary renal disease or nephrosclerosis; fasting blood sugar level, since hyperglycemia is noted in diabetes and pheochromocytoma; plasma lipids, as an indicator of atherosclerosis risk and an additional target for therapy; serum uric acid which, if elevated, is a relative contraindication to diuretic therapy; and basal electrolytes. Measurement of the plasma aldosterone/renin ratio is indicated to screen for mineralocorticoid excess in hypertensive patients with hypokalemic alkalosis (even if they are taking diuretics), resistant hypertension, or an adrenal incidentaloma.
D. Electrocardiography and Chest Radiographs
Electrocardiographic criteria are highly specific but not very sensitive for left ventricular hypertrophy. The strain pattern of ST-T wave changes is a sign of more advanced disease and is associated with a poor prognosis. A chest radiograph is not necessary in the workup for uncomplicated hypertension since it usually does not yield additional information.
E. Echocardiography
Although echocardiography has been advocated to determine the need for drug therapy in patients with borderline or mildly elevated pressures, it is unusual to find left ventricular mass readings above the upper 75% confidence limits in the absence of systolic hypertension. The primary role of echocardiography should be to evaluate patients with clinical symptoms or signs of cardiac disease.
F. Diagnostic Studies
Additional diagnostic studies are indicated only if the clinical presentation or routine tests suggest secondary or complicated hypertension. These may include tests such as 24-hour urine free cortisol, plasma metanephrine and the plasma aldosterone/renin ratio for endocrine causes of hypertension, renal ultrasound to diagnose primary renal disease (polycystic kidneys, obstructive uropathy), and testing for renal artery stenosis. Further evaluation may include abdominal imaging studies (ultrasound, CT scan, or MRI) or renal arteriography.
G. Summary
Since most hypertension is primary, few studies are necessary beyond those listed above. If conventional therapy is unsuccessful or if symptoms suggest a secondary cause, further studies are indicated.
Nonpharmacologic Therapy
Lifestyle modification may have an impact on morbidity and mortality. A diet rich in fruits, vegetables, and low-fat dairy foods and low in saturated and total fats (DASH diet) has been shown to lower blood pressure. Additional measures can prevent or mitigate hypertension or its cardiovascular consequences as shown in Table 11-2.
All patients with high-normal or elevated blood pressures, those who have a family history of cardiovascular complications of hypertension, and those who have multiple coronary risk factors should be counseled about nonpharmacologic approaches to lowering blood pressure. Approaches of proved but modest value include weight reduction, reduced alcohol consumption and, in some patients, reduced salt intake. Gradually increasing activity levels should be encouraged
P.438
in previously sedentary patients, but strenuous exercise training programs in already active individuals may have less benefit. Calcium and potassium supplements have been advocated, but their ability to lower blood pressure is limited.
Smoking cessation will reduce overall cardiovascular risk.
Bray GA et al: A further subgroup analysis of the effects of the DASH diet and three dietary sodium levels on blood pressure: results of the DASH-Sodium Trial. Am J Cardiol 2004;94:222.
Hooper L et al: Advice to reduce dietary salt for prevention of cardiovascular disease. Cochrane Database Syst Rev 2004;(1): CD003656.
Krousel-Wood MA et al: Primary prevention of essential hypertension. Med Clin North Am 2004;88:223.
Stewart KJ: Exercise training and the cardiovascular consequences of type 2 diabetes and hypertension: plausible mechanisms for improving cardiovascular health. JAMA 2002;288:1622.
Whelton SP et al: Effect of aerobic exercise on blood pressure: a meta-analysis of randomized controlled trials. Ann Intern Med 2002;136:493.
Wilburn AJ et al: The natural treatment of hypertension. J Clin Hypertens (Greenwich) 2004;6:242.
Who should be Treated with Medications?
Many excellent trials have shown that drug therapy of patients with stage 2 hypertension reduces the incidence of stroke by 30 50%, congestive heart failure by 40 50%, and progression to accelerated hypertension syndromes. The decreases in fatal and nonfatal coronary heart disease and cardiovascular and total mortality have been less dramatic, ranging from 10% to 15%. This lesser decrease in coronary heart disease has generated controversy. Some experts have attributed the decreased benefit to characteristics of the drugs (primarily diuretics and -blockers), such as their adverse effect on lipid profiles and electrolyte balance. Others believe it is due to the more chronic and multifactorial nature of coronary artery disease, the generally low-risk populations included in trials, and the large number of crossovers from placebo to active therapy. Several studies in older persons with predominantly systolic hypertension have confirmed that antihypertensive therapy prevents fatal and nonfatal myocardial infarction and overall cardiovascular mortality. These trials have also placed the focus on control of systolic blood pressure in contrast to the historical emphasis on diastolic blood pressures.
The decision to initiate drug therapy is relatively straightforward once hypertension has been unequivocally diagnosed (Table 11-1 and Figure 11-1), but less clear in persons with prehypertension (blood pressure of 120 139/80 89 mm Hg). In the latter group, treatment decisions should be based on an assessment of overall cardiovascular risk rather than the level of blood pressure alone. The JNC criteria for institution of therapy (Table 11-1) suggest that patients with prehypertension should be treated if they exhibit at least one additional high-risk condition with compelling indications (listed in Table 11-4), such as chronic kidney disease or diabetes mellitus. In the presence of compelling indications, the target blood pressure should be < 130/80 mm Hg in persons with prehypertension just as in those with hypertension. Table 11-5 lists the major risk factors for cardiovascular morbidity and mortality and the cardiovascular manifestations that predispose to further complications. The BHS promotes a similar approach but goes further by introducing a consideration of overall predicted cardiovascular risk (Figure 11-2). According to the BHS recommendations, risk analysis should be used to target treatment to patients with borderline hypertension who are most likely to benefit, particularly individuals at high combined risk of coronary heart or stroke event (> 20 30% within 10 years). A risk calculation tool can be downloaded from the BHS web site at http://www.bhsoc.org/Cardiovascular_Risk_Charts_and_Calculators.htm (in using this tool, convert cholesterol from mmol/L to mg/dL by multiplying by 38.7). A free PDA-based coronary heart disease risk calculator is available at http://www.statcoder.com/cholesterol.htm. In general, 20% total cardiovascular risk (which includes stroke) is equivalent to 15% coronary heart disease risk.
Goals of Treatment
Treatment should ideally be offered to all persons in whom blood pressure reduction, irrespective of initial blood pressure levels, will reduce overall cardiovascular risk (see above). Blood pressure targets for hypertensive patients at the greatest risk for cardiovascular events, particularly diabetic patients, should be lower (< 130/80 mm Hg) than for individuals at lower total cardiovascular risk (< 140/90 mm Hg). As discussed below, hypertensive patients with chronic kidney disease should also be treated until blood pressure is < 130/80 mm Hg. However, since there does not seem to be a blood pressure level below which risk plateaus, these recommendations should be taken as reasonable goals pending further information on optimal targets, which may be even lower. There is no clear consensus on blood pressure goals in the treatment of prehypertension.
Large-scale trials in hypertension have focused on discrete end points occurring over relatively short intervals, thereby placing the emphasis on the prevention of catastrophic events in advanced disease. More recently, in parallel with a new emphasis on hypertension in the context of overall cardiovascular risk, attention is turning to the importance of the long view. Accordingly, treatment of persons with hypertension should focus on comprehensive risk reduction. More careful consideration should be given to the possible long-term adverse consequences of the metabolic derangements linked to some antihypertensives (particularly conventional -blockers and thiazide diuretics).
Table 11-4. Clinical trial and guideline basis for compelling indications for individual drug classes. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Statins should be more widely used. In this respect, there is now evidence from the Anglo-Scandinavian
P.439
Cardiac Outcomes Trial (ASCOT) that statins can significantly improve outcomes in persons with hypertension (with modest background cardiovascular risk) whose total cholesterol is < 250 mg/dL. The BHS guidelines recommend that statins be offered as secondary prevention to patients whose total cholesterol exceeds 135 mg/dL if they have documented coronary artery disease or a history of ischemic stroke. In addition, statins should be considered as primary prevention in patients with long-standing type 2 diabetes mellitus or in those with type 2 diabetes mellitus who are older than age 50 years, and perhaps in all persons with type 2 diabetes mellitus. Ideally, total and low-density lipoprotein (LDL) cholesterol should be reduced by 30% and 40% respectively, or to approximately < 155 mg/dL and < 77 mg/dL, whichever is the greatest reduction. However, total and LDL cholesterol levels of < 194 mg/dL and < 116 mg/dL respectively, or reductions of 25% and 30% are regarded as clinically acceptable objectives. Primary prevention with statins might also be reasonably extended to all patients with total cholesterol > 135 mg/dL and a total cardiovascular risk > 20% (to similar target cholesterol levels), but trial evidence for this is not currently available.
Low-dose aspirin (81 mg/day) is likely to be beneficial in patients older than age 50 with either target organ damage or elevated total cardiovascular risk (> 20 30%). Care should be taken to ensure that blood pressure is controlled to the recommended levels in patients receiving aspirin to minimize the risk of bleeding.
Table 11-5. Cardiovascular risk factors. | ||
|---|---|---|
|
P.440
Friday G et al: Control of hypertension and risk of stroke recurrence. Stroke 2002;33:2652.
Lawes CM et al: Blood pressure and stroke: an overview of published reviews. Stroke 2004;35:776.
Sever PS et al; ASCOT investigators: Prevention of coronary and stroke events with atorvastatin in hypertensive patients who have average or lower-than-average cholesterol concentrations, in the Anglo-Scandinavian Cardiac Outcomes Trial Lipid Lowering Arm (ASCOT-LLA): a multicentre randomised controlled trial. Lancet 2003;361:1149.
Snow V et al: The evidence base for tight blood pressure control in the management of type 2 diabetes mellitus. Ann Intern Med 2003;138:587.
Whelton PK et al: Strategies for improvement of awareness, treatment and control of hypertension: results of a panel discussion. J Hum Hypertens 2004;18:563.
Whitworth JA: 2003 World Health Organization (WHO)/International Society of Hypertension (ISH) statement on management of hypertension. J Hypertens 2003;21:1983.
Drug Therapy
General Principles
There are now many classes of potentially antihypertensive drugs of which five (diuretics, -blockers, ACE inhibitors, calcium channel blockers, and ARBs) are suitable for initial or single-drug therapy based on efficacy and tolerability. A number of considerations enter into the selection of the initial drug for a given patient. These include the weight of evidence for beneficial effects on clinical outcomes, the safety and tolerability of the drug, its cost, demographic differences in response, concomitant medical conditions, and lifestyle issues. The specific classes of antihypertensive medications are discussed below, and guidelines for the choice of initial medications are offered.
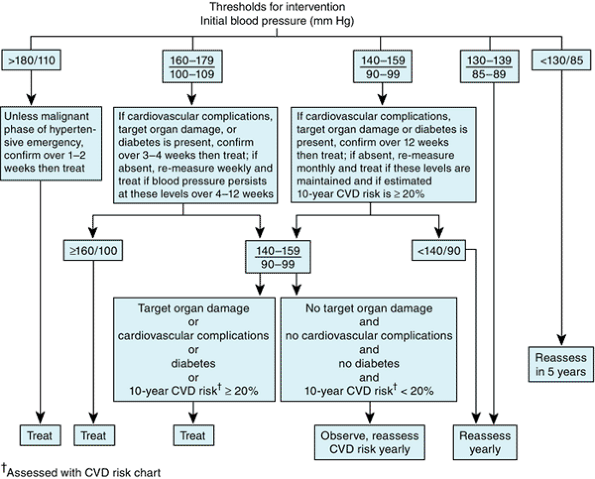 |
Figure 11-2. British Hypertension Society algorithm for diagnosis and treatment of hypertension, incorporating total cardiovascular risk in deciding which prehypertensive patients to treat. (CVD = cardiovascular disease.) (Reproduced with permission from: Guidelines for management of hypertension: report of the Fourth Working Party of the British Hypertension Society, 2004-BHS IV. J Hum Hypertens 2004;18:139 185. ) |
Current Antihypertensive Agents
A. Diuretics
Diuretics are the antihypertensives that have been most extensively studied and most consistently effective in clinical trials. They lower blood pressure initially by decreasing plasma volume (by suppressing tubular reabsorption of sodium, thus increasing the excretion of sodium and water) and cardiac output, but during long-term therapy their major hemodynamic effect is reduction of peripheral vascular resistance. Most of the antihypertensive effect of these agents is achieved at lower dosages than used previously (typically, 12.5 or 25 mg of hydrochlorothiazide or equivalent), but their biochemical and metabolic effects are dose related. The thiazide diuretics are the most widely used (Table 11-6). During long-term therapy, hydrochlorothiazide may be administered every other day with undiminished efficacy. The loop diuretics (such as furosemide) may lead to electrolyte and volume depletion more readily than the thiazides and have short durations of action; therefore, loop diuretics should not be used in hypertension except in the presence of renal dysfunction (serum creatinine above 2.5 mg/dL). Relative to the -blockers and the ACE inhibitors, diuretics are more potent in blacks, older individuals, the obese, and other subgroups with increased plasma volume or low plasma renin activity. Interestingly, they are relatively more effective in smokers than in nonsmokers. Long-term diuretic administration also mitigates the loss of bone mineral content in older women at risk for osteoporosis.
Overall, diuretics administered alone control blood pressure in 50% of patients with mild to moderate hypertension and can be used effectively in combination with all other agents. They are also useful for lowering isolated or predominantly systolic hypertension. Some observations suggest that the use of thiazide diuretics as initial therapy has been associated with greater reductions in myocardial infarction than -blockers.
The adverse effects of diuretics relate primarily to the metabolic changes listed in Table 11-6. Impotence, skin rashes, and photosensitivity are less frequent. Hypokalemia has been a concern but is uncommon at the recommended dosages (12.5 25 mg hydrochlorothiazide). The risk can be minimized by limiting dietary salt or increasing dietary potassium; potassium replacement is not usually required to maintain serum K+ at > 3.5 mmol/L. Higher serum levels are prudent in patients at special risk from intracellular potassium depletion, such as those taking digoxin or with a history of ventricular arrhythmias.
P.441
If higher doses of diuretic are required, the drug should be used in combination with a potassium-sparing agent or with an ACE inhibitor or ARB. Diuretics reduce insulin sensitivity and cause modest increases in blood glucose. Compared with ACE inhibitors and ARBs, diuretic therapy is associated with a slightly higher incidence of new-onset diabetes. Diuretics also increase serum uric acid and may precipitate gout. Increases in blood glucose, triglycerides, LDL cholesterol, and plasma insulin may occur but are relatively minor during long-term low-dose therapy.
B. -Adrenergic Blocking Agents
These drugs are effective in hypertension because they decrease the heart rate and cardiac output. Even after continued use of -blockers, cardiac output remains lower and systemic vascular resistance higher with agents that do not have intrinsic sympathomimetic or -blocking activity. The -blockers also decrease renin release and are more efficacious in populations with elevated plasma renin activity, such as younger white patients. They neutralize the reflex tachycardia caused by vasodilators and are especially useful in patients with associated conditions that benefit from the cardioprotective effects of these agents. These include individuals with angina pectoris, previous myocardial infarction, and stable congestive heart failure as well as those with migraine headaches and somatic manifestations of anxiety. In some clinical trials, -blockers have not been as effective as diuretics in preventing first myocardial infarctions.
Although all -blockers appear to be similar in antihypertensive potency, controlling approximately 50% of patients, they differ in a number of pharmacologic properties (these differences are summarized in Table 11-7), including those relatively specific to the cardiac 1-receptors (cardioselectivity) and whether they also block the 2-receptors in the bronchi and vasculature; at higher dosages, however, all agents are nonselective. The -blockers also differ in their pharmacokinetics and lipid solubility which determines whether they cross the blood-brain barrier and affect the incidence of central
P.442
P.443
P.444
P.445
P.446
nervous system side effects and route of metabolism. Labetalol and carvedilol are combined - and -blockers and, unlike most -blockers, decrease peripheral vascular resistance.
Table 11-6. Antihypertensive drugs: diuretics. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Table 11-7. Antihypertensive drugs: -adrenergic blocking agents. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
The side effects of all -blockers include inducing or exacerbating bronchospasm in predisposed patients (eg, those with asthma and some patients with chronic obstructive pulmonary disease [COPD]); sinus node dysfunction and atrioventricular (AV) conduction depression (resulting in bradycardia or AV block); precipitating or worsening clinically important left ventricular failure; nasal congestion; Raynaud's phenomenon; and central nervous system symptoms with nightmares, excitement, depression, and confusion. Fatigue, lethargy, and impotence may occur. All -blockers tend to increase plasma triglycerides. The nonselective and, to a lesser extent, the cardioselective ( 1-selective) -blockers tend to depress the protective HDL fraction of plasma cholesterol. As with diuretics, the changes are blunted with time and dietary changes.
-Blockers have traditionally been considered contraindicated in patients with congestive heart failure. Evolving experience suggests that they have a propitious effect on the natural history of patients with chronic stable heart failure and reduced ejection fraction (see Chapter 10). -Blockers are used cautiously in patients with type 1 diabetes, since they can mask the symptoms of hypoglycemia and prolong these episodes by inhibiting gluconeogenesis. Although they may increase blood glucose levels in type 2 diabetics, the prognosis of these patients on balance is improved. These drugs should also be used with caution in patients with advanced peripheral vascular disease associated with rest pain or nonhealing ulcers, but they are generally well tolerated in patients with mild claudication. In treatment of pheochromocytoma, -blockers should not be administered until -blockade has been established. Otherwise, blockade of vasodilatory 2-adrenergic receptors will allow unopposed vasoconstrictor -adrenergic receptor activation with worsening of hypertension.
Because of the lack of efficacy in prevention of myocardial infarction and inferiority compared with other drugs in prevention of stroke and left ventricular hypertrophy, there is now increasing doubt whether -blockers should still be regarded as ideal first-line agents in the treatment of hypertension without specific compelling indications (such as active coronary artery disease). In addition to the adverse metabolic changes associated with their use, some experts have suggested that the therapeutic shortcomings of -blockers are the consequence of the particular hemodynamic profile associated with these drugs. Pressure peaks in the aorta are augmented by reflection of pressure waves from the peripheral circulation. These reflected waves are delayed in patients taking ACE inhibitors and thiazide diuretics, resulting in decreased systolic and pulse pressures. By contrast, -blockers have no effect on reflection of pressure waves, possibly because peripheral resistance vessels are a reflection point and peripheral resistance is not decreased by -blockers. This might explain why -blockers are less effective at control of systolic and pulse pressure.
The ASCOT trial showed that the atenolol/bendroflumethiazide combination was inferior to the amlodipine/perindopril combination in predominantly white patients with modestly elevated cardiovascular risk. Subsequent analyses indicated that differences in blood pressure and HDL cholesterol accounted for the excess risk of stroke and coronary events respectively in the -blocker group. Despite these concerns, the compelling indications for -blockers remain, such as active coronary artery disease and impaired left ventricular function. Great care should be exercised if the decision is made, in the absence of compelling indications, to remove -blockers from the treatment regimen since abrupt withdrawal can precipitate acute coronary events and severe increases in blood pressure.
C. Angiotensin-Converting Enzyme Inhibitors
ACE inhibitors are being increasingly used as the initial medication in mild to moderate hypertension (Table 11-8). Their primary mode of action is inhibition of the renin-angiotensin-aldosterone system, but they also inhibit bradykinin degradation, stimulate the synthesis of vasodilating prostaglandins and, sometimes, reduce sympathetic nervous system activity. These latter actions may explain why they exhibit some effect even in patients with low plasma renin activity. ACE inhibitors appear to be more effective in younger white patients. They are relatively less effective in blacks and older persons and in predominantly systolic hypertension. Although as single therapy they achieve adequate antihypertensive control in only about 40 50% of patients, the combination of an ACE inhibitor and a diuretic or calcium channel blocker is potent.
ACE inhibitors are the agents of choice in persons with type 1 diabetes with frank proteinuria or evidence of renal dysfunction because they delay the progression to end-stage renal disease. Many authorities have expanded this indication to include persons with type 2 diabetes and those who have type 1 diabetes with microalbuminuria, even when they do not meet the usual criteria for antihypertensive therapy. The Heart Outcomes Prevention Evaluation (HOPE) trial demonstrated that the ACE inhibitor ramipril reduces the number of cardiovascular deaths, nonfatal myocardial infarctions, and nonfatal strokes and also reduces the incidence of new-onset heart failure, renal dysfunction, and new-onset diabetes in a population of patients at high risk for vascular events. Although this was not specifically a hypertensive population, the benefits were associated with a modest reduction in blood pressure, and the results inferentially support the use of ACE inhibitors in similar hypertensive patients. ACE inhibitors may also delay the progression of other forms of renal disease. They are a drug of choice (usually in conjunction with a diuretic and a -blocker) in patients with congestive heart failure and are indicated also in asymptomatic patients with reduced ejection fractions whether due to myocardial infarction or to other causes.
Table 11-8. Antihypertensive drugs: ACE inhibitors and angiotensin II receptor blockers. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
P.447
P.448
ACE inhibitors have effects on mortality and most cardiovascular outcomes similar to those achieved with diuretics and -blockers. However, compared with calcium channel blockers, ACE inhibitors are associated with lower incidences of coronary events and heart failure.
An advantage of the ACE inhibitors is their relative freedom from troublesome side effects. Severe hypotension can occur in patients with bilateral renal artery stenosis; acute renal failure may ensue but is usually reversible with discontinuation of ACE inhibition. Hyperkalemia may develop in patients with intrinsic renal disease and type IV renal tubular acidosis (commonly seen in diabetics) and in the elderly. A chronic dry cough is common, seen in 10% of patients or more, and may require stopping the drug. Dizziness occurs but may not be related to the degree of blood pressure lowering. Skin rashes are observed with any ACE inhibitor. Taste alterations are seen more often with captopril than with the non-sulfhydryl-containing agents (enalapril and lisinopril) but often disappear with continued therapy. Angioedema is an uncommon but potentially dangerous side effect of all agents of this class because of their inhibition of kininase.
D. Angiotensin II Receptor Blockers
Although losartan, the first member of this group, was less potent than high doses of ACE inhibitors in reducing blood pressure, the newer ARBs (valsartan, irbesartan, candesartan, telmisartan, and eprosartan) appear to be equipotent to ACE inhibitors (Table 11-8). A growing body of data indicates that ARBs can improve cardiovascular outcomes in patients with hypertension as well as in patients with related conditions such as heart failure and type 2 diabetes with nephropathy. ARBs have not been compared with ACE inhibitors in randomized controlled trials in patients with hypertension, but two trials comparing losartan with captopril in heart failure and post-myocardial infarction left ventricular dysfunction showed trends toward worse outcomes in the losartan group. Whether this suggestion of reduced efficacy is specific to losartan or may also be true for other ARBs is as yet unknown. However, the Losartan Intervention for Endpoints (LIFE) trial in nearly 9000 hypertensive patients with electrocardiographic evidence of left ventricular hypertrophy comparing
P.449
losartan with the -blocker atenolol as initial therapy demonstrated a significant reduction in stroke with losartan. Of note is that in diabetic patients, death and myocardial infarction were also reduced, and there was a lower occurrence of new-onset diabetes. In this trial, as in the Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT) with an ACE inhibitor, blacks exhibited less blood pressure reduction and less benefit with regard to clinical end points.
Unlike ACE inhibitors, the ARBs do not cause cough and are only infrequently associated with skin rashes, the most common side effects of the ACE inhibitors. However, they still present a risk of hypotension and renal failure in patients with bilateral renal artery stenosis and hyperkalemia, and, rarely but much less frequently than with ACE inhibitors angioedema.
E. Calcium Channel Blocking Agents
These agents act by causing peripheral vasodilation but with less reflex tachycardia and fluid retention than other vasodilators. They are effective as single-drug therapy in approximately 60% of patients in all demographic groups and all grades of hypertension (Table 11-9). As a result, they may be preferable to -blockers and ACE inhibitors in blacks and older subjects. Calcium channel blockers and diuretics are less additive when given together than when either is combined with -blockers or ACE inhibitors. However, verapamil and diltiazem should be combined cautiously with -blockers because of their potential for depressing AV conduction and sinus node automaticity as well as contractility.
Initial concerns about possible adverse cardiac effects of calcium channel blockers have been convincingly allayed by several subsequent large studies which have demonstrated that calcium channel blockers are equivalent to ACE inhibitors, thiazide diuretics, and -blockers in prevention of coronary heart disease, major cardiovascular events, cardiovascular death, and total mortality. Diabetic patients receiving calcium channel blockers may have higher rates of heart failure and myocardial infarction than those receiving ACE inhibitors, and in other studies, heart failure has been more common than in patients treated with diuretics or ACE inhibitors. Whether these outcomes reflect beneficial effects of the comparators or specific risks of calcium channel blockers is uncertain. A protective effect against stroke with calcium blockers is well established, and in two trials (ALLHAT and the Systolic Hypertension in Europe trial), these agents appeared to be more effective than diuretic-based therapy.
The most common side effects of calcium channel blockers are headache, peripheral edema, bradycardia, and constipation (especially with verapamil in the elderly). The dihydropyridine agents nifedipine, nicardipine, isradipine, felodipine, nisoldipine, and amlodipine are more likely to produce symptoms of vasodilation, such as headache, flushing, palpitations, and peripheral edema. Calcium channel blockers have negative inotropic effects and may cause or exacerbate heart failure in patients with cardiac dysfunction. Amlodipine is the only calcium channel blocker with established safety in patients with severe heart failure. Most calcium channel blockers are now available in preparations that can be administered once daily.
F. -Adrenoceptor Antagonists
Prazosin, terazosin, and doxazosin (Table 11-10) block postsynaptic -receptors, relax smooth muscle, and reduce blood pressure by lowering peripheral vascular resistance. These agents are effective as single-drug therapy in some individuals, but tachyphylaxis may appear during long-term therapy and side effects are relatively common. These include marked hypotension and syncope after the first dose which, therefore, should be small and be given at bedtime. Postdosing palpitations, headache, and nervousness may continue to occur during long-term therapy; they may be less frequent or severe with doxazosin because of its more gradual onset of action.
Unlike the -blockers and diuretics, the -blockers have no adverse effect on serum lipid levels in fact, they increase HDL cholesterol while reducing total cholesterol. Whether this is beneficial in the long term has not been established. In ALLHAT, persons receiving doxazosin as initial therapy had a significant increase in heart failure hospitalizations and a higher incidence of stroke relative to the persons receiving diuretics and were removed from the study. To summarize, -blockers should generally not be used as initial agents to treat hypertension except perhaps in men with symptomatic prostatism.
G. Drugs with Central Sympatholytic Action
Methyldopa, clonidine, guanabenz, and guanfacine (Table 11-10) lower blood pressure by stimulating -adrenergic receptors in the central nervous system, thus reducing efferent peripheral sympathetic outflow. These agents are effective as single therapy in some patients, but they are usually used as second- or third-line agents because of the high frequency of drug intolerance, including sedation, fatigue, dry mouth, postural hypotension, and impotence. An important concern is rebound hypertension following withdrawal. Methyldopa also causes hepatitis and hemolytic anemia and is avoided except in individuals who have already tolerated long-term therapy. There is considerable experience with methyldopa in pregnant women, and it is still used for this population. Clonidine is available in patches and may have particular value in patients in whom compliance is a troublesome issue.
Table 11-9. Antihypertensive drugs: calcium channel blocking agents. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Table 11-10. -Adrenoceptor blocking agents, sympatholytics, and vasodilators. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
H. Arteriolar Dilators
Hydralazine and minoxidil (Table 11-10) relax vascular smooth muscle and produce peripheral vasodilation. When given alone, they stimulate reflex tachycardia, increase myocardial contractility, and cause headache, palpitations,
P.450
P.451
P.452
and fluid retention. They are usually given in combination with diuretics and -blockers in resistant patients. Hydralazine produces frequent gastrointestinal disturbances and may induce a lupus-like syndrome. Minoxidil causes hirsutism and marked fluid retention; this agent is reserved for the most refractory of cases.
I. Peripheral Sympathetic Inhibitors
These agents are now used infrequently and usually in refractory hypertension. Reserpine remains a cost-effective antihypertensive agent (Table 11-10). Its reputation for inducing mental depression and its other side effects sedation, nasal stuffiness, sleep disturbances, and peptic ulcers has made it unpopular, though these problems are uncommon at low dosages. Guanethidine and guanadrel inhibit catecholamine release from peripheral neurons but frequently cause orthostatic hypotension (especially in the morning or after exercise), diarrhea, and fluid retention.
Developing an Antihypertensive Regimen
Historically, data from a number of large trials support the overall conclusion that antihypertensive therapy with diuretics and -blockers has a major beneficial effect on a broad spectrum of cardiovascular outcomes. Similar placebo-controlled data pertaining to the newer agents are generally lacking, except for stroke reduction with the calcium channel blocker nitrendipine in the Systolic Hypertension in Europe trial. However, there is substantial evidence that ACE inhibitors, and to a lesser extent ARBs, reduce adverse cardiovascular outcomes in other related populations (eg, patients with diabetic nephropathy, heart failure, or postmyocardial infarction and individuals at high risk for cardiovascular events). Most large clinical trials that have compared outcomes in relatively unselected patients have failed to show a difference between newer agents such as ACE inhibitors, calcium channel blockers, and ARBs and the older diuretics and -blockers with regard to survival, myocardial infarction, and stroke. Therefore, experts recommend diuretics as the first-line treatment of most older patients with hypertension because these agents are less expensive than the newer agents. Exceptions are appropriate for individuals who have specific indications for another class of agent, such as postmyocardial infarction patients ( -blockers, ACE inhibitors), patients with diabetic nephropathy (ACE inhibitors, ARBs), or other comorbid conditions. Table 11-4 provides suggestions for individualizing first-line treatment based on compelling indications.
More recently, the perception that all antihypertensive drugs are equally effective at controlling cardiovascular risk has been challenged by the results of the ASCOT trial, which suggest that more modern agents (amlodipine/perindopril) are superior to the older combination (atenolol/bendroflumethiazide). For the reasons discussed above, many experts would suggest that -blockers no longer be considered ideal first-line drugs in the treatment of hypertension without compelling indications for their use and would tend to restrict the use of thiazide diuretics to older patients in whom they are particularly effective, The predominant use of thiazides in older patients would also limit exposure to the cumulative metabolic consequences of these drugs, a particular concern in young persons with hypertension who are subject to lifelong therapy.
For the purpose of devising an optimal treatment regimen, drugs can be divided into two complementary groups easily remembered as AB and CD. A and B refer to drugs that interrupt the renin-angiotensin system (ACE /ARB and -blockers) and C and D refer to those that do not (calcium channel blockers and thiazide diuretics). Combinations of drugs between these groups are likely to be more potent in lowering blood pressure than combinations within a group. Drugs A/B are more effective in young, white persons, in whom renins tend to be higher, and drugs C/D are more effective in old or black persons, in whom renin levels are generally lower. It is also important to note that antihypertensive treatment is effective at reducing cardiovascular risk at all ages, including the very elderly.
Figure 11-3 illustrates guidelines established by the BHS for developing a rational antihypertensive regimen. In these guidelines, B is placed in parentheses. This reflects the increasingly prevalent view that -blockers should no longer be considered an ideal first-line agent. In trials that include patients with systolic
P.453
hypertension, most patients require two or more medications and even then a substantial proportion of patients does not achieve the goal systolic blood pressure of < 140 mm Hg (< 130 mm Hg in high-risk individuals). In diabetic patients, three or four drugs are usually required to reduce systolic blood pressure to < 140 mm Hg. In many patients, blood pressure cannot be maintained at the recommended goal of < 130 mm Hg with any combination. As a result, debating the appropriate first-line agent is less relevant than determining the most appropriate combinations of agents. This has led many experts and practitioners to reconsider the use of fixed-dose combination antihypertensive agents as first-line therapy in patients with substantially elevated systolic pressures (> 160 mm Hg) or difficult-to-control hypertension (associated diabetes or renal dysfunction). Based both on antihypertensive efficacy and complementarity, combinations of a diuretic and an ACE inhibitor (or an ARB if patient is intolerant of ACE inhibitor) or a diuretic and a -blocker are recommended. In younger white patients, the best choice is probably a combination of an ACE inhibitor and a calcium channel blocker. The initial use of low-dose combinations allows faster blood pressure reduction without substantially higher intolerance rates and is likely to be better accepted by patients.
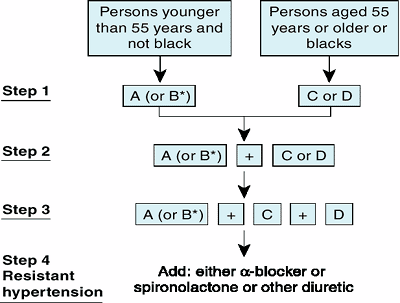 |
Figure 11-3. The British Hypertension Society's recommendations for combining blood pressure lowering drugs. The ABCD rule. A = Angiotensin-converting enzyme inhibitor or angiotensin receptor blocker; B = -blocker (the parentheses indicate that -blockers should no longer be considered ideal first-line agents); C = calcium channel blockers; D = diuretic (thiazide). (Reproduced with permission from: Guidelines for management of hypertension: report of the Fourth Working Party of the British Hypertension Society, 2004-BHS IV. J Hum Hypertens 2004;18:139 185. ) |
When an initial agent is selected, the patient should be informed of common side effects and the need for diligent compliance. Treatment should start at a low dose, and unless the initial blood pressure is very high (> 160/100 mm Hg), follow-up visits should usually be at 4- to 6-week intervals to allow for full medication effects to be established (especially with diuretics) before further titration or adjustment. If, after titration to usual doses, the patient has shown a discernible but incomplete response and a good tolerance of the initial drug, a second medication should be added.
Hypertension can be controlled in most patients with one-drug or two-drug regimens that combine complementary agents. A small number of patients require three, four, or even more medications in combination. Patients who are compliant with their medications and who do not respond to these combinations should usually be evaluated for secondary hypertension before proceeding to more complex regimens.
Special Considerations in the Treatment of Diabetic Hypertensive Patients
Hypertensive patients with diabetes are at particularly high risk for cardiovascular events. More aggressive treatment of hypertension in these patients prevents progressive nephropathy, myocardial infarction, and stroke. Treatment recommendations suggest a target of < 130/80 mm Hg. Because of their beneficial effects in diabetic nephropathy, ACE inhibitors (and ARBs in intolerant patients) should be part of the initial treatment regimen. However, most diabetics require combinations of three to five agents to achieve these goals, usually including a diuretic and a calcium channel blocker or -blocker. In addition to rigorous blood pressure control, treatment of persons with diabetes should include aggressive treatment of other risk factors and early intervention for coronary disease and left ventricular dysfunction.
Treatment of Hypertension in Chronic Kidney Disease
Hypertension is present in 40% of patients with a glomerular filtration rate (GFR) of 60 90 mL/min, and 75% of patients with a GFR < 30 mL/min. Many factors play a role in the hypertension of renal failure, including volume; the renin-angiotensin system; renal artery disease; activation of the sympathetic nervous system; and increased arterial stiffness and changes in vasoactive mediators, such as prostaglandins, endothelin, and parathyroid hormone. ACE inhibitors and ARBs have been shown to delay progression of renal impairment in persons with type 1 and type 2 diabetes, respectively. It is also likely that inhibition of the renin-angiotensin system protects renal function in nondiabetic renal disease associated with significant proteinuria.
As discussed above, hypertension should be treated until blood pressure reaches < 130/80 mm Hg in patients with chronic kidney disease. There is a lack of definitive data to show that tighter blood pressure control slows the decline of GFR in persons with hypertensive chronic kidney disease without high-grade proteinuria. However, since all patients with chronic kidney disease are at high risk for cardiovascular damage, treatment of blood pressure to the < 130/80 mm Hg target is appropriate, and interruption of the renin-angiotensin system would seem a reasonable approach. Furthermore, it has recently been demonstrated that ACE inhibitors remain protective and safe in renal disease associated with significant proteinuria and creatinine as high as 5 mg/dL. It should be noted that such treatment would likely result in acute worsening of renal function in patients with significant renal artery stenosis, so renal function and electrolytes should be monitored carefully after introduction of ACE inhibitors.
Hypertension Management in Blacks
Substantial evidence indicates that blacks are not only more likely to become hypertensive and more susceptible to the cardiovascular complications of hypertension they also respond differently to many antihypertensive medications. This may reflect genetic differences in the cause of hypertension or the subsequent responses to it, differences in occurrence of comorbid conditions such as diabetes or obesity, or environmental factors such as diet, activity, stress, or access to health care services. In any case, as in all persons with hypertension, a multifaceted program of education and lifestyle modification is warranted. Because it appears that ACE inhibitors and ARBs in the absence of concomitant diuretics are less effective in blacks than in whites, initial therapy should generally be a diuretic or a diuretic combination, with the
P.454
use of additional agents as discussed above. Some experts have recommended a goal blood pressure of 130/80 mm Hg for blacks at high risk for cardiovascular events as well as those with diabetes.
Treatment of Additional Cardiovascular Risk Factors
Because the goal is to reduce cardiovascular morbidity and mortality, attention must be paid to the management of other risk factors. Elevated LDL cholesterol should be aggressively treated (see above), and patients should be urged to stop smoking, exercise regularly, and lose weight.
Follow-Up of the Treated Hypertensive Patient
Once blood pressure is controlled on a well-tolerated regimen, follow-up visits can be infrequent and laboratory testing limited to tests appropriate for the patient and the medications used. Yearly monitoring of blood lipids is recommended, and an electrocardiogram should be repeated at 2- to 4-year intervals depending on whether initial abnormalities are present, the presence of coronary risk factors, and age.
Patients who have had excellent blood pressure control for several years, especially if they have lost weight and initiated favorable lifestyle modifications, should be considered for step-down of therapy to determine whether lower doses or discontinuation of medications are feasible.
August P: Initial treatment of hypertension. N Engl J Med 2003;348:620.
Barzilay JI et al; ALLHAT Collaborative Research Group: Cardiovascular outcomes using doxazosin vs. chlorthalidone for the treatment of hypertension in older adults with and without glucose disorders: a report from the ALLHAT study. J Clin Hypertens (Greenwich) 2004;6:116.
Brewster LM et al: Systematic review: antihypertensive drug therapy in black patients. Ann Intern Med 2004;14:614.
Chobanian AV et al: The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: The JNC 7 Report. JAMA 2003;289:2560.
Dahlof B et al: Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 2002;359:995.
Dahlof B et al; ASCOT Investigators: Prevention of cardiovascular events with an antihypertensive regimen of amlodipine adding perindopril as required versus atenolol adding bendroflumethiazide as required, in the Anglo-Scandinavian Cardiac Outcomes Trial-Blood Pressure Lowering Arm (ASCOT-BPLA): a multicentre randomised controlled trial. Lancet 2005;366:895.
Iino Y et al; Japanese Losartan Therapy Intended for the Global Renal Protection in Hypertensive Patients (JLIGHT) Study Investigators: Renoprotective effect of losartan in comparison to amlodipine in patients with chronic kidney disease and hypertension. Hypertens Res 2004;27:21.
Julius S et al; VALUE trial group: Outcomes in hypertensive patients at high cardiovascular risk treated with regimens based on valsartan or amlodipine: the VALUE randomised trial. Lancet 2004;363:2022.
Khan NA et al; Canadian Hypertension Education Program: The 2004 Canadian recommendations for the management of hypertension: Part II Therapy. Can J Cardiol 2004;20:41.
Kuschnir E et al: Effects of the combination of low-dose nifedipine GITS 20 mg and losartan 50 mg in patients with mild to moderate hypertension. J Cardiovasc Pharmacol 2004;43: 300.
Lindholm LH et al: Should beta blockers remain first choice in the treatment of primary hypertension? A meta-analysis. Lancet 2005;366:1545.
London GM et al; REASON Project Investigators: Mechanism(s) of selective systolic blood pressure reduction after a low-dose combination of perindopril/indapamide in hypertensive subjects: comparison with atenolol. J Am Coll Cardiol 2004;43:92.
Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic. The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA 2002;288:2981.
Papademetriou V et al: Stroke prevention with the angiotensin II type 1-receptor blocker candesartan in elderly patients with isolated systolic hypertension: the Study on Cognition and Prognosis in the Elderly (SCOPE). J Am Coll Cardiol 2004; 44:1175.
Psaty BM et al: Health outcomes associated with various antihypertensive therapies used as first-line agents: a network meta-analysis. JAMA 2003;289:2534.
Sehgal AR: Overlap between whites and blacks in response to antihypertensive drugs. Hypertension 2004;43:566.
Staessen JA et al; Treatment of Hypertension Based on Home or Office Blood Pressure (THOP) Trial Investigators: Antihypertensive treatment based on blood pressure measurement at home or in the physician's office: a randomized controlled trial. JAMA 2004;291:955.
Stergiou GS et al; World Health Organization-International Society of Hypertension (WHO-ISH); USA Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC-7); European Society of Hypertension-European Society of Cardiology (ESH-ESC): New European, American and International guidelines for hypertension management: agreement and disagreement. Expert Rev Cardiovasc Ther 2004;2:359.
Verberk WJ et al: Home versus Office blood pressure Measurements: Reduction of Unnecessary treatment Study: rationale and study design of the HOMERUS trial. Blood Press 2003;12:326.
Vijan S et al: Treatment of hypertension in type 2 diabetes mellitus: blood pressure goals, choice of agents, and setting priorities in diabetes care. Ann Intern Med 2003;138:593.
Wing LM et al: A comparison of outcomes with angiotensin-converting-enzyme inhibitors and diuretics for hypertension in the elderly. N Engl J Med 2003;348:583.
Resistant Hypertension
Resistant hypertension is defined in JNC 7 as the failure to reach blood pressure control in patients who are adherent to full doses of an appropriate three-drug
P.455
regimen (including a diuretic). In this situation, the clinician should first exclude potential identifiable causes of hypertension (Table 11-3), and then carefully explore reasons why the patient might not be at goal blood pressure (Table 11-11). The clinician should pay particular attention to the type of diuretic being used in relation to the patient's renal function. If goal blood pressure cannot be achieved by these measures, consultation with a hypertension specialist should be considered.
Table 11-11. Causes of resistant hypertension. | ||
|---|---|---|
|
Hypertensive Urgencies & Emergencies
Hypertensive emergencies have become less frequent in recent years but still require prompt recognition and aggressive but careful management. A spectrum of urgent presentations exists, and the appropriate therapeutic approach varies accordingly.
Hypertensive urgencies are situations in which blood pressure must be reduced within a few hours. These include patients with asymptomatic severe hypertension (systolic blood pressure > 220 mm Hg or diastolic pressure > 125 mm Hg that persists after a period of observation) and those with optic disk edema, progressive target organ complications, and severe perioperative hypertension. Elevated blood pressure levels alone in the absence of symptoms or new or progressive target organ damage rarely require emergency therapy. Parenteral drug therapy is not usually required, and partial reduction of blood pressure with relief of symptoms is the goal.
Hypertensive emergencies require substantial reduction of blood pressure within 1 hour to avoid the risk of serious morbidity or death. Although blood pressure is usually strikingly elevated (diastolic pressure > 130 mm Hg), the correlation between pressure and end-organ damage is often poor. It is the latter that determines the seriousness of the emergency and the approach to treatment. Emergencies include hypertensive encephalopathy (headache, irritability, confusion, and altered mental status due to cerebrovascular spasm), hypertensive nephropathy (hematuria, proteinuria, and progressive renal dysfunction due to arteriolar necrosis and intimal hyperplasia of the interlobular arteries), intracranial hemorrhage, aortic dissection, preeclampsia-eclampsia, pulmonary edema, unstable angina, or myocardial infarction. Malignant hypertension is by historical definition characterized by encephalopathy or nephropathy with accompanying papilledema. Progressive renal failure usually ensues if treatment is not provided. The therapeutic approach is identical to that used with other antihypertensive emergencies.
Parenteral therapy is indicated in most hypertensive emergencies, especially if encephalopathy is present. The initial goal in hypertensive emergencies is to reduce the pressure by no more than 25% (within minutes to 1 or 2 hours) and then toward a level of 160/100 mm Hg within 2 6 hours. Excessive reductions in pressure may precipitate coronary, cerebral, or renal ischemia. To avoid such declines, the use of agents that have a predictable, dose-dependent, transient, and not precipitous antihypertensive effect is preferable. In that regard, the use of sublingual or oral fast-acting nifedipine preparations is best avoided.
Acute ischemic stroke is often associated with marked elevation of blood pressure, which will usually fall spontaneously. In such cases, antihypertensives should only be used if the blood pressure exceeds 220/120 mm Hg, and blood pressure should be reduced cautiously by 10 15%. If thrombolytics are to be given, blood pressure should be maintained at < 185/110 mm Hg during treatment and for 24 hours following treatment.
In hemorrhagic stroke, the aim is to minimize bleeding with a target mean arterial pressure of < 130 mm Hg. In acute subarachnoid hemorrhage, as long as the bleeding source remains uncorrected, a compromise must be struck between preventing further bleeding and maintaining cerebral perfusion in the face of cerebral vasospasm. In this situation, blood pressure goals depend on the patient's usual blood pressure. In normotensive patients, the target should be a systolic blood pressure of 110 120 mm Hg; in hypertensive patients, blood pressure should be treated to 20% below baseline pressure. In the treatment of hypertensive emergencies complicated by (or precipitated by) central nervous system injury, labetalol or nicardipine are good choices, since they are nonsedating and do not cause significant cerebral vasodilation,
P.456
which can increase intracranial pressure (a potential problem with sodium nitroprusside). In hypertensive emergencies arising from catecholaminergic mechanisms, such as pheochromocytoma or cocaine use, -blockers can worsen the hypertension because of unopposed peripheral vasoconstriction; phentolamine is a better choice. Labetalol is useful in these patients if the heart rate must be controlled.
Pharmacologic Management
A. Parenteral Agents
A growing number of agents are available for management of acute hypertensive problems. (Table 11-12 lists drugs, dosages, and adverse effects.) Sodium nitroprusside is the agent of choice for the most serious emergencies because of its rapid and easily controllable action, but continuous monitoring is essential when this agent is used. In the presence of myocardial ischemia, intravenous nitroglycerin or an intravenous -blocker, such as labetalol or esmolol, is preferable.
1. Nitroprusside sodium
This agent is given by controlled intravenous infusion gradually titrated to the desired effect. It lowers the blood pressure within seconds by direct arteriolar and venous dilation. Monitoring with an intra-arterial line avoids hypotension. Nitroprusside in combination with a -blocker is especially useful in patients with aortic dissection.
2. Nitroglycerin, intravenous
This agent is a less potent antihypertensive than nitroprusside and should be reserved for patients with accompanying acute ischemic syndromes.
3. Labetalol
This combined - and -blocking agent is the most potent adrenergic blocker for rapid blood pressure reduction. Other -blockers are far less potent. Excessive blood pressure drops are unusual. Experience with this agent in hypertensive syndromes associated with pregnancy has been favorable.
4. Esmolol
This rapidly acting -blocker is approved only for treatment of supraventricular tachycardia but is often used for lowering blood pressure. It is less potent than labetalol and should be reserved for patients in whom there is particular concern about serious adverse events related to -blockers.
5. Nicardipine
Intravenous nicardipine is the most potent antihypertensive agent and the longest acting of the parenteral calcium channel blockers. As a primarily arterial vasodilator, it has the potential to precipitate reflex tachycardia, and for that reason it should not be used without a -blocker in patients with coronary artery disease.
6. Fenoldopam
Fenoldopam is a peripheral dopamine-1 (DA1) receptor agonist that causes a dose-dependent reduction in arterial pressure without evidence of tolerance, rebound, or withdrawal or deterioration of renal function. In higher dosage ranges, tachycardia may occur.
7. Enalaprilat
This is the active form of the oral ACE inhibitor enalapril. The onset of action is usually within 15 minutes, but the peak effect may be delayed for up to 6 hours. Thus, enalaprilat is used primarily as an adjunctive agent.
8. Diazoxide
Diazoxide acts promptly as a vasodilator without decreasing renal blood flow. To avoid hypotension, it should be given in small boluses or as an infusion rather than as the previously recommended large bolus. One use of diazoxide has been in preeclampsia-eclampsia. Hyperglycemia and sodium and water retention may occur. The drug should be used only for short periods and is best combined with a loop diuretic.
9. Hydralazine
Hydralazine can be given intravenously or intramuscularly, but its effect is less predictable than that of other drugs in this group. It produces reflex tachycardia and should not be given without -blockers in patients with possible coronary disease or aortic dissection. Hydralazine is now used primarily in pregnancy and in children, but even in these situations, newer agents are supplanting it.
10. Trimethaphan
The ganglionic blocking agent trimethaphan is titrated with the patient sitting; its activity depends on this. The patient can be placed supine if the hypotensive effect is excessive. The effect occurs within a few minutes and persists for the duration of the infusion. This agent has largely been replaced by nitroprusside and newer medications.
11. Diuretics
Intravenous loop diuretics can be very helpful when the patient has signs of heart failure or fluid retention, but the onset of their hypotensive response is slow, making them an adjunct rather than a primary agent for hypertensive emergencies. Low dosages should be used initially (furosemide, 20 mg or bumetanide, 0.5 mg). They facilitate the response to vasodilators, which often stimulate fluid retention.
B. Oral Agents
Patients with less severe acute hypertensive syndromes can often be treated with oral therapy. Abrupt blood pressure lowering is not usually necessary in asymptomatic individuals, and the use of agents such as rapid-acting nifedipine probably causes more adverse effects than benefits.
1. Clonidine
Clonidine, 0.2 mg orally initially, followed by 0.1 mg every hour to a total of 0.8 mg, will usually lower blood pressure over a period of several hours. Sedation is frequent, and rebound hypertension may occur if the drug is stopped.
2. Captopril
Captopril, 12.5 25 mg orally, will also lower blood pressure in 15 30 minutes. The response is variable and may be excessive.
Table 11-12. Drugs for hypertensive emergencies and urgencies. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
3. Nifedipine
Fast-acting nifedipine capsules are commonly used in the emergency department or urgent care setting because they usually provide a rapid reduction in blood pressure. However, the nifedipine
P.457
P.458
P.459
effect is unpredictable and may be excessive, resulting in hypotension and reflex tachycardia. Because myocardial infarction and stroke have been reported in this setting, the use of nifedipine without concomitant -blocker therapy is not advised.
C. Subsequent Therapy
When the blood pressure has been brought under control, combinations of oral antihypertensive agents can be added as parenteral drugs are tapered off over a period of 2 3 days. Most subsequent regimens should include a diuretic.
Cherney D et al: Management of patients with hypertensive urgencies and emergencies. J Gen Intern Med 2002;17:947.
Devlin JW et al: Fenoldopam versus nitroprusside for the treatment of hypertensive emergency. Ann Pharmacother 2004; 38:755.
Khanna A et al: Malignant hypertension presenting as hemolysis, thrombocytopenia, and renal failure. Rev Cardiovasc Med 2003;4:255.
Migneco A et al: Hypertensive crises: diagnosis and management in the emergency room. Eur Rev Med Pharmacol Sci 2004; 8:143.
Phillips RA et al: Hypertensive emergencies: diagnosis and management. Prog Cardiovasc Dis 2002;45:33.
EAN: 2147483647
Pages: 49